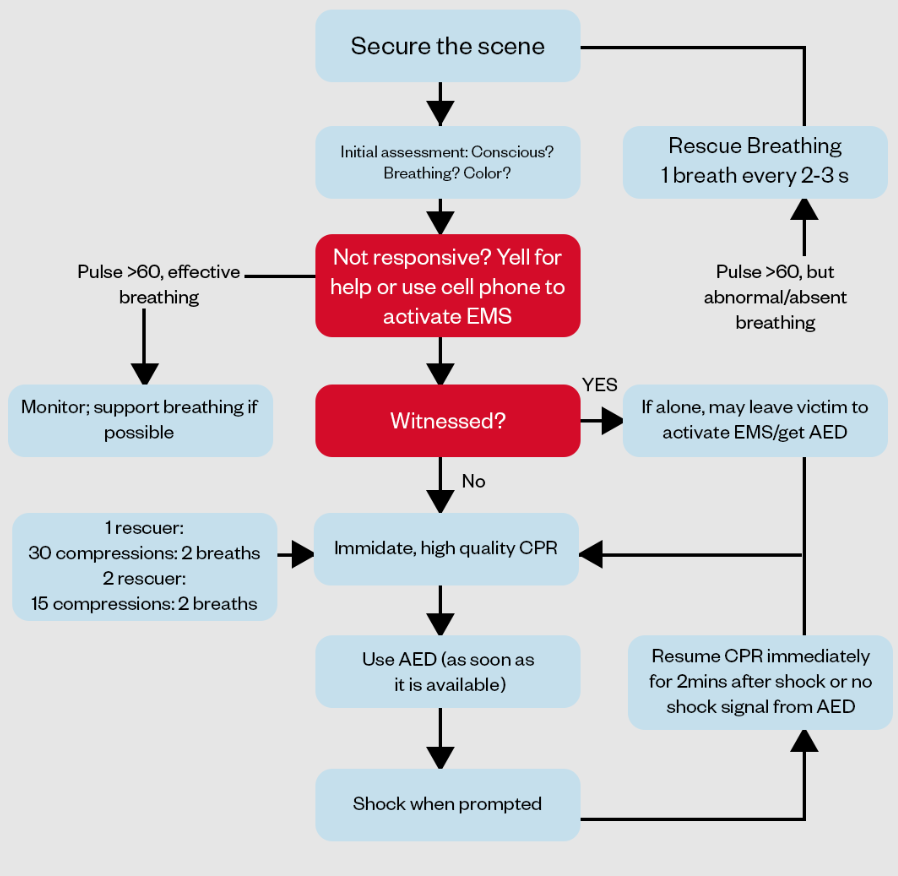
When a child’s breathing is in trouble, knowing how to quickly check if their oxygenation and ventilation are effective can make all the difference. You might wonder, how do you really tell if your little patient is getting enough oxygen or if their lungs are working properly?
Understanding these signs isn’t just important—it’s lifesaving. You’ll discover simple, clear ways to assess oxygenation and ventilation during Pediatric Advanced Life Support (PALS). By the end, you’ll feel confident spotting the crucial clues that guide urgent care decisions. Ready to sharpen your skills and improve outcomes?
Let’s dive in.
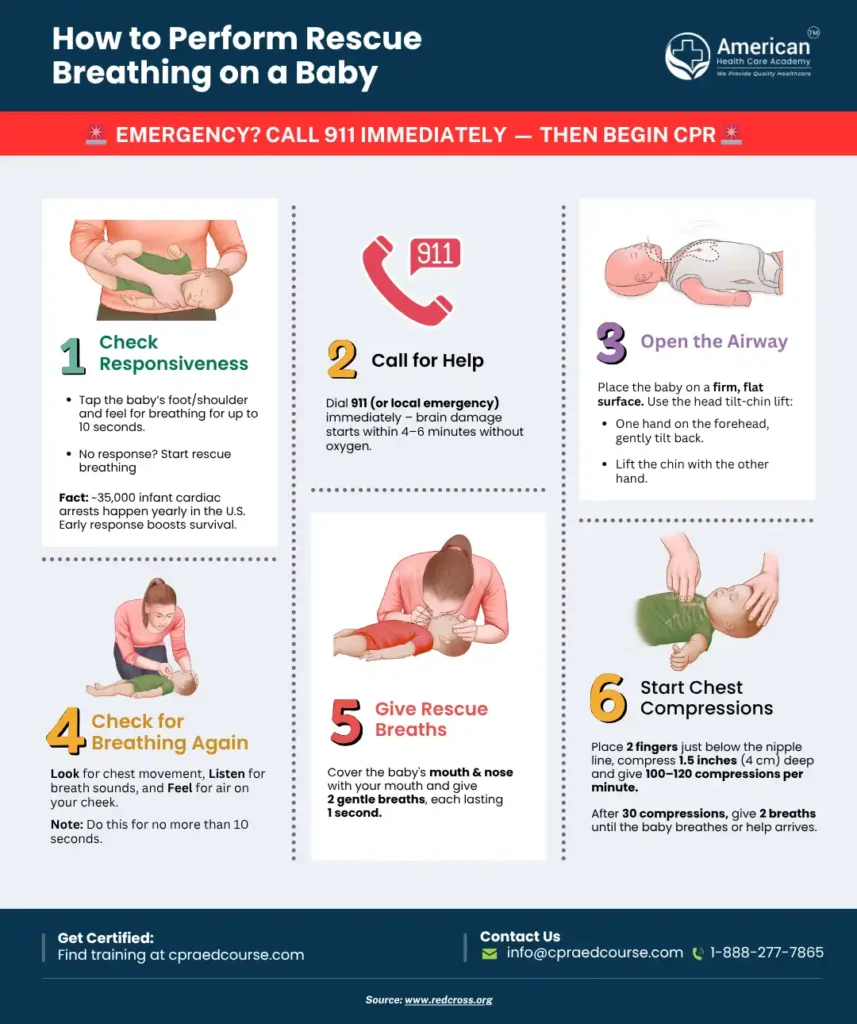
Credit: cpraedcourse.com
Signs Of Effective Oxygenation
Recognizing the signs of effective oxygenation is vital when assessing a child’s respiratory status in Pediatric Advanced Life Support (PALS). These signs offer immediate clues about how well oxygen is reaching the tissues. Paying close attention to these indicators helps you make quick, informed decisions during critical moments.
Skin Color And Capillary Refill
One of the simplest ways to gauge oxygenation is by observing skin color. Healthy oxygen levels usually mean pink, well-perfused skin. Pale, mottled, or bluish tones can signal inadequate oxygen delivery.
Capillary refill time adds another layer to your assessment. Pressing on the child’s nail bed or skin and watching how fast color returns gives insight into blood flow and oxygenation. Ideally, color should return within 2 seconds.
Have you ever noticed how a slight delay in capillary refill changed your approach in an emergency? This quick check can steer your actions more than you might expect.
Pulse Oximetry Readings
Pulse oximetry is a non-invasive tool that provides real-time oxygen saturation levels (SpO2). Values above 94% are generally considered acceptable in most pediatric patients, but individual situations may vary.
Keep in mind that factors like poor circulation, motion, or nail polish can affect the accuracy of these readings. Always correlate pulse oximetry results with clinical signs.
Imagine relying solely on numbers without assessing the child’s overall appearance. Would you trust a reading of 98% if the child looks blue? Probably not. Use pulse oximetry as a guide, not the only source.
Breath Sounds And Respiratory Effort
Listening to breath sounds helps identify how well air moves in and out of the lungs. Clear, equal breath sounds on both sides usually indicate effective ventilation and oxygenation.
Notice the child’s work of breathing. Are they using accessory muscles? Is there nasal flaring or grunting? These signs suggest the child is struggling to oxygenate properly.
Have you ever detected subtle wheezing or crackles that hinted at a deeper problem? Paying attention to these details can change the course of your intervention swiftly.
Evaluating Ventilation Efficiency
Evaluating ventilation efficiency is vital in Pediatric Advanced Life Support (PALS). It ensures the child receives enough air to support life. Proper ventilation helps maintain oxygen and carbon dioxide balance. Careful assessment guides effective treatment and improves outcomes.
Chest Rise And Symmetry
Observe the chest for visible rise and fall with each breath. Symmetrical chest movement shows both lungs receive air evenly. Uneven or absent chest rise may indicate airway blockage or lung collapse. Watch closely during bag-mask ventilation or intubation. Proper chest rise confirms effective air delivery to the lungs.
End-tidal Co2 Monitoring
End-tidal CO2 (ETCO2) measures carbon dioxide at the airway’s end. It reflects how well the patient exhales carbon dioxide. A normal ETCO2 value indicates good ventilation and circulation. Low or absent ETCO2 can signal poor airway placement or ventilation issues. Continuous ETCO2 monitoring helps adjust ventilation in real time.
Respiratory Rate And Pattern
Count the breaths per minute to check the respiratory rate. Normal rates vary by age but must be steady and regular. Irregular breathing or very fast or slow rates may show distress. Watch the breathing pattern for signs of effort or obstruction. Proper rate and pattern support effective gas exchange in the lungs.
Tools For Oxygenation And Ventilation Assessment
Assessing oxygenation and ventilation effectively is crucial in Pediatric Advanced Life Support (PALS). The right tools help you monitor a child’s respiratory status and adjust treatment promptly. Understanding these tools allows you to respond quickly when every second counts.
Pulse Oximeter Use And Limitations
A pulse oximeter measures oxygen saturation (SpO2) non-invasively. It’s simple to use and provides continuous monitoring, which is vital during resuscitation or respiratory distress.
However, it has limitations. Poor perfusion, movement, or nail polish can cause inaccurate readings. Also, it doesn’t measure ventilation or carbon dioxide levels, so relying solely on it can miss hypoventilation issues. Have you ever noticed a normal SpO2 but the patient still looks distressed? That’s why you need more than just this tool.
Capnography In Pediatric Care
Capnography measures end-tidal carbon dioxide (ETCO2) and gives real-time feedback about ventilation. It’s especially useful during intubation to confirm tube placement and monitor effectiveness of ventilation.
It also helps detect early signs of respiratory failure or circulation problems. However, it requires specific equipment and expertise to interpret the waveforms accurately. Do you know how a sudden drop in ETCO2 could signal an airway obstruction or cardiac arrest?
Blood Gas Analysis
Blood gas analysis provides detailed information about oxygenation, ventilation, and acid-base balance. It’s the most comprehensive way to assess respiratory status, especially in critically ill children.
Although it requires blood samples and lab processing, the data can guide precise adjustments in oxygen therapy and ventilation settings. Have you seen how changes in PaCO2 and pH can influence your next clinical decision?
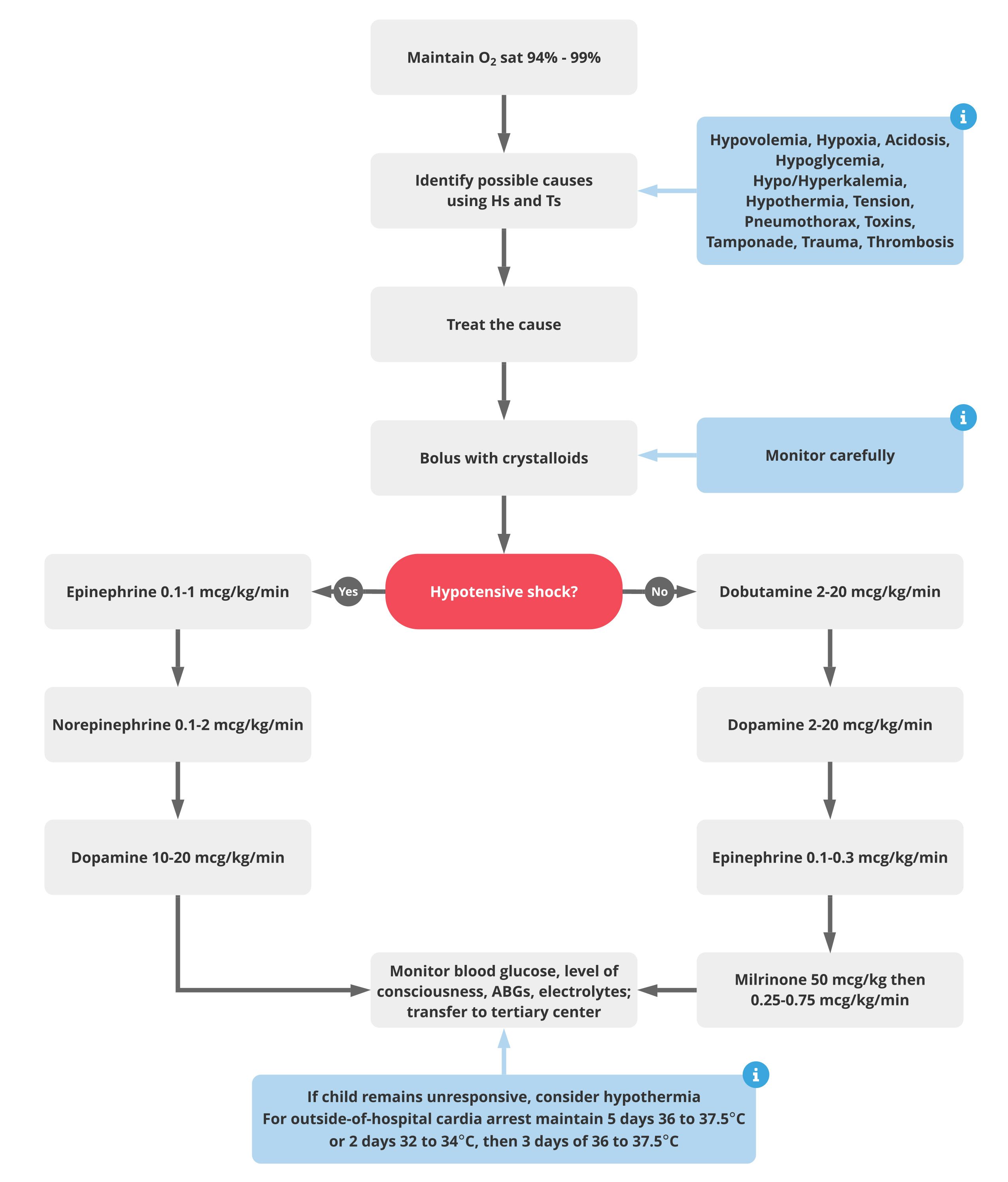
Credit: www.aclsmedicaltraining.com
Common Challenges In Assessment
Assessing effective oxygenation and ventilation in PALS comes with challenges. These challenges can affect the accuracy of the assessment process. Recognizing and addressing these issues is vital for proper patient care.
Artifacts And False Readings
Artifacts are common in medical assessments. They can lead to false readings. These artifacts often arise from external electronic interference. They can distort the data collected from monitoring devices. Identifying and correcting these artifacts is crucial. This ensures accurate readings of oxygenation and ventilation.
Patient Movement And Cooperation
Patient movement can disrupt assessment accuracy. Children may find it hard to stay still during evaluations. This movement can affect sensor placement. It can also cause fluctuations in readings. Ensuring patient cooperation helps in gathering reliable data.
Equipment Calibration And Maintenance
Regular equipment calibration is necessary. Proper maintenance ensures devices function correctly. Malfunctioning equipment can provide incorrect data. Routine checks and servicing help maintain the equipment’s accuracy and reliability. This guarantees precise assessments in clinical settings.
Improving Assessment Accuracy
Improving assessment accuracy in effective oxygenation and ventilation during Pediatric Advanced Life Support (PALS) is essential to ensure timely and appropriate interventions. Relying solely on one form of assessment can lead to missed signs or delayed responses. Combining multiple approaches and tools helps you gain a clearer picture of the patient’s respiratory status.
Combining Clinical Signs With Monitoring
Clinical signs like skin color, chest movement, and respiratory effort give you immediate, visible clues about a child’s oxygenation and ventilation. However, these signs can be subtle or misleading, especially in infants or critically ill children. That’s why pairing these observations with monitoring devices like pulse oximeters and capnography improves your accuracy.
For example, a child might appear pink but still have low oxygen saturation. Continuous pulse oximetry alerts you to this discrepancy early. Do you consistently check both signs and monitors during your assessments?
Regular Training And Simulation
Practice sharpens your ability to recognize and respond to oxygenation and ventilation issues quickly. Simulation training provides a safe environment to experience real-life scenarios without risk. It helps you build muscle memory and confidence in interpreting clinical signs and monitor readings.
During simulations, focus on recognizing subtle changes in ventilation quality and oxygenation status. Have you ever noticed how simulations reveal gaps in your assessment skills that you might overlook in real emergencies?
Protocols And Checklists
Standardized protocols and checklists guide your assessment process, minimizing errors and omissions. These tools ensure you assess key parameters systematically, such as respiratory rate, breath sounds, oxygen saturation, and end-tidal CO2. They also help your team communicate clearly during critical moments.
Using checklists can prevent skipping important steps under pressure. Next time you prepare for a PALS event, consider how a simple checklist might improve your assessment accuracy and patient outcomes.
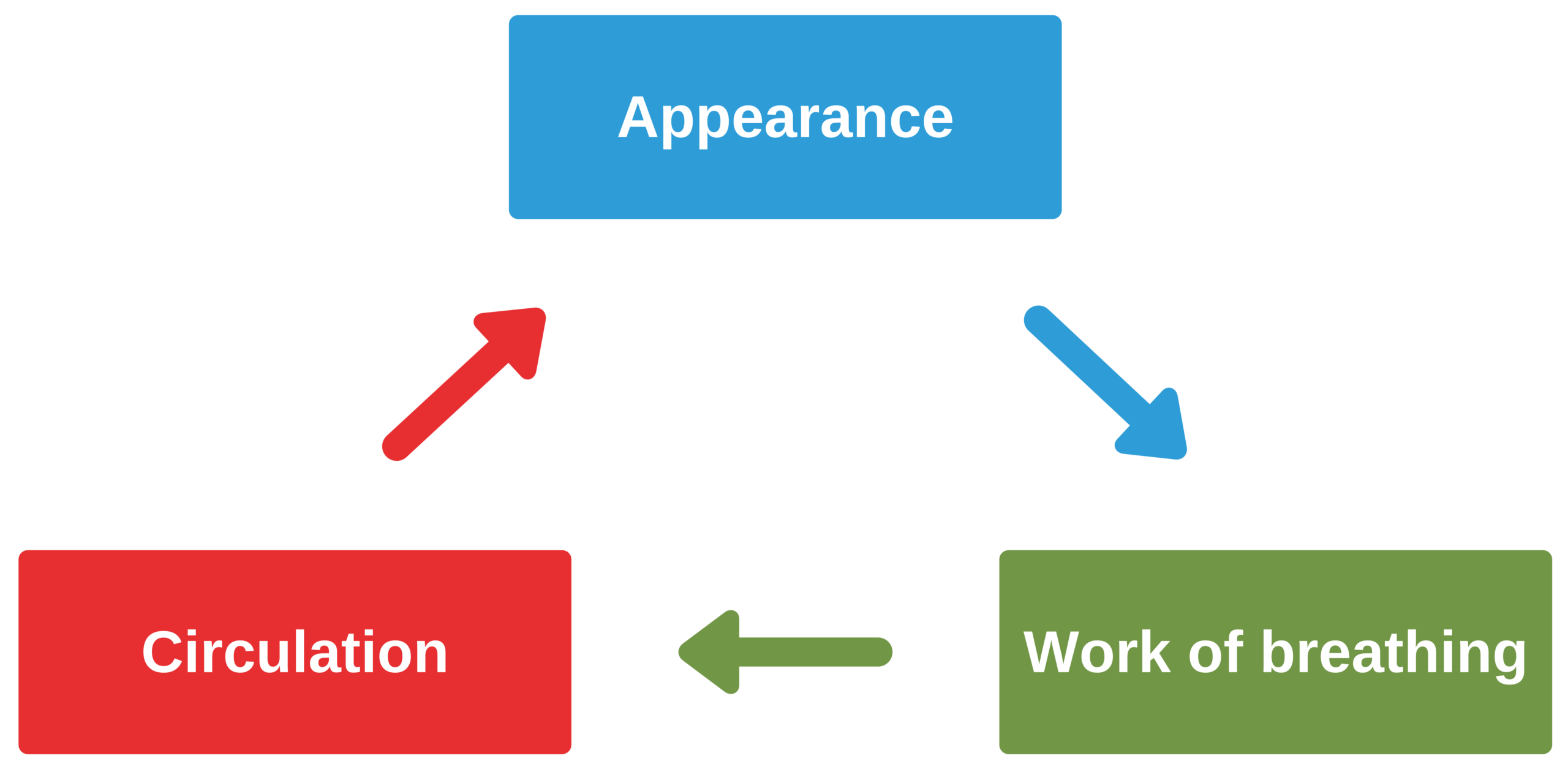
Credit: aclscertification.org
Frequently Asked Questions
What Is The Importance Of Assessing Oxygenation In Pals?
Assessing oxygenation in PALS ensures adequate oxygen delivery to tissues. It helps detect hypoxemia early and guides proper interventions to prevent organ damage and improve survival outcomes.
How Is Ventilation Effectiveness Evaluated In Pediatric Patients?
Ventilation effectiveness is evaluated by monitoring respiratory rate, chest rise, and carbon dioxide levels. Capnography and blood gases provide precise data on ventilation quality.
What Tools Measure Oxygenation And Ventilation In Pals?
Pulse oximetry measures oxygen saturation, while capnography assesses ventilation by monitoring exhaled CO2. Blood gas analysis offers comprehensive respiratory status information.
Why Monitor End-tidal Co2 In Pediatric Resuscitation?
End-tidal CO2 monitoring confirms proper airway placement and ventilation quality. It helps detect respiratory failure early and guides adjustments during resuscitation.
Conclusion
Effective oxygenation and ventilation assessment saves children’s lives. Watch for chest rise and listen to breath sounds. Check pulse oximetry for oxygen levels regularly. Observe skin color for signs of good blood flow. Use capnography to monitor carbon dioxide removal.
Quick, clear actions help respond to problems early. Practice these steps often to build confidence. Clear assessments guide proper treatment and improve outcomes. Keep skills sharp; every second counts in PALS care.