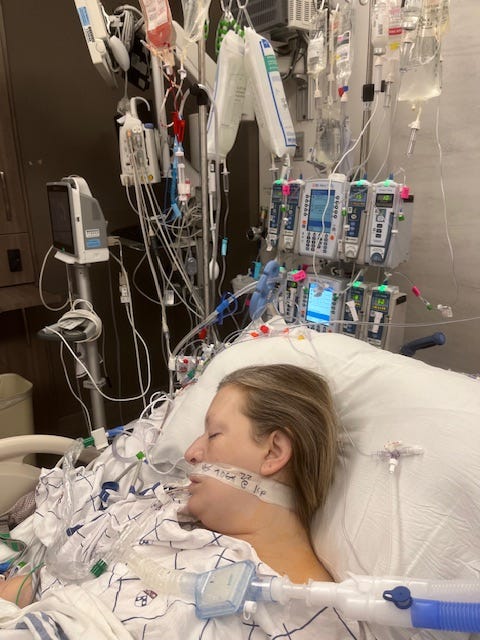
Have you ever wondered what it feels like to be on a ventilator? You might think being on a machine that helps you breathe means you’re completely unconscious.
But is that really true? Understanding whether you are conscious while on a ventilator can change how you feel about medical treatments and ease a lot of fears. You’ll discover what happens to your mind and body when you’re connected to a ventilator.
By the end, you’ll have clear answers and feel more in control of this critical experience. Keep reading to uncover the surprising truth about consciousness on a ventilator.
Consciousness On A Ventilator
Being on a ventilator can feel like entering a world where your body is partly controlled by machines. Yet, many wonder about the state of their mind during this time. Understanding consciousness on a ventilator helps you grasp what it means to be aware or unaware while relying on life-support.
What Being Conscious Means
Consciousness is your ability to experience thoughts, feelings, and surroundings. It means you can respond to stimuli, like voices or touch, and know where you are. But consciousness isn’t simply “awake” or “asleep.”
It covers a range from full alertness to deep unconsciousness. Imagine hearing your family’s voices but not being able to speak back—that’s a state of partial consciousness. Knowing this can help you understand what patients might feel during ventilation.
Levels Of Awareness During Ventilation
When on a ventilator, your awareness can vary widely. You might be fully alert and able to communicate, or deeply sedated and unaware. Here are some common levels:
- Full Consciousness:You can interact, follow commands, and are aware of your environment.
- Light Sedation:You may feel drowsy but still respond to voices or touch.
- Deep Sedation:You are mostly unaware of surroundings, often unable to respond.
- Unconsciousness:No awareness or response, similar to being in a coma.
Have you ever wondered what it’s like to be aware but trapped inside your body? Many patients report mixed memories of sensations and dreams while ventilated. This shows how complex consciousness can be during such critical care.

Credit: preop.com
How Ventilators Work
Ventilators help people breathe when their lungs cannot do the job alone. These machines push air into the lungs to keep oxygen flowing. They support breathing in different ways, depending on the patient’s needs. Understanding how ventilators work can ease concerns about being conscious while using one.
Mechanical Breathing Support
A ventilator moves air into and out of the lungs. It uses a tube placed in the windpipe. The machine controls how much air enters and leaves the lungs. It can adjust the speed and pressure of the breaths. This support helps keep oxygen levels steady in the body.
The ventilator can work in different modes:
- Assist control, where the machine fully controls breathing.
- Support mode, where the machine helps with some breaths.
- Spontaneous breathing, where the patient starts breaths and the machine assists.
These modes allow the machine to match the patient’s breathing needs.
Sedation And Its Role
Sedation helps patients feel calm and comfortable on a ventilator. It reduces anxiety and the feeling of breathlessness. Doctors decide sedation levels carefully to keep the patient alert if possible. Too much sedation can make the patient unconscious, but too little may cause discomfort.
Sedation helps patients tolerate the breathing tube. It also prevents fighting against the machine’s breathing support. Nurses and doctors monitor sedation closely to balance comfort and awareness.
Sedation And Awareness
Being on a ventilator often requires sedation to keep patients calm and comfortable. Sedation helps reduce stress and prevents fighting against the machine. Awareness during ventilation varies. Some patients may feel fully asleep. Others might have moments of partial awareness. Understanding sedation and awareness helps ease fears about this experience.
Types Of Sedatives Used
Doctors use different sedatives to help patients on ventilators. Common drugs include:
- Propofol – fast-acting and easy to control
- Midazolam – helps with anxiety and memory loss
- Fentanyl – provides pain relief and sedation
- Dexmedetomidine – keeps patients calm without deep sleep
Each drug has a specific role. Doctors adjust doses based on patient needs. The goal is comfort without too much sedation.
Possibility Of Partial Awareness
Sometimes patients may feel some awareness while sedated. It can be confusing or frightening. Partial awareness may include:
- Hearing voices or sounds
- Feeling pressure or movement
- Dream-like or unclear memories
This happens because sedatives do not always block all senses. Medical teams monitor patients closely to manage this. They aim to minimize discomfort and anxiety during ventilation.
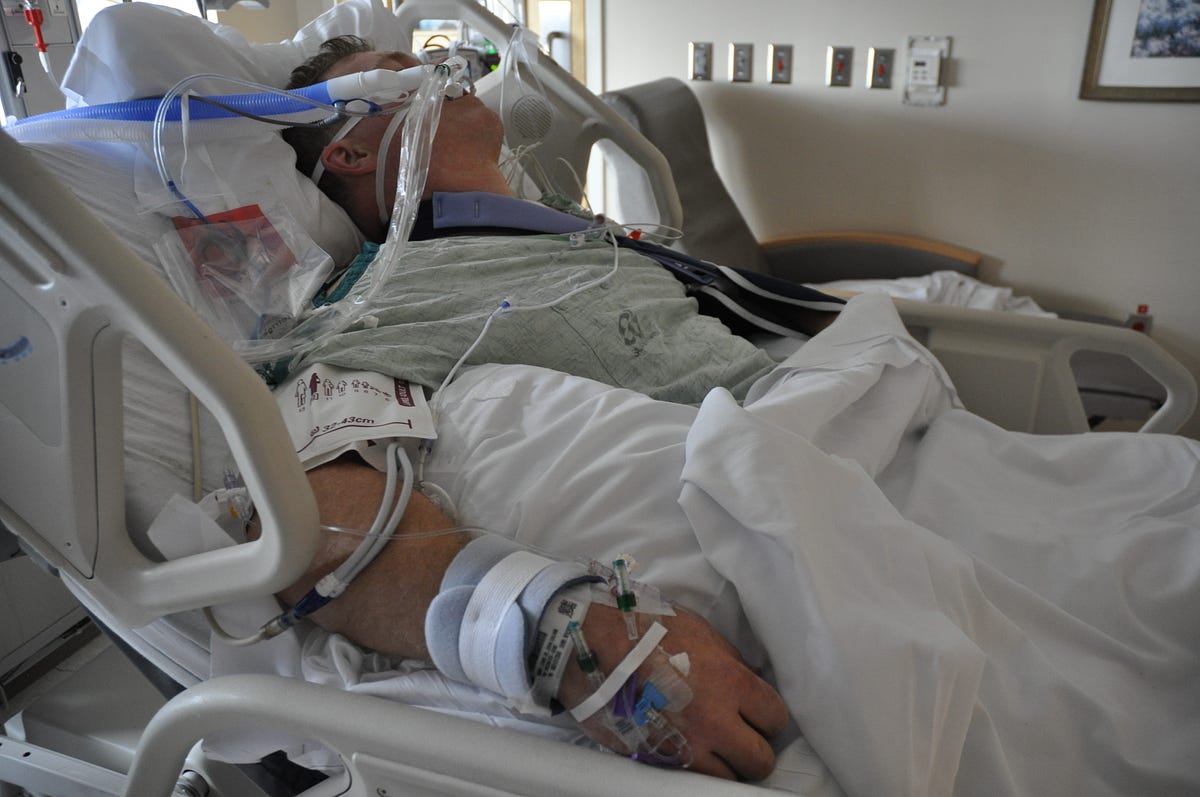
Credit: medium.com
Patient Experiences On Ventilators
Patient experiences on ventilators vary widely and can be quite complex. While many patients are fully sedated and unaware, others report vivid memories or sensations. Understanding these experiences helps you grasp what being on a ventilator might really feel like.
Reported Memories And Dreams
Some patients recall strange dreams or fragmented memories while on a ventilator. These can include surreal images, noises, or feelings of floating. One patient described feeling like they were trapped underwater, struggling to breathe despite the machine’s assistance.
These memories often mix reality with imagination. Patients might remember voices or conversations in the room, even if they were unconscious. This raises the question: how much of what you experience is real, and how much is your mind trying to make sense of a confusing situation?
Cases Of Awareness During Ventilation
A few patients report moments of awareness while still on the ventilator. They might hear doctors talking or feel pain but be unable to respond. This can be frightening and isolating, as they are conscious but locked inside their own body.
These cases highlight the importance of clear communication and sedation management. If you or a loved one is on a ventilator, ask the medical team about sedation levels and what signs of awareness to watch for. Knowing this can help you advocate for comfort and dignity during a vulnerable time.
Risks Of Being Conscious
‘Risks of Being Conscious’ explores the anxiety and discomfort faced by ventilated patients. Consciousness on a ventilator can cause distress, leading to challenges in communication and emotional strain.
Being conscious while on a ventilator can be a complex experience, fraught with potential risks that can impact both your mind and body. Understanding these risks is crucial to managing the experience effectively if you or a loved one find yourselves in this situation. Being aware can mean different things, from feeling slight discomfort to experiencing significant distress.Psychological Impact
Being conscious on a ventilator can take a toll on your mental health. You might feel disoriented and confused about your surroundings, which can lead to feelings of fear and helplessness. Imagine being in a hospital room, hearing the hum of machines, and not fully understanding what’s happening—it’s enough to cause anxiety. Some people report feelings of paranoia and hallucinations, which can further amplify distress. It’s important to communicate any unusual experiences to your healthcare team. They can offer reassurance and possibly adjust your medication to ease these symptoms.Physical Discomfort And Anxiety
Physically, being conscious on a ventilator can be challenging. You might experience a dry mouth or throat irritation due to the tube, which can be uncomfortable. The feeling of being tethered to machines can also induce anxiety, as it limits your movement and independence. You may also feel shortness of breath if the ventilator settings aren’t perfectly aligned with your needs. It’s crucial to express any discomfort to the medical staff, as they can often make adjustments to improve your comfort. Have you ever found yourself in a similar situation where you felt physically restricted? How did you cope with the discomfort and anxiety? Your experiences and insights can make a difference in managing these challenges effectively.
Credit: www.healthysimulation.com
Monitoring Consciousness Levels
Monitoring consciousness levels in patients on ventilators is vital for their care. It helps medical staff understand the patient’s awareness and comfort. Knowing how alert or responsive a patient is guides treatment and adjustments to support.
Consciousness monitoring involves various tools and techniques. These tools track brain activity, responsiveness, and pain levels. Ensuring comfort reduces stress and aids recovery. Both aspects work together to improve patient outcomes.
Tools And Techniques
Doctors use specific tools to check consciousness in ventilated patients. One common tool is the Glasgow Coma Scale (GCS). It scores eye, verbal, and motor responses to stimuli. This score shows how awake or responsive a patient is.
Brain activity can also be monitored using EEG (electroencephalogram). EEG measures electrical signals in the brain. It helps detect changes in brain function and alertness.
Other methods include pupillary light reflex tests and sedation scales. Pupillary tests check how pupils react to light. Sedation scales help assess the depth of sedation or drowsiness.
Ensuring Patient Comfort
Comfort plays a big role in consciousness monitoring. A comfortable patient is easier to assess accurately. Nurses and doctors adjust ventilator settings to reduce discomfort.
Pain management is crucial. Caregivers use pain scales to detect and treat pain quickly. Proper pain control helps patients stay calm and responsive.
Regular checks and gentle care improve patient comfort. Soft bedding, quiet rooms, and calm voices help too. Comfort supports better healing and clearer consciousness signs.
Improving Patient Care On Ventilators
Improving patient care on ventilators requires a delicate balance between medical needs and the patient’s comfort and awareness. Care teams must focus on strategies that support both the physical and emotional well-being of those relying on ventilators. Paying attention to sedation levels and communication can transform the patient’s experience and recovery journey.
Balancing Sedation And Awareness
Finding the right sedation level is crucial. Too much sedation can leave patients feeling detached and confused once they wake up, while too little can cause distress or discomfort during ventilation.
Healthcare providers often adjust sedation based on the patient’s condition and responses. Asking yourself—how awake should a patient be to participate in their care without feeling pain or anxiety?—can guide these decisions.
In some cases, light sedation allows patients to remain partially aware, reducing confusion and aiding faster recovery. Monitoring vital signs and patient feedback helps ensure sedation stays within a safe, comfortable range.
Communication Methods For Patients
Being unable to speak can make ventilated patients feel isolated. Yet, simple communication tools can make a huge difference.
- Using picture boards or yes/no cards helps patients express basic needs and feelings.
- Technology like eye-tracking devices or simple writing tools can empower those who are more alert.
- Regular check-ins with clear, calm verbal explanations reduce anxiety and build trust.
Have you ever wondered how small gestures, like holding a patient’s hand or explaining each step of care, impact their mental state? These efforts often ease fear and foster a sense of control during a vulnerable time.
Frequently Asked Questions
Can Patients Be Conscious While On A Ventilator?
Yes, many patients remain conscious on a ventilator. Sedation levels vary based on medical needs. Consciousness depends on illness severity and treatment goals.
How Does A Ventilator Affect Brain Awareness?
A ventilator supports breathing but does not directly alter brain awareness. Sedatives or medications given with ventilation may impact consciousness levels.
Can Patients Communicate When On A Ventilator?
Some ventilated patients can communicate using eye movements or writing. Communication depends on sedation, ventilator type, and patient condition.
What Causes Unconsciousness During Ventilation?
Unconsciousness may result from sedation, illness severity, or brain injury. Ventilation itself does not cause unconsciousness but supports breathing.
Conclusion
Being conscious on a ventilator can feel confusing and scary. Many patients stay awake but need help to breathe. Doctors and nurses work hard to keep you safe and comfortable. Your mind may stay alert even when machines assist your breathing.
Understanding this helps reduce fear and builds trust in care. Always ask questions and share your feelings with your medical team. Staying informed brings peace during a tough time. Remember, you are not alone in this journey. Support is close, and recovery is possible.