Have you ever wondered if you can talk while using a trach ventilator? If you or someone you care about relies on this type of breathing support, you might feel unsure about what’s possible when it comes to speaking.
The good news is, communication isn’t always lost with a trach ventilator. Understanding how it works and what options you have can open the door to sharing your thoughts and feelings again. Keep reading to discover how you can regain your voice and connect with others, even while on a trach ventilator.
What Is A Trach Ventilator?
A trach ventilator helps people breathe when they cannot do so on their own. It connects to a tracheostomy tube, which is placed directly into the windpipe. This device supports or takes over the breathing process. Many patients use it in hospitals or at home for long-term care.
Understanding what a trach ventilator does is important for patients and caregivers. It can maintain oxygen levels and remove carbon dioxide from the body. The machine works by pushing air into the lungs through the tracheostomy tube.
How Does A Trach Ventilator Work?
The ventilator pushes air through the trach tube into the lungs. It controls the rate and depth of breaths. Sensors monitor oxygen and pressure levels. The machine adjusts to meet the patient’s breathing needs.
Who Needs A Trach Ventilator?
- People with lung diseases
- Patients after major surgery
- Individuals with spinal cord injuries
- Those with severe respiratory failure
Types Of Trach Ventilators
| Type | Description |
|---|---|
| Invasive Ventilators | Connected directly through the tracheostomy tube. |
| Non-Invasive Ventilators | Use masks, not tubes, but can be used with trachs in some cases. |
How Trach Ventilators Affect Speech
Understanding how a trach ventilator affects your ability to speak is crucial if you or a loved one uses one. Speaking involves more than just vocal cords; it depends on airflow and how the ventilator interacts with your airway. Let’s break down what happens and why speech can become challenging.
Impact On Vocal Cords
The vocal cords need air passing through them to produce sound. With a trach ventilator, air often bypasses the vocal cords because it flows directly through the tracheostomy tube. This means your vocal cords get less air, making it harder to speak or produce a normal voice.
Some people notice their voice sounds weak or breathy. Others may find they can only speak in short phrases before needing to take a breath. Have you tried simple breathing exercises to help strengthen your voice in this situation?
Role Of The Cuff
The cuff is a small balloon that surrounds the trach tube. When inflated, it seals the airway to prevent air leaks and helps with ventilation. However, this seal also stops air from reaching the vocal cords, which can silence your voice completely.
Deflating the cuff during speaking can allow air to flow over your vocal cords again. But this must be done carefully to avoid compromising your breathing or safety. Have you discussed cuff management options with your healthcare provider to find the best balance for your speech?
Airflow Changes
Normally, air travels from your lungs through the vocal cords, mouth, and nose to create speech sounds. A trach ventilator changes this airflow by directing it out through the tracheostomy tube instead. This shift means less air reaches the mouth and vocal cords, disrupting your ability to speak naturally.
Some devices, like speaking valves, redirect airflow back through your vocal cords. These can improve speech but require proper fitting and training. Have you explored speaking valve options or worked with a speech therapist to maximize your communication?
Methods To Enable Talking With A Trach
Talking with a trach ventilator can be challenging. Various methods help patients regain their voice. These techniques focus on allowing airflow through the vocal cords. The right approach depends on the patient’s condition and type of trach tube. Here are common ways to enable speech while using a trach ventilator.
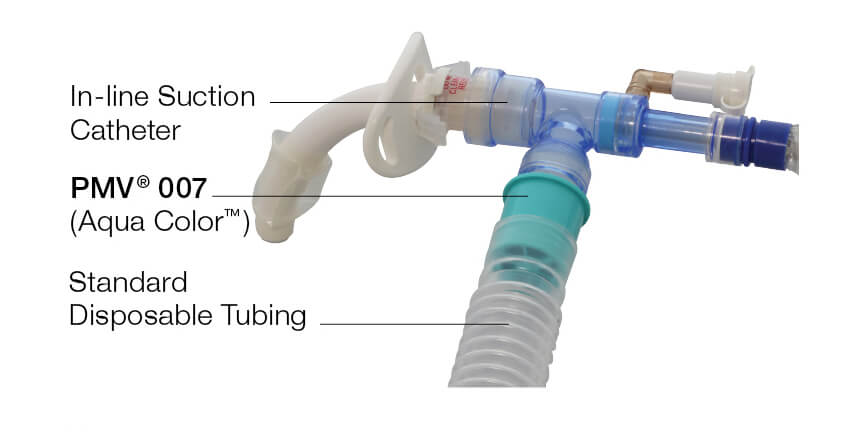
Speaking Valves
Speaking valves are small devices placed on the trach tube. They allow air to enter during inhalation but close during exhalation. This closure directs air through the vocal cords, producing sound. Speaking valves improve communication without removing the trach tube. Patients often find it easier to speak with these valves.
Cuff Deflation Technique
The cuff on a trach tube seals the airway to prevent air leaks. Deflating the cuff allows air to pass around the tube. This air flows through the vocal cords, enabling speech. Cuff deflation must be done carefully to avoid breathing issues. Medical staff usually assist with this technique to ensure safety.
Use Of Passy-muir Valve
The Passy-Muir valve is a popular type of speaking valve. It fits onto the trach tube and directs airflow over the vocal cords. This valve helps patients speak clearly and improves swallowing. It also supports lung health by promoting natural breathing patterns. Many healthcare providers recommend the Passy-Muir valve for talking with a trach.
Credit: tracheostomyeducation.com
Challenges In Speaking On A Trach Ventilator
Speaking while using a trach ventilator presents many challenges. The device helps with breathing but affects normal speech. Understanding these challenges helps in finding ways to communicate better. Speech is often limited by physical and emotional factors that come with the ventilator.
Physical Barriers
The trach tube sits in the windpipe, blocking air from passing through the vocal cords. Without air flow, the cords cannot vibrate to make sound. This makes normal speech very difficult or impossible. Some people use special valves or devices to help air reach the vocal cords.
Physical discomfort also affects speaking. The tube may cause irritation or dryness in the throat. Movement of the tube can lead to coughing or difficulty controlling voice. These factors limit the ability to speak clearly and comfortably.
Respiratory Limitations
Ventilators control breathing, so speech timing depends on machine settings. Many cannot hold breath long enough to form words properly. Speaking may tire the person quickly due to limited air supply.
The pressure from the ventilator sometimes affects voice strength. Soft or weak speech is common. Breathing patterns must be coordinated with talking, which is hard for many users.
Emotional Factors
Frustration often arises from being unable to speak freely. This can lead to anxiety or withdrawal from social interactions. Communication barriers may cause feelings of isolation or sadness.
Confidence in speaking may decrease over time. Users may avoid talking to reduce embarrassment or effort. Emotional support and patience are vital for improving communication.
Therapies To Improve Communication
Communication can be challenging for people using a trach ventilator. Therapies exist to help improve speaking abilities and interaction. These therapies focus on strengthening speech skills and using tools to aid communication. They support patients in expressing their needs and feelings more clearly.
Speech Therapy Approaches
Speech therapists work closely with trach patients to restore voice and speech. They use exercises to improve breath control and vocal cord function. Techniques include:
- Tracheoesophageal puncture training for voice production
- Breathing exercises to coordinate speech with ventilation
- Voice therapy to strengthen weak vocal muscles
- Swallowing therapy to prevent choking during speech
Therapists tailor plans to each patient’s needs. Regular sessions help increase confidence and clarity in speech.
Alternative Communication Tools
When speech is limited, other tools help patients express themselves. These devices and methods include:
- Communication boards with pictures or words
- Electronic speech-generating devices
- Tablet apps designed for easy typing or symbols
- Eye-tracking systems for patients with limited movement
These tools allow patients to share thoughts and make choices. They improve social interaction and reduce frustration.

Credit: tracheostomyeducation.com
Safety Tips When Talking With A Trach
Talking with a trach ventilator requires care. Ensure the trach tube is clean and secure. Use a speaking valve if possible, and practice slow, clear speech to avoid strain.
Talking with a trach ventilator requires special care and understanding. It’s essential to know safety tips to ensure effective and safe communication. Whether you are the patient or a caregiver, these guidelines can make conversations smoother and safer.Ensure Proper Humidification
Always check the humidification of the trach. Dry air can irritate the airway. This can lead to discomfort or complications. Use a humidifier if needed. This helps maintain moisture levels. It makes speaking easier and safer.Monitor For Signs Of Distress
Keep an eye on the person speaking. Look for any signs of distress. These include coughing, difficulty breathing, or changes in color. Stop the conversation if you notice any of these signs. Take appropriate action immediately.Use A Speaking Valve
Consider using a speaking valve. It helps in producing sound while talking. Ensure the valve is clean and functioning. This can enhance communication efficiency. Only use it if the healthcare provider recommends it.Maintain Cleanliness Of The Trach
Regularly clean the trach area. This prevents infections and ensures safety. Use the recommended cleaning solutions. Follow the care routine as advised by healthcare professionals.Practice Gentle Communication Techniques
Speak slowly and clearly. Give time for responses. Use simple words and short sentences. Encourage the person to rest if needed. This reduces strain on the voice and airway.Provide Adequate Support
Offer physical and emotional support. Be patient and understanding. Create a comfortable environment. It helps reduce anxiety and promotes better communication.Consult Healthcare Professionals
Always consult with healthcare providers. Follow their guidelines for trach care and communication. They can offer tailored advice and solutions. This ensures the well-being of the person using the trach.Real-life Experiences From Trach Users
Hearing directly from people who use trach ventilators can give you clear insight into what it’s really like to communicate while managing breathing support. These users often share practical tips and unexpected challenges that help you understand the day-to-day reality beyond medical descriptions.
How Users Adapt Their Speech Techniques
Many trach users find creative ways to speak despite the ventilator’s restrictions. Some use speaking valves, which redirect airflow to the vocal cords, allowing natural speech. Others rely on whispering or short phrases to conserve energy and reduce breathlessness.
One user mentioned how practicing simple words daily helped regain confidence. Could small, consistent efforts improve your own communication?
Challenges Faced During Conversations
Communication isn’t always smooth. Background noise and fatigue often make speaking harder. Users report needing to pause frequently and use gestures or writing to fill in gaps.
Imagine trying to explain something important when your voice fades quickly—how would you prepare for that?
Emotional Impact Of Limited Speech
Some users share feelings of frustration or isolation when they can’t easily express themselves. But many also describe moments of joy when they successfully communicate, even if briefly.
These experiences highlight the value of patience from both users and their listeners. How do you think empathy changes the way you communicate?
Tools And Devices That Help Communication
- Speaking valves attached to the trach tube
- Text-to-speech apps on smartphones
- Picture boards or written notes
One individual found that combining a speaking valve with a tablet app made conversations much easier. What simple tool could make your communication smoother?
Credit: tracheostomyeducation.com
Frequently Asked Questions
Can You Speak With A Trach Ventilator?
Yes, some patients can speak with a trach ventilator using specialized speaking valves. These valves allow air to pass over the vocal cords, enabling speech. However, speech ability depends on the ventilator settings and the patient’s condition.
How Does A Speaking Valve Work With A Trach?
A speaking valve redirects airflow through the vocal cords when exhaling. It fits onto the trach tube and lets air enter but not escape, allowing sound production. This helps patients communicate verbally while on a ventilator.
What Are Common Challenges Talking With A Trach Ventilator?
Speaking with a trach ventilator can be difficult due to airflow restrictions. Patients may feel breathless or tired when using speaking valves. Proper medical guidance and therapy can improve speech ability and comfort.
Is It Safe To Use A Speaking Valve On A Ventilator?
Yes, speaking valves are safe when used under medical supervision. Healthcare providers assess suitability based on ventilator settings and patient health. Incorrect use can cause breathing difficulties, so professional guidance is crucial.
Conclusion
Talking with a trach ventilator is possible for many people. It may need some tools or therapy to help. Every person’s situation is different, so doctors guide the best way. Patience and practice often improve communication skills. Support from family and caregivers also plays a big role.
Understanding this helps reduce fear and frustration. Clear speech can happen, even with a trach ventilator. Keep hope and stay positive through the process. Small steps lead to better talking over time.