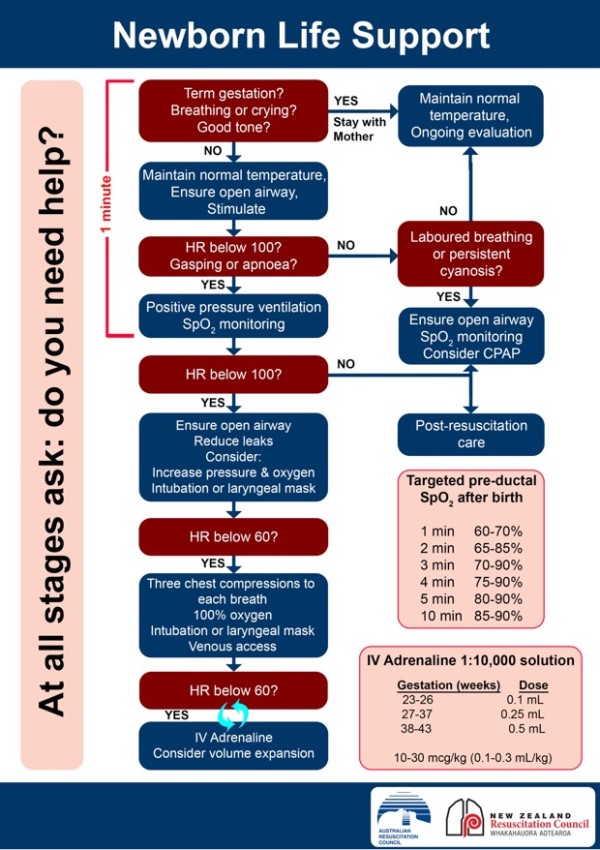
When you’re providing positive pressure ventilation (PPV) during newborn resuscitation, knowing the correct ventilation rate is crucial. Your actions can make a life-saving difference, but getting the timing wrong might reduce the effectiveness of your efforts.
Are you confident you’re delivering breaths at the right speed? Understanding the correct ventilation rate in neonatal resuscitation protocols (NRP) isn’t just a guideline—it’s a key step in giving your little patient the best start possible. Keep reading to discover exactly how to get it right and why it matters so much.
Basics Of Ppv In Nrp
Positive Pressure Ventilation (PPV) is a key skill in Neonatal Resuscitation Program (NRP). It supports newborns who struggle to breathe at birth. Understanding the basics helps caregivers deliver the right care quickly and effectively. Proper ventilation rate and technique improve newborn outcomes. This section explains what PPV is, its role, and when to start it.
What Is Positive Pressure Ventilation
Positive Pressure Ventilation means pushing air into a baby’s lungs. It helps open the airways and improves oxygen flow. Healthcare providers use a bag and mask or a device to deliver air. This support mimics the baby’s natural breathing effort. PPV is gentle but effective in stabilizing breathing.
Role Of Ppv In Neonatal Resuscitation
PPV is critical when newborns do not breathe or cry after birth. It helps clear fluid from the lungs and starts oxygen exchange. Using PPV can prevent brain damage caused by low oxygen. It gives the baby time to begin normal breathing. PPV is often the first step in resuscitation.
When To Initiate Ppv
Start PPV if the baby is not breathing or gasping. Also, if the heart rate is below 100 beats per minute, begin PPV. Check breathing and heart rate within the first minute after birth. Quick action is vital to support the baby’s survival. Use gentle breaths at a proper rate to avoid lung injury.

Credit: quizlet.com
Determining The Correct Ventilation Rate
Determining the correct ventilation rate during Positive Pressure Ventilation (PPV) in neonatal resuscitation is crucial for effective support. The right rate ensures adequate oxygen delivery while minimizing potential lung injury. Let’s break down how to identify and adjust this rate based on newborn needs and clinical signs.
Recommended Ventilation Rates For Newborns
The Neonatal Resuscitation Program (NRP) advises a ventilation rate of about 40 to 60 breaths per minutefor newborns requiring PPV. This rate strikes a balance between providing enough breaths to oxygenate and avoiding excessive pressure or volume.
Maintaining this rate means delivering approximately one breath every second, which feels rapid but is necessary to meet the newborn’s oxygen demands during critical moments. Are you confident you can keep this pace steady during resuscitation? Practicing with a timer or metronome can help maintain consistency.
Factors Influencing Ventilation Rate
Several factors affect how you should set the ventilation rate for a newborn:
- Gestational age:Preterm infants often need gentler ventilation with careful rate adjustment due to fragile lungs.
- Birth condition:A newborn with meconium-stained fluid or airway obstruction may require modified rates or techniques.
- Heart rate response:A slow or irregular heart rate may signal the need to reassess ventilation speed and effectiveness.
Understanding these variables helps you tailor your approach rather than sticking rigidly to a single rate. Have you noticed how subtle changes in a baby’s condition can affect your ventilation decisions?
Adjusting Rate Based On Clinical Response
Watch the newborn’s chest rise as your primary visual cue. Adequate chest movement usually means your rate and volume are appropriate. If the chest doesn’t rise well, increasing the rate slightly or checking mask fit can improve ventilation.
Monitor the heart rate continuously. If it remains below 100 beats per minute, consider adjusting your ventilation technique or rate. Sometimes slowing down breaths allows more time for lung inflation and better oxygen exchange.
Remember, ventilation is dynamic. Your ability to read and respond to the newborn’s immediate feedback can make a life-saving difference. How often do you pause to reassess and adjust during PPV?
Techniques For Effective Ventilation
Effective ventilation techniques ensure proper breathing support during PPV. They are crucial for patient safety and recovery. Knowing the right methods helps in delivering optimal care.
Proper Mask Placement And Seal
A correct mask fit is essential for effective ventilation. Place the mask over the nose and mouth. Ensure it covers both areas without gaps. Use two fingers on the chin to hold the mask. This helps in keeping a tight seal. A proper seal prevents air leakage during ventilation. Adjust the mask if you see any air escaping. A good seal ensures the air goes into the lungs.
Optimal Pressure Settings
Adjust pressure settings to match patient needs. Start with the lowest effective pressure. Increase gradually if needed. Monitor the patient’s response closely. Too high pressure can cause lung damage. Too low pressure may not ventilate the lungs properly. Use manometers to measure pressure accurately. Keep pressure within safe limits.
Monitoring Chest Rise
Observe the chest for adequate rise during ventilation. A visible rise indicates proper air entry into the lungs. No chest rise may mean inadequate ventilation or mask seal issues. Adjust mask placement and pressure if needed. Consistent chest rise ensures effective ventilation. This confirms air is reaching the lungs efficiently.

Credit: www.studocu.com
Common Challenges And Solutions
Providing positive pressure ventilation (PPV) requires careful attention to several common challenges. These challenges can affect the ventilation rate and overall effectiveness. Identifying and solving these issues quickly ensures better outcomes for newborns in need of resuscitation. The following sections cover frequent problems and practical solutions.
Addressing Mask Leak
Mask leak reduces the amount of air delivered to the lungs. It happens when the mask does not fit tightly on the face. Check the mask size and position carefully. Use gentle pressure with your hand to hold the mask firmly. Avoid pressing too hard as this can cause injury. Reposition the mask if you see air escaping. Look for chest rise to confirm effective ventilation.
Managing Airway Obstruction
Airway obstruction can block airflow despite correct ventilation rate. Common causes include a blocked nose or tongue falling back. Open the airway by tilting the head slightly back. Use a jaw thrust to lift the chin forward. Clear the mouth and nose of any secretions or debris. Suction gently if needed to keep the airway clear. Watch for signs of obstruction like no chest movement.
Recognizing And Correcting Inadequate Ventilation
Inadequate ventilation means the lungs do not receive enough air. Signs include a weak or absent chest rise. Check for mask leaks and airway blockages first. Confirm the ventilation rate matches neonatal resuscitation program (NRP) guidelines. Adjust pressure and volume carefully. Use a metronome or timer to keep a steady rate. Monitor the baby’s heart rate and oxygen levels. Adjust ventilation based on these vital signs.
Monitoring And Assessment During Ppv
Monitoring and assessment are vital during positive pressure ventilation (PPV). They help ensure the baby receives the right ventilation rate and support. Careful observation allows quick adjustments. This improves the chance of a good outcome. Continuous monitoring helps detect problems early and guides clinical decisions.
Using Pulse Oximetry
Pulse oximetry measures oxygen levels in the blood. It provides real-time feedback on oxygen delivery. The sensor attaches to the baby’s hand or foot. Watch for oxygen saturation levels between 90% and 95%. This range indicates effective oxygenation without causing damage. Low saturation suggests the need to adjust ventilation. High levels may require reducing oxygen concentration.
Heart Rate Assessment
Heart rate is the best immediate sign of ventilation success. Check the pulse after each ventilation cycle. A heart rate above 100 beats per minute shows good response. If it remains under 60, increase ventilation efforts. Use a stethoscope or palpate the umbilical cord. Rapid, steady heart rate rise means improved circulation and oxygenation.
Signs Of Effective Ventilation
Look for chest rise with each ventilation. It shows air enters the lungs. Listen for breath sounds on both sides. Equal sounds mean proper lung inflation. Monitor skin color for pinkness, indicating good oxygen levels. Watch for reduced respiratory effort or crying. These signs confirm that ventilation meets the baby’s needs.

Credit: www.pediatric.theclinics.com
Updates And Guidelines In Nrp
The Neonatal Resuscitation Program (NRP) regularly updates its guidelines to improve newborn care. These updates reflect new research and clinical findings. Staying informed about ventilation rate recommendations is vital for healthcare providers. Accurate ventilation rates during Positive Pressure Ventilation (PPV) can save newborn lives and reduce complications.
Recent Changes In Ventilation Recommendations
NRP recently revised the recommended ventilation rates for newborns. The current guideline suggests a rate of 40 to 60 breaths per minute during PPV. This range aims to optimize oxygen delivery and lung inflation. Earlier guidelines allowed a wider range but lacked precision.
The changes focus on improving the timing and pressure of breaths. Providers should deliver slow, gentle breaths to avoid lung injury. The new recommendations also emphasize monitoring chest rise for effective ventilation.
Evidence Supporting Current Practices
Studies show that 40 to 60 breaths per minute improve newborn outcomes. Research highlights better oxygenation and less lung trauma with this rate. Controlled ventilation reduces the risk of brain injury and other complications.
Clinical trials confirm that following updated NRP guidelines leads to faster recovery. The evidence supports gentle, consistent breaths over rapid or forceful ventilation. Training programs now focus on teaching these best practices to healthcare workers.
Frequently Asked Questions
What Is The Correct Ventilation Rate For Ppv In Nrp?
The recommended ventilation rate for PPV in NRP is 40 to 60 breaths per minute. This rate ensures effective lung inflation and oxygen delivery for newborns needing respiratory support.
How Does Ventilation Rate Affect Newborn Resuscitation?
Proper ventilation rate maintains adequate oxygenation and prevents lung injury. Too fast or too slow rates can cause inadequate gas exchange or barotrauma.
Why Is 40-60 Breaths Per Minute Ideal In Nrp Ppv?
This range balances sufficient ventilation with the newborn’s lung capacity. It supports effective oxygenation without causing damage from over-ventilation.
Can Ventilation Rate Vary Based On Newborn Condition?
Yes, ventilation rates may adjust based on heart rate and chest rise. Clinicians monitor these signs to optimize ventilation during resuscitation.
Conclusion
Providing the correct ventilation rate during PPV is vital for patient safety. The NRP guidelines help ensure proper breaths per minute. Too fast or too slow can harm the baby. Always follow the recommended rate to support healthy breathing. Clear, steady breaths make a difference.
Keep practicing to build confidence and skill. Proper ventilation helps newborns start life strong. Simple steps lead to better outcomes.