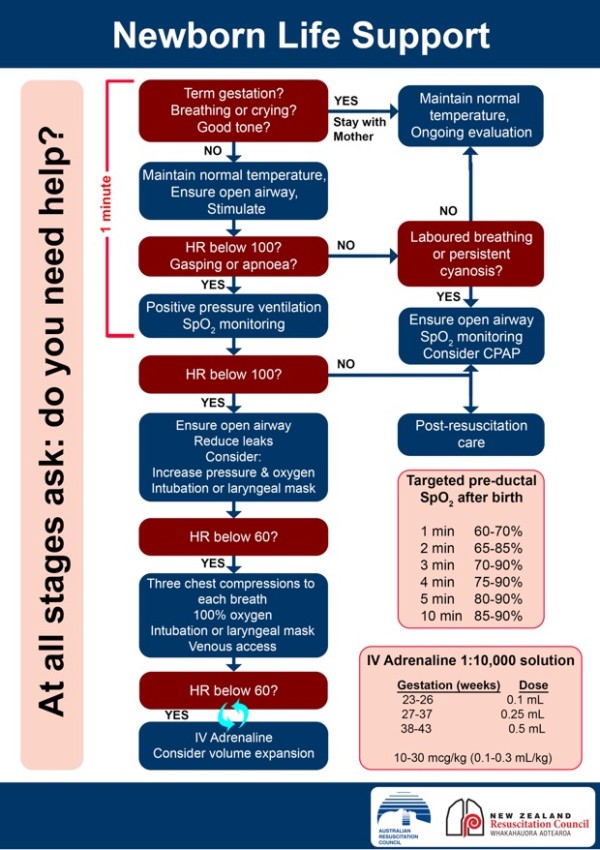
When providing positive pressure ventilation to a term newborn, every second counts. You want to make sure your baby gets the best start possible, but it can feel overwhelming if you’re not sure what steps to take.
This guide is here to help you understand exactly what you need to do, why it matters, and how to do it safely and effectively. By the time you finish reading, you’ll feel confident and ready to act with calm and precision.
Keep reading—your newborn’s breath depends on it.
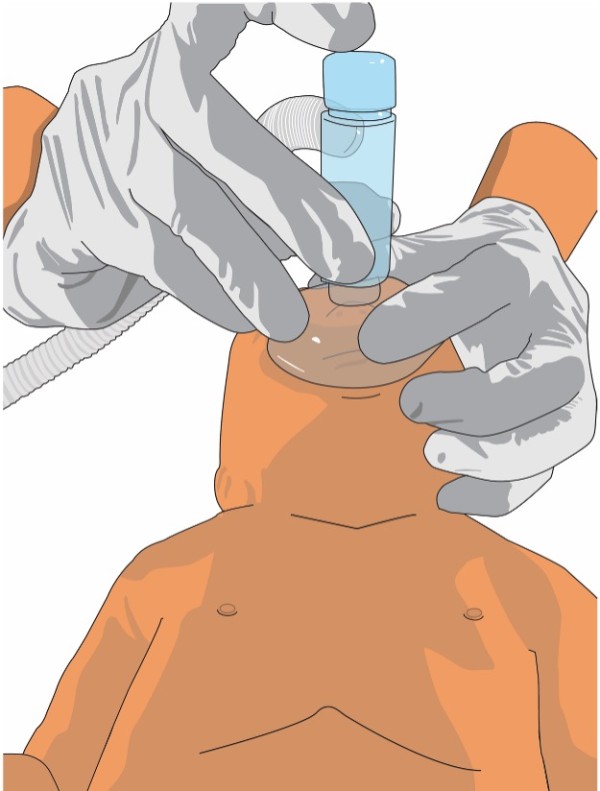
Credit: www.anzcor.org
Preparing For Ventilation
Preparing for positive pressure ventilation in a term newborn requires careful planning. The process ensures the newborn receives proper support immediately after birth. Quick and precise actions improve the baby’s chance of breathing well on their own.
Equipment Check
All equipment must be ready and working before birth. Check the bag and mask for leaks or damage. Ensure the oxygen source is connected and functioning. Have suction devices nearby to clear airways if needed. Keep a pulse oximeter ready to monitor oxygen levels.
Team Coordination
The team must understand their roles clearly. Assign tasks like airway management and monitoring vital signs. Communicate using simple and direct language. Practice calm and steady movements to avoid delays. Prepare to adjust roles quickly if the situation changes.
Assessing The Newborn
Observe the newborn’s breathing effort and heart rate right after birth. Look for signs of distress like weak breathing or low heart rate. Check muscle tone and skin color to gauge health. Use this information to decide if ventilation is necessary. Act promptly to provide support when needed.
Starting Positive Pressure Ventilation
Starting positive pressure ventilation (PPV) is crucial for helping a term newborn breathe effectively. This process supports the baby’s lungs to open and deliver oxygen. Quick and correct action can prevent complications and improve the baby’s condition.
Successful ventilation depends on three key factors: proper mask placement, setting the right ventilation parameters, and ensuring an effective seal. Each step requires careful attention to detail to support the newborn’s breathing.
Proper Mask Placement
Place the mask gently over the baby’s nose and mouth. The mask should cover both areas completely without pressing too hard. Avoid covering the eyes or pushing the chin down. Keep the baby’s head in a neutral position to open the airway.
Setting Ventilation Parameters
Start with a pressure of 20 to 25 cm H2O for each breath. Set the rate at 40 to 60 breaths per minute. Use a gentle, steady rhythm to mimic natural breathing. Monitor the baby’s chest rise to adjust pressure if needed.
Ensuring Effective Seal
Hold the mask firmly but softly against the face. Check for air leaks around the edges of the mask. A good seal ensures air goes into the lungs, not out. Adjust hand position or mask size to fix leaks quickly.
Monitoring During Ventilation
Monitoring during positive pressure ventilation is essential to ensure that a term newborn receives the right support for effective breathing. Without careful observation, you might miss signs that indicate whether the ventilation is helping or causing stress. Paying close attention to key indicators can guide you in adjusting your technique and improving the newborn’s chances of a smooth transition to independent breathing.
Observing Chest Movement
Watch the newborn’s chest closely as you provide ventilation. The chest should rise gently and symmetrically with each breath you give. If you notice uneven or minimal chest movement, it might mean the mask seal isn’t tight or the pressure is too low.
Have you ever felt uncertain if your ventilation was effective? Visual cues like chest rise give immediate feedback. Adjust your hand position or pressure until the chest moves appropriately to ensure air is reaching the lungs.
Checking Heart Rate
Heart rate is a critical sign of how well the newborn is responding to ventilation. You should check the heart rate within the first 30 seconds of starting ventilation. A rising heart rate generally means the baby is improving; a rate below 100 beats per minute suggests you need to continue or adjust your efforts.
Use a stethoscope or palpate the base of the umbilical cord if you’re in an emergency. Quick, accurate heart rate assessment can guide you in deciding whether to increase ventilation pressure or seek additional help.
Assessing Oxygenation
Oxygen saturation monitors can give you real-time data about how well oxygen is reaching the baby’s blood. Place the sensor on the right hand or wrist for the most reliable reading. You should look for a gradual increase in saturation, aiming for levels above 90% within the first 10 minutes.
Don’t rely solely on equipment—combine the readings with clinical signs like skin color and activity. If oxygenation remains low despite proper ventilation, it might signal underlying problems needing urgent attention.
Troubleshooting Common Issues
Troubleshooting common issues during positive pressure ventilation (PPV) in term newborns is crucial for effective resuscitation. You need to quickly identify and resolve problems to ensure the baby receives adequate oxygen. Knowing what to look for and how to respond can make a significant difference in outcomes.
Managing Airway Obstruction
Airway obstruction is a frequent challenge during PPV. If you notice poor chest rise despite proper mask placement, check for blockages like the tongue or secretions. Gently reposition the head into a neutral or slightly extended position to open the airway.
Sometimes suctioning the mouth and nose clears the obstruction. Avoid excessive force with the mask, as this can worsen the blockage. Have a suction device ready and be prepared to switch to a more advanced airway if needed.
Adjusting Ventilation Technique
Proper ventilation technique is key to effective PPV. If the newborn’s chest doesn’t rise, try adjusting the mask seal or repositioning the head. Ensure you deliver slow, steady breaths rather than rapid puffs.
Watch the baby’s response closely. If oxygen saturation doesn’t improve, consider increasing the pressure slightly but avoid overventilation. Have you observed how subtle changes in your technique can instantly improve chest movement?
When To Escalate Support
If your efforts don’t improve the newborn’s condition quickly, be ready to escalate support. This may involve inserting an endotracheal tube or using a T-piece resuscitator for more controlled ventilation.
Continuous monitoring is essential—assess heart rate, color, and breathing effort. If the heart rate remains below 60 beats per minute despite effective ventilation, initiate chest compressions and seek advanced help immediately.
Post-ventilation Care
Carefully monitor the newborn’s breathing and heart rate after positive pressure ventilation. Keep the baby warm and watch for any signs of distress or complications. Regularly check oxygen levels to ensure proper recovery.
Post-ventilation care for term newborns is crucial in ensuring a smooth transition to independent breathing. After the immediate concerns of positive pressure ventilation (PPV) are addressed, attention shifts to supporting the newborn’s respiratory and overall health. This stage requires careful management and attention to detail to avoid complications and promote optimal recovery.Weaning From Ventilation
Weaning a newborn from ventilation involves gradually reducing the support as the baby shows signs of respiratory improvement. It’s essential to monitor the baby’s effort and oxygen levels closely. Have you noticed how some newborns seem to thrive when given the chance to breathe on their own? This is the goal, but it requires patience and precise timing. Adjust the ventilator settings incrementally, allowing the newborn to take on more responsibility for their breathing. Health professionals often use a step-down approach, where support is reduced in stages. This gradual process helps to prevent the newborn from becoming overwhelmed.Ongoing Monitoring
Continuous monitoring is crucial once the newborn begins the weaning process. Pay close attention to vital signs such as heart rate, respiratory rate, and oxygen saturation. Are the values within the expected range? This ongoing assessment helps detect any signs of distress or fatigue early on. Utilize advanced monitoring equipment when available to provide real-time data. This information aids in making informed decisions about the newborn’s readiness to reduce or discontinue ventilation support.Documentation And Reporting
Accurate documentation and reporting are vital components of post-ventilation care. Record every change in ventilator settings and the baby’s response. This information provides a comprehensive view of the newborn’s progress and can be invaluable during follow-up care. Effective communication among the healthcare team ensures everyone is on the same page regarding the newborn’s condition and care plan. Have you ever considered how a single piece of overlooked information can impact patient care? Meticulous documentation helps avoid such pitfalls and promotes a collaborative approach to care.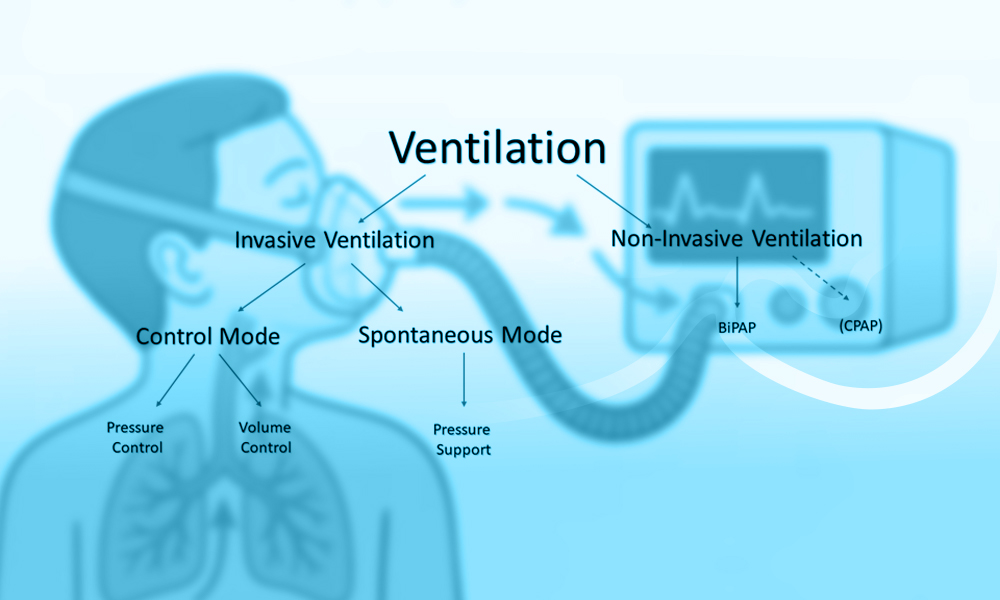
Credit: www.biosysmed.com
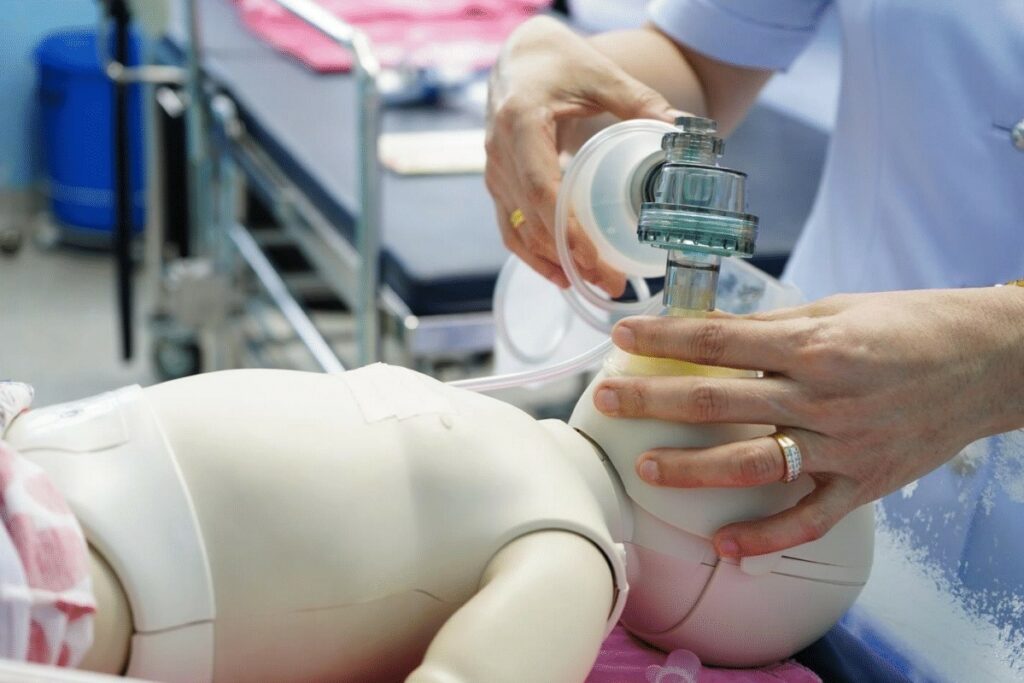
Credit: aclscertification.org
Frequently Asked Questions
What Is Positive Pressure Ventilation In Newborns?
Positive pressure ventilation (PPV) helps newborns breathe by delivering air through a mask. It supports lung inflation when spontaneous breathing is weak or absent. PPV is crucial during resuscitation to ensure oxygen reaches the lungs effectively.
When Should Ppv Be Started For A Term Newborn?
Start PPV if the newborn shows no breathing or weak breathing after birth. Also initiate if the heart rate is below 100 beats per minute. Early intervention improves oxygen delivery and prevents complications.
How To Properly Deliver Ppv To A Term Newborn?
Use a correctly sized mask and ensure a good seal on the face. Deliver breaths at 40-60 per minute with gentle pressure to avoid lung injury. Monitor chest rise to confirm effective ventilation.
What Are Common Complications Of Ppv In Newborns?
Overventilation may cause lung injury or air leaks like pneumothorax. Inadequate ventilation can lead to low oxygen levels and brain damage. Proper technique and monitoring reduce these risks.
Conclusion
Providing positive pressure ventilation to a term newborn requires care and attention. Always check the baby’s chest rise to ensure effective breaths. Use gentle pressure to avoid lung injury. Stay calm and act quickly to support breathing. Training and practice improve your confidence and skills.
Remember, every second counts to help the newborn breathe well. Safe and proper ventilation can save lives and promote healthy starts. Keep learning and stay prepared for these critical moments.