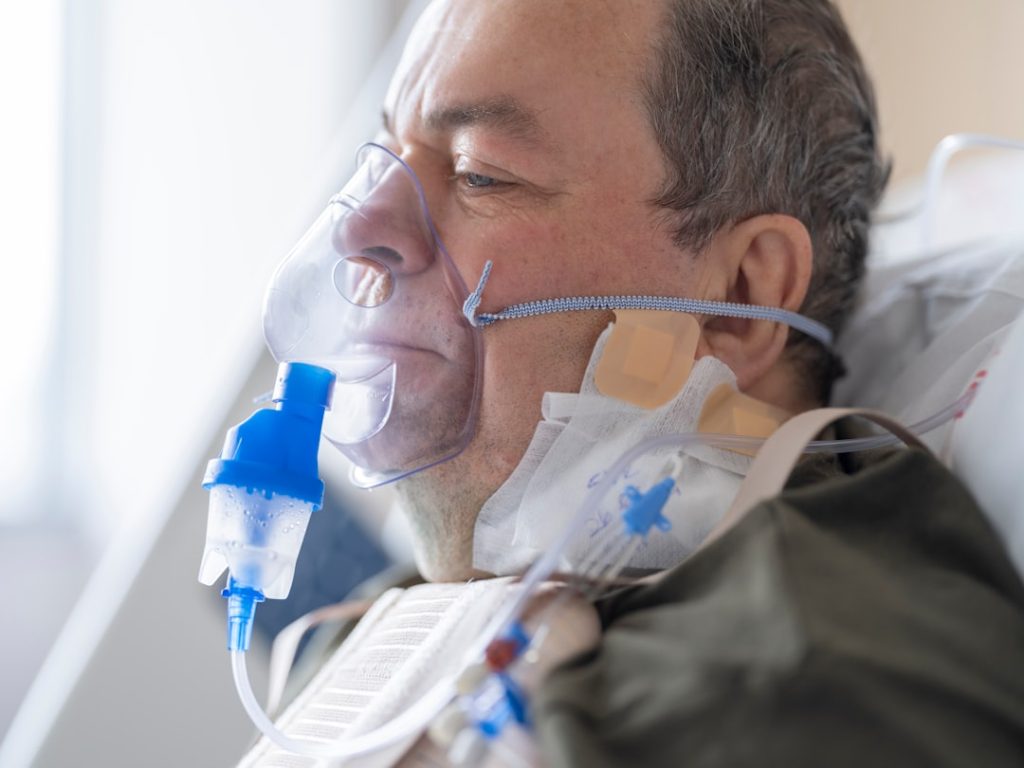
If you or a loved one is on a ventilator, you need to know how to prevent ventilator-associated pneumonia (VAP). This serious infection can happen quickly and make recovery much harder.
But here’s the good news: there are simple, effective steps you can take to lower the risk. You’ll learn exactly what causes VAP and how you can protect yourself or someone you care about. Don’t wait—understanding these life-saving tips could make all the difference.
Keep reading to take control of your health and safety.

Credit: www.bjaed.org
Causes Of Ventilator Associated Pneumonia
Understanding the causes of Ventilator Associated Pneumonia (VAP) is crucial to preventing it effectively. VAP develops in patients who are on mechanical ventilation, typically in intensive care units. Identifying what triggers this infection helps you take targeted actions to reduce the risk and improve patient outcomes.
Role Of Mechanical Ventilation
Mechanical ventilation supports breathing but can also introduce bacteria into the lungs. The ventilator tube bypasses natural defenses like coughing and mucous clearance, allowing germs to settle in the lower respiratory tract.
Secretions can pool above the tube cuff and drip into the lungs, creating an ideal environment for infection. Have you noticed how even a small leak or improper tube placement can increase contamination risk? This highlights why careful management of the ventilator is essential.
Common Risk Factors
- Prolonged Ventilation:The longer a patient stays on a ventilator, the higher the chance of infection.
- Poor Oral Hygiene:Bacteria from the mouth can travel down the airway and cause pneumonia.
- Underlying Health Conditions:Conditions like diabetes or weakened immunity make infection more likely.
- Use of Sedatives:Sedation reduces cough reflex and clearance of secretions.
- Improper Suctioning Techniques:If suctioning is not done correctly, it can introduce pathogens.
Addressing these risk factors means you can directly impact the chances of VAP developing. What small changes in care routines could reduce these risks in your setting? Sometimes, the answers lie in consistent attention to the details that matter most.
Hygiene Practices In Icu
Hygiene practices in the ICU are essential to prevent ventilator-associated pneumonia. Cleanliness reduces the risk of infection. Strict hygiene protocols protect both patients and staff.
Hand Hygiene Protocols
Hand hygiene is the first line of defense in infection control. Healthcare workers must wash hands before and after patient contact. Use alcohol-based hand rubs or soap and water. Nails should be short and clean. Avoid wearing rings or bracelets that can harbor germs. Hand hygiene stations must be easily accessible in the ICU. Regular training helps staff follow proper handwashing techniques.
Equipment Sterilization
All ventilator equipment must be thoroughly sterilized. Use approved disinfectants to clean reusable parts. Single-use items should be discarded after use. Store sterilized equipment in clean, dry areas. Check sterilization processes regularly to ensure effectiveness. Proper sterilization prevents bacteria from spreading through devices. Staff should wear gloves when handling equipment to maintain cleanliness.
Patient Positioning Strategies
Patient positioning plays a crucial role in preventing ventilator-associated pneumonia (VAP). Proper positioning helps reduce the risk of secretions entering the lungs, which can lead to infection. Let’s focus on two key strategies that you can apply right away to protect your patients.
Elevating The Head Of Bed
Raising the head of the bed between 30 and 45 degrees is a simple yet powerful way to prevent VAP. This position helps minimize the risk of aspiration by keeping stomach contents from flowing back into the lungs.
Healthcare workers often overlook this small adjustment, but it makes a big difference. Ask yourself: Are you consistently checking and maintaining this angle throughout the day? Even brief lapses can increase the risk of pneumonia.
Avoiding Supine Position
Lying flat on the back, or the supine position, increases the chance of lung infection in ventilated patients. This position allows secretions and gastric contents to pool and potentially be inhaled.
Encourage turning patients to their side or elevating their upper body instead. Have you noticed how patients tolerate these positions better than you expected? Comfort and safety can go hand in hand when you pay attention to positioning.

Credit: pharmeasy.in
Oral Care Techniques
Oral care plays a key role in preventing ventilator-associated pneumonia (VAP). Keeping the mouth clean reduces harmful bacteria that cause lung infections. Effective oral care techniques help protect patients on ventilators from dangerous complications.
Regular Oral Hygiene
Regular oral hygiene lowers bacterial growth in the mouth. Cleaning the teeth, gums, and tongue removes plaque and debris. Use a soft toothbrush or foam swabs to clean gently. Perform oral care at least twice daily. Moisturize the mouth to prevent dryness, which encourages bacteria. Check for any sores or inflammation to address problems early.
Use Of Antiseptic Mouthwashes
Antiseptic mouthwashes reduce germs that cause pneumonia. Chlorhexidine is a common choice for patients on ventilators. It kills bacteria in the mouth and throat quickly. Use mouthwash as part of the daily oral care routine. Follow the doctor’s instructions for correct concentration and frequency. Avoid overuse to prevent irritation or resistance.
Ventilator Circuit Management
Proper ventilator circuit management reduces the risk of infection by keeping tubes clean and dry. Regularly changing circuits and using sterile techniques help prevent pneumonia in ventilated patients. Careful handling minimizes harmful germs entering the lungs.
Ventilator Circuit Management is a critical aspect of preventing Ventilator Associated Pneumonia (VAP). Proper management of the ventilator circuit can significantly reduce the risk of infection in patients. This involves careful attention to routine practices and protocols designed to maintain a sterile environment and minimize potential contamination.Routine Circuit Changes
Regularly changing the ventilator circuit is essential to minimize infection risks. The timing of these changes should be based on clinical guidelines rather than arbitrary schedules. For example, only change the circuit when visibly soiled or malfunctioning. This approach reduces the chances of introducing pathogens into the system. Hospitals often have different protocols, but the goal remains the same: prevent unnecessary exposure. Are you following your facility’s guidelines for routine circuit changes? Ensuring adherence to these guidelines can make a significant difference.Minimizing Circuit Disconnections
Every disconnection of the ventilator circuit can increase the risk of contamination. Limiting the frequency of these disconnections is crucial. This involves planning ahead to address potential needs without unnecessary interruptions. Consider scenarios where adjustments might be needed and plan accordingly. This proactive approach can help maintain a closed system, reducing the risk of introducing harmful pathogens. Have you ever thought about how each disconnection could potentially impact patient safety? By focusing on these aspects of ventilator circuit management, you can contribute to a safer environment for patients. Implementing these practices not only aligns with best practices but also empowers you to take an active role in preventing VAP.Sedation And Weaning Protocols
Sedation and weaning protocols play a crucial role in preventing ventilator-associated pneumonia (VAP). Managing sedation carefully and promoting timely weaning from mechanical ventilation can reduce complications and improve patient outcomes. Let’s dive into how adjusting sedation and moving patients off ventilators early can make a difference.
Reducing Sedation Levels
Keeping sedation levels as low as possible helps your patient stay alert and responsive. Over-sedation can suppress cough reflexes and slow breathing, increasing the risk of pneumonia.
Try daily sedation interruptions or light sedation strategies. These allow you to assess the patient’s readiness to breathe on their own while minimizing drug effects. You might notice patients who are less sedated clear their lungs more effectively and have fewer infections.
Have you considered how sedation impacts your patient’s ability to protect their airway? Reducing sedation helps maintain natural defenses against lung infections.
Early Weaning From Ventilation
Moving patients off the ventilator as soon as safely possible is key to preventing VAP. The longer a patient stays intubated, the higher their risk of developing pneumonia.
Use weaning protocols that include regular assessments of breathing strength and readiness. This might involve spontaneous breathing trials or gradual reduction of ventilator support. Early extubation not only lowers infection risk but also shortens ICU stays.
Ask yourself: Is there a clear plan to evaluate when your patient can breathe independently? Early weaning depends on timely decisions and close monitoring.
Use Of Antibiotic Stewardship
Antibiotic stewardship plays a crucial role in preventing ventilator-associated pneumonia (VAP). It means using antibiotics wisely to treat infections without causing harm. Misusing antibiotics can lead to resistant bacteria, making infections harder to treat and increasing risks for patients on ventilators.
Preventing Antibiotic Resistance
Antibiotic resistance happens when bacteria change and no longer respond to medicines. This makes infections like VAP more dangerous. You can help stop this by avoiding unnecessary antibiotics and sticking to the right dose and duration.
Think about a patient I worked with who had a lung infection. The team chose a targeted antibiotic based on lab tests instead of broad-spectrum drugs. This approach not only cured the infection but also reduced the chance of resistant bacteria developing.
Appropriate Antibiotic Use
Using antibiotics correctly means selecting the right drug, dose, and treatment length. Start treatment based on culture results when possible, not just symptoms. This ensures the medicine fights the specific bacteria causing the infection.
- Review antibiotic therapy regularly and stop it when no longer needed.
- Educate healthcare staff about guidelines for antibiotic use in ventilated patients.
- Monitor patient response to adjust treatment quickly if necessary.
Could your healthcare team improve how they use antibiotics? Small changes in prescribing habits can save lives and keep antibiotics effective for everyone.

Credit: www.liebertpub.com
Staff Training And Awareness
Staff training and awareness are crucial in preventing ventilator-associated pneumonia (VAP). Educating healthcare teams helps reduce infection risks. Proper knowledge ensures effective infection control practices. Understanding the importance of hygiene and protocols is vital. Staff training and awareness empower teams to protect patients.
Regular Education Sessions
Regular education sessions are essential for healthcare staff. These sessions provide up-to-date information on VAP prevention. They focus on hygiene practices and equipment management. Interactive workshops engage staff, enhancing learning and retention. Regular training ensures the team remains informed and vigilant.
Monitoring Compliance
Monitoring compliance with protocols is key to reducing VAP risks. Regular audits help identify areas needing improvement. Compliance checks ensure staff follows best practices consistently. Feedback from audits guides further training needs. Monitoring ensures a high standard of patient care is maintained.
Frequently Asked Questions
What Is Ventilator-associated Pneumonia (vap)?
Ventilator-associated pneumonia is a lung infection occurring in patients using mechanical ventilation. It develops 48 hours or more after intubation. VAP increases hospital stays, costs, and mortality risks, making prevention crucial in healthcare settings.
How Can Oral Care Prevent Ventilator-associated Pneumonia?
Regular oral care reduces bacteria in the mouth, lowering infection risks. Using antiseptic mouthwash and toothbrushing prevents bacterial buildup. Proper oral hygiene is a simple, effective VAP prevention strategy for ventilated patients.
Why Is Head-of-bed Elevation Important For Vap Prevention?
Elevating the head of the bed between 30-45 degrees helps prevent aspiration. This position reduces the risk of stomach contents entering the lungs. It is a vital, easy step to decrease ventilator-associated pneumonia incidence.
How Does Hand Hygiene Reduce Ventilator-associated Pneumonia?
Hand hygiene prevents the spread of harmful bacteria to ventilated patients. Healthcare workers must wash hands before and after patient contact. Proper handwashing is one of the most effective VAP prevention practices.
Conclusion
Preventing ventilator-associated pneumonia saves lives and reduces risks. Clean hands and proper hygiene help stop infections. Regularly changing ventilator equipment keeps germs away. Positioning patients carefully lowers lung infection chances. Following these steps protects patients during care. Everyone involved in care plays a key role.
Small actions make a big difference every day. Stay aware and keep safety a top priority. Prevention is possible with simple, consistent efforts.