When someone’s breathing is weak or has stopped, knowing how often to provide bag mask ventilations can make all the difference. If you’re ever in an emergency, your quick actions could save a life.
But how do you know the right pace to give breaths without causing harm? This article will guide you step-by-step, so you feel confident and ready to help when it matters most. Keep reading—you’ll discover simple tips that could turn a scary moment into a chance to save someone’s life.

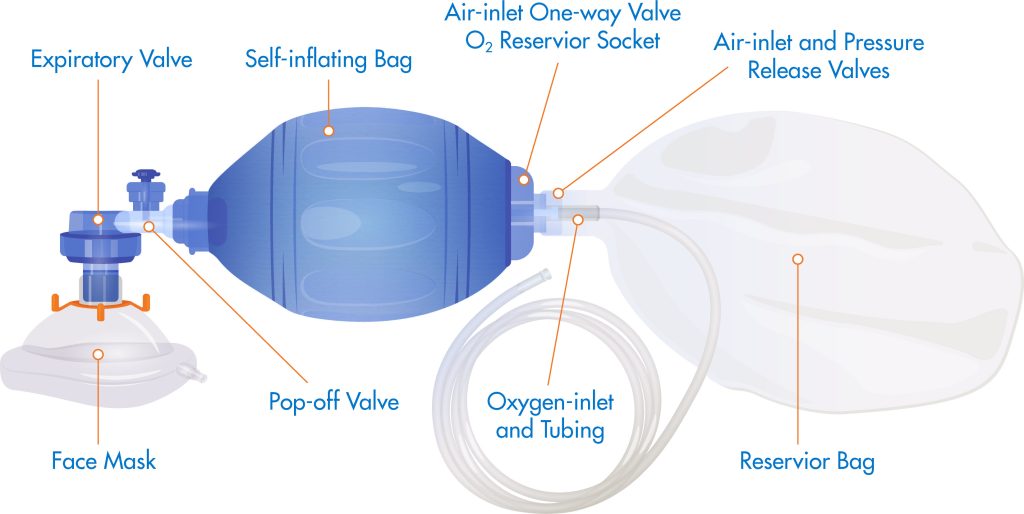
Credit: heartstartcpr.net
Basics Of Bag Mask Ventilation
Understanding the basics of bag mask ventilation is essential for anyone involved in emergency care or resuscitation. This skill can make the difference between life and death by ensuring a patient receives enough oxygen when they cannot breathe on their own. Let’s break down what makes this technique effective and why it matters.
Purpose And Importance
Bag mask ventilation helps deliver air to a patient’s lungs when they are not breathing adequately. It supports oxygen exchange, preventing brain damage and other complications caused by low oxygen levels.
Imagine you are the first responder in a critical situation. The ability to provide proper ventilation can stabilize the patient until advanced help arrives. Would you feel confident knowing exactly why and when to use this technique?
This method is especially important in situations like cardiac arrest, respiratory failure, or trauma. It buys crucial time, maintaining oxygen flow while preparing for further interventions.
Key Components
- Bag:A self-inflating bag stores and delivers air when squeezed.
- Mask:A tight seal over the patient’s nose and mouth ensures air goes into the lungs, not leaking out.
- Valve:Controls the direction of airflow, preventing exhaled air from returning to the bag.
- Oxygen Source:Optional but recommended to increase oxygen concentration.
Each part must work together seamlessly. Even a small leak or poor seal can reduce the effectiveness of ventilation. Have you ever tried sealing a mask and found it tricky? That challenge shows why practice is critical.
Mastering these components and understanding their role sets the foundation for knowing how often and how effectively to provide breaths during ventilation.

Credit: em3.org.uk
When To Start Ventilations
Knowing exactly when to start bag mask ventilations can be a lifesaver. It’s not just about rushing to act but recognizing clear signs that the patient needs help breathing. Your timely intervention can make all the difference.
Signs Of Respiratory Distress
Look for rapid or shallow breathing, grunting, or the use of neck and chest muscles to breathe. Blue lips or fingertips signal low oxygen levels and demand immediate attention. If the patient becomes confused, drowsy, or unresponsive, these are urgent signs that ventilation should begin without delay.
In one emergency I handled, the patient’s breathing slowed to a near stop while still conscious. Recognizing these subtle clues early allowed me to start ventilations quickly and stabilize the situation before it worsened.
Patient Assessment
Check the airway first—ensure it’s clear and open. Listen for breath sounds and feel for chest movement. If the patient is not breathing or breathing inadequately, it’s time to start ventilations.
Don’t wait for the patient to lose consciousness completely. If the breathing is ineffective, your action now can prevent further complications. Always reassess regularly to adjust ventilation frequency based on the patient’s response.
Optimal Ventilation Rates
Providing the right number of bag mask ventilations is vital during resuscitation. Too fast or too slow can harm the patient. Optimal ventilation rates help maintain proper oxygen levels and support breathing effectively. Knowing the correct pace improves outcomes and reduces complications.
Adult Ventilation Frequency
For adults, give one ventilation every 5 to 6 seconds. This means about 10 to 12 breaths per minute. Each breath should last around 1 second and make the chest rise visibly. Avoid giving too many breaths, as this can cause air to enter the stomach and increase pressure in the chest.
Child And Infant Rates
Children and infants need faster ventilations than adults. Deliver one breath every 3 to 5 seconds. This equals about 12 to 20 breaths per minute. Use gentle breaths to avoid lung injury. Watch the chest rise with each ventilation to confirm effective breaths.
Techniques For Effective Ventilation
Effective bag mask ventilation is more than just squeezing a bag. It requires precision and care to ensure the patient receives the right amount of air without causing harm. Understanding the techniques that improve ventilation can make a significant difference in patient outcomes.
Proper Mask Seal
A tight mask seal is crucial. Without it, air escapes and ventilation becomes ineffective.
Use your thumb and index finger to form a “C” shape around the mask, while the other fingers lift the jaw. This technique helps create a secure seal and keeps the airway open.
Have you noticed how even a small leak can reduce the volume of air delivered? That’s why checking the seal before each ventilation is essential.
Controlled Breathing
Delivering breaths too quickly or forcefully can cause complications. Aim for slow, steady breaths that mimic natural breathing patterns.
Typically, one breath every 5 to 6 seconds is ideal for adults. This timing allows the lungs to fill and empty properly without causing pressure buildup.
Try counting out loud as you breathe for the patient. It helps maintain a consistent pace and prevents rushing.
Avoiding Overventilation
Overventilation can lead to increased pressure in the chest, reducing blood flow to vital organs. It also raises the risk of gastric inflation, which can cause vomiting and aspiration.
Pay attention to chest rise rather than how hard you squeeze the bag. Gentle squeezes are often enough to see adequate chest movement.
Have you ever felt the urge to squeeze harder during emergencies? Resisting that urge and focusing on technique can improve safety and effectiveness.
Adjusting Ventilation Based On Patient Condition
Adjusting the rate and volume of bag mask ventilations depends heavily on the patient’s specific condition. You need to recognize signs that indicate whether to speed up or slow down your ventilations. Understanding these nuances can improve outcomes and avoid complications.
Cardiac Arrest Scenarios
During cardiac arrest, the priority is maintaining oxygen delivery without causing harm. You should provide ventilations at a rate of about 10 breaths per minute, roughly one breath every 6 seconds.
Too many breaths can increase intrathoracic pressure and reduce blood flow to the heart. I once witnessed a trainee increase ventilation rate out of nervousness, which actually compromised circulation. This experience showed me the importance of controlled, steady breaths.
Keep your breaths gentle and consistent. Watch for chest rise to ensure effective ventilation but avoid over-inflation. Remember, your goal is to support circulation, not replace it.
Respiratory Failure Cases
In cases of respiratory failure, the ventilation rate often needs to be higher. You might deliver 12 to 20 breaths per minute, depending on the patient’s oxygen levels and carbon dioxide retention.
Patients struggling to breathe on their own may require smaller, more frequent breaths to match their natural rhythm. You can adjust the volume and speed based on how well the patient responds.
Ask yourself: is the patient improving with your current ventilation rate? If not, tweak your approach carefully. Watch for changes in skin color, consciousness, and chest movement to guide your adjustments.

Credit: brieflands.com
Common Mistakes And How To Avoid Them
When providing bag-mask ventilation, mistakes can occur. These errors can impact the effectiveness of the procedure. Understanding common mistakes helps improve patient outcomes. Let’s explore some frequent errors and how to avoid them.
Inadequate Ventilation Rate
A common mistake is the wrong ventilation rate. Ventilating too slowly can lead to insufficient oxygen. Ventilating too quickly can cause hyperventilation. Both can affect patient stability.
Ensure to count breaths accurately. Use a timer or metronome if needed. The standard rate is 10-12 breaths per minute for adults. For children, aim for 20 breaths per minute. Practice helps maintain a consistent rhythm.
Excessive Ventilation Pressure
Applying too much pressure is another mistake. This can cause lung injury or air leakage. Avoid forceful squeezing of the bag. Excessive pressure can also inflate the stomach. This may lead to vomiting and aspiration.
Use gentle, controlled squeezes. Feel for chest rise to gauge pressure. A good seal is also crucial. Check for air leaks around the mask. Practice helps develop a natural feel for pressure.
Monitoring And Troubleshooting
Proper timing for bag mask ventilations ensures effective breathing support. Watch chest rise and adjust ventilation rate to avoid over or under-ventilating. Regular checks help spot problems quickly and keep the patient stable.
Monitoring and troubleshooting are key parts of successful bag mask ventilation. Careful observation ensures effective ventilation and helps catch problems early. Watch for signs that show how well the ventilation is working. Adjust techniques if needed to improve patient outcomes.Signs Of Effective Ventilation
Look for visible chest rise with each ventilation. This indicates air reaching the lungs. Listen for breath sounds using a stethoscope. They confirm air entry into the lungs. Check the patient’s skin color. It should improve, indicating better oxygenation. Monitor heart rate and oxygen levels. Stable or improving levels signal effective ventilation.When To Reassess Technique
Reassess if chest rise is absent or minimal. Check the mask seal if ventilation seems ineffective. Adjust the position of the head and neck. Ensure the airway is open. Listen for unusual sounds that suggest airway obstruction. Re-evaluate the technique regularly, especially if the patient’s condition changes.Training And Practice Tips
Training and practice are key to providing effective bag mask ventilations. Regular practice helps maintain skill and confidence. It also improves response time during emergencies. Focused training ensures proper technique and ventilation rate. Consistent practice helps keep knowledge fresh and accurate.
Simulation Exercises
Simulation exercises mimic real-life scenarios. They provide hands-on experience without risk. Practice with different patient types and situations. Use manikins to simulate breathing and airway challenges. Repeat exercises often to build muscle memory. This helps maintain smooth and effective ventilations. Trainers can give feedback to improve technique. Simulations build confidence for real emergencies.
Regular Skill Updates
Skills can decline without regular refreshers. Schedule training sessions every few months. Review the correct ventilation rate and technique. Update knowledge on new guidelines or tools. Practice with peers to share tips and correct mistakes. Use checklists to track progress and skills. Continuous learning keeps skills sharp and reliable. It also reduces errors during critical moments.
Frequently Asked Questions
How Often Should Bag Mask Ventilations Be Provided?
Bag mask ventilations should be given at a rate of 10-12 breaths per minute for adults. For infants, the rate is 12-20 breaths per minute. This ensures adequate oxygen delivery and prevents lung overinflation.
What Is The Ideal Ventilation Rate For Bag Mask Use?
The ideal ventilation rate is one breath every 5-6 seconds for adults. For children and infants, it’s one breath every 3-5 seconds. Consistency in timing maintains effective oxygenation and prevents hyperventilation.
Can Too Frequent Bag Mask Ventilations Cause Harm?
Yes, excessive ventilation can lead to gastric inflation and decreased cardiac output. It is crucial to maintain the recommended ventilation rate to avoid complications during resuscitation.
When Should Bag Mask Ventilation Be Initiated?
Bag mask ventilation should start immediately when a patient shows inadequate breathing or apnea. Early intervention improves oxygen delivery and increases survival chances during emergencies.
Conclusion
Providing bag mask ventilations at the right rate saves lives. Aim for 10 to 12 breaths per minute for adults. Watch chest rise to ensure good air delivery. Avoid giving breaths too fast or too slow. Practice helps improve timing and technique.
Stay calm and focus on steady, clear breaths. Proper ventilation supports oxygen flow and patient recovery. Keep learning and practicing to feel confident. Every breath counts in emergencies.