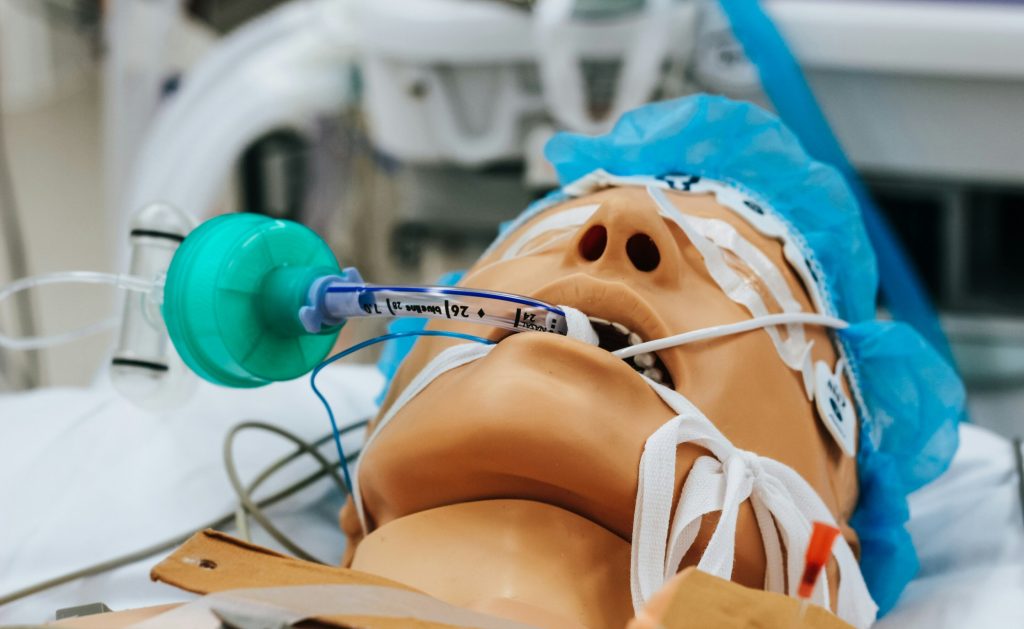
If you or a loved one is facing brain surgery, one question you might be asking is, “How long will I be on a ventilator after the operation?” This is a crucial concern because being on a ventilator affects your recovery and comfort. Understanding what to expect can ease your mind and help you prepare for the days ahead.
You will discover the key factors that influence ventilator time, what the process looks like, and how doctors work to get you breathing on your own again. Keep reading to gain clear, simple answers that can help you feel more in control during this challenging time.
Factors Influencing Ventilator Duration
The time a patient spends on a ventilator after brain surgery varies widely. Several key factors influence this duration. Understanding these helps families and caregivers prepare better. Doctors consider these aspects to plan post-surgery care effectively.
Type Of Brain Surgery
Different brain surgeries affect breathing needs differently. Major surgeries like tumor removal often require longer ventilator support. Minor procedures may need only brief assistance. Surgeries near the brainstem can impact breathing control directly. This leads to extended ventilator use.
Patient’s Age And Health
Older patients tend to need longer ventilator support. Their lungs and muscles are usually weaker. Pre-existing health conditions like lung or heart disease affect recovery time. Younger patients with good health often breathe independently sooner. Strong immune systems also help shorten ventilator duration.
Surgical Complications
Complications during or after surgery can delay breathing recovery. Infections or bleeding near the brain may prolong ventilator use. Swelling in brain tissues can impact breathing centers. Emergency reoperations increase the need for ventilator support. Careful monitoring is crucial to manage these risks.
Typical Ventilator Timeframes
After brain surgery, patients often need help breathing. This help comes from a machine called a ventilator. The length of time a patient stays on a ventilator varies. It depends on the surgery type and the patient’s condition. Understanding typical ventilator timeframes helps families prepare for recovery.
Short-term Ventilation
Many patients only need a ventilator for a short time. This usually lasts a few hours to a couple of days. The goal is to support breathing while the patient wakes from anesthesia. Doctors monitor vital signs closely during this period. Most patients can breathe on their own soon after surgery.
Short-term ventilation is common in less complex surgeries. It allows time to ensure the brain and lungs work well. Nurses and doctors check for signs of complications. If recovery is smooth, the ventilator is removed quickly.
Extended Ventilation Needs
Some patients need ventilators for longer periods. This can range from several days to weeks. Extended ventilation happens if the brain or lungs have trouble recovering. It can also occur if there are complications like swelling or infection.
Longer ventilation requires careful care to avoid lung problems. Doctors and therapists work to help the patient regain breathing strength. They may use special techniques to prevent muscle weakness. Family support and patience are important during this time.
Signs Of Successful Weaning
Recognizing the signs of successful weaning from a ventilator after brain surgery is crucial for both patients and caregivers. It means the patient’s body is ready to breathe on its own, reducing the risk of complications. Knowing what to look for can help you stay informed and involved in the recovery process.
Improved Breathing Patterns
One clear sign is a steady and natural breathing rhythm without the ventilator’s help. You might notice the patient taking deeper, more regular breaths. This shows the lungs and respiratory muscles are regaining strength.
Watch for fewer episodes of rapid or shallow breathing. These can indicate stress or weakness. A smooth, calm breathing pattern is a positive step toward full independence.
Stable Vital Signs
Vital signs like heart rate, blood pressure, and oxygen levels should remain steady during and after weaning attempts. Fluctuations might mean the body is struggling without mechanical support.
For example, if oxygen saturation stays above 90% without extra oxygen, it’s a good indicator that the lungs are functioning well. Regular monitoring helps you understand if the body is adapting to breathing on its own.
Neurological Progress
Since brain surgery affects the nervous system, improvements here are just as important. You may see increased alertness, better muscle control, or more purposeful movements.
These signs suggest the brain is healing and can support the body’s natural breathing drive. Ask yourself: Is the patient responding more to their environment? Such progress often aligns with successful ventilator weaning.

Credit: ca.style.yahoo.com
Risks Of Prolonged Ventilation
Spending an extended time on a ventilator after brain surgery carries serious risks. The longer you rely on mechanical breathing support, the greater the chance of complications that can slow your recovery and affect your overall health. Understanding these risks helps you stay informed and prepared to discuss care options with your medical team.
Infections And Pneumonia
Being on a ventilator for a long time increases the risk of lung infections, especially ventilator-associated pneumonia (VAP). Bacteria can enter your lungs through the breathing tube, causing inflammation and difficulty breathing. Doctors often watch closely for signs like fever, coughing, or changes in mucus to catch infections early.
If you or a loved one face prolonged ventilation, ask how the care team prevents infections. Simple steps like regular oral care and changing ventilator tubes can make a big difference.
Lung Injury
Ventilators push air into your lungs, but if used too aggressively, they can cause damage. This damage might include lung swelling or pressure injuries that make breathing even harder when you try to come off the machine. Finding the right balance in ventilator settings is crucial to protect your lungs while supporting your breathing.
Have you discussed with your healthcare provider how they monitor lung health during ventilation? Knowing this can help you feel more in control of the process.
Muscle Weakness
When the ventilator does most of the work, your breathing muscles don’t get the usual exercise. This can lead to muscle weakness, making it tough to breathe independently once the ventilator is removed. Physical therapy and gradual weaning from the ventilator are key strategies to rebuild strength.
Consider asking about breathing exercises or therapies that can keep your muscles active even while on the ventilator. Small efforts here can speed your path to recovery.
Supportive Care During Ventilation
Determining ventilator duration after brain surgery depends on individual recovery speed. Medical teams monitor vital signs closely. They adjust support based on patient needs. Regular assessments ensure optimal care during this critical phase.
Supporting a patient on a ventilator after brain surgery is vital. This phase involves careful attention to various needs. Each aspect of supportive care plays a crucial role in recovery. Focused care can enhance the healing process significantly.Sedation Management
Sedation is essential for patient comfort. It helps reduce stress and anxiety. The right sedation level is critical. Too much sedation can delay recovery. Too little can cause discomfort. Medical teams monitor sedation closely. They adjust doses as needed. This ensures the patient remains calm and safe.Physical Therapy
Physical therapy is important during ventilation. It helps maintain muscle strength. Therapists work with patients even in bed. Simple exercises are beneficial. They prevent muscle stiffness. Regular movement boosts circulation. It also helps prevent blood clots. Physical therapy is a key part of recovery.Nutritional Support
Good nutrition aids healing. Patients may not eat normally while on a ventilator. Nutritional needs are met in other ways. Tube feeding is common. It provides essential nutrients. A dietitian often plans the meals. This ensures a balanced diet. Proper nutrition supports overall health and recovery.
Credit: www.kentonline.co.uk
Family Involvement And Communication
Family involvement and communication play a key role after brain surgery. Ventilator support can be stressful for both the patient and their loved ones. Clear communication helps families understand the situation and prepare for what lies ahead. Being involved in care decisions offers comfort and hope during tough times.
Setting Expectations
Doctors and nurses explain how long ventilator support may last. Families learn about possible challenges and recovery steps. Realistic expectations reduce confusion and fear. Knowing what might happen helps families stay calm and focused.
Emotional Support
Family members need emotional care too. Sharing feelings and worries with hospital staff helps reduce stress. Support groups or counseling can provide relief. Comfort from loved ones strengthens the patient’s will to heal.
Updates On Progress
Regular updates keep families informed about the patient’s condition. Medical teams share changes in breathing ability and brain function. Timely news helps families plan visits and care. Staying informed creates trust and eases anxiety.
Preparing For Ventilator Removal
Preparing for ventilator removal after brain surgery is a careful process. The medical team watches the patient closely to ensure safety. The goal is to help the patient breathe on their own again. This step requires patience and careful checks.
Breathing Trials
Breathing trials test if the patient can breathe without help. The ventilator support is lowered gradually. The patient tries to breathe on their own for short periods. Nurses and doctors watch for signs of stress or fatigue. These trials help decide if the patient is ready.
Assessing Readiness
Doctors check many factors before removing the tube. They look at the patient’s breathing strength and oxygen levels. The patient’s mental state and muscle control are important too. Stable vital signs and no severe swelling are good signs. The team decides only when all signs are positive.
Post-extubation Care
After removing the ventilator tube, care continues closely. The patient’s breathing is monitored for any problems. Nurses assist with coughing and clearing mucus from the lungs. Oxygen support might still be given if needed. This care helps the patient recover smoothly and safely.
Credit: drgurneetsawhney.com
Frequently Asked Questions
How Long Do Patients Stay On Ventilators After Brain Surgery?
Patients typically remain on ventilators for 24 to 72 hours after brain surgery. The exact duration depends on surgery complexity and recovery speed. Doctors monitor breathing and neurological status closely to decide when to safely remove the ventilator.
What Factors Affect Ventilator Duration After Brain Surgery?
Ventilator time depends on surgery type, patient health, and brain function recovery. Complications like swelling or infections can extend ventilation needs. Each patient’s response to surgery influences how quickly they can breathe independently.
Can Ventilator Support Impact Brain Surgery Recovery?
Yes, ventilator support ensures stable breathing, crucial for brain healing. Prolonged ventilation might increase infection risk but is essential if breathing is weak. Proper ventilator management aids smooth recovery and reduces complications.
When Is It Safe To Remove A Ventilator Post Brain Surgery?
Ventilators are removed once patients breathe independently and neurological signs improve. Doctors assess oxygen levels, breathing strength, and alertness before extubation. Safety is the priority to avoid respiratory distress after removal.
Conclusion
Time on a ventilator after brain surgery varies by patient and surgery type. Doctors watch breathing closely to decide when to remove the ventilator. Some recover quickly, while others need more support. Rest and care are key parts of healing.
Trust your medical team and stay patient through recovery. Every step brings progress. Keep hope and focus on small improvements each day.