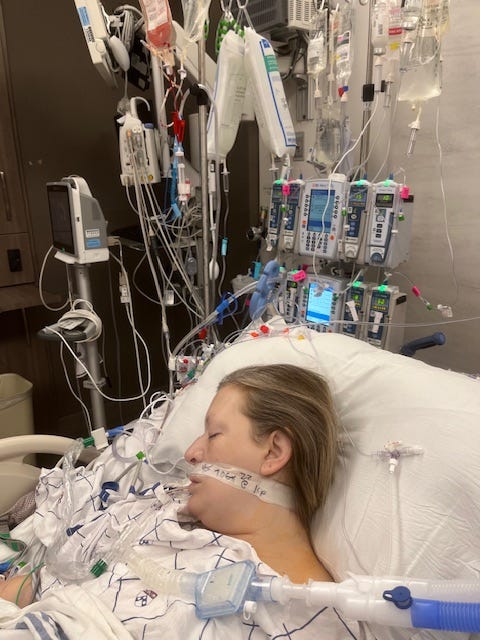
Have you ever wondered what it’s like for someone to be on a ventilator? Is the person awake and aware, or are they completely unconscious?
If someone you care about is on a ventilator, these questions can feel overwhelming. Understanding what consciousness means in this situation can help ease your fears and give you clarity. You’ll discover how being on a ventilator affects awareness, what signs to look for, and what you can expect while your loved one is receiving this life-saving support.
Keep reading to learn the truth behind this complex topic—it might change how you see the experience altogether.
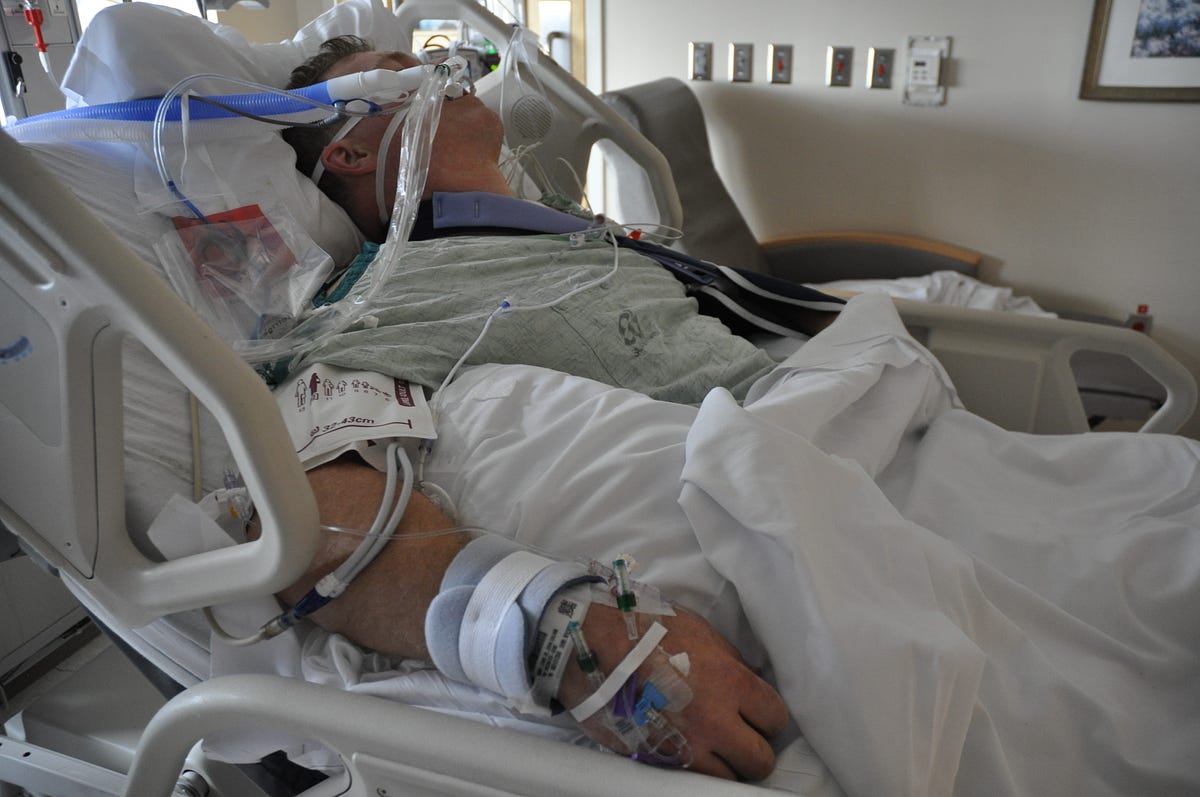
Credit: medium.com
Consciousness And Ventilators
Understanding consciousness in patients on ventilators is important for families and caregivers. Ventilators support breathing but do not directly affect awareness. Consciousness depends on brain function, not the breathing machine. This section explains consciousness and how ventilators work.
What Consciousness Means In Medical Terms
Consciousness means being awake and aware of surroundings. It involves the brain’s ability to respond to stimuli. Doctors assess consciousness using simple tests, like asking questions or checking reflexes. Levels of consciousness range from full alertness to deep coma. Brain injuries or illnesses can lower consciousness. Being on a ventilator does not automatically mean unconsciousness.
How Ventilators Work
Ventilators help patients breathe by pushing air into the lungs. They replace or support natural breathing when a person cannot breathe well. The machine controls airflow, oxygen levels, and pressure. Ventilators have settings adjusted by medical staff. They do not affect brain activity or awareness. Patients on ventilators can be fully conscious or sedated, depending on their condition.
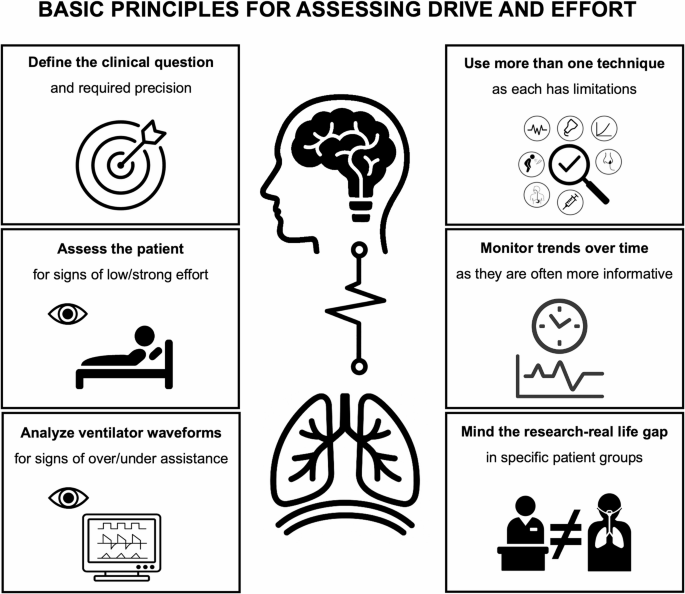
Credit: ccforum.biomedcentral.com
Factors Affecting Awareness
Understanding whether someone is conscious while on a ventilator depends on several key factors. Awareness can vary greatly based on medical conditions, treatments, and brain activity. Let’s break down the main elements that influence consciousness in these situations.
Sedation And Medication Effects
Medications given to patients on ventilators often include sedatives and painkillers. These drugs are essential to keep you comfortable and calm, but they can also dull your awareness.
The level and type of sedation directly impact how awake or responsive you may feel. Sometimes, doctors adjust medications to find a balance where you’re pain-free yet still able to respond.
Have you ever noticed how some medicines make you feel foggy or alert? This effect can be similar for ventilated patients, making it hard to tell if they’re fully aware or just under medication’s influence.
Brain Function And Injury
Your brain controls consciousness, so any injury or illness affecting it plays a major role in awareness levels. Conditions like strokes, trauma, or infections can reduce your brain’s ability to keep you awake and alert.
Even without visible injury, brain swelling or lack of oxygen can cloud your consciousness. Doctors often use brain scans and tests to understand how your brain is functioning while on the ventilator.
Think about how a headache or dizziness affects your focus—brain issues on a ventilator can have a much stronger impact on awareness.
Levels Of Consciousness On Ventilators
Consciousness isn’t just “on” or “off.” There are different levels that describe how awake and responsive you are during ventilation.
- Alert:Fully awake, aware of surroundings, and able to communicate.
- Drowsy:Somewhat awake but easily drift off or less responsive.
- Unresponsive:No response to external stimuli; often the result of deep sedation or brain injury.
Understanding these levels helps you grasp why someone might appear unconscious yet still have some awareness. It also highlights why caregivers carefully monitor and adjust treatment to support the best possible level of consciousness.
Signs Of Awareness
Recognizing signs of awareness in someone on a ventilator can be challenging. The ventilator supports breathing, but it does not always indicate unconsciousness. Caregivers and medical staff watch closely for subtle clues. These signals help determine if the person remains aware or responsive despite their condition.
Physical Responses To Stimuli
Small movements may show awareness. Gentle squeezing of a hand or a slight twitch in fingers can be meaningful. Reacting to touch, pain, or sound suggests the brain processes sensory input. Sometimes, patients may move their limbs or try to adjust their position. These responses often occur without the person needing to speak.
Eye Movement And Communication
Eyes reveal a lot about awareness. Following objects or people with their eyes is a key sign. Blinking in response to questions or commands shows understanding. Some patients use eye movements to communicate simple messages. Even subtle changes in gaze direction can indicate attention or recognition.
Brain Activity Monitoring
Doctors use tools to measure brain signals. Electroencephalograms (EEGs) record electrical activity in the brain. Patterns in these signals help identify levels of consciousness. Functional MRI scans show areas of the brain that respond to stimuli. This monitoring provides objective evidence about awareness beyond physical signs.
Assessing Consciousness In Patients
Assessing consciousness in patients on a ventilator is a crucial part of medical care. It helps doctors understand the patient’s brain function and guide treatment decisions. Consciousness can be hard to judge because the patient cannot speak or move freely. Medical teams use careful observation and tests to determine awareness levels. These assessments help identify if a patient is awake, responsive, or deeply unconscious.
Common Clinical Tests
Doctors use several clinical tests to check consciousness in ventilated patients. The Glasgow Coma Scale (GCS) is a standard tool. It measures eye, verbal, and motor responses. Scores range from 3 to 15, with lower scores indicating deeper unconsciousness.
Other tests include:
- Checking pupil reaction to light
- Observing spontaneous or reflex movements
- Testing responses to pain stimuli
These tests provide quick information about brain function. They are simple but effective at bedside assessment.
Use Of Technology In Assessment
Technology supports clinical evaluations by adding objective data. Electroencephalograms (EEG) monitor brain wave activity. They help detect awareness even when physical responses are absent. Functional MRI scans can show brain activity patterns. They are useful for detailed studies but less common in daily care.
Other tools like pupillometers measure pupil size and reaction precisely. These devices give accurate, repeatable results. Technology enhances the accuracy of consciousness assessment in ventilated patients.
Emotional And Psychological Considerations
When a loved one is on a ventilator, emotions run high. It’s an overwhelming experience filled with uncertainty. The emotional and psychological impact is profound. Both patients and families face unique challenges. Understanding these can help in offering the right support.
Patient Experiences And Memories
Patients on ventilators may have varied experiences. Some recall vivid memories. Others may feel confused or scared. The noise from machines can add stress. Sedatives might blur their sense of time. Despite this, small gestures can bring comfort. Holding hands or gentle words can reassure them.
Family And Caregiver Perspectives
Families often feel helpless. Watching a loved one on a ventilator is tough. They worry about recovery and long-term effects. Caregivers provide crucial support. Their role is both physically and emotionally demanding. They must balance hope with reality. Open communication with medical staff is key. It helps families feel involved and informed.

Credit: www.hospitalstore.com
Ethical And Medical Implications
The ethical and medical implications of consciousness in patients on ventilators raise profound questions. Understanding how sedation affects awareness and the challenges in end-of-life care can change how you view critical care. These topics push us to consider not only medical facts but also the values guiding treatment decisions.
Decisions On Sedation Levels
Choosing the right sedation level is a delicate balance. Too much sedation can leave a patient unaware but disconnected from their surroundings. Too little might cause distress or discomfort.
Doctors often adjust sedation based on vital signs and patient responses, but you might wonder: can a patient silently experience pain or fear even when sedated?
Recent practices encourage minimal sedation to keep patients as alert as possible while ensuring comfort. This approach helps you and healthcare providers communicate better with the patient when possible.
End-of-life Care And Awareness
Awareness during end-of-life care on a ventilator brings emotional and ethical challenges. Families often ask if their loved one can hear or understand them. This question influences how they interact with the patient.
Medical teams must respect the patient’s dignity, balancing life support with quality of life. You might face difficult choices about continuing ventilation or focusing on comfort care.
Clear communication about prognosis and patient wishes is vital. Have you ever thought about how awareness affects the decisions you would want made for you or a family member?
Improving Patient Comfort And Awareness
Improving patient comfort and awareness is crucial for those on a ventilator. Patients often feel scared and confused due to limited movement and communication. Comfort helps reduce stress and can improve recovery. Awareness allows patients to engage with caregivers and feel less isolated.
Health teams focus on adjusting the ventilator and finding ways to communicate. These steps help patients feel safer and more in control despite the machines.
Adjusting Ventilator Settings
Caregivers carefully set the ventilator to match the patient’s breathing needs. This prevents discomfort caused by too much or too little air pressure. Adjustments include:
- Changing air volume to avoid lung strain
- Setting breathing rate to match patient effort
- Controlling oxygen levels to keep blood healthy
- Using sedation wisely to avoid over-sedation
Proper settings reduce feelings of breathlessness and anxiety. Patients can breathe more naturally and feel less trapped by the machine.
Communication Strategies
Communication is key for awareness and comfort. Many patients cannot speak with the ventilator tube in place. Nurses and doctors use:
- Simple yes/no signals like blinking or hand squeezes
- Writing boards or letter charts for basic messages
- Technology like speech-generating devices when possible
- Frequent updates from caregivers to explain care steps
Clear communication helps patients express needs and reduces fear. It also builds trust between patients and healthcare providers.
Frequently Asked Questions
Can Patients On Ventilators Stay Conscious?
Yes, many patients on ventilators remain conscious. Consciousness depends on their medical condition and sedation levels. Ventilators assist breathing but do not necessarily induce unconsciousness.
How Do Doctors Assess Consciousness On A Ventilator?
Doctors use neurological exams and monitoring tools to assess consciousness. They check eye response, movement, and brain activity to determine awareness in ventilated patients.
Can Sedatives Affect Consciousness On Ventilators?
Yes, sedatives often reduce consciousness to keep patients comfortable. Sedation levels vary based on treatment needs and can range from light to deep sedation.
What Signs Indicate Awareness In Ventilated Patients?
Signs include eye movement, purposeful gestures, and response to stimuli. These cues help medical staff gauge if a ventilated patient is conscious and aware.
Conclusion
People on ventilators may be conscious, but it varies widely. Doctors check brain activity and responses carefully. Some patients stay awake and aware; others remain deeply asleep. Family members should ask medical staff for updates. Understanding this helps reduce fear and confusion.
Care teams work hard to keep patients safe and comfortable. Each case is unique, so stay informed and patient. This knowledge brings hope during tough times.