If you or a loved one is on a ventilator, you probably have many questions. One of the hardest to face is: how long is too long to be on a ventilator?
Understanding this can help you make important decisions about care and recovery. This article will guide you through what to expect, what risks are involved, and how doctors decide when it’s time to start weaning off the machine. Keep reading to gain clarity and feel more in control during a difficult time.
Ventilator Basics
Understanding the basics of ventilators is essential if you or a loved one ever faces the reality of mechanical breathing support. Ventilators are complex machines, but their main job is straightforward: to help patients breathe when they can’t do it well enough on their own. Knowing how they work and the different types available can help you feel more informed and less overwhelmed in critical moments.
Purpose Of Mechanical Ventilation
Mechanical ventilation supports or replaces natural breathing. It delivers oxygen to the lungs and removes carbon dioxide from the body.
People might need a ventilator for various reasons:
- Severe lung infections like pneumonia
- Injury or surgery that affects breathing
- Chronic lung diseases such as COPD
- Neurological conditions that weaken respiratory muscles
Without this support, the body’s organs can suffer from lack of oxygen. So, ventilators buy time for healing or for doctors to treat the underlying problem.
Types Of Ventilators
Ventilators come in several types, each designed for specific patient needs and conditions. The two broad categories are invasive and non-invasive ventilators.
- Invasive ventilatorsrequire a tube inserted into the windpipe. This method is common in intensive care when patients cannot breathe at all on their own.
- Non-invasive ventilatorsuse masks to deliver air and are often used for patients who need some breathing assistance but can still breathe independently.
Within these categories, you’ll find machines with different settings and modes. For instance, some ventilators provide a fixed number of breaths per minute, while others adjust based on your own breathing efforts.
Have you ever wondered how doctors decide which ventilator type is best? It’s a careful balance between the patient’s condition and how invasive the support needs to be.
Typical Duration On A Ventilator
Understanding the typical duration on a ventilator is crucial if you or a loved one faces this medical intervention. The length of time someone stays on a ventilator varies widely depending on the underlying condition and response to treatment. Knowing what to expect can help you prepare emotionally and physically for the journey ahead.
Short-term Use
Most people use a ventilator for a short period, often just a few hours to a few days. This usually happens after surgeries or acute illnesses where breathing support is temporarily needed. For example, patients recovering from anesthesia during surgery might require ventilation until they can breathe on their own again.
Short-term ventilation reduces the risk of complications. You might wonder how quickly breathing can return to normal. In many cases, the goal is to wean off the ventilator as soon as possible to avoid muscle weakness and infections.
Extended Use Scenarios
Extended use of a ventilator can last weeks or even months in some cases. Conditions like severe pneumonia, chronic lung disease, or spinal cord injuries may require longer support. For instance, people with COVID-19-related respiratory failure sometimes need ventilation for several weeks.
Long-term ventilation carries more risks, including lung damage and infections. Are you prepared to manage these challenges if faced with extended ventilation? Families often need to make tough decisions about ongoing care and quality of life during this time.
Risks Of Prolonged Ventilation
Spending an extended period on a ventilator can be life-saving, but it also comes with its share of risks. Understanding these risks helps you recognize why medical teams carefully weigh the benefits against potential complications. How long is too long often depends on how your body and mind respond to being on mechanical support.
Physical Complications
Prolonged ventilation can lead to several physical issues that affect your recovery. Muscle weakness is common because your breathing muscles aren’t working as hard, which can delay your ability to breathe independently.
There’s also a higher chance of lung infections like pneumonia. The ventilator tube bypasses your natural defenses, allowing bacteria easier access to your lungs. If you notice any sudden fever or increased mucus, it’s crucial to alert your care team immediately.
Other problems include damage to your vocal cords and airway, caused by the tube pressing on delicate tissues. This can result in a sore throat or difficulty speaking after the ventilator is removed. Have you ever wondered how such small tubes can cause such discomfort?
Psychological Impact
Being on a ventilator is not just physically challenging; it can take a serious toll on your mental health. Many patients report feelings of anxiety and confusion, especially if sedation is involved.
Sleep disturbances are frequent because the ICU environment is noisy and bright, making it hard for your brain to rest. This lack of sleep can worsen confusion and mood swings, creating a cycle that’s tough to break.
Some people experience post-traumatic stress disorder (PTSD) after their time on the ventilator. Flashbacks or nightmares about the experience can linger long after discharge. If you find yourself feeling overwhelmed, talking to a mental health professional can make a big difference.
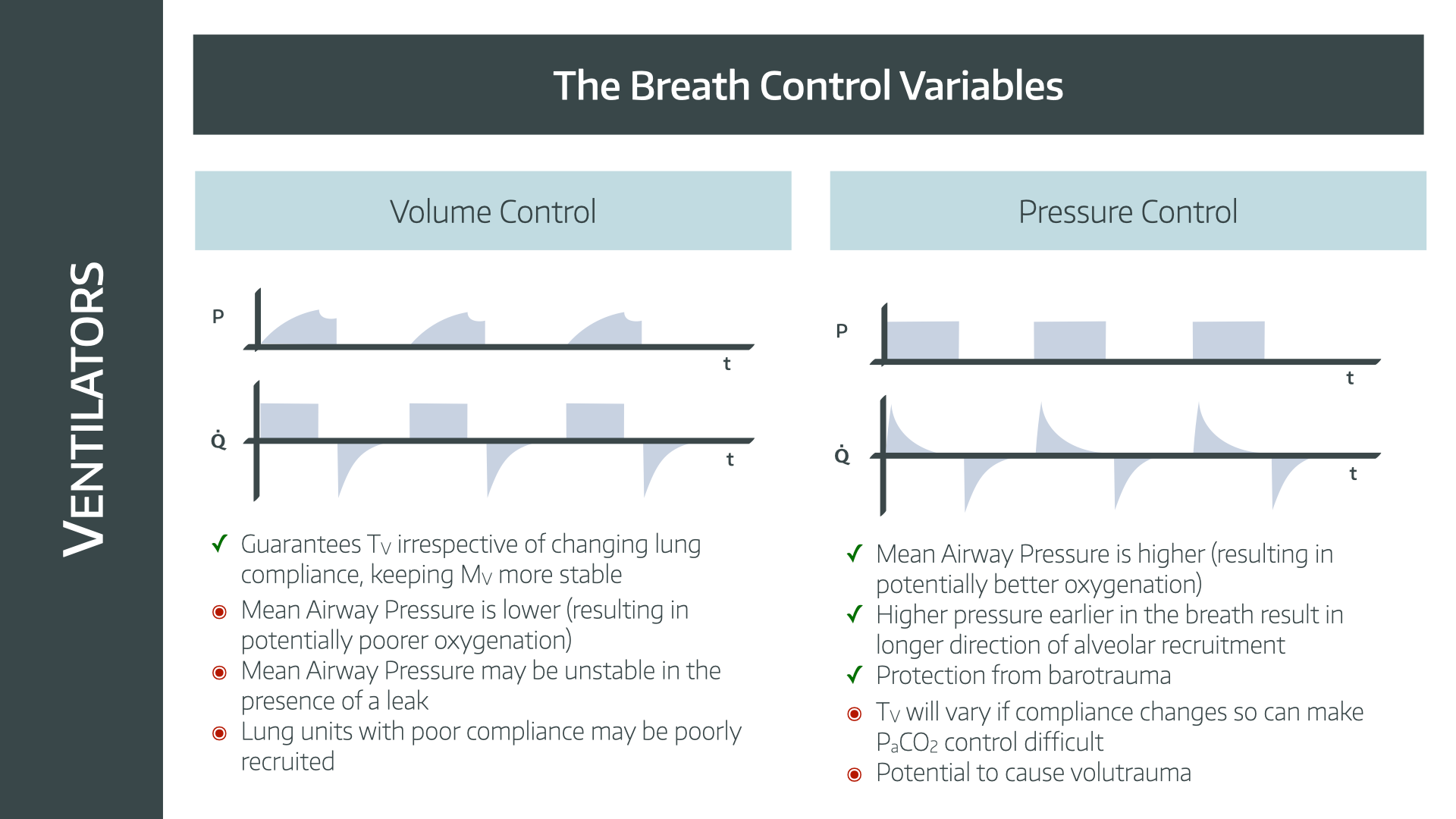
Credit: www.anaestheasier.com
Factors Affecting Ventilation Length
The length of time a person spends on a ventilator depends on many factors. These factors help doctors decide the best course of care. Understanding them can clear up why some patients need longer support.
Each patient’s situation is unique. Their health and the severity of their illness play big roles in how long they stay on a ventilator.
Patient’s Health Condition
A patient’s overall health affects ventilation length. Strong lungs and good muscle strength help people recover faster. Older age or chronic diseases may slow recovery.
People with weak immune systems may face longer ventilation times. Conditions like diabetes or heart problems add extra risks. Healthy patients often breathe on their own sooner.
Underlying Illness Severity
The seriousness of the illness causing breathing problems matters. Severe lung infections or injuries require longer support. Mild cases might only need a few days on the ventilator.
Some illnesses damage the lungs deeply. This damage can extend ventilation needs. Quick treatment and early care improve chances to wean off faster.
Weaning Off The Ventilator
Weaning off the ventilator is a crucial phase in a patient’s recovery. It means reducing and stopping the machine that helps with breathing. The goal is to help the patient breathe on their own again. This process needs careful monitoring and support.
Doctors watch for signs that show the patient is ready. They use different techniques to make the transition smooth and safe. The right timing helps avoid complications and speeds up recovery.
Signs Of Readiness
- Stable breathing rate and pattern without distress
- Good oxygen levels in the blood
- Strong cough to clear airways
- Ability to follow simple commands
- Stable heart rate and blood pressure
- No signs of infection or worsening illness
Weaning Techniques
Doctors use different methods based on the patient’s condition. These include:
- Spontaneous Breathing Trials:Patient tries breathing without help for short times.
- Pressure Support Ventilation:Machine gives less help as patient breathes more.
- Continuous Positive Airway Pressure (CPAP):Keeps airways open while patient breathes alone.
- Gradual Reduction:Slowly lowering ventilator settings to encourage natural breathing.
Each step is carefully watched. The team looks for any signs of trouble. The goal is to keep the patient safe and comfortable during weaning.
When To Consider Alternative Approaches
Prolonged ventilator use can lead to complications. It’s important to assess the patient’s recovery progress. Exploring alternative treatments may improve outcomes and comfort.
Deciding when to consider alternative approaches for ventilator support is a crucial aspect of patient care. It’s not just about the medical implications but also the quality of life for the patient. If you’re facing this decision, you’re likely considering how to balance medical necessity with compassionate care.Tracheostomy
A tracheostomy could be a viable option when prolonged ventilator support is necessary. This procedure involves creating an opening in the neck to place a tube directly into the windpipe. It can offer more comfort and mobility compared to a traditional ventilator. Many find that a tracheostomy allows for easier communication and a better overall experience. It’s often recommended if the patient is expected to be on a ventilator for more than a couple of weeks. However, it’s crucial to discuss the benefits and risks with your healthcare provider to make an informed decision.Palliative Care Options
Palliative care focuses on providing relief from the symptoms and stress of a serious illness. It is not limited to end-of-life situations and can be considered at any stage of illness. This approach can include pain management, emotional support, and even spiritual guidance. Consider whether the patient’s current ventilator use aligns with their long-term goals and values. If the ventilator is causing more discomfort than relief, palliative care might offer a better quality of life. Engage with a palliative care team to explore options that prioritize comfort and dignity. Is it time to think about these alternatives for yourself or a loved one? The decision is deeply personal and should be made with compassion and careful thought. Always prioritize open communication with your healthcare team and loved ones.Role Of Medical Team And Family
The role of the medical team and family is crucial when deciding how long a patient should stay on a ventilator. Both parties bring unique perspectives that influence care plans. Medical professionals offer expert knowledge about the patient’s condition and prognosis. Families provide insight into the patient’s wishes and values.
Working together helps balance medical facts and personal preferences. This collaboration guides decisions about continuing or stopping ventilation support. Trust and understanding are essential for this sensitive process.
Decision Making Process
The decision process involves careful evaluation of the patient’s health. Doctors assess lung function, response to treatment, and overall condition. They consider risks of prolonged ventilation, such as infections or muscle weakness.
Family members share what the patient would want. They discuss quality of life and future goals. Sometimes, ethics committees join to support difficult choices.
Clear steps help avoid confusion:
- Review medical data regularly
- Discuss options openly with family
- Respect patient’s values and wishes
- Plan for different outcomes
Communication Strategies
Good communication reduces stress and misunderstandings. Medical staff use simple words to explain complex issues. They listen carefully to family concerns and questions.
Frequent updates keep everyone informed. Visual aids and written summaries can help understanding. Emotional support plays a key role during talks.
- Hold regular family meetings
- Encourage questions and honest answers
- Use clear, simple language
- Provide emotional and psychological support
This open dialogue builds trust. It helps families feel involved and respected in the care process.

Credit: www.goodrx.com

Credit: www.nejm.org
Frequently Asked Questions
How Long Can A Person Safely Stay On A Ventilator?
A person can typically stay on a ventilator for days to weeks safely. Prolonged use increases risks like infections and lung damage. Doctors continuously evaluate the need for ventilation and aim to wean patients off as soon as possible.
What Are Risks Of Being On A Ventilator Too Long?
Long-term ventilator use can cause lung injury, infections, and muscle weakness. It may also lead to complications like pneumonia and difficulty breathing independently. Medical teams monitor these risks closely to minimize harm and plan timely extubation.
When Should Doctors Consider Removing A Ventilator?
Doctors consider ventilator removal when a patient can breathe independently with stable oxygen levels. Improvement in underlying condition and strength to maintain airway are key factors. Weaning trials help determine readiness for safe ventilator discontinuation.
Can Long Ventilator Use Affect Recovery Time?
Yes, prolonged ventilator use can delay recovery due to muscle weakness and lung issues. It may require longer rehabilitation and respiratory therapy. Early weaning and physical therapy support faster recovery and better outcomes.
Conclusion
Being on a ventilator for too long can cause problems. Doctors watch closely to decide the right time to stop. Each patient’s needs are different. Quick recovery is the goal, but safety matters most. Families should ask questions and stay informed.
Careful decisions help protect health and improve chances. Ventilators save lives but require careful use. Understanding the risks helps everyone prepare better. Always trust medical teams to guide the process.