Have you ever wondered how your lungs manage to bring oxygen into your body so efficiently? The secret lies in a delicate balance called ventilation-perfusion coupling.
At the heart of this process is lung perfusion—how blood flows through your lungs to pick up oxygen. Understanding how lung perfusion works can give you a clearer picture of how your body fuels itself every moment you breathe. Stick with me, and you’ll discover the fascinating dance between air and blood that keeps you alive and thriving.
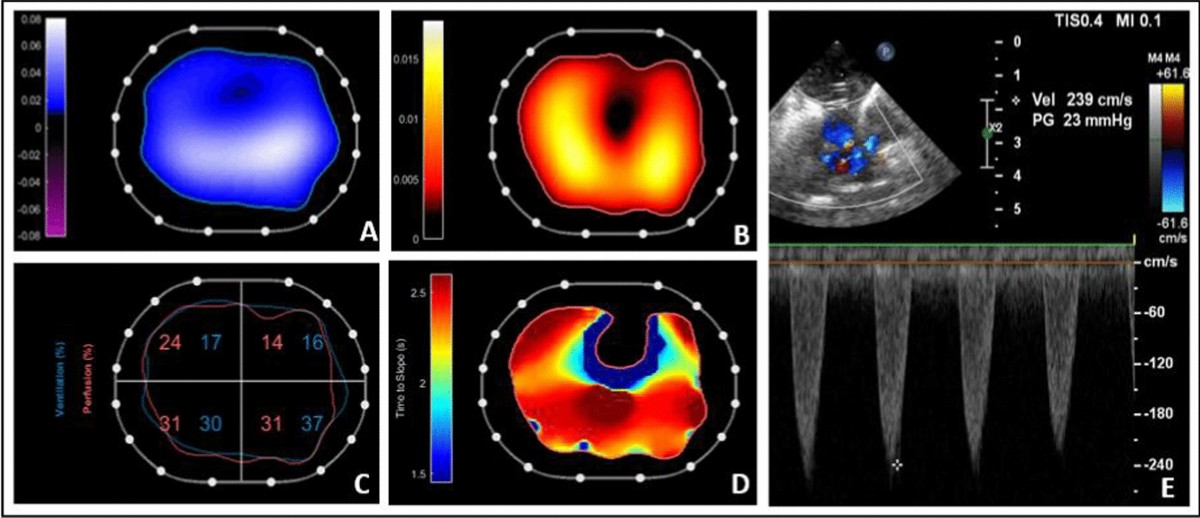
Credit: icm-experimental.springeropen.com
Lung Perfusion Basics
Lung perfusion is a key process that supports breathing. It ensures blood flows through the lungs to pick up oxygen. This oxygen-rich blood then travels to the rest of the body. Understanding lung perfusion basics helps explain how ventilation and perfusion work together for efficient gas exchange.
Blood Flow In The Lungs
Blood enters the lungs through the pulmonary arteries. These arteries carry deoxygenated blood from the heart. Inside the lungs, blood moves through smaller vessels. It reaches tiny blood vessels called capillaries. Proper blood flow is essential for oxygen to enter the blood.
Role Of Pulmonary Capillaries
Pulmonary capillaries are very thin and surround air sacs. They allow oxygen to pass from the air into the blood. At the same time, carbon dioxide moves from the blood to the air sacs. This exchange happens quickly due to the capillaries’ thin walls. Healthy capillaries ensure efficient gas transfer in the lungs.
Ventilation And Perfusion Interaction
Ventilation and perfusion interaction is vital for effective lung function. It ensures that oxygen reaches the blood and carbon dioxide leaves the body efficiently. This interaction depends on how well air reaches the lungs (ventilation) and how well blood flows in lung vessels (perfusion). The balance between these two processes is key for healthy breathing and oxygen supply.
Matching Air And Blood Flow
Air must reach the alveoli where blood vessels surround them. Proper matching means air supply fits blood flow perfectly. If air reaches areas with little blood flow, oxygen cannot enter the blood. If blood flows to areas without air, it carries less oxygen. The lungs adjust blood vessel size to match air supply. This keeps the ventilation and perfusion balanced for better gas exchange.
Impact On Gas Exchange
Good matching improves oxygen absorption and carbon dioxide removal. Poor matching leads to low oxygen in the blood. It can cause breathlessness and reduce energy. The lungs constantly monitor and adjust ventilation and perfusion. This ensures the body gets enough oxygen to work well. Proper interaction supports all body organs and keeps us healthy.
Mechanisms Regulating Perfusion
The regulation of lung perfusion is vital for efficient gas exchange. It ensures that blood flows to areas of the lung with enough oxygen. This balance helps the body maintain proper oxygen levels. The body uses several mechanisms to adjust blood flow in the lungs. These mechanisms react quickly to changes in oxygen levels and other signals. Understanding these processes helps explain how the lungs work well in different conditions.
Hypoxic Pulmonary Vasoconstriction
Hypoxic pulmonary vasoconstriction (HPV) is a key mechanism in lung perfusion. It occurs when blood vessels in low-oxygen areas of the lung narrow. This narrowing reduces blood flow to poorly ventilated regions. Blood is then redirected to parts of the lung with higher oxygen levels. This process improves oxygen uptake by matching blood flow to air supply. HPV helps prevent wasted blood flow and maintains efficient breathing.
Neural And Chemical Influences
The nervous system also controls lung perfusion. Nerves can cause blood vessels to widen or narrow. This action adjusts blood flow based on body needs. Chemical signals like oxygen and carbon dioxide levels affect these nerves. Hormones and local chemicals also influence vessel size. Together, neural and chemical signals fine-tune lung blood flow. They ensure the lungs respond quickly to changes in the body’s oxygen demand.
Factors Affecting Perfusion Efficiency
Perfusion efficiency plays a vital role in how well the lungs deliver blood to the alveoli. Several factors influence this process, shaping how oxygen and carbon dioxide exchange occurs. Understanding these factors helps explain variations in lung function across different situations.
Gravity And Body Position
Gravity affects blood flow in the lungs by pulling blood toward the lower regions. When a person stands, blood pools more at the lung bases. Lying down shifts this distribution depending on the body position.
Different positions change which lung areas receive more blood. For example:
- In a supine position, blood flow spreads more evenly across the lungs.
- In a side-lying position, the lung on the lower side gets more perfusion.
This shift impacts how well ventilation and perfusion match. It also influences oxygen levels in the blood.
Lung Diseases Impact
Certain lung diseases reduce perfusion efficiency by damaging blood vessels or alveoli. Conditions like pulmonary embolism block blood flow in lung arteries. This stops blood from reaching parts of the lung.
Diseases such as chronic obstructive pulmonary disease (COPD) cause inflammation and narrowing of airways. This lowers airflow and disturbs the balance of ventilation and perfusion.
Pulmonary fibrosis thickens lung tissue, making gas exchange harder. These conditions cause mismatch and lower oxygen delivery to the body.
Measuring Lung Perfusion
Measuring lung perfusion is a vital aspect of understanding ventilation-perfusion coupling. It’s essential for diagnosing and managing various respiratory conditions. With the right techniques and tools, healthcare professionals can get a detailed look at how well blood flows through the lungs.
Imaging Techniques
Imaging techniques are at the forefront of measuring lung perfusion. Technologies like CT scans and MRI offer a non-invasive window into the body. These methods provide high-resolution images, allowing doctors to pinpoint areas where blood flow might be compromised.
Another popular imaging method is the use of nuclear medicine scans, such as a V/Q scan. This involves inhaling a radioactive gas and injecting a radioactive substance into the bloodstream. The resulting images reveal how well air and blood are distributed throughout the lungs.
Each imaging technique has its own advantages and limitations. For example, while CT scans provide detailed images, they expose patients to radiation. MRI, on the other hand, avoids this but can be less accessible due to cost and availability.
Clinical Assessment Methods
Clinical assessment methods complement imaging techniques in evaluating lung perfusion. These often involve physical examinations and listening to lung sounds using a stethoscope. Simple yet effective, these methods can offer immediate insights into a patient’s lung condition.
Blood gas analysis is another key clinical method. By examining the levels of oxygen and carbon dioxide in the blood, doctors can infer how well the lungs are functioning. This test provides crucial data on lung efficiency and perfusion status.
Pulse oximetry is a common, non-invasive tool used in clinical settings. It measures oxygen saturation in the blood, offering a quick snapshot of respiratory health. While not as detailed as imaging, it’s invaluable for real-time monitoring.
How do you think these methods might evolve with technology? The future of measuring lung perfusion could hold even more precise and less invasive techniques. Staying informed ensures the best care and outcomes for patients.

Credit: quizlet.com
Clinical Relevance Of Perfusion
Perfusion plays a vital role in lung function and overall respiratory health. It involves the flow of blood through the lung’s capillaries, allowing oxygen to enter the blood and carbon dioxide to leave. Proper perfusion ensures that oxygen reaches the body’s tissues efficiently. Disruptions in perfusion can lead to serious health problems. Understanding its clinical relevance helps in diagnosing and treating many lung conditions.
Perfusion In Respiratory Disorders
Many lung diseases affect perfusion and disturb ventilation-perfusion balance. Conditions like pulmonary embolism block blood flow in the lungs. This blockage reduces oxygen delivery to the body. Chronic obstructive pulmonary disease (COPD) also alters perfusion by damaging lung tissue. In pneumonia, inflammation causes fluid buildup, impairing blood flow. Poor perfusion worsens symptoms like shortness of breath and low oxygen levels. Monitoring perfusion helps doctors assess disease severity and plan treatment.
Therapeutic Approaches
Treatments often target improving lung perfusion and oxygen delivery. Oxygen therapy increases the amount of oxygen in the blood. Medications like anticoagulants prevent blood clots and improve blood flow. In severe cases, surgery may remove blockages or damaged lung parts. Physical therapy and breathing exercises support better lung function. Newer therapies focus on restoring normal ventilation-perfusion matching to enhance breathing efficiency. Early intervention can prevent complications and improve quality of life.

Credit: www.mdpi.com
Frequently Asked Questions
What Is Lung Perfusion In Ventilation Perfusion Coupling?
Lung perfusion is the blood flow through lung capillaries. It delivers oxygen-poor blood to alveoli for oxygen exchange, crucial in ventilation-perfusion coupling.
How Does Ventilation Affect Lung Perfusion?
Ventilation supplies air to alveoli, influencing blood flow. Proper ventilation ensures optimal perfusion for efficient gas exchange in lungs.
Why Is Ventilation-perfusion Coupling Important?
It matches airflow and blood flow in lungs, maximizing oxygen uptake. This balance maintains healthy respiratory function and prevents blood oxygen deficits.
What Happens If Lung Perfusion Is Impaired?
Impaired perfusion reduces oxygen delivery to blood. It can cause hypoxia, respiratory distress, and disrupt ventilation-perfusion balance, affecting overall lung efficiency.
Conclusion
Lung perfusion plays a key role in how our lungs work. It helps match blood flow to the air we breathe in. This balance makes sure oxygen reaches the body well. Poor perfusion can lead to breathing problems and low oxygen.
Understanding this process helps us see how lungs keep us healthy. It also shows why doctors check lung function carefully. Keeping this system working right is important for good health. Simple steps like avoiding smoking can protect lung perfusion. Healthy lungs mean better energy and easier breathing every day.





