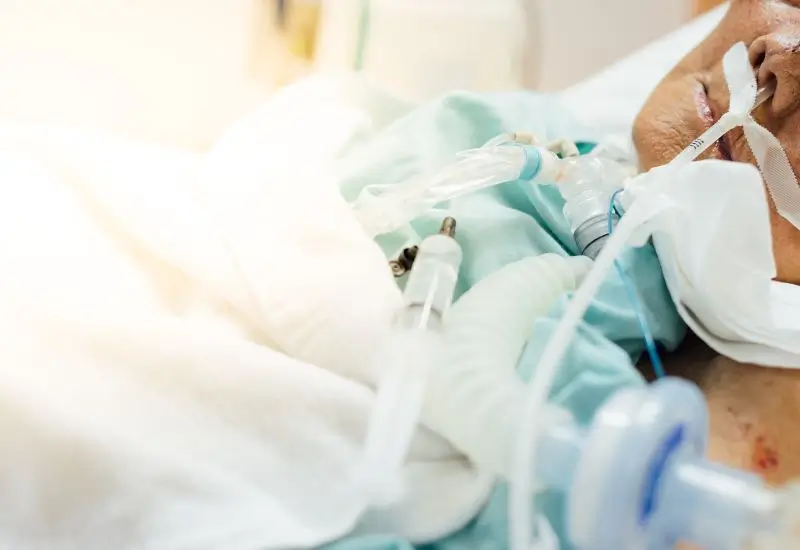
If you or someone you care about has been on a ventilator, you might be wondering what comes next. The experience can be overwhelming, and recovery often brings many questions and challenges.
Knowing what to expect after being on a ventilator can help you feel more in control and prepared. This article will guide you through the common steps of recovery, what changes you might notice, and how to support your healing process.
Keep reading to understand what lies ahead and how to navigate it with confidence.

Credit: www.apexhospitals.com
Physical Recovery
Physical recovery after being on a ventilator can be challenging, but understanding what to expect helps you take control of your healing journey. Your body has been through a lot, and it needs time and care to regain strength and function. Let’s look closely at key areas that often need attention during this phase.
Muscle Weakness And Fatigue
After being on a ventilator, many people experience muscle weakness and fatigue. Your muscles may feel weak because they haven’t been used much during ventilation. Simple tasks like walking or lifting your arms might feel exhausting at first.
It’s important to start moving gently, even if it’s just sitting up or stretching your legs. Physical therapy can help you regain strength step by step. Have you noticed how small movements gradually make daily activities easier?
Breathing Exercises And Lung Health
Your lungs need extra attention once you come off the ventilator. Breathing exercises can improve lung capacity and clear out mucus. Techniques like deep breathing or using an incentive spirometer can make a big difference.
Try setting aside time each day for these exercises, and notice any improvement in your breathing. Have you felt your breath becoming steadier with regular practice?
Managing Pain And Discomfort
Pain and discomfort are common after being on a ventilator, especially around the neck or chest area where the tube was placed. Managing this pain is crucial for your overall recovery and mobility.
Discuss pain relief options with your healthcare provider and don’t hesitate to ask for help. Using heat packs, gentle massage, or prescribed medication can ease discomfort and help you move more freely. What strategies have you found most helpful in managing your pain?
Credit: www.theglobeandmail.com
Emotional And Mental Health
Recovering from a ventilator can be tough on your mind and emotions. Many people feel scared, confused, or sad after this experience. It is normal to face emotional and mental challenges during recovery. Understanding these feelings helps you handle them better. Support and care play a big role in healing your mental health.
Coping With Anxiety And Depression
Anxiety and depression often appear after being on a ventilator. You might feel restless, worried, or very tired. Some days can feel harder than others. Simple steps can help ease these feelings:
- Practice deep breathing or relaxation exercises.
- Talk about your feelings with trusted people.
- Keep a daily routine to bring normalcy.
- Engage in light activities to boost mood.
Remember, these feelings do not last forever. Seeking help early improves your recovery.
Post-traumatic Stress Symptoms
Ventilator use can cause post-traumatic stress symptoms. Nightmares, flashbacks, or feeling jumpy are common signs. You may avoid places or thoughts related to the hospital stay. These symptoms can last weeks or months. Recognizing them is the first step to healing.
Talk openly about what you remember and how you feel. Write down your thoughts or share them with a counselor. These actions can reduce the power of traumatic memories over time.
Support Systems And Counseling
Support systems are key to mental health recovery. Family, friends, and support groups provide comfort and understanding. Professional counseling offers safe space to explore emotions.
- Counselors teach coping skills for stress and fear.
- Group therapy connects you with others with similar experiences.
- Online forums offer 24/7 support and advice.
Do not hesitate to ask for help. Emotional care is as important as physical healing.
Nutrition And Hydration
After being on a ventilator, your body needs extra care to rebuild strength and support healing. Nutrition and hydration play a crucial role in this recovery journey. Understanding how to manage these aspects can help you regain energy and improve your overall well-being.
Importance Of Proper Nutrition
Your body works hard to heal after ventilator use, and it needs the right fuel. Eating a balanced diet with enough protein supports muscle repair, especially for your lungs and respiratory muscles.
Include foods like chicken, fish, eggs, beans, and dairy to meet your protein needs. Also, don’t forget fruits and vegetables for essential vitamins and minerals that boost your immune system.
Have you noticed how small meals throughout the day make eating easier? Try eating smaller portions more frequently if large meals feel overwhelming.
Hydration Tips For Recovery
Hydration is often overlooked but is vital for recovery. Water helps thin mucus in your lungs, making breathing easier and reducing the risk of infection.
Aim to drink at least 8 cups of fluids daily. You can include water, herbal teas, and broth-based soups to stay hydrated.
If drinking plain water feels boring, try adding slices of lemon or cucumber for flavor without extra calories.
Supplements And Vitamins
Sometimes, your diet alone might not provide all the nutrients you need. Supplements can fill gaps and support your recovery process.
Vitamin D and calcium are important for bone health, especially if you were inactive for a while. Vitamin C helps with immune function and wound healing.
Before starting any supplements, talk to your healthcare provider to make sure they are safe and appropriate for you.
Physical Therapy And Mobility
After being on a ventilator, physical therapy plays a crucial role. It helps patients regain their strength and mobility. This process involves tailored exercises and activities. These help restore physical functions and enhance recovery.
Rebuilding Strength
Rebuilding strength is a primary goal in physical therapy. Patients often experience muscle weakness after prolonged bed rest. Therapists design specific exercises to target weakened muscles. These exercises gradually increase in intensity as strength improves. Consistent practice is essential for effective recovery. Strengthening exercises may include light weightlifting or resistance bands. These help patients regain muscle mass and endurance.
Range Of Motion Exercises
Range of motion exercises are vital for joint flexibility. They involve moving joints in specific directions to prevent stiffness. These exercises improve circulation and reduce pain. Therapists guide patients through gentle stretching routines. Regular practice enhances joint mobility and functional movement. Simple activities like arm lifts or leg bends are common. Such movements help maintain joint health and flexibility.
Preventing Complications
Physical therapy also focuses on preventing complications. Prolonged immobility can lead to issues like bed sores or blood clots. Therapists implement strategies to minimize these risks. Encouraging regular movement and position changes is key. They may also use equipment like special cushions or compression garments. These tools support patient comfort and safety during recovery.
Follow-up Care
After being on a ventilator, follow-up care is essential for full recovery. It helps track health progress and prevents complications. Patients often need ongoing support to regain strength and lung function.
Regular Medical Checkups
Doctors schedule frequent visits to monitor recovery. These checkups help catch any new or worsening issues early. Patients should attend all appointments for best care.
Monitoring Lung Function
Lung tests measure how well the lungs work after ventilation. These tests guide treatment and breathing exercises. Regular monitoring helps detect any lasting lung damage.
Medication Management
Medications may be needed to control symptoms or prevent infections. Doctors adjust medicines based on recovery progress and test results. Patients must follow prescriptions carefully and report side effects.
Common Challenges
After being on a ventilator, you may face several challenges that affect your daily life and recovery. These common issues can be surprising and frustrating, but understanding them helps you prepare and manage better. Here’s what you might expect and how to handle these difficulties.
Dealing With Fatigue
Fatigue after ventilation is more than just feeling tired. Your body has been through a lot, and energy levels can remain low for weeks or even months.
You might notice that simple tasks like walking or climbing stairs drain you quickly. It helps to pace yourself and take frequent breaks.
Have you considered keeping a daily journal to track your energy peaks and plan activities accordingly? This small step can make a big difference in managing your day.
Sleep Disturbances
Many people find their sleep patterns disrupted after ventilation. You might struggle to fall asleep or wake up frequently during the night.
Creating a calming bedtime routine and avoiding screens before sleep can improve rest quality. If sleep problems persist, talk to your healthcare provider about possible treatments.
Ask yourself if your bedroom environment supports good sleep—dark, quiet, and cool rooms often help promote better rest.
Cognitive Changes
You may experience memory lapses, trouble concentrating, or slower thinking after coming off a ventilator. This is sometimes called “brain fog.”
Engaging in simple mental exercises like puzzles or reading can gradually boost your cognitive function. Be patient with yourself; recovery in this area takes time.
Have you noticed if certain activities make thinking easier or harder? Identifying these triggers can guide you to better manage your daily tasks.
Tips For Caregivers
Caring for someone after a ventilator can be challenging. The person may feel weak and scared. Caregivers play a key role in recovery. They help with physical needs and emotional healing. Here are simple tips to support both the patient and yourself.
Providing Emotional Support
Being on a ventilator can feel lonely and frightening. Offer kind words and patience. Listen carefully to their feelings. Show you care without rushing them. Small acts like holding hands can calm anxiety. Encourage hope and positive thoughts every day.
Assisting With Daily Activities
The patient may need help with basic tasks. This includes bathing, dressing, and eating. Keep a routine to create comfort and predictability. Encourage independence but be ready to assist. Use gentle motions and speak clearly. Respect their pace and offer breaks often.
Recognizing Warning Signs
Watch for changes in breathing or alertness. Call for help if the patient:
- Has difficulty breathing or fast breaths
- Shows confusion or extreme sleepiness
- Develops a fever or cough
- Has chest pain or swelling
Early action can prevent serious problems. Keep emergency numbers and medical info handy. Stay calm and focused during any concerns.

Credit: www.getinge.com
Frequently Asked Questions
What Physical Challenges Occur After Ventilator Use?
After ventilator use, patients often face muscle weakness and fatigue. Breathing can feel difficult initially. Physical therapy helps regain strength and lung function efficiently.
How Long Does Recovery Take Post-ventilator?
Recovery time varies widely, usually from weeks to months. Factors include age, overall health, and illness severity. Consistent medical care and rehab improve recovery speed.
Will I Need Respiratory Therapy After Ventilator Removal?
Many patients benefit from respiratory therapy post-ventilator. It aids lung healing, improves breathing, and prevents complications. Therapy plans are personalized based on patient needs.
Can Mental Health Be Affected After Ventilator Use?
Yes, anxiety, depression, and PTSD are common after ventilator use. Psychological support and counseling are vital for emotional recovery and wellbeing.
Conclusion
Recovering after being on a ventilator takes time and patience. Your body needs rest to heal and regain strength. You may feel weak or tired at first. Breathing exercises and physical therapy help improve lung function. Support from family and healthcare providers is important.
Small steps lead to big progress. Stay positive and follow your doctor’s advice. Every day brings a little more strength. Recovery is a journey, not a race. Keep focusing on your health and healing.