Are you struggling to understand why your ventilator isn’t working as smoothly as it should? Breath stacking can be a hidden problem that makes breathing uncomfortable and even dangerous for patients relying on ventilators.
If you’ve noticed unusual breathing patterns or alarms going off, it’s crucial to act quickly. You’ll discover simple, effective steps to fix breath stacking on a ventilator. By the end, you’ll feel confident in managing this issue and improving patient comfort and safety.
Keep reading to learn exactly what to do when breath stacking happens.
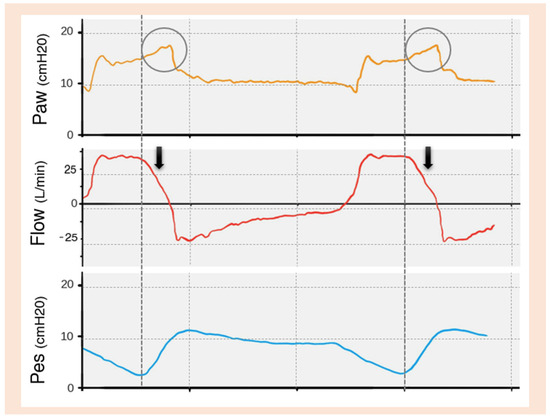
Credit: www.mdpi.com
Causes Of Breath Stacking
Breath stacking on a ventilator can be a serious issue, leading to discomfort and potential lung injury. Understanding the causes is essential to fix it effectively. Let’s break down the main factors that often contribute to this problem so you can better identify and address them.
Ventilator Settings Impact
The way the ventilator is set plays a crucial role in breath stacking. If the inspiratory time is too long or the expiratory time too short, the next breath may start before the lungs have fully emptied. This overlap causes air to stack, increasing pressure inside the lungs.
Improper trigger sensitivity can also cause problems. If the ventilator is set to trigger breaths too quickly, it may deliver breaths on top of each other. Have you checked if your settings allow enough time for full exhalation before the next breath begins?
Patient-related Factors
Your patient’s condition can also influence breath stacking. Patients with obstructive lung diseases, like COPD or asthma, often have delayed exhalation. This makes it harder for them to fully exhale before the ventilator initiates the next breath.
Additionally, patient effort can vary. If the patient initiates breaths more rapidly than the ventilator expects, breath stacking can occur. Are you monitoring your patient’s respiratory rate and effort closely enough to spot this mismatch?
Equipment Malfunctions
Sometimes, the cause lies in the ventilator equipment itself. Faulty valves or leaks in the circuit can disrupt normal airflow and timing. This disruption can prevent complete exhalation, leading to air trapping and breath stacking.
Regular equipment checks can prevent these issues. Have you inspected your ventilator circuits for leaks or malfunctioning parts recently? Small defects often go unnoticed until symptoms like breath stacking emerge.
Identifying Breath Stacking
Identifying breath stacking is crucial for patients on ventilators. Breath stacking happens when breaths overlap, causing discomfort and poor ventilation. Early detection helps prevent lung injury and improves patient care.
Clinical Signs
- Increased breathing effort or visible distress
- Rapid shallow breathing or irregular breathing pattern
- Elevated heart rate or blood pressure changes
- Use of accessory muscles for breathing
- Decreased oxygen saturation or cyanosis
Monitoring Techniques
- Continuous observation of ventilator waveforms
- Checking for incomplete exhalation before next breath
- Assessing pressure and flow curves for abnormalities
- Regular auscultation of lung sounds for wheezing or crackles
- Monitoring patient comfort and synchrony with the ventilator
Diagnostic Tools
- Capnography to measure exhaled carbon dioxide levels
- Pulse oximetry for oxygen saturation trends
- Chest X-rays to assess lung expansion and volume
- Arterial blood gas analysis for ventilation status
- Ventilator software reports for breath timing and volume
Adjusting Ventilator Settings
Adjusting ventilator settings plays a key role in fixing breath stacking. This issue happens when breaths overlap, causing discomfort and poor ventilation. Fine-tuning the machine helps ensure each breath is delivered fully and safely. Small changes can make a big difference in patient comfort and lung function.
Tidal Volume Modifications
Tidal volume is the amount of air delivered in each breath. Reducing tidal volume can prevent over-inflation of the lungs. It lowers the risk of breath stacking by allowing more time for full exhalation. Increase tidal volume cautiously, only if the patient requires more air. Always monitor lung pressure and patient response closely.
Respiratory Rate Adjustments
Respiratory rate controls how many breaths the ventilator gives per minute. Lowering the rate gives more time for the lungs to empty before the next breath. This reduces breath stacking risk and improves ventilation efficiency. Raising the rate may worsen breath stacking. Adjust the rate based on patient comfort and blood gas results.
Inspiratory Time Changes
Inspiratory time is how long each breath lasts during inhalation. Shortening inspiratory time allows more time for exhalation. This helps prevent breaths from overlapping. Lengthening inspiratory time may cause breath stacking by reducing exhalation time. Adjust inspiratory time carefully to balance adequate oxygen delivery and complete exhalation.

Credit: ccforum.biomedcentral.com
Addressing Patient Factors
Addressing patient factors is crucial when fixing breath stacking on a ventilator. These factors directly influence how well the ventilator synchronizes with the patient’s breathing. Understanding and managing them can reduce discomfort and improve ventilation effectiveness.
Sedation And Comfort
Ensuring your patient is comfortable can prevent breath stacking. Anxiety or pain often causes irregular breathing patterns, making synchronization difficult. Adjusting sedation levels carefully can calm the patient without suppressing their respiratory drive.
Have you noticed that a lightly sedated patient breathes more smoothly? It’s a balance between too much and too little sedation. Tailoring sedation to each patient’s needs helps minimize breath stacking and improves overall comfort.
Managing Airway Resistance
High airway resistance can cause incomplete exhalation, leading to breath stacking. Check for mucus buildup, bronchospasm, or tube kinks that increase resistance. Clearing secretions and using bronchodilators can make a significant difference.
Simple interventions, like suctioning or repositioning the tube, often reduce resistance effectively. Don’t overlook the impact of small airway issues on ventilator performance. What small changes could you make now to lower airway resistance?
Improving Lung Compliance
Poor lung compliance means the lungs are stiff and harder to inflate, which can cause breath stacking. Treating underlying conditions such as pneumonia, edema, or fibrosis improves lung flexibility. Using appropriate ventilator settings tailored to lung mechanics is key.
Have you adjusted PEEP or tidal volume based on compliance changes recently? Even subtle improvements in lung compliance can reduce breath stacking episodes. Focus on optimizing lung conditions alongside ventilator settings for best results.
Equipment Checks And Maintenance
Fixing breath stacking on a ventilator involves checking the settings and ensuring proper patient-ventilator synchronization. Regular equipment checks can prevent issues. Maintenance and timely adjustments can enhance patient comfort and safety.
Ensuring your ventilator equipment is functioning correctly is crucial to prevent breath stacking. Routine checks and maintenance can significantly enhance performance and reliability. Regular maintenance not only extends the life of your equipment but also ensures patient safety.Inspecting Tubing And Valves
The tubing and valves in a ventilator play a pivotal role in air delivery. Regular inspections can help you spot any wear or damage early. Look for any cracks, leaks, or blockages that could impede airflow. A friend once shared how a simple tear in the tubing went unnoticed and led to inconsistent ventilation. By inspecting your tubing regularly, you can prevent such issues.Ensuring Proper Alarm Settings
Alarm settings are your first line of defense against potential ventilator mishaps. Make sure they are set accurately to alert you to any irregularities. Consider what could happen if an alarm doesn’t sound when needed. Are the alarms configured to your patient’s specific needs? Double-checking these settings can make a significant difference in emergency situations.Regular Device Calibration
Calibration is essential for accurate ventilator performance. Regular calibration ensures that the ventilator provides the correct volume and pressure of air. A healthcare professional once mentioned how regular calibration helped maintain the precision of their devices. Are you scheduling these calibrations frequently enough? Keeping a log of calibration dates can help you stay on top of this critical task. Engage with your equipment actively. Regular maintenance and checks can prevent many common ventilator issues, ensuring optimal performance and patient safety.
Credit: www.liebertpub.com
Advanced Therapies And Techniques
Advanced therapies and techniques offer powerful tools to manage breath stacking on a ventilator effectively. These approaches go beyond basic settings and require a deeper understanding of respiratory mechanics. Implementing them correctly can significantly improve patient comfort and ventilation efficiency.
Use Of Peep And Cpap
Positive End-Expiratory Pressure (PEEP) helps keep the airways open at the end of expiration, reducing the risk of breath stacking. By maintaining a baseline pressure, PEEP prevents alveolar collapse and promotes better oxygen exchange.
Continuous Positive Airway Pressure (CPAP) provides a constant pressure throughout the breathing cycle, which can stabilize breathing patterns. Adjusting PEEP or CPAP levels carefully is crucial—too high can cause overdistension, too low may not prevent breath stacking.
Alternative Ventilation Modes
Switching to different ventilation modes can directly address breath stacking. Modes like Pressure Support Ventilation (PSV) or Adaptive Support Ventilation (ASV) allow more patient control over breath timing and volume.
These modes adjust support based on patient effort, reducing the chance of overlapping breaths. If you’ve struggled with fixed ventilation settings, trying alternative modes might be the key to smoother breathing cycles.
Recruitment Maneuvers
Recruitment maneuvers temporarily increase airway pressure to open collapsed lung areas. This can improve lung compliance and reduce areas prone to breath stacking.
However, these maneuvers must be used with caution and monitored closely due to risks like barotrauma. Have you considered how carefully timed recruitment maneuvers could enhance your patient’s ventilation without causing harm?
Preventing Breath Stacking
Preventing breath stacking is key to safe ventilator care. It reduces risks and improves patient comfort. Proper prevention helps avoid lung injury and other complications.
Routine Monitoring Protocols
Regular checks of ventilator settings are essential. Monitor tidal volume, respiratory rate, and airway pressure closely. Use alarms to detect abnormal breathing patterns early. Document patient responses to ventilation frequently. Adjust settings based on continuous assessment to prevent breath stacking.
Staff Training And Education
Train healthcare staff on ventilator management basics. Emphasize recognizing signs of breath stacking quickly. Provide clear guidelines for ventilator adjustments. Encourage teamwork and communication during patient care. Ongoing education ensures updated knowledge and skills.
Early Intervention Strategies
Act promptly at the first sign of breath stacking. Use sedation carefully to reduce patient-ventilator asynchrony. Adjust inspiratory time and flow rates to match patient needs. Consider non-invasive support if appropriate. Early actions prevent worsening and promote better outcomes.
Frequently Asked Questions
What Causes Breath Stacking On A Ventilator?
Breath stacking occurs due to incomplete exhalation before the next breath. It often results from high respiratory rates or airway obstruction. Identifying the cause helps tailor ventilator settings and prevent complications like lung overdistension.
How Can Ventilator Settings Reduce Breath Stacking?
Adjusting tidal volume, respiratory rate, and inspiratory flow can minimize breath stacking. Increasing expiratory time allows full exhalation. Careful monitoring ensures optimal settings and patient comfort while preventing breath stacking.
What Are Signs Of Breath Stacking In Patients?
Look for increased airway pressure, decreased oxygen saturation, and patient distress. Breath stacking may cause difficulty in ventilator cycling and abnormal lung sounds. Early detection is vital for timely intervention.
Can Sedation Help Manage Breath Stacking?
Yes, sedation can reduce patient-ventilator asynchrony, which may cause breath stacking. Proper sedation levels improve comfort and synchronization, decreasing the risk of breath stacking and related complications.
Conclusion
Fixing breath stacking on a ventilator improves patient comfort and safety. Adjust ventilator settings carefully and monitor breathing patterns closely. Communicate with healthcare providers to address issues quickly. Small changes can prevent serious problems. Stay patient and check equipment regularly.
Breath stacking is manageable with the right approach. Keep learning and stay attentive to the patient’s needs. Care and precision matter most in ventilator management.





