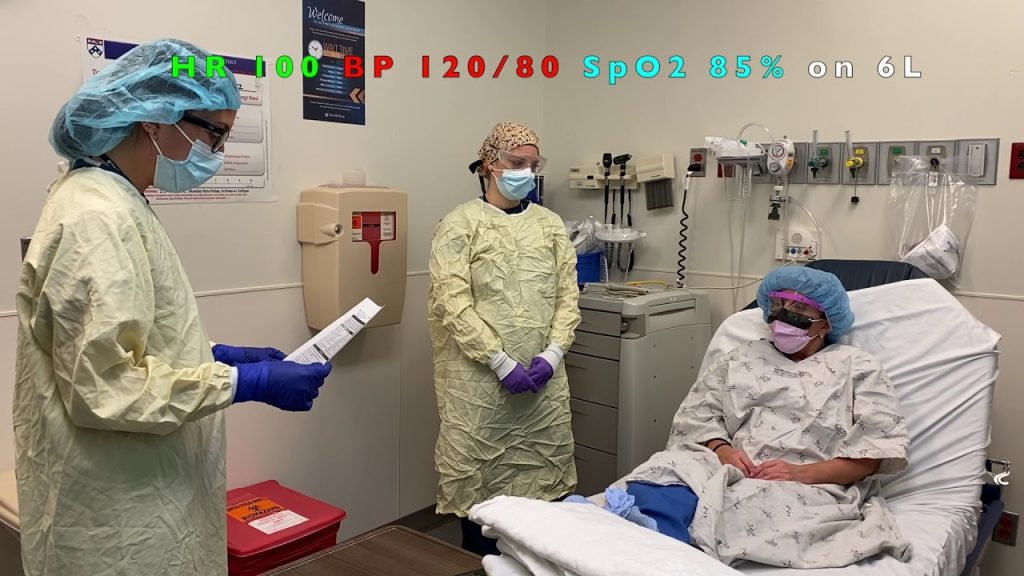
Have you ever wondered what it feels like to be awake while on a ventilator? If you or a loved one is facing this situation, it can bring up a mix of fear, confusion, and questions.
You might worry about comfort, awareness, and what to expect during this critical time. Understanding what happens when you are awake on a ventilator can ease your mind and help you feel more in control. Keep reading to discover what you need to know about this experience and how it affects you.

Credit: www.theguardian.com
Being Awake While On A Ventilator
Being awake while on a ventilator can feel overwhelming. You might imagine it as being trapped in a machine, unable to speak or move freely. Yet, many patients find ways to stay mentally present and even communicate despite the challenges.
Why Patients Stay Awake
Many people on ventilators remain awake because their medical condition doesn’t require deep sedation. Doctors often aim to keep patients conscious to monitor their neurological status and avoid the risks linked to heavy sedation.
Sometimes, staying awake helps you participate in your own care. You might be able to follow simple commands or express discomfort, which can improve your treatment and recovery.
Have you ever wondered how awareness during such a critical time affects your sense of control? Being awake might actually give you a chance to stay connected with your surroundings.
Common Experiences
Patients on ventilators often report feeling anxious or frustrated because they cannot speak. However, many learn to use gestures or communication boards to express their needs.
Some describe strange sensations like dry mouth, difficulty swallowing, or a constant need to clear their throat. These feelings can be uncomfortable but usually improve with time and care.
You might also notice moments of confusion or vivid dreams, especially if medications are involved. These experiences can be unsettling but talking about them with your care team can help.
- Difficulty speaking but able to communicate non-verbally
- Feeling scared but also aware of the support around you
- Physical discomfort such as muscle weakness or dry mouth
- Fluctuating awareness due to medications or illness
What would you want your medical team to know about how you feel while awake on a ventilator? Sharing your experience could improve care for yourself and others.
How Ventilators Work
Understanding how ventilators work can help you grasp what happens when someone is awake while using one. Ventilators are machines designed to assist or completely take over the breathing process. They deliver oxygen to the lungs and help remove carbon dioxide, which is vital when the body cannot breathe properly on its own.
Types Of Ventilators
Ventilators come in different types, each suited for specific medical needs. Some are designed for short-term use, like during surgery or severe illness, while others support long-term breathing difficulties.
- Invasive Ventilators:These require a tube inserted into the windpipe. They provide full breathing support but usually require sedation.
- Non-invasive Ventilators:These use masks or nasal plugs to help you breathe. They allow you to stay awake and communicate more easily.
- Portable Ventilators:Smaller and lighter, these are used for patients who need breathing support outside of hospital settings.
Have you ever wondered which type might be used if you or a loved one needed breathing support?
Breathing Support Mechanisms
Ventilators assist breathing by pushing air into the lungs and then allowing it to flow out naturally or with assistance. The machine controls the volume, pressure, and timing of each breath to match your body’s needs.
- Volume-Controlled Breathing:The ventilator delivers a set amount of air with each breath, ensuring consistent lung inflation.
- Pressure-Controlled Breathing:The machine regulates the pressure of the air going into the lungs to prevent damage from too much force.
- Assisted Breathing:The ventilator senses when you try to breathe and helps by providing extra air, allowing you to remain awake and somewhat independent.
Imagine how it feels to have a machine sync with your own breathing efforts. This connection can make a big difference in comfort and awareness during ventilation.
Sedation And Comfort
Being awake on a ventilator can feel strange and uncomfortable. Sedation helps ease anxiety and pain while keeping the patient calm. Comfort is a top priority for doctors and nurses. They use different medicines to help patients relax without losing control. Understanding sedation can help patients and families feel more at ease during this tough time.
Sedation Options
Doctors choose sedation based on how much support the patient needs. Common sedation types include:
- Light sedation: Helps patients stay calm and relaxed, but aware.
- Moderate sedation: Patients feel sleepy but can respond to simple commands.
- Deep sedation: Patients are mostly unconscious and unaware of surroundings.
Medicines used can include opioids for pain and benzodiazepines for anxiety. Some patients receive a mix to balance effects. Nurses carefully watch vital signs and adjust doses to keep sedation safe and effective.
Balancing Awareness And Comfort
It is important to find the right balance between comfort and awareness. Too much sedation can cause confusion or longer recovery. Too little can lead to discomfort and stress.
Medical teams aim to keep patients calm without complete unconsciousness. This approach helps patients communicate needs and cooperate with care. Family support and clear explanations can also improve comfort and reduce fear.
Risks Of Being Awake
Being awake while on a ventilator brings a unique set of risks that many don’t expect. Your body and mind face challenges that go beyond the usual concerns of critical illness. Understanding these risks can help you prepare and cope better if you or a loved one experiences this situation.
Physical Challenges
Staying awake on a ventilator means your muscles, especially those used for breathing, may feel weak and tired. The ventilator does most of the work, but your body still has to adjust, which can cause discomfort and fatigue.
You might experience sore throat or mouth dryness from the breathing tube. Movement restrictions can also lead to stiffness and pressure sores because you can’t change positions easily.
- Muscle weakness due to inactivity
- Discomfort from the breathing tube
- Risk of pressure sores from limited movement
- Difficulty swallowing or speaking
Have you ever felt trapped in your own body? This physical limitation can make recovery feel even harder.
Emotional Impact
Being awake and aware while connected to a machine can be frightening. Anxiety and fear often rise because you understand what’s happening but feel powerless to change it.
Many patients report feelings of isolation, even when surrounded by medical staff. The noise of the ventilator and hospital environment can increase stress and disrupt sleep, deepening emotional strain.
- Increased anxiety and fear
- Feelings of loneliness and isolation
- Stress from hospital noises and interruptions
- Potential for depression or PTSD
Imagine knowing you’re fighting for every breath but feeling completely alone. How would that affect your hope and will to get better?
Communication While Awake
Being awake on a ventilator can be overwhelming. Communication can seem challenging. But it’s important for expressing needs and emotions. Patients can use non-verbal methods and technology to communicate. These methods help bridge the gap between patient and caregiver.
Non-verbal Methods
Non-verbal communication is essential for ventilated patients. Gestures like nodding or shaking the head convey simple messages. Patients can also use hand signals to indicate needs or feelings. Writing on a whiteboard is another effective method. It allows patients to share thoughts without speaking.
Facial expressions also play a crucial role. Smiles, frowns, or raised eyebrows can express emotions. Caregivers should pay attention to these subtle cues. Understanding these signals improves patient comfort and care.
Technology Aids
Technology offers tools to assist communication. Tablets and smartphones can have communication apps. These apps convert text into speech. They help patients express complex thoughts easily.
Eye-tracking technology is another helpful tool. It allows patients to select words or phrases using eye movements. This method provides a voice for those unable to speak. Specialized keyboards can also aid communication. They allow typing with minimal physical movement. These technologies enhance communication and improve patient experience.

Credit: www.respirehomecare.com
Coping Strategies
Coping with being awake on a ventilator can feel overwhelming. The experience affects the mind and body deeply. Managing stress and emotions plays a key role in recovery. Simple strategies can help ease anxiety and build strength. Support from others also brings comfort and hope.
Mental Health Support
Feeling scared or confused is normal. Talking to a therapist can help sort these feelings. Mental health professionals offer tools to manage fear and sadness. Meditation and breathing exercises calm the mind and reduce stress. Keeping a journal helps express thoughts clearly. Rest and sleep improve emotional well-being. Small, positive thoughts can lift the spirit every day.
Family And Caregiver Roles
Family and caregivers provide more than physical care. Their presence gives emotional support and reassurance. Simple acts like holding hands or speaking softly help patients feel safe. Caregivers should learn to recognize signs of distress. Patience and kindness build trust and comfort. Families can help by sharing updates with medical staff. Encouraging small progress boosts morale for both sides.
What To Expect During Recovery
Recovering from being on a ventilator can feel overwhelming, but knowing what to expect helps you stay prepared and focused. Your body has been through a lot, and the road to normal breathing involves several important steps. Understanding these phases can make you feel more in control and ready to face each challenge.
Weaning Off The Ventilator
Weaning off the ventilator means slowly reducing your dependence on the machine. This process doesn’t happen overnight; doctors and nurses carefully monitor your breathing strength and comfort.
You might start by breathing on your own for short periods while still connected. This helps your lungs and muscles regain strength without feeling rushed.
Expect some ups and downs—sometimes you’ll breathe easily, other times you might feel tired or short of breath. This is normal. The medical team adjusts the support based on how your body responds.
Post-ventilator Care
Once you’re off the ventilator, your recovery is just beginning. Your lungs may still be weak, and your muscles could feel stiff or sore from lying in bed for so long.
Physical therapy often starts quickly to help you regain strength and mobility. Simple exercises like sitting up, walking short distances, and breathing exercises are common.
Nutrition plays a key role too. Eating well helps your body heal faster and gives you energy to keep improving.
Do you notice small improvements each day? Celebrate them—they show your progress and keep motivation high.
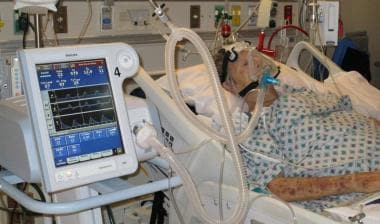
Credit: emedicine.medscape.com
Frequently Asked Questions
Can Patients Stay Awake While On A Ventilator?
Yes, many patients remain awake and aware while on a ventilator. Sedation levels vary based on medical needs and comfort. Healthcare providers adjust settings to balance breathing support and consciousness. Awake patients can communicate and participate in care decisions.
How Does A Ventilator Affect Patient Consciousness?
A ventilator itself does not cause unconsciousness. Sedatives or medications given alongside may induce sleep or sedation. Consciousness depends on illness severity and treatment protocols. Some patients are fully alert, while others are lightly sedated for comfort.
What Signs Indicate Awareness On A Ventilator?
Awake patients can respond to voices, follow commands, or move limbs. Eye opening and purposeful movements suggest awareness. Nurses and doctors monitor these signs to assess consciousness levels and adjust care accordingly.
Is It Painful To Be Awake On A Ventilator?
Being awake on a ventilator is usually not painful. Discomfort may arise from the breathing tube or illness. Medical teams manage pain and anxiety with medications and support. Patients often receive reassurance and care to enhance comfort.
Conclusion
Being awake on a ventilator can feel strange and scary. Knowing what to expect helps reduce fear and confusion. Medical teams work hard to keep patients comfortable and safe. Breathing machines support life but do not take control away. Staying calm and asking questions makes a big difference.
Each person’s experience is unique and deserves care. Understanding this helps families and patients feel less alone. Trust in the process and focus on healing day by day. Support and patience bring hope through the challenge.