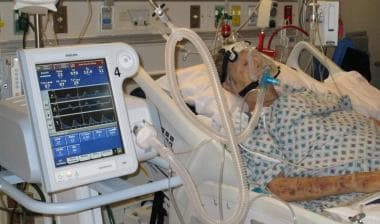
Have you ever wondered if you can stay awake while on a ventilator? It might sound surprising, but many people believe that being on a ventilator means you must be unconscious or heavily sedated.
The truth is, you can often be awake and alert even when a machine is helping you breathe. Understanding this can ease your fears and help you feel more in control if you or a loved one ever face this situation.
Keep reading to discover how being awake on a ventilator works, what it feels like, and what you can expect during this experience.
Purpose Of A Ventilator
Ventilators help patients breathe by moving air in and out of the lungs. Patients can stay awake on ventilators. This allows them to communicate and interact, making the process less stressful.
The purpose of a ventilator is to assist with breathing. It provides oxygen to the lungs when they cannot function on their own. This can be due to illness, injury, or surgery. Ventilators play a crucial role in medical care. They ensure patients receive the necessary oxygen to survive.How Ventilators Support Breathing
Ventilators help by pushing air into the lungs. This process is called mechanical ventilation. It mimics the natural breathing process. The ventilator adjusts oxygen levels based on the patient’s needs. It can also remove carbon dioxide from the body. This is vital for maintaining the body’s pH balance.Common Conditions Requiring Ventilation
Several conditions may require the use of a ventilator. These include severe pneumonia and chronic obstructive pulmonary disease (COPD). Asthma attacks that do not respond to treatment may need ventilation support. Traumatic injuries affecting the chest or lungs might also require a ventilator. Surgery patients sometimes use ventilators during recovery. This helps ensure safe and effective breathing post-operation.Being Awake While On A Ventilator
Being awake while on a ventilator may sound surprising, but it’s more common than you might think. Patients can sometimes remain conscious and even communicate while receiving ventilator support. Understanding how this works can help you feel more informed and less anxious about the process.
Sedation Practices And Awake Patients
Doctors often use sedation to keep patients calm and comfortable when on a ventilator. However, sedation levels vary depending on the patient’s condition and treatment goals. Some patients stay lightly sedated or completely awake to reduce complications related to deep sedation.
Being awake can allow you to participate in your care, communicate needs, and even start physical therapy sooner. This approach requires careful monitoring to balance comfort and awareness without causing distress. Have you ever wondered how hospitals decide the right sedation level for each patient?
Awake Ventilation Vs. Sedated Ventilation
Awake ventilation means you breathe with the ventilator’s help but remain conscious. This can help maintain muscle strength and reduce the risk of delirium. On the other hand, sedated ventilation keeps you unconscious, which might be necessary for severe cases or when invasive procedures are performed.
Choosing between awake and sedated ventilation depends on many factors, including your overall health and the reason for ventilation. Awake ventilation can be challenging but offers benefits like faster recovery and better communication. How would you feel knowing you could stay awake and talk to your loved ones even while on a ventilator?
Types Of Ventilation Methods
Ventilation supports breathing when lungs cannot work well alone. Different types of ventilation methods help patients in various conditions. Each method varies by how air is delivered and patient comfort. Understanding these types helps explain if you can stay awake on a ventilator.
Non-invasive Ventilation
Non-invasive ventilation (NIV) uses masks instead of tubes. The mask fits over the nose, mouth, or both. It helps push air into the lungs without surgery. Patients usually stay awake and can communicate. NIV supports breathing during sleep or illness. It reduces the need for more invasive methods. Common types include CPAP and BiPAP machines. These machines adjust pressure to help lungs work better.
Invasive Ventilation With Intubation
Invasive ventilation requires a tube placed in the airway. This tube goes through the mouth or nose into the windpipe. It connects to a ventilator machine for full breathing support. Patients often need sedation to stay comfortable. Staying awake is possible but depends on the medical condition. Intubation is used in serious breathing problems or surgery. This method ensures precise control of oxygen and air flow. Careful monitoring is essential to prevent complications.

Credit: healthcare-in-europe.com
Patient Experience On A Ventilator
Being awake while on a ventilator can be a complex and deeply personal experience. It involves more than just the mechanics of breathing support; it affects how you communicate and feel physically. Understanding these aspects can prepare you or your loved ones for what to expect and how to cope.
Communication Challenges
One of the biggest hurdles when you’re awake on a ventilator is speaking. The breathing tube often passes through your vocal cords, making normal speech impossible.
This can feel isolating. Imagine wanting to tell someone about your pain or ask a simple question but being unable to speak. Many patients use alternative communication methods like:
- Writing notes on a board or paper
- Using hand signals or blinking to answer yes/no questions
- Electronic communication devices designed for non-verbal patients
These tools help, but they require patience from both you and caregivers. How would you express your needs if you couldn’t speak?
Physical Sensations And Comfort
The physical feeling of being on a ventilator can be strange and sometimes uncomfortable. You might feel the tube in your throat, which can cause a tickling or scratching sensation.
Some patients describe pressure or tightness around their chest as the machine helps them breathe. Nurses and doctors often adjust settings to improve comfort, but it’s important to speak up about what you feel.
Simple actions like repositioning, adjusting sedation levels, or using humidifiers can make a big difference. Have you ever had to communicate discomfort without words? This experience can teach resilience and new ways to connect.
Risks And Complications
Being awake on a ventilator carries certain risks and complications. Understanding these helps patients and caregivers prepare better. The experience can be challenging due to physical and emotional factors. Medical teams work hard to reduce these issues and keep patients safe.
Potential Discomfort And Anxiety
Awake patients may feel discomfort from the breathing tube. The tube can irritate the throat and mouth. This often causes coughing or a dry sensation.
Many patients feel anxious or scared while on a ventilator. The noise and restriction can increase stress. Anxiety may worsen breathing difficulty and overall discomfort.
Doctors and nurses use calming techniques and medications to ease anxiety. Communication tools help patients express their needs despite the tube. Comfort measures improve the patient’s overall experience.
Managing Airway And Lung Risks
The ventilator can increase the risk of lung infections. Bacteria may enter through the breathing tube, causing pneumonia. Careful hygiene and monitoring reduce this risk.
Ventilator-associated lung injury is another concern. Improper pressure or volume settings may damage the lungs. Regular checks and adjustments prevent injury.
Secretions can build up around the airway. This may block airflow or cause infection. Suctioning and cleaning keep the airway clear and safe.
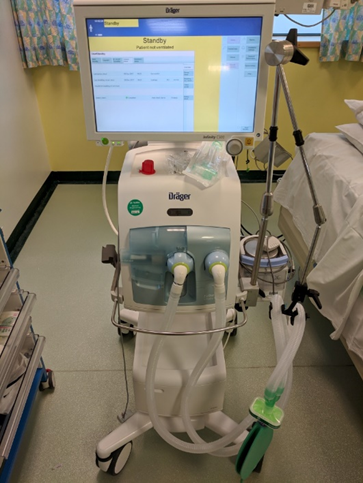
Credit: www.gatesheadhealth.nhs.uk
Care And Monitoring
Care and monitoring are vital for patients awake on a ventilator. Constant observation ensures safety and comfort. Medical teams focus on both physical and emotional well-being. Monitoring helps detect any issues early. Adjustments are made to support breathing and reduce stress.
Role Of Medical Staff
Medical staff play a key role in managing awake patients on ventilators. Nurses and respiratory therapists check vital signs regularly. They watch for signs of discomfort or breathing difficulty. Doctors assess the patient’s overall condition daily. Communication with the patient helps tailor care and reduce anxiety.
Staff also provide guidance on using the ventilator properly. They educate patients about what to expect. Emotional support is crucial for patients who feel scared or confused. Staff coordinate with family members to create a calm environment.
Adjusting Ventilator Settings For Awake Patients
Ventilator settings must be carefully adjusted for awake patients. Settings balance between supporting breathing and allowing patient effort. Too much support can weaken muscles. Too little support causes fatigue and distress.
Settings like breathing rate, volume, and pressure are fine-tuned. Changes happen gradually to avoid sudden discomfort. Patients may communicate feedback through gestures or speech. Monitoring tools track oxygen levels and carbon dioxide.
The goal is to keep breathing natural and comfortable. Adjustments also help patients participate in therapy and daily activities. This approach aids recovery and maintains patient alertness.
Recovery And Weaning Off The Ventilator
Recovery and weaning off the ventilator mark a critical phase in a patient’s journey towards breathing independently again. Being awake while on a ventilator can influence how smoothly this transition occurs. Understanding the signs that indicate you’re ready and the steps involved in removing ventilation support can empower you or your loved ones to approach this process with confidence.
Signs Of Readiness
Recognizing when you are ready to start weaning from the ventilator is crucial. Doctors look for stable vital signs like steady heart rate and blood pressure. You should be able to breathe on your own for brief periods without distress.
Other signs include:
- Improved lung function and oxygen levels
- Ability to cough and clear secretions effectively
- Strong mental alertness and cooperation
Have you noticed how your energy levels and breathing patterns change throughout the day? These subtle shifts often signal your lungs are ready to take on more work.
Steps To Remove Ventilation Support
Weaning off the ventilator is a gradual process tailored to your condition. It often starts with shorter periods of spontaneous breathing while still connected to the machine. Medical staff closely monitor your response during these trials.
Key steps include:
- Reducing ventilator settings to increase your breathing effort
- Performing spontaneous breathing trials to test endurance
- Assessing blood gases to ensure proper oxygen and carbon dioxide levels
Patience plays a big role here. Sometimes, you might feel ready, but your body needs more time. How do you handle these moments of uncertainty during recovery?
Ultimately, successful weaning depends on your body’s strength and the support of your healthcare team. Staying engaged and informed can make you an active participant in your own healing.

Credit: www.zoll.com
Frequently Asked Questions
Can Patients Stay Awake While On A Ventilator?
Yes, many patients can remain awake while on a ventilator. Sedation levels vary based on illness severity. Awake patients can communicate and participate in care.
How Does Being Awake Affect Ventilator Use?
Being awake allows better breathing control and quicker recovery. It helps reduce sedation risks and promotes lung function improvement during ventilation.
What Are The Challenges Of Being Awake On A Ventilator?
Awake patients may experience discomfort, anxiety, or difficulty speaking. Proper support, including pain management and communication aids, is essential for comfort.
Is It Safe To Be Awake During Mechanical Ventilation?
Yes, staying awake is safe when closely monitored by medical staff. Care teams adjust sedation and support to ensure patient safety and comfort.
Conclusion
Being awake on a ventilator is possible for many patients. Doctors carefully monitor and adjust the settings to keep patients comfortable. This helps patients breathe without needing full sedation. Staying awake allows patients to communicate and participate in their care.
It also helps with faster recovery and fewer complications. Each case is different, and medical teams decide what works best. Understanding this can ease fears about ventilator use. Clear communication and care are key during this process.