Have you ever wondered how often you should provide ventilations during an emergency? Knowing the right timing can make a huge difference in saving a life.
If you’ve ever felt unsure or worried about doing it correctly, you’re not alone. This article will guide you step-by-step, so you feel confident and ready when it matters most. Keep reading to discover the essential tips that could help you become a lifesaver.

Credit: itsairborne.com
Importance Of Ventilation Timing
Timing is crucial when providing ventilations, especially in emergency situations like CPR. Delivering breaths at the right moment can significantly improve oxygen flow to the lungs and brain. If you ventilate too quickly or too slowly, you might reduce the effectiveness of rescue efforts.
Understanding The Ideal Ventilation Rate
You should aim to provide ventilations at a steady, controlled rate. For adults, this typically means one breath every 5 to 6 seconds during CPR. If you breathe too often, it can increase pressure in the chest, limiting blood flow and reducing the chance of survival.
Think about your own breathing pattern when calm versus stressed—breathing too fast feels unnatural and doesn’t help your body. Matching the right ventilation timing keeps the process smooth and effective.
How Timing Affects Oxygen Delivery
Oxygen delivery depends on how well the lungs can absorb the air you provide. If ventilations are spaced well, the lungs have time to fill and empty properly. This maximizes oxygen exchange and helps vital organs get the air they need.
When timing is off, air can get trapped or pushed out too quickly, which lowers oxygen levels. Have you noticed how shallow, rapid breaths leave you feeling short of air? The same principle applies here.
Impact On Chest Compressions And Circulation
Ventilation timing must sync with chest compressions for CPR to be effective. Interrupting compressions for too long to give breaths can reduce blood circulation. On the other hand, ventilating too fast without enough compressions limits oxygenated blood flow.
Balancing these actions requires practice. Think about it as a rhythm where both parts must work together to keep the heart and lungs functioning during emergencies.
Adjusting Ventilation Timing Based On The Situation
The ideal timing may change depending on the person’s condition or environment. For example, infants and children often need faster breaths than adults. In some cases, like drowning, the timing and volume of breaths might need adjustment.
Always pay attention to the victim’s response and adjust accordingly. How quickly can you sense when something isn’t working and adapt your approach? Staying alert to these cues makes all the difference.
Ventilation Frequency In Cpr
Ventilation frequency in CPR is crucial to keep oxygen flowing to the brain and body. Giving breaths too fast or too slow can cause harm. The right rhythm helps improve survival chances. Different age groups need different ventilation rates. Understanding these rates ensures effective CPR.
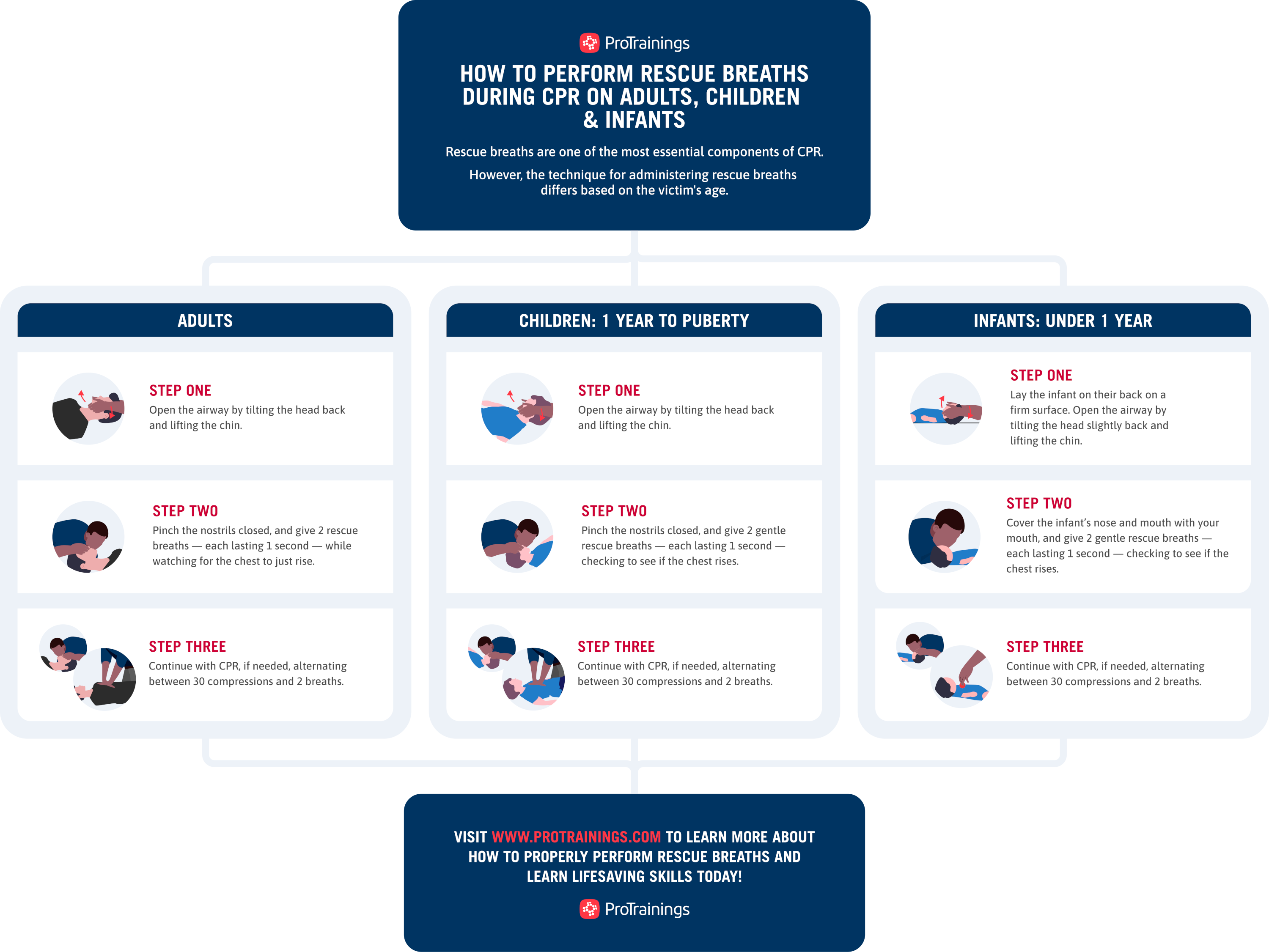
Adults
For adults, provide 2 breaths after every 30 chest compressions. Each breath should last about 1 second. Watch for the chest to rise. Avoid giving breaths too quickly or forcefully. This allows oxygen to enter the lungs properly.
Children
In children, give 2 breaths after every 30 compressions if alone. If two rescuers are present, give 2 breaths after every 15 compressions. Make sure each breath lasts about 1 second. The chest should rise gently with each breath.
Infants
For infants, use the same ventilation rate as children. Provide 2 breaths after 30 compressions when alone. If two rescuers help, give 2 breaths after 15 compressions. Use gentle breaths. Watch the chest rise to confirm air entry.
Factors Affecting Ventilation Rate
Understanding how often to provide ventilations depends on several key factors. These factors influence how much air the patient needs and the timing of breaths. Adjusting the ventilation rate correctly can improve the patient’s chances of recovery. Knowing what affects this rate helps responders act more effectively.
Patient Condition
The patient’s health and age affect ventilation needs. Children and infants require faster breaths than adults. If the patient has lung disease or injuries, the rate may change. Monitoring breathing effort and pulse guides the ventilation speed. A weak pulse or shallow breathing needs careful adjustment.
Rescue Environment
The surroundings impact how ventilations are given. Noisy or crowded places can make timing difficult. Cold weather may slow breathing, requiring more breaths per minute. Limited space or equipment affects how you provide air. Always adapt to the environment for the best results.
Type Of Rescue Breathing
The method used changes the ventilation rate. Mouth-to-mouth breathing differs from using a mask or bag-valve device. Devices often allow more controlled and consistent breaths. Manual rescue requires more attention to timing. Choose the type that fits the situation and patient needs.
Credit: www.protrainings.com
Signs You Need To Adjust Ventilation
Knowing when to adjust ventilation is crucial for effective respiratory support. If you miss the signs, the patient might not get enough oxygen or could suffer from over-ventilation. Staying alert to these indicators helps you respond quickly and keep the airway open and clear.
Chest Rise Observation
Watching the chest rise is one of the simplest ways to check if your ventilations are effective. The chest should lift visibly with each breath you provide. If the rise is weak or absent, it’s a clear sign that you need to adjust your technique.
Maybe you’re giving breaths too fast or too slow, or the seal around the mask isn’t tight enough. Ask yourself: Does the chest move enough to suggest air is actually entering the lungs? If not, fix your hand positioning or the ventilation rate immediately.
Patient Response
The patient’s reactions provide valuable clues about ventilation quality. Are they becoming more alert or showing signs of distress? Changes in skin color, like turning blue or pale, can mean they aren’t getting enough oxygen.
Sometimes, you might notice coughing or gagging, signaling discomfort or airway irritation. These signs should prompt you to reassess the ventilation volume and frequency. What changes did you notice in your last ventilation attempt?
Airway Obstruction
Airway blockage is a common reason ventilation needs adjustment. If you feel resistance when giving breaths, it could mean the airway is partially or fully blocked. This often happens due to the tongue falling back or secretions blocking airflow.
Try repositioning the head or using suction if available. Ignoring airway obstruction can worsen the patient’s condition quickly. Do you regularly check for and clear obstructions before and during ventilation?
Common Mistakes In Ventilation Timing
Ventilation is crucial for effective respiratory support. Yet, timing mistakes can occur. These mistakes lead to serious health problems. Understanding common errors helps ensure proper ventilation.
Overventilation Risks
Overventilation can cause several health issues. It can lead to low carbon dioxide levels in the blood. This condition is known as hypocapnia. Hypocapnia may result in dizziness and confusion. It can also cause muscle cramps and tingling sensations. In severe cases, it may lead to respiratory alkalosis. This disrupts the body’s pH balance. Overventilation can also increase the risk of lung injury. Too much pressure on the lungs causes harm. Monitoring ventilation rates is essential to avoid these risks.
Underventilation Consequences
Underventilation is equally dangerous. It results in inadequate oxygen supply to the body. This can cause hypoxia, a condition with low oxygen levels. Hypoxia leads to fatigue and shortness of breath. In extreme cases, it may cause organ damage. Underventilation also leads to hypercapnia. This is an excess of carbon dioxide in the blood. Symptoms include headaches and flushed skin. Severe hypercapnia can cause confusion or even coma. Regular monitoring helps prevent these consequences.
Tips For Effective Ventilation Delivery
Delivering ventilations effectively can make a critical difference in emergency situations. It’s not just about how often you provide breaths, but how well you do it. Paying attention to technique, equipment use, and airway management ensures the air you deliver actually helps the patient.
Proper Technique
Focus on giving slow, steady breaths that last about one second each. Fast or forceful breaths can cause air to enter the stomach, leading to complications. Watch the patient’s chest rise with each breath to confirm you’re delivering enough air without overdoing it.
Have you noticed how easy it is to lose track of timing under pressure? Practicing the rhythm beforehand builds confidence and accuracy. Remember, quality beats quantity every time when it comes to ventilation.
Using Equipment Correctly
Whether you’re using a bag-valve mask or mouth-to-mouth, ensure the device fits securely. A poor seal wastes your effort and reduces oxygen delivery. Check the equipment regularly so you’re ready to act without delay.
- Adjust the mask to cover both nose and mouth completely.
- Use two hands if possible to maintain a tight seal.
- Be aware of the equipment’s limits; some masks require specific pressure levels.
Have you ever struggled with a mask slipping during ventilation? It’s a common challenge that proper grip and positioning can fix immediately.
Maintaining Airway Patency
Air can’t get in if the airway is blocked. Tilt the head back and lift the chin to open the airway before you start ventilations. If you suspect a spinal injury, use a jaw-thrust maneuver instead.
Clearing the mouth of any obstructions like vomit or foreign objects is crucial. Even small blockages can stop air from reaching the lungs. Ask yourself: Is the airway truly open before every breath?
These small checks can drastically improve the effectiveness of each ventilation you provide. Your attention to detail might be the factor that saves a life.
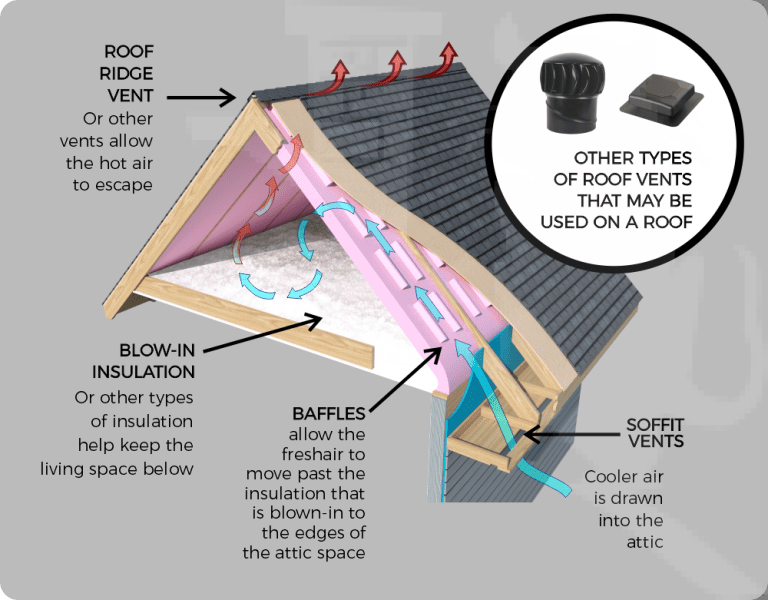
Credit: www.northeast-home.com
Frequently Asked Questions
How Often Should Ventilations Be Given During Cpr?
Ventilations should be provided every 6 seconds during CPR. This equals 10 breaths per minute. Proper timing ensures effective oxygen delivery.
Why Is Correct Ventilation Frequency Important?
Correct ventilation frequency maintains oxygen levels without causing lung damage. Too many breaths can lead to complications. Proper timing supports better patient outcomes.
How To Adjust Ventilation Rate For Infants And Children?
For infants and children, give one breath every 3-5 seconds. This equals 12-20 breaths per minute. Adjusting rate matches their smaller lung capacity.
What Happens If Ventilations Are Given Too Quickly?
Giving breaths too quickly can cause stomach inflation. This increases risk of vomiting and airway blockage. Slow, steady breaths improve safety.
Conclusion
Providing ventilations at the right times saves lives. Keep the rate steady and clear. Too fast or too slow can cause harm. Practice the correct method often to stay confident. Knowing how often to give ventilations helps in emergencies. Stay calm, act quickly, and follow simple steps.
Your actions can make a big difference. Remember, consistent and proper ventilations improve chances of recovery. Always be ready to help when needed.





