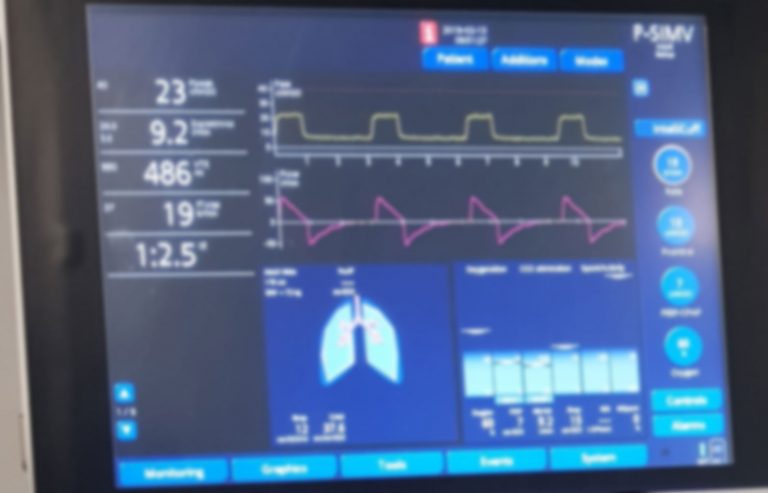
If you’re caring for someone on a ventilator or working in a healthcare setting, knowing how to read a ventilator monitor is crucial. These monitors display important information about breathing and oxygen levels, but the numbers and graphs can feel confusing at first.
Don’t worry—this guide will help you understand what each reading means and how to use this knowledge to ensure the best care. By the end, you’ll feel confident interpreting ventilator data and making informed decisions. Let’s dive in and unlock the key to understanding your ventilator monitor.

Credit: www.youtube.com
Basics Of Ventilator Monitors
Ventilator monitors display critical information for patients on breathing machines. They help healthcare staff track breathing rates, pressure, and oxygen levels. Understanding these basics allows quick interpretation of the patient’s condition. This knowledge supports better care and timely adjustments to treatment.
Key Components To Watch
- Tidal Volume (Vt):Amount of air delivered per breath.
- Respiratory Rate (RR):Number of breaths per minute.
- Peak Inspiratory Pressure (PIP):Highest pressure during inhalation.
- Positive End-Expiratory Pressure (PEEP):Pressure maintained at end of exhalation.
- Oxygen Concentration (FiO2):Percentage of oxygen in the air delivered.
- Minute Ventilation (MV):Total air volume breathed per minute.
Common Display Types
Ventilator monitors use different screen layouts to show data clearly. Numeric displays provide exact values for vital signs. Waveform displays show breathing patterns in real time.
Waveforms include:
- Pressure Waveform:Shows pressure changes during breathing cycles.
- Volume Waveform:Illustrates the amount of air delivered over time.
- Flow Waveform:Displays airflow into and out of the lungs.
Understanding these visual cues helps detect problems early. It also guides adjustments to ventilator settings for patient safety.
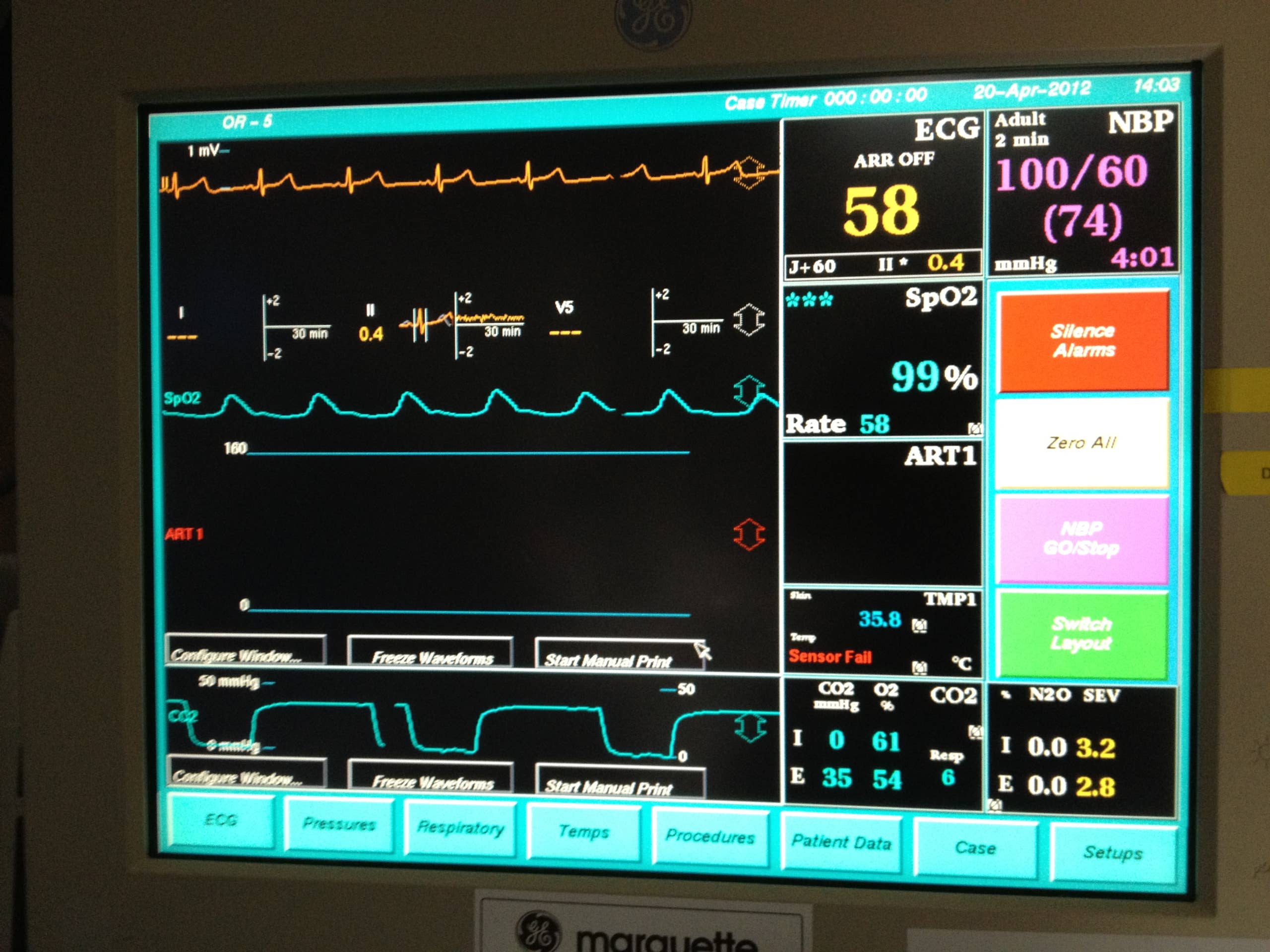
Credit: owlcation.com
Essential Ventilator Parameters
Understanding essential ventilator parameters is key to reading a ventilator monitor effectively. These parameters give critical information about a patient’s breathing status and ventilator settings. Monitoring these values helps ensure the patient receives the right support.
Each parameter reflects a different aspect of ventilation. Knowing what each number means can guide healthcare providers in adjusting treatment for better patient outcomes. Below are the main parameters to focus on.
Tidal Volume
Tidal volume measures the amount of air delivered to the lungs with each breath. It is usually shown in milliliters (mL). Proper tidal volume helps avoid lung injury by preventing too much or too little air from entering the lungs.
Respiratory Rate
Respiratory rate shows the number of breaths a patient takes per minute. It indicates how often the ventilator is assisting breathing. Changes in this rate can signal improvement or distress in the patient’s condition.
Peak Inspiratory Pressure
Peak inspiratory pressure (PIP) measures the highest pressure reached during inhalation. High PIP values may suggest airway resistance or lung stiffness. Monitoring PIP helps protect the lungs from damage caused by excessive pressure.
Positive End-expiratory Pressure
Positive end-expiratory pressure (PEEP) keeps the lungs slightly inflated after exhalation. It prevents lung collapse and improves oxygen exchange. Adjusting PEEP is important for patients with weak or injured lungs.
Oxygen Concentration
Oxygen concentration shows the percentage of oxygen delivered to the patient. It is vital to maintain adequate oxygen levels in the blood. This value guides oxygen therapy to meet the patient’s needs safely.
Interpreting Waveforms
Understanding waveforms on a ventilator monitor is key to assessing patient breathing. These waveforms show how air moves in and out of the lungs during ventilation. Each waveform offers unique information about lung mechanics and ventilator performance. Learning to read them helps detect problems early and guides treatment decisions.
Pressure Waveform
The pressure waveform displays airway pressure over time. It shows the pressure needed to deliver each breath. Look for a smooth rise and fall during inspiration and expiration. Sharp peaks or plateaus may indicate airway resistance or lung stiffness. A sudden drop might suggest leaks or disconnections. Consistent pressure waveforms mean the ventilator is working properly.
Flow Waveform
The flow waveform measures the speed of air entering and leaving the lungs. Positive values represent inhalation, negative values show exhalation. A steady, smooth curve is ideal. A rapid peak followed by a slow decline suggests normal lung emptying. Irregular or flat flow patterns can indicate obstructions or patient-ventilator mismatch. Watching this waveform helps adjust ventilator settings for comfort and safety.
Volume Waveform
The volume waveform tracks the amount of air delivered during each breath. It rises during inhalation and falls during exhalation. The total volume delivered should match the set tidal volume. Low or inconsistent volumes may mean leaks, poor lung compliance, or patient effort. This waveform helps monitor actual lung inflation and guides ventilation adjustments for best oxygenation.
Recognizing Alarms And Alerts
Recognizing alarms and alerts on a ventilator monitor is crucial for ensuring patient safety. These signals are designed to catch your attention immediately when something needs urgent care or adjustment. Understanding what each alarm means and how to respond can make a real difference in critical situations.
Common Alarm Types
Ventilator monitors use different alarms to highlight various issues. Some alarms warn about airway problems, while others signal machine malfunctions or patient distress. Here are a few common types you should know:
- High Pressure Alarm:Indicates increased resistance or blockage in the airway. It might mean a kinked tube or mucus buildup.
- Low Pressure Alarm:Signals a leak or disconnection in the breathing circuit.
- Apnea Alarm:Alerts you if the patient stops breathing for a set time.
- High Respiratory Rate Alarm:Warns if the patient’s breathing rate is too fast.
- Low Oxygen Alarm:Indicates the oxygen level is below the set threshold.
Each alarm sounds differently and may include visual cues on the monitor. Paying attention to both helps you quickly identify the problem.
Prioritizing Responses
Not all alarms require the same urgency. Some indicate immediate danger, while others are reminders to check or adjust settings. Knowing which alarms demand your fastest action is key to patient care.
Ask yourself: Could this alarm mean the patient is in immediate danger? If yes, act right away—check the airway, connections, and vital signs. If it’s a less critical alert, you can plan a timely response, but never ignore it.
One time, I hesitated on a low pressure alarm, thinking it was minor. It turned out the patient’s tube had partially disconnected, risking oxygen deprivation. That moment taught me to always prioritize alarms that affect oxygen delivery or breathing first.
To manage alarms effectively:
- Respond to high-priority alarms immediately.
- Check the ventilator settings and patient condition regularly.
- Document and communicate any recurring alarms with your team.
How confident are you in distinguishing between urgent and routine ventilator alarms? Sharpening this skill can improve outcomes and reduce stress during critical moments.
Troubleshooting Common Issues
Understanding ventilator monitor readings helps spot common problems quickly. Check for unusual alarms or unexpected values. Clear, simple steps make troubleshooting easier and safer.
Troubleshooting common issues on a ventilator monitor can feel overwhelming, especially when you are in the middle of a critical situation. Yet, having the skills to quickly identify and resolve these issues can make a significant difference in patient care. Knowing where to look and what to listen for can turn potential problems into manageable tasks.Detecting Airway Obstruction
An airway obstruction can cause alarms to blare and your heart rate to spike. When this happens, check for visible signs of distress in the patient. Look for secretions or kinks in the tube that might be blocking airflow. A handy trick is to gently suction the airway and see if resistance decreases. Pay close attention to the ventilator’s pressure readings. If they’re higher than usual, an obstruction might be the culprit.Identifying Leaks
Leaks can lead to insufficient ventilation, making it crucial to detect them early. Listen for hissing sounds around the ventilator tubing or mask, which can indicate a leak. You can also observe the tidal volume readings on the monitor. If they are lower than expected, it might point to a leak. Ensure all connections are tight and that the mask fits snugly.Managing Patient-ventilator Asynchrony
Patient-ventilator asynchrony can cause discomfort and inefficient ventilation. It occurs when the patient’s breathing pattern doesn’t match the ventilator’s settings. Observe the patient’s chest movements and compare them to the ventilator cycles. Adjust the sensitivity settings on the ventilator to better align with the patient’s natural breathing efforts. Sometimes, a small adjustment can make a big difference in synchronizing their breathing with the machine. When was the last time you had to troubleshoot a ventilator monitor? Remember, each issue you solve enhances your confidence and skills in providing top-notch care.Tips For Quick And Accurate Monitoring
Mastering quick and accurate ventilator monitoring can make a real difference in patient care. You need to stay sharp and focused because every second counts. These tips will help you read the monitor efficiently and catch crucial changes before they escalate.
Checklist For Rapid Assessment
Start with a mental checklist to ensure nothing is overlooked during your quick scan. This habit keeps your evaluation structured and consistent.
- Check the tidal volume:Is it within the prescribed range? Low or high values may indicate problems.
- Assess respiratory rate:Watch for abnormal breathing patterns or sudden changes.
- Monitor peak airway pressure:High pressure might signal airway obstruction or poor lung compliance.
- Observe oxygen saturation:Drops below target levels require immediate attention.
- Review alarms:Are any active? Don’t ignore them—alarms are your early warning system.
Keeping this checklist in mind helps you cover all vital signs swiftly. Have you ever missed a critical sign by jumping straight to one parameter? This approach prevents that.
Utilizing Monitor Features Efficiently
Modern ventilator monitors come packed with features that can speed up your assessment. Do you know how to use them to your advantage?
- Use trend displays:They show how parameters change over time, helping you spot gradual deterioration.
- Set customized alarms:Tailor alarm limits to the patient’s condition to reduce false alerts and focus on real issues.
- Activate waveform analysis:Visual graphs of pressure, volume, and flow provide deeper insight into lung mechanics.
- Leverage built-in calculators:Some monitors offer quick calculations for compliance and resistance, saving time on manual math.
Once, I relied solely on numbers without checking waveforms, missing early signs of a patient’s worsening status. Don’t make the same mistake—explore all features your monitor offers. How might your assessments improve if you used these tools regularly?

Credit: www.vhtc.org
Frequently Asked Questions
What Are The Key Parameters On A Ventilator Monitor?
Key parameters include tidal volume, respiratory rate, oxygen saturation, peak inspiratory pressure, and PEEP. These help assess patient ventilation and lung function accurately.
How Do I Interpret Tidal Volume Readings?
Tidal volume shows the air amount delivered per breath. Normal values depend on patient size and condition. It ensures effective ventilation without lung injury.
Why Is Monitoring Oxygen Saturation Important?
Oxygen saturation indicates blood oxygen levels. It helps detect hypoxia early, ensuring timely intervention to maintain adequate oxygen delivery to tissues.
What Does Peak Inspiratory Pressure Indicate?
Peak inspiratory pressure measures the highest pressure during inhalation. High values may suggest airway resistance or lung stiffness, requiring medical assessment.
Conclusion
Reading a ventilator monitor helps you understand patient care better. Watch the numbers closely to track breathing and oxygen levels. Each value tells a part of the patient’s health story. Practice often to feel confident and notice changes quickly. Clear knowledge aids quick decisions in urgent moments.
Keep learning and stay calm while reading the monitor. This skill supports better care and safer treatment. Simple steps lead to strong understanding. Keep these tips in mind for daily use.