Have you ever wondered how your breathing system works when you’re just sitting still or resting? Understanding something called “dead space ventilation” can change the way you think about your lungs and breathing.
It’s a key part of how your body manages air, but many people don’t know what it really means or why it matters. You’ll discover what dead space ventilation is, why it’s important for your health, and how it affects the way you breathe every day.
Keep reading, and you’ll gain insights that can help you take better care of your lungs and overall well-being.
Credit: www.academia.edu
Dead Space Ventilation Basics
Understanding dead space ventilation is key to grasping how breathing works efficiently. It explains how some air we breathe does not participate in gas exchange. This section breaks down the basics of dead space ventilation.
Definition Of Dead Space
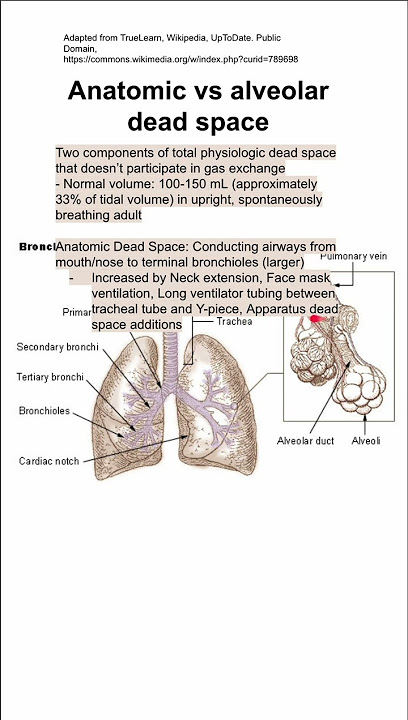
Dead space refers to areas in the respiratory system where air does not reach the blood for gas exchange. This air fills the lungs but does not participate in oxygen or carbon dioxide transfer. It is important to know that dead space air is not wasted but plays a role in normal breathing.
Types Of Dead Space
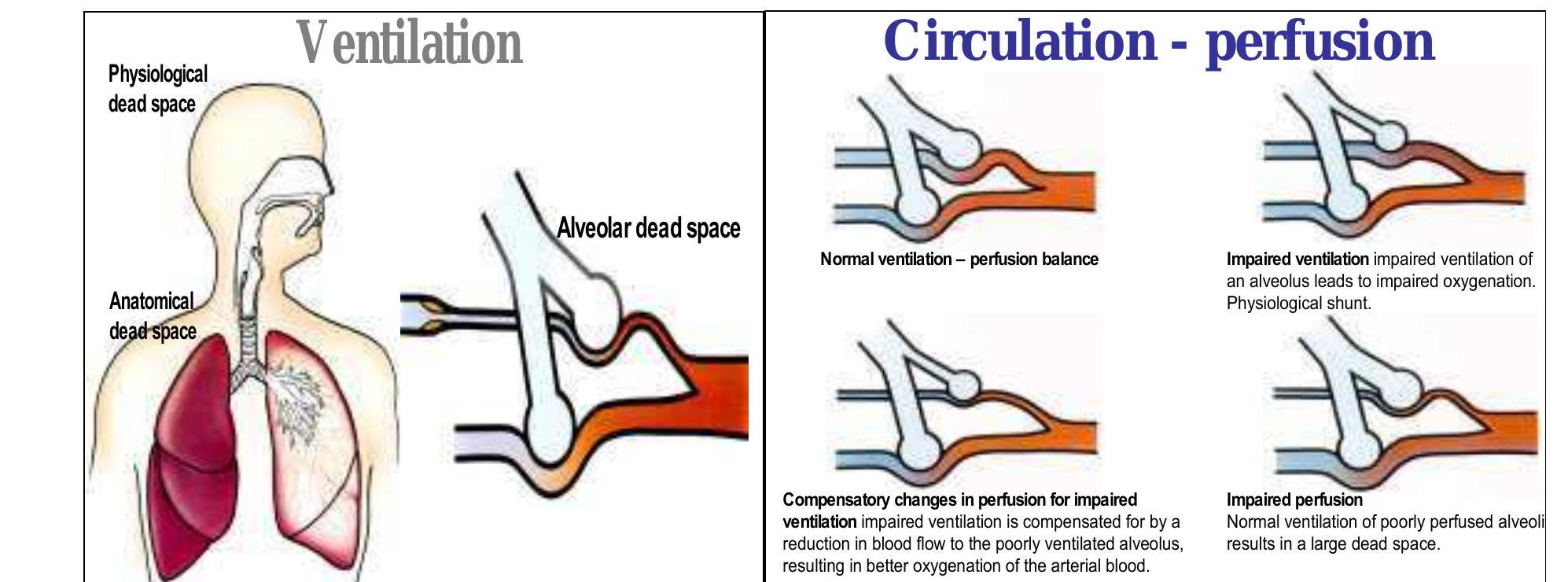
- Anatomic Dead Space:Air in the airways like the nose, trachea, and bronchi where no gas exchange occurs.
- Alveolar Dead Space:Air in alveoli that are ventilated but not perfused by blood, so no gas exchange happens.
- Physiologic Dead Space:The total of anatomic and alveolar dead space combined. It shows the full volume of air not involved in gas exchange.
Physiological Importance
Dead space helps maintain proper airflow and lung function. It prevents sudden changes in lung volume and pressure. By filling airways, dead space supports humidifying and warming of inhaled air. It also plays a role in controlling the balance of oxygen and carbon dioxide in the body.
Credit: medclubhu.weebly.com
Causes Of Dead Space Ventilation
Dead space ventilation happens when part of the air you breathe doesn’t participate in gas exchange. Understanding what causes this can help you recognize issues with breathing efficiency. Various factors can increase dead space, and these fall into three main categories: anatomical, physiological, and pathological.
Anatomical Factors
Anatomical dead space refers to the parts of your respiratory system where air flows but no gas exchange occurs. This includes your nose, throat, trachea, and bronchi. If these areas are larger than normal, more air stays trapped without reaching the lungs’ alveoli.
For example, people with larger airways naturally have higher anatomical dead space. You might notice this if you compare the breathing of adults to children—children have smaller airways, so less anatomical dead space. Have you ever wondered why taking deep breaths doesn’t always feel equally effective? It could be due to variations in this space.
Physiological Factors
Physiological dead space includes both anatomical dead space and any alveoli that are ventilated but not perfused with blood. This means air reaches the alveoli but doesn’t exchange oxygen and carbon dioxide properly.
Changes in blood flow or ventilation patterns can increase physiological dead space. For instance, during exercise, blood flow improves and dead space decreases, making breathing more efficient. But if you’re at high altitude or have certain lung conditions, this balance can shift the other way.
Pathological Conditions
Several diseases can increase dead space ventilation by damaging the lungs or affecting blood flow. Conditions like pulmonary embolism block blood flow, turning parts of your lungs into dead space. Chronic obstructive pulmonary disease (COPD) and acute respiratory distress syndrome (ARDS) also raise dead space by damaging alveoli.
Think about someone with a lung clot struggling to breathe during activity. This struggle is partly due to increased dead space ventilation. How would your daily activities change if your lungs couldn’t efficiently exchange gases? Understanding these conditions can help you spot early signs and seek timely care.
Effects On Respiratory Function
Dead space ventilation affects how well the lungs perform. It changes how air moves and how oxygen reaches the blood. These effects can influence breathing and overall lung function. Understanding these changes helps in managing respiratory health better.
Impact On Gas Exchange
Dead space ventilation reduces the amount of fresh air reaching the alveoli. This lowers the oxygen entering the bloodstream. Carbon dioxide removal also decreases, causing buildup in the body. Less efficient gas exchange means tissues get less oxygen to work well.
Changes In Breathing Patterns
The body tries to fix dead space by changing breathing. Breaths may become faster or deeper to increase fresh air intake. Sometimes, breathing becomes irregular or labored. These changes aim to improve oxygen levels but can cause fatigue over time.
Clinical Implications
Increased dead space ventilation is common in lung diseases. It can worsen symptoms like shortness of breath and low oxygen levels. Doctors monitor dead space to adjust treatments like oxygen therapy. Proper management can improve comfort and lung function in patients.

Credit: www.youtube.com
Measuring Dead Space Ventilation
Dead space ventilation refers to the part of breathing where air fills the lungs but does not participate in gas exchange. Measuring it helps understand how much air is wasted during breathing. This is important for assessing lung function and respiratory health.
Measuring Dead Space Ventilation is crucial for understanding lung efficiency. It helps determine how much of the air inhaled is not used for gas exchange. This can be vital for diagnosing and managing respiratory conditions. Let’s explore the techniques, tools, and limitations involved in measuring dead space ventilation.Techniques And Tools
Several methods exist to measure dead space ventilation. The Bohr equation is a common technique. It calculates dead space using expired carbon dioxide levels. Another method involves using a capnograph. This tool provides real-time CO2 waveforms. It helps identify anatomical and alveolar dead space. Another advanced tool is the volumetric capnography. It measures the volume of CO2 during a breath. This provides more detailed insights into dead space.Interpreting Results
Understanding the results is key. A higher dead space ratio indicates inefficiency. It means a larger portion of inhaled air doesn’t contribute to gas exchange. This can signal issues such as lung diseases or ventilation problems. Healthcare providers analyze these results. They use them to make informed decisions about patient care. It guides treatment plans and interventions.Limitations Of Measurement
Measuring dead space ventilation has limitations. Accuracy depends on the technique used. Some methods require expensive equipment. Others may not account for all variables affecting dead space. Patient conditions can also affect measurements. Movement or inconsistent breathing can skew results. Thus, it is essential to consider these factors during evaluation.Management And Treatment Approaches
Managing dead space ventilation requires a precise and tailored approach. The goal is to optimize breathing while minimizing complications. Understanding effective strategies and interventions can make a significant difference in patient outcomes.
Ventilation Strategies
Choosing the right ventilation strategy is crucial. You may need to adjust tidal volume and respiratory rate to reduce dead space. Sometimes, using techniques like permissive hypercapnia helps balance oxygen delivery and carbon dioxide removal.
High-frequency ventilation or non-invasive ventilation can be effective depending on the patient’s condition. Have you considered how small changes in ventilator settings could improve gas exchange? Tailoring these settings to individual needs is key.
Therapeutic Interventions
Besides mechanical support, therapeutic interventions play a vital role. Positioning the patient to enhance lung expansion can reduce dead space. Physical therapy, including breathing exercises, might improve ventilation efficiency.
Medications that reduce airway inflammation or loosen mucus can also assist in managing dead space. What if simple interventions like suctioning or humidification could prevent ventilation complications? These small steps often make a big impact.
Monitoring And Adjustments
Continuous monitoring is essential for effective management. Regular blood gas analysis helps track oxygen and carbon dioxide levels. You can then adjust ventilation settings based on these results to maintain optimal gas exchange.
Use tools like capnography to get real-time feedback on ventilation efficiency. Are you actively responding to changes in your patient’s condition? Timely adjustments can prevent deterioration and support recovery.
Dead Space In Different Clinical Settings
Dead space ventilation varies significantly depending on the clinical setting, affecting patient outcomes and treatment strategies. Understanding how dead space behaves in different scenarios helps you grasp its impact on breathing efficiency and gas exchange. Let’s look at how dead space plays a role in critical care, pulmonary diseases, and surgical environments.
Critical Care
In critical care, managing dead space is crucial for patients on mechanical ventilation. Increased dead space can indicate worsening lung function and may require adjustments in ventilator settings.
Have you noticed how small changes in ventilator parameters can drastically improve a patient’s oxygen levels? That’s often because reducing dead space improves alveolar ventilation, helping CO2 removal.
Monitoring dead space helps you tailor ventilation strategies, preventing complications like ventilator-induced lung injury. Tools like volumetric capnography give real-time insights into dead space changes.
Pulmonary Diseases
Pulmonary conditions such as COPD, asthma, and pulmonary embolism often increase physiological dead space. This makes breathing less efficient, causing patients to feel short of breath even at rest.
For example, in COPD, damaged airways trap air, increasing dead space and reducing effective gas exchange. Knowing this can guide you to focus on therapies that improve ventilation-perfusion matching.
Can adjusting your treatment plan to target dead space reduction improve a patient’s quality of life? Targeted interventions like pulmonary rehabilitation and medication adjustments can make a real difference.
Surgical Considerations
During surgery, dead space ventilation becomes particularly important, especially under general anesthesia. Anesthesia can increase dead space by altering breathing patterns and airway resistance.
For instance, using endotracheal tubes or masks adds mechanical dead space, affecting ventilation efficiency. Anesthesiologists must balance these factors to maintain proper gas exchange.
Have you considered how positioning and ventilation mode during surgery affect dead space? Proper management can prevent postoperative respiratory complications and speed up recovery.
Frequently Asked Questions
What Is Dead Space Ventilation In Respiratory Care?
Dead space ventilation refers to air that fills the lungs but doesn’t participate in gas exchange. It includes anatomical and physiological dead space. This concept helps assess ventilation efficiency and optimize respiratory support.
Why Is Dead Space Ventilation Important In Medicine?
Dead space ventilation indicates how much air bypasses oxygen exchange. High dead space can reduce breathing efficiency and worsen respiratory conditions. Monitoring it aids in diagnosing lung diseases and adjusting ventilator settings.
How Does Dead Space Affect Breathing Efficiency?
Increased dead space means more wasted air during breathing. This reduces oxygen intake and can strain respiratory muscles. Efficient ventilation minimizes dead space to improve oxygen delivery and patient comfort.
Can Dead Space Ventilation Be Measured Clinically?
Yes, it can be measured using techniques like capnography and volumetric analysis. These methods help quantify dead space volume and assess lung function in patients.
Conclusion
Dead space ventilation helps remove unused air from the lungs. It improves breathing and oxygen flow in the body. Understanding this process can aid in better lung health. It plays a key role in medical treatments and breathing support. Keep learning about how your lungs work every day.
Simple steps can support clearer and easier breathing. Dead space ventilation matters more than many realize. Breathe well, live well.