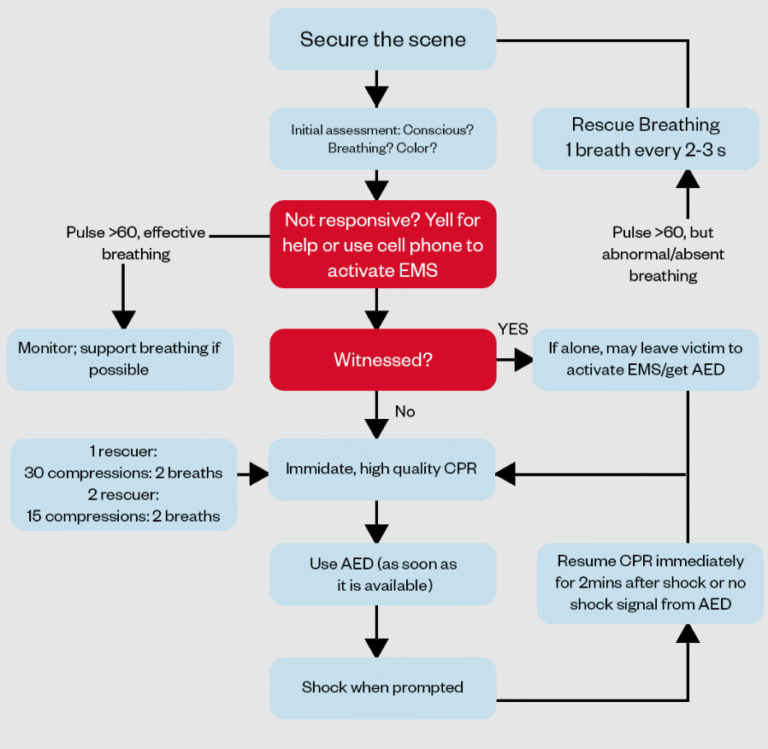
When someone’s life is on the line, every second counts—and how you perform CPR can make all the difference. One key question many people ask is: what is the correct ventilation rate for CPR?
Getting this right can improve the chances of survival and prevent serious complications. If you want to be confident and effective when helping in an emergency, understanding the proper ventilation rate is essential. Keep reading, and you’ll discover simple, clear guidance that could help you save a life when it matters most.

Credit: heartstarters.ca
Cpr Ventilation Basics
Understanding the basics of CPR ventilation is vital for effective resuscitation. Ventilation helps deliver oxygen to the lungs and keeps vital organs alive. Proper technique and rate improve the chances of survival. Let’s explore the key points about ventilation during CPR.
Role Of Ventilation In Cpr
Ventilation provides oxygen to the lungs during CPR. This oxygen then reaches the blood and organs. It helps prevent brain damage and supports life. Without ventilation, the body quickly runs out of oxygen. Rescue breaths are part of CPR to supply this oxygen. They must be done correctly to be effective.
How Ventilation Supports Circulation
Ventilation and circulation work together during CPR. Chest compressions pump blood through the body. Ventilation adds oxygen to that blood. Oxygen-rich blood reaches the heart and brain. This keeps cells healthy and functioning. Proper ventilation rate ensures enough oxygen but avoids lung injury. Both must be balanced for the best results.
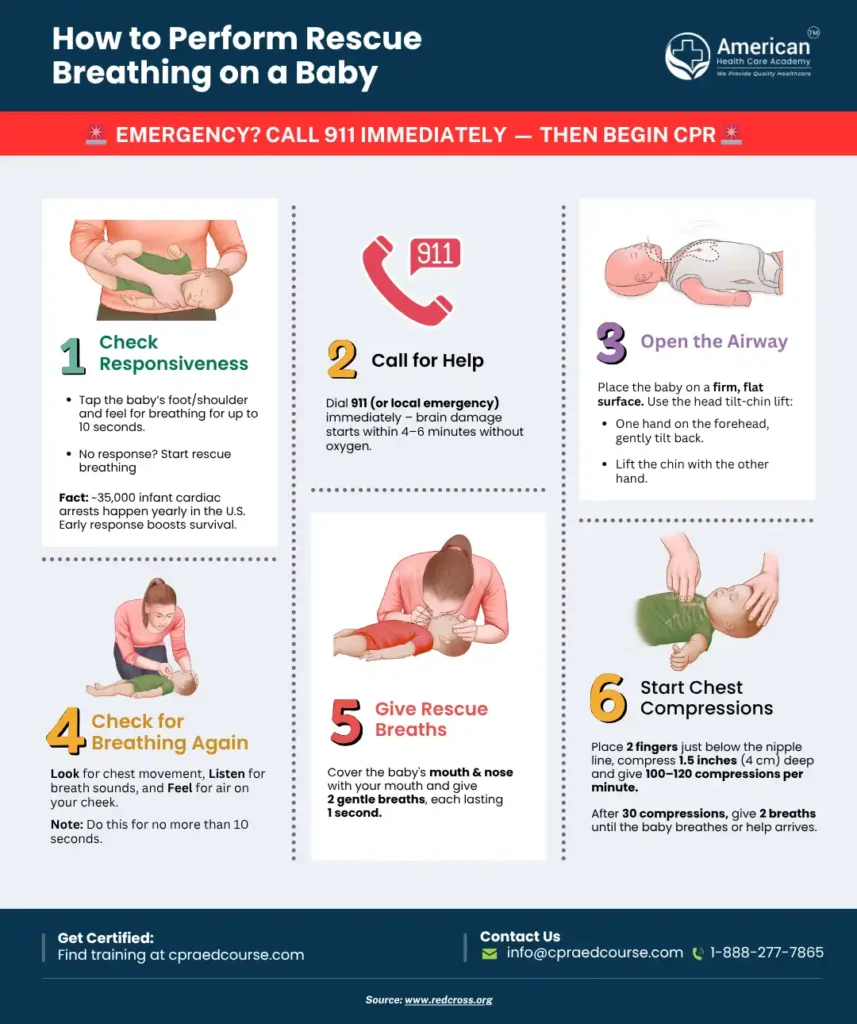
Credit: cpraedcourse.com
Recommended Ventilation Rates
Correct ventilation rate plays a vital role in effective CPR. It helps supply oxygen to the lungs and vital organs. Following recommended rates ensures the best chance of survival and reduces complications. Ventilation rates differ by age and the type of life support provided. Understanding these guidelines helps responders deliver proper breaths during CPR.
Adult Ventilation Guidelines
For adults, give 1 breath every 6 seconds during CPR. That equals about 10 breaths per minute. Each breath should last about 1 second and make the chest rise visibly. Avoid giving breaths too fast or too slow. Too many breaths can cause stomach inflation and reduce blood flow.
Child And Infant Ventilation Rates
Children and infants need breaths more often than adults. Deliver 1 breath every 2 to 3 seconds. This means 20 to 30 breaths per minute. Use gentle breaths to avoid lung injury. Watch for chest rise to confirm proper ventilation. Use mouth-to-mouth or a mask as appropriate.
Differences For Advanced Vs. Basic Life Support
Basic Life Support (BLS) focuses on chest compressions and rescue breaths. Ventilation rates follow the standard guidelines for adults, children, and infants. Advanced Life Support (ALS) providers use advanced airway devices. Once an advanced airway is in place, give breaths every 6 seconds without pausing compressions. This allows continuous blood flow and oxygen delivery during CPR.
Techniques For Effective Ventilation
Effective ventilation is vital during CPR to supply oxygen to the lungs. Proper techniques ensure air reaches the lungs without causing harm. Understanding these methods can improve the chances of survival.
Mouth-to-mouth Method
This traditional method involves sealing your mouth over the person’s mouth. Pinch the nose shut to prevent air from escaping. Deliver slow, steady breaths lasting about one second each. Watch for the chest to rise, indicating air entry. Avoid giving breaths too fast or too forcefully.
Use Of Bag-valve-mask Devices
A bag-valve-mask (BVM) device helps deliver breaths efficiently. Place the mask firmly over the person’s nose and mouth. Squeeze the bag gently to push air into the lungs. This method provides more oxygen than mouth-to-mouth. Training is necessary to use a BVM correctly.
Proper Head Positioning
Head position opens the airway for effective ventilation. Tilt the head back slightly by lifting the chin. Avoid pressing on the soft tissues under the chin. Check the mouth for any blockages before giving breaths. Proper positioning prevents air from entering the stomach.

Credit: www.youtube.com
Common Ventilation Mistakes
Ventilation during CPR is a critical skill that can determine the outcome for the person in need. Yet, many rescuers make common mistakes that can reduce the effectiveness of their efforts. Understanding these errors helps you avoid them and provide better care in emergencies.
Overventilation Risks
Giving too many breaths or blowing too hard can cause serious problems. Overventilation increases pressure in the chest, making it harder for the heart to pump blood effectively. It may also lead to stomach inflation, which raises the risk of vomiting and choking.
Have you ever felt the urge to breathe faster under stress? That natural reaction can cause you to overventilate during CPR. Staying calm and sticking to the recommended rate—about one breath every 6 seconds—helps protect the patient.
Underventilation Consequences
On the flip side, giving too few breaths or not enough air means the body gets less oxygen. This can cause the brain and organs to suffer from low oxygen, worsening the person’s condition. Even if chest compressions are perfect, underventilation still harms the chances of survival.
Think about how slow or shallow breathing feels when you’re tired—this is similar to what happens if you don’t provide enough ventilation during CPR. Make sure your breaths are deep enough to cause the chest to rise visibly, signaling effective ventilation.
Avoiding Airway Obstructions
Keeping the airway open is essential for air to reach the lungs. Common mistakes include not tilting the head back enough or missing a blockage in the mouth. Even a small obstruction can prevent air from entering and ruin your ventilation efforts.
Have you ever choked on food? That feeling shows how quickly an airway blockage can stop breathing. Before giving breaths, always perform a quick look and sweep of the mouth if you see any visible objects. Proper head tilt and chin lift techniques open the airway efficiently and improve your success rate.
Adjustments In Special Situations
Special situations need changes in CPR ventilation rates to match the patient’s condition. Correct breaths help keep oxygen flowing without causing harm. Adjusting the rate ensures effective support during emergencies.
In the realm of CPR, knowing the correct ventilation rate is crucial. Yet, there are special situations where standard protocols need adjustments. These scenarios require quick thinking and adaptation to ensure the best possible outcome for the patient. Let’s dive into some of these unique circumstances and explore how they can impact your approach to CPR.Ventilation During Cpr With An Advanced Airway
When an advanced airway is in place, the dynamics of CPR change significantly. Continuous chest compressions become a priority, while ventilation is provided at a rate of 10 breaths per minute. This setup allows for uninterrupted compressions, which are vital for maintaining blood flow. Have you ever wondered how this affects oxygen delivery? With the advanced airway, the simultaneous compressions and ventilations optimize oxygenation without losing the rhythm. It’s a seamless synergy that requires precision and coordination from the resuscitation team.Handling Ventilation In Drowning Cases
Drowning victims present a unique challenge in CPR, as their primary issue is often hypoxia. Immediate and effective ventilation is critical to restore oxygen levels. The usual CPR protocol may need to be adjusted to focus more on ventilation. Think about the importance of clearing water from the airway before delivering breaths. This step ensures that air, not water, reaches the lungs. In such cases, it’s crucial to act swiftly but carefully to maximize recovery chances.Considerations For Covid-19 And Infectious Patients
The COVID-19 pandemic has reshaped how we approach CPR, especially concerning ventilation. Protecting both the rescuer and patient is paramount, making personal protective equipment (PPE) essential. This can alter the speed and efficiency of ventilation delivery. How do you balance safety with effectiveness? Using barrier devices and minimizing direct mouth-to-mouth contact are key strategies. Additionally, adjusting ventilation techniques to reduce aerosol generation helps protect everyone involved, maintaining safety without compromising care.Latest Research And Updates
Staying updated with the latest research on CPR ventilation rates is crucial for anyone involved in emergency care. Recent studies have refined our understanding of how often and how much air should be delivered during CPR to improve survival rates and reduce complications. Let’s dive into the evolving guidelines, expert debates, and what the future might hold for CPR ventilation.
Changes In Guidelines Over Time
CPR ventilation rates have shifted significantly over the years. Earlier protocols recommended delivering breaths every 5 to 6 seconds, but newer evidence suggests a slower rate can be more effective.
For example, the American Heart Association now advises giving one breath every 6 to 8 seconds for adults during CPR, which balances oxygen delivery without causing excessive chest pressure. These changes reflect a better understanding of how ventilation impacts blood flow and oxygenation during resuscitation.
Expert Opinions And Controversies
Experts don’t always agree on the ideal ventilation rate, which can confuse those learning CPR. Some argue that more frequent breaths risk over-inflating the lungs, reducing blood flow to vital organs.
Others believe that in certain situations, such as drowning or pediatric cases, faster ventilation is necessary to meet oxygen demands. This ongoing debate highlights how CPR must be tailored to the patient’s condition, not just follow a fixed rate.
Future Directions In Cpr Ventilation
Technology and new research are paving the way for more personalized CPR techniques. Devices that monitor real-time oxygen levels and lung pressures could guide rescuers on exactly when and how much to ventilate.
Imagine CPR with smart feedback helping you adjust ventilation rates on the spot—this could drastically improve outcomes. Are you ready to embrace these advancements in life-saving skills?
Frequently Asked Questions
What Is The Recommended Ventilation Rate For Adult Cpr?
The recommended ventilation rate for adult CPR is 10 to 12 breaths per minute. Provide one breath every 5 to 6 seconds. This ensures adequate oxygen delivery without causing lung injury or excessive chest pressure.
How Many Breaths Per Minute Should A Child Receive During Cpr?
For children, the ventilation rate during CPR is about 12 to 20 breaths per minute. This means one breath every 3 to 5 seconds, supporting their higher metabolic needs effectively.
Why Is Correct Ventilation Rate Important In Cpr?
Correct ventilation rates prevent over-ventilation, which can reduce blood flow to the heart. It also avoids under-ventilation, ensuring the brain gets enough oxygen during resuscitation.
Does Ventilation Rate Differ Between Cpr With And Without Advanced Airway?
Yes. With an advanced airway, give continuous breaths at 10 per minute without pausing chest compressions. Without an airway, provide 2 breaths after every 30 compressions.
Conclusion
Correct ventilation rate during CPR saves lives and improves outcomes. Deliver breaths steadily, about one every 5 to 6 seconds. Avoid giving too many or too few breaths. Keep the chest rising with each breath but do not overinflate. Proper timing helps oxygen reach the lungs and brain.
Always follow updated CPR guidelines from trusted sources. Practice ensures quick and confident response in emergencies. Stay calm, focus on steady breaths, and keep chest compressions going. This knowledge can make a real difference in critical moments.