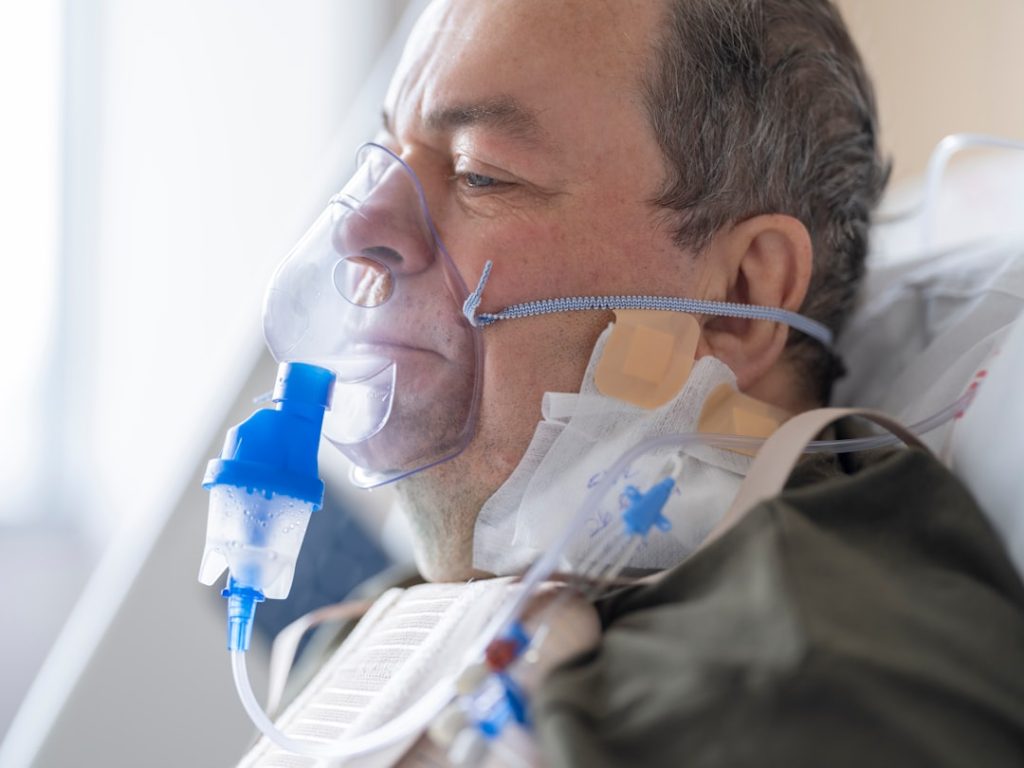
When it comes to helping someone breathe during a medical emergency or critical illness, the method used to ventilate a patient can make all the difference. You might wonder which technique is safest, most effective, or easiest to manage.
Understanding the preferred method of ventilation can help you feel more confident if you ever face such a situation—whether as a healthcare provider, caregiver, or even a concerned family member. Keep reading to discover the key approaches and why one stands out as the best choice for patient care.
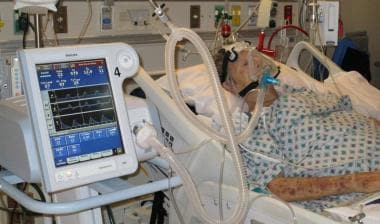
Credit: emedicine.medscape.com
Types Of Ventilation Methods
Ventilation supports patients who cannot breathe well on their own. It helps deliver oxygen and remove carbon dioxide. Various types of ventilation methods exist. Each suits different patient needs and conditions. Understanding these methods aids in choosing the right care.
Invasive Ventilation
Invasive ventilation uses a tube inserted into the airway. This tube connects to a mechanical ventilator. It controls breathing by pushing air into the lungs. This method is common in critical care or surgery. It allows precise control of oxygen and air pressure.
Risks include infection and damage to the airway. Patients often require sedation during this process. It is usually reserved for severe breathing problems.
Non-invasive Ventilation
Non-invasive ventilation uses masks or similar devices. It delivers air without needing a tube inside the airway. This method is less risky and more comfortable. It helps patients with mild to moderate breathing issues.
Common types include CPAP and BiPAP machines. These support breathing during sleep or lung disease flare-ups. The mask fits tightly over the nose or mouth. It improves oxygen levels and reduces work of breathing.
High-frequency Ventilation
High-frequency ventilation uses rapid breaths with small volumes of air. It differs from regular ventilation by delivering breaths very fast. This technique protects the lungs from injury. It is often used in newborns or severe lung injury cases.
This method requires special ventilators and skilled care. It helps maintain oxygen while minimizing lung stress. High-frequency ventilation is a specialized option for critical patients.
Criteria For Choosing Ventilation
Choosing the right ventilation method for a patient requires careful consideration of several key factors. These criteria help healthcare providers tailor respiratory support to the patient’s specific needs, improving outcomes and minimizing complications. Understanding these elements puts you in a better position to grasp why one approach is preferred over another in different situations.
Patient Condition And Diagnosis
Your patient’s overall health and underlying diagnosis directly influence ventilation choices. For example, someone with chronic obstructive pulmonary disease (COPD) might benefit more from non-invasive ventilation to avoid airway trauma. On the other hand, a patient with severe trauma or airway obstruction may require invasive mechanical ventilation to secure the airway.
Consider the presence of comorbidities like heart failure or neurological impairment as well. These can change how the patient tolerates certain ventilation methods. Have you ever noticed how two patients with similar respiratory issues respond differently based on their other health problems?
Severity Of Respiratory Failure
The level of respiratory distress plays a huge role in deciding ventilation strategy. Mild to moderate respiratory failure might be managed effectively with less invasive support like CPAP or BiPAP. Severe respiratory failure often demands invasive ventilation to ensure adequate oxygenation and carbon dioxide removal.
Assessing blood gas levels and clinical signs helps determine severity quickly. You might find that early intervention with the right ventilation reduces the risk of further lung injury. What signs do you look for to decide when non-invasive methods are no longer sufficient?
Duration Of Ventilation Needed
How long the patient will need ventilatory support also matters. Short-term ventilation, such as during surgery or acute episodes, may lean towards invasive methods for secure airway control. For longer-term support, non-invasive ventilation can help reduce complications like infections or vocal cord damage.
Planning ahead for ventilation duration helps avoid unnecessary risks. Sometimes, switching from invasive to non-invasive ventilation as the patient improves makes a big difference in recovery speed. Have you considered how the expected timeline impacts your ventilation choice?
Advantages Of Invasive Ventilation
Invasive ventilation offers distinct advantages that make it a preferred choice in many critical care scenarios. It provides a higher level of control and reliability, especially for patients whose breathing is severely compromised. Understanding these benefits can help you grasp why invasive ventilation remains essential in intensive medical care.
Control Over Airway And Breathing
Invasive ventilation gives medical professionals direct control over the patient’s airway. This means the airway is secured with a tube, reducing the risk of obstruction or aspiration.
You can adjust the breathing rate, volume, and oxygen concentration precisely to meet the patient’s needs. This control is crucial when spontaneous breathing isn’t sufficient or safe.
Suitability For Severe Cases
Patients with severe respiratory failure or trauma often require invasive ventilation. It supports breathing when non-invasive methods are ineffective or impossible due to the patient’s condition.
For instance, if your lungs are damaged or swollen, invasive ventilation can maintain adequate oxygen levels and carbon dioxide removal, helping prevent further complications.
Monitoring And Adjustments
Invasive ventilation allows continuous monitoring of key respiratory parameters like airway pressure and lung compliance. This real-time data enables quick adjustments to optimize ventilation settings.
Imagine being able to instantly change the support level based on how your lungs respond—this adaptability can improve outcomes and reduce risks.

Credit: www.jacc.org
Benefits Of Non-invasive Ventilation
Non-invasive ventilation (NIV) offers many advantages for patients needing breathing support. It helps improve breathing without inserting tubes into the airway. This method supports lung function while reducing many risks linked to invasive ventilation. Patients often tolerate NIV better, making treatment smoother and more effective.
Reduced Risk Of Infection
NIV avoids the need for a breathing tube through the throat. This lowers the chance of bacteria entering the lungs. It reduces infections like pneumonia, common in invasive ventilation. Fewer infections mean faster recovery and less hospital time.
Patient Comfort And Mobility
NIV uses masks or nasal devices, which are less painful. Patients can speak, eat, and drink while receiving support. This freedom improves comfort and helps maintain normal activities. Patients can move more freely, aiding faster healing and better mental health.
Use In Moderate Respiratory Distress
NIV works well for patients with moderate breathing problems. It helps improve oxygen levels and reduces breathing effort. Early use can prevent worsening and avoid the need for invasive ventilation. This approach supports breathing while keeping patients safer and more comfortable.
Expert Recommendations
Expert recommendations on ventilating patients highlight the importance of evidence-based choices tailored to individual needs. These insights come from a mix of authoritative guidelines, real-world clinical experiences, and evolving practices. Understanding these recommendations can help you grasp why certain ventilation methods are preferred in specific situations.
Guidelines From Medical Societies
Leading medical organizations such as the American Thoracic Society and the European Society of Intensive Care Medicine emphasize lung-protective ventilation strategies. They recommend using lower tidal volumes (6 ml/kg of predicted body weight) to reduce lung injury risks. Additionally, they suggest careful monitoring of plateau pressures to keep them below 30 cm H₂O for safer ventilation.
These guidelines also stress individualized settings based on patient condition rather than a one-size-fits-all approach. Are you aware of how these standards influence the choice between invasive and non-invasive ventilation in critical care?
Case Studies And Clinical Trials
Clinical trials provide concrete evidence supporting specific ventilation methods. For example, studies comparing non-invasive ventilation (NIV) with invasive mechanical ventilation (IMV) in COPD exacerbations show NIV reduces complications and mortality. Such case studies illustrate how patient outcomes improve when ventilation matches the underlying condition.
One interesting trial revealed that early use of high-flow nasal cannula (HFNC) oxygen therapy can reduce the need for intubation in hypoxemic respiratory failure. These findings challenge traditional reliance on invasive methods and encourage you to consider less invasive options when appropriate.
Trends In Ventilation Practices
Recent trends favor personalized ventilation strategies and the integration of new technologies. You might notice an increase in the use of advanced ventilators that adapt in real-time to a patient’s breathing patterns. This shift aims to enhance comfort while minimizing lung damage.
Moreover, the adoption of protocols combining sedation management with ventilation settings has gained traction. This holistic approach encourages you to think beyond just the ventilator and consider the entire patient experience. How might embracing these trends change your perspective on patient ventilation?
Technological Innovations
In recent years, technological innovations have significantly improved the way we ventilate patients, making the process more efficient and patient-friendly. These advancements offer healthcare professionals new tools to enhance patient care, optimize treatment outcomes, and reduce complications. Let’s explore some of the leading technological innovations in patient ventilation that are reshaping the healthcare landscape.
Advanced Ventilator Modes
Modern ventilators now come with advanced modes that cater to individual patient needs. Adaptive support ventilation (ASV) and neurally adjusted ventilatory assist (NAVA) are just a couple of examples.
ASV automatically adjusts the breathing pattern based on the patient’s lung mechanics and effort, reducing the need for manual settings. NAVA, on the other hand, uses the patient’s own respiratory signals to tailor ventilation, providing a more comfortable and synchronized experience.
Remote Monitoring Systems
Remote monitoring systems have become a game-changer in patient ventilation. These systems allow healthcare providers to keep an eye on patients’ respiratory status from a distance, ensuring timely interventions.
Imagine being able to adjust ventilator settings without being physically present at the bedside. This not only frees up time for clinicians but also ensures that patients receive the most appropriate care, even in the middle of the night.
Artificial Intelligence In Ventilation
Artificial Intelligence (AI) is making waves in the medical field, and ventilation is no exception. AI algorithms can analyze vast amounts of data to predict patient outcomes and suggest optimal ventilator settings.
AI-driven systems can alert medical teams about potential issues before they become critical, allowing for proactive management. How might AI redefine the boundaries of patient care in the future?
These technological innovations are not just transforming patient care; they are enhancing the capabilities of healthcare providers. As you consider these advancements, think about how they might impact the future of healthcare and patient treatment.
Challenges And Considerations
Ventilating a patient effectively is more than just choosing the right equipment. You must navigate a complex landscape of challenges and considerations that affect outcomes. Understanding these hurdles helps you prepare better and respond faster.
Complications And Risks
Every ventilation method carries potential complications. For example, improper settings can cause lung injury or oxygen toxicity.
Ventilation may also lead to infections like ventilator-associated pneumonia. Monitoring closely and adjusting treatment promptly is crucial to avoid these risks.
Have you ever encountered unexpected patient reactions? These moments highlight why vigilance is key during ventilation.
Resource Availability
Not all healthcare settings have the same tools. You might have access to advanced ventilators in a hospital, but what if you’re in a remote clinic?
Limited resources force you to adapt. Simple manual ventilation devices can be lifesaving when machines are unavailable or malfunctioning.
Consider how resource constraints shape your approach and decision-making. What creative solutions have you seen or used under pressure?
Training And Expertise
Ventilation demands skill and knowledge. Proper training ensures you set the ventilator correctly and respond to patient needs effectively.
Even the best equipment is useless without expertise. Regular drills and continued education keep your skills sharp and your confidence high.
Think about the last time you learned a new technique or updated your knowledge. How did that change your patient care?

Credit: www.sentec.com
Frequently Asked Questions
What Is The Best Method For Patient Ventilation?
The preferred method is mechanical ventilation using a ventilator. It supports breathing when patients cannot breathe independently. This method ensures consistent oxygen delivery and effective carbon dioxide removal.
When Should Non-invasive Ventilation Be Used?
Non-invasive ventilation is ideal for patients with mild to moderate respiratory failure. It avoids intubation and reduces complications. Masks or nasal devices deliver pressurized air to support breathing.
How Does Invasive Ventilation Differ From Non-invasive?
Invasive ventilation involves inserting an endotracheal tube into the airway. Non-invasive uses masks without tubes. Invasive ventilation is for severe respiratory distress or when non-invasive methods fail.
Why Is Proper Ventilation Important For Patient Outcomes?
Proper ventilation maintains adequate oxygen levels and removes carbon dioxide. It prevents lung injury and supports organ function. Effective ventilation improves recovery and reduces mortality risk.
Conclusion
Choosing the right way to ventilate a patient saves lives. Doctors must assess each case carefully. The preferred method depends on the patient’s condition and needs. Clear breathing helps the body get oxygen and heal faster. Simple tools often work well but advanced support may be needed too.
Good ventilation improves comfort and recovery chances. Always follow expert advice and monitor patients closely. Proper care makes a big difference in outcomes. Understanding ventilation helps everyone support better health.