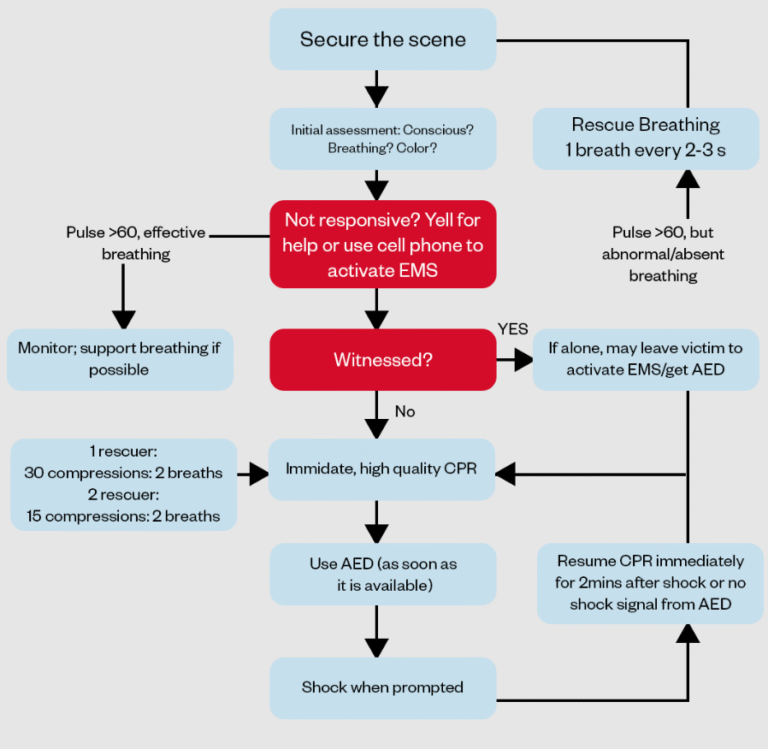
When it comes to managing advanced airways, knowing the right ventilation rate can make all the difference in your patient’s outcome. If you’re unsure about how fast or slow to ventilate, you’re not alone.
Getting this rate just right helps ensure your patient gets enough oxygen without causing harm. You’ll discover clear, practical guidelines on the recommended ventilation rate with advanced airway devices. By the end, you’ll feel confident in your approach and ready to apply this knowledge when it matters most.
Keep reading to learn exactly what you need to know.
Ventilation Rate Basics
Understanding the basics of ventilation rate is crucial for effective airway management. Ventilation rate refers to how many breaths are given per minute during advanced airway support. Getting this rate right ensures the patient receives enough oxygen without causing harm.
Proper ventilation helps maintain stable blood oxygen and carbon dioxide levels. It supports vital organ function and aids in patient recovery. The correct rate varies depending on the patient’s condition and age but generally stays within recommended guidelines.
Importance Of Proper Ventilation
Proper ventilation keeps oxygen flowing to the lungs and bloodstream. It prevents oxygen deprivation, which can damage organs and tissues. Correct rates also help remove carbon dioxide from the body efficiently.
Controlled ventilation reduces the risk of lung injury. It avoids overinflation and pressure buildup in the lungs. Delivering the right breath volume and rate supports better patient outcomes during emergencies or surgery.
Effects Of Incorrect Rates
Too fast ventilation can cause low carbon dioxide levels, leading to dizziness or heart issues. It may also increase pressure in the chest, reducing blood flow back to the heart.
Too slow ventilation causes carbon dioxide buildup, making the blood acidic. This can harm organs and worsen the patient’s condition. Both extremes can delay recovery or cause further complications.
Maintaining the recommended ventilation rate is key. It balances oxygen delivery and carbon dioxide removal effectively. This balance supports overall patient health during advanced airway care.
Advanced Airway Techniques
Advanced airway techniques are essential tools in emergency and critical care settings. They help secure a patient’s airway and ensure adequate ventilation, especially when basic methods fall short. Understanding these techniques allows you to provide more effective respiratory support and improve patient outcomes.
Types Of Advanced Airways
There are several types of advanced airways you should be familiar with:
- Endotracheal Tube (ETT):Inserted through the mouth or nose into the trachea, it provides a secure airway and protects against aspiration.
- Laryngeal Mask Airway (LMA):A supraglottic device that sits above the vocal cords, easier to place than an ETT but less protective.
- Combitube:A dual-lumen device used when intubation is difficult, allowing ventilation even if placed in the esophagus.
Each device has its specific use case, advantages, and limitations. Knowing these helps you choose the right airway for the situation quickly.
Placement Considerations
Correct placement of advanced airways is critical. Misplacement can lead to inadequate ventilation or injury.
Before insertion, assess the patient’s anatomy and condition. Factors like jaw mobility, neck size, and presence of trauma affect your approach.
After placement, confirm the airway’s position using capnography, chest rise, and breath sounds. Continuous monitoring is vital to catch any displacement early.
Have you ever struggled with airway placement under pressure? Practicing techniques regularly can build confidence and reduce errors when every second counts.
Recommended Rates By Experts
Experts agree that the right ventilation rate is crucial when managing an advanced airway. Too fast or too slow can both cause serious problems. Understanding the recommended rates helps you provide safe and effective care, whether you’re working with adults, children, or newborns.
Adult Ventilation Rates
For adults, experts recommend delivering ventilations at a rate of 10 to 12 breaths per minute. That means about one breath every 5 to 6 seconds. This rate supports adequate oxygen delivery without causing excessive pressure in the lungs.
Have you noticed how quick breaths can sometimes make patients feel uncomfortable? Keeping the pace steady can prevent complications like gastric inflation or reduced blood flow to the heart. Focus on smooth, controlled breaths rather than rushing through them.
Pediatric Ventilation Rates
Children require faster ventilation rates than adults. The advised rate is around 12 to 20 breaths per minute. That breaks down to one breath every 3 to 5 seconds, depending on the child’s age and size.
Think about how a child’s smaller lungs and faster metabolism affect their breathing needs. Delivering the right rate ensures they get enough oxygen without overinflating their lungs. If you’re uncertain, err on the side of gentler, more frequent breaths to match their natural rhythm.
Neonatal Ventilation Rates
Newborns have the highest ventilation rates, typically 40 to 60 breaths per minute. This means giving one breath approximately every 1 to 1.5 seconds. Their tiny lungs and high oxygen demands make precise timing critical.
When I first assisted in neonatal resuscitation, I realized how easily improper rates can affect outcomes. Even small delays or rushed breaths can lead to poor oxygen exchange. Pay close attention to the rhythm and volume to support these vulnerable patients effectively.

Credit: www.youtube.com
Guideline Sources
Guideline sources provide trusted recommendations on ventilation rates with advanced airways. These guidelines help healthcare providers give safe and effective care during resuscitation. Different organizations offer specific advice based on research and clinical experience.
American Heart Association
The American Heart Association (AHA) sets widely accepted standards for advanced airway ventilation. It recommends delivering one breath every 6 seconds, which equals 10 breaths per minute. This rate helps maintain proper oxygen levels and avoids lung injury. The AHA also stresses the importance of monitoring chest rise and avoiding excessive ventilation.
European Resuscitation Council
The European Resuscitation Council (ERC) provides clear ventilation guidelines for advanced airways. They advise the same rate as the AHA: 10 breaths per minute. The ERC highlights gentle, controlled breaths to reduce complications. Their guidelines emphasize coordination between chest compressions and ventilation for better patient outcomes.
Other Key Organizations
Several other groups contribute to ventilation recommendations:
- The International Liaison Committee on Resuscitation (ILCOR) supports consistent ventilation rates worldwide.
- The World Health Organization (WHO) offers guidance for emergency airway management in resource-limited settings.
- Specialty societies, such as those for anesthesiology or critical care, provide tailored advice for specific patient groups.
Each organization bases its advice on clinical evidence and aims to improve survival rates during resuscitation.
Adjusting Ventilation Rates
Recommended ventilation rates with an advanced airway are typically 10 breaths per minute. Each breath should last about one second to ensure proper oxygen delivery. Adjusting the rate helps maintain stable carbon dioxide levels and supports patient safety.
Adjusting ventilation rates is essential in medical care with advanced airways. Proper ventilation ensures the patient receives the right amount of oxygen. It can be life-saving in critical situations. Ventilation rates depend on several factors. These include patient condition and continuous monitoring.Patient Condition Factors
Different patients have different needs. Age, health, and medical history affect ventilation. A child needs a different rate than an adult. Conditions like asthma or COPD also influence rates. Clinicians must adjust based on these conditions. They assess the patient’s current state and adjust accordingly.Monitoring And Feedback
Monitoring equipment provides real-time data. It helps track the effectiveness of ventilation. Feedback from these tools is crucial. It allows for adjustments to meet patient needs. Monitoring ensures the patient is stable. It also helps prevent complications. This data-driven approach enhances patient safety and care quality.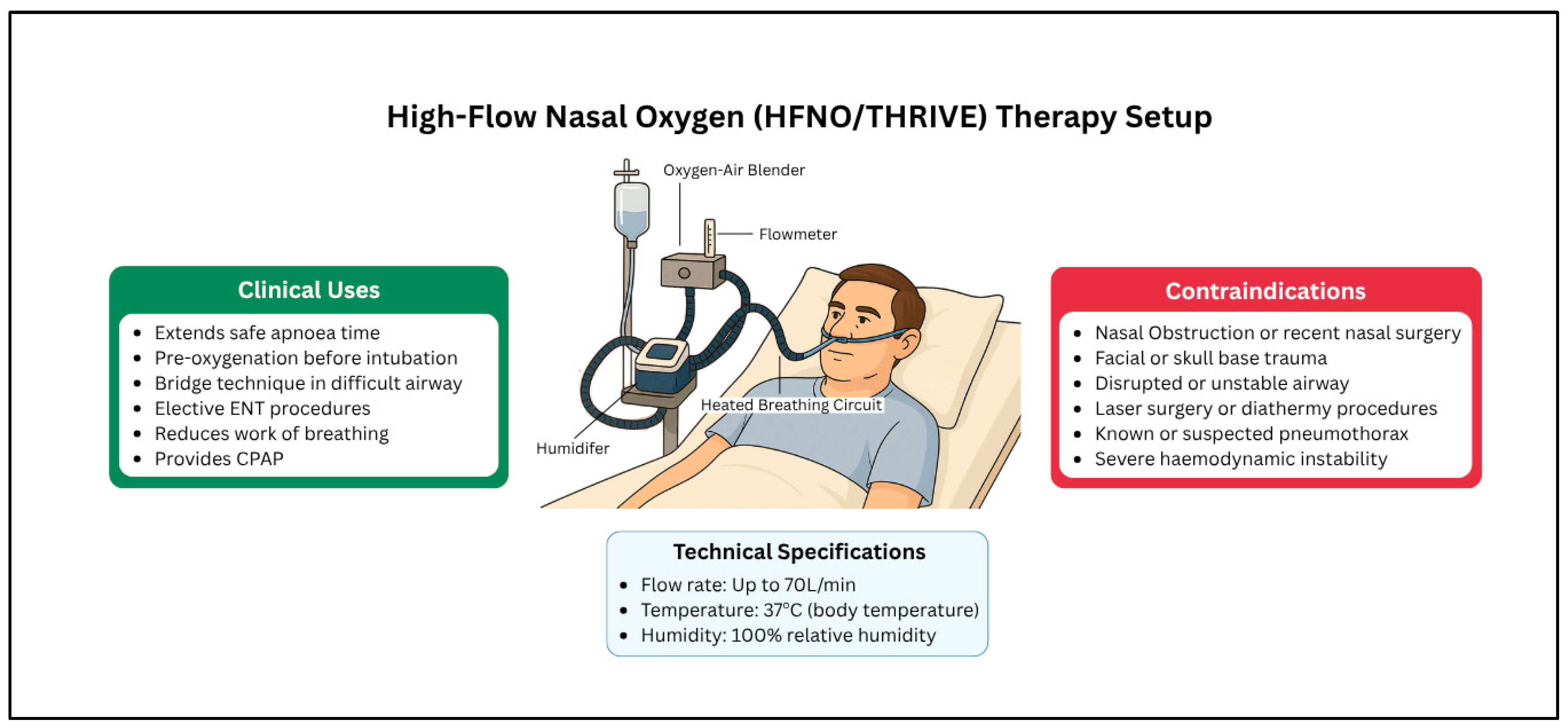
Credit: www.mdpi.com
Common Mistakes To Avoid
Ensuring the right ventilation rate with an advanced airway is critical, but many make avoidable errors that can affect patient outcomes. Understanding common mistakes helps you provide safer, more effective care. Let’s look at some pitfalls you should watch out for and how to steer clear of them.
Overventilation Risks
Giving too many breaths per minute can cause serious problems. Overventilation increases pressure in the chest, reducing blood flow back to the heart. This may lower cardiac output and worsen the patient’s condition.
Excess carbon dioxide removal can also lead to respiratory alkalosis, which disrupts the body’s acid-base balance. Too much ventilation can cause lung injury by forcing air into fragile alveoli. Have you noticed how easy it is to speed up the rate under stress? It’s crucial to maintain control and stick to recommended rates.
Underventilation Consequences
On the flip side, not giving enough breaths slows oxygen delivery and carbon dioxide removal. This can quickly lead to hypoxia and acidosis, putting vital organs at risk. In emergency settings, underventilation may delay recovery or worsen brain injury.
Many underestimate how dangerous a low ventilation rate can be. It’s tempting to slow down to avoid overventilation, but this creates its own hazards. How often do you pause to check if your ventilation matches the patient’s needs? Adjusting rate based on ongoing assessment is key to avoiding this mistake.

Credit: www.acls.net
Frequently Asked Questions
What Is The Ideal Ventilation Rate With An Advanced Airway?
The recommended ventilation rate with an advanced airway is 10 breaths per minute. This rate ensures adequate oxygen delivery without causing lung injury or reducing cardiac output. It is crucial during resuscitation to maintain proper oxygenation and carbon dioxide removal.
Why Is Controlling Ventilation Rate Important With Advanced Airways?
Controlling ventilation rate prevents hyperventilation, which can cause low carbon dioxide levels and reduce blood flow to the brain. Proper rates improve patient outcomes by balancing oxygenation and circulation during emergency care or anesthesia.
How Does Ventilation Rate Affect Patient Outcomes?
Appropriate ventilation rates optimize oxygen delivery and carbon dioxide removal. Too fast or too slow rates can cause complications like lung damage or poor blood circulation. Maintaining the recommended rate improves survival and neurological outcomes.
Can Ventilation Rates Vary With Patient Condition?
Yes, ventilation rates may vary based on patient age, condition, and clinical guidelines. However, 10 breaths per minute is standard for adults with advanced airways during resuscitation. Adjustments should be made by medical professionals as needed.
Conclusion
Maintaining the right ventilation rate with an advanced airway saves lives. It helps deliver oxygen without causing harm. Too fast or too slow can hurt the patient. Always follow recommended guidelines carefully. Proper ventilation supports better breathing and recovery. Training and practice improve your confidence and skills.
Stay calm and focus on steady breaths. This simple step makes a big difference in emergency care. Remember, clear and controlled ventilation is key.