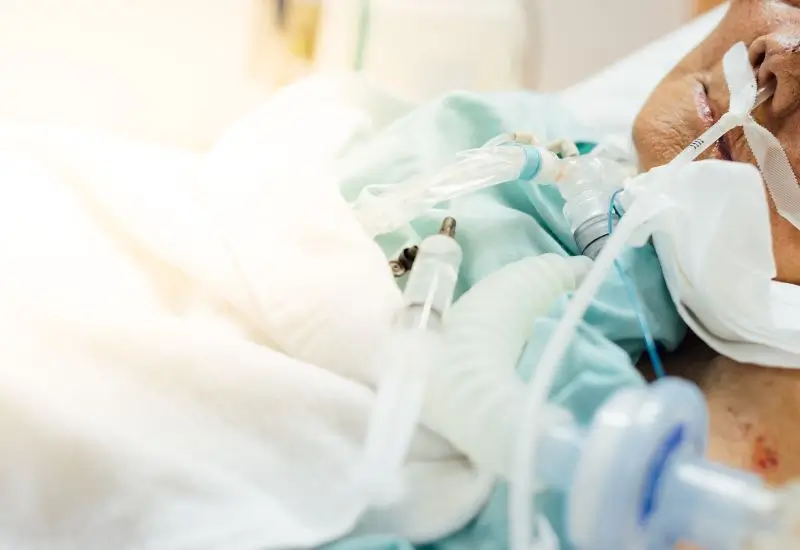
You’ve just heard the good news—your ventilator is being removed. This moment can bring relief, but it also raises many questions.
What changes will you notice? How will your body respond? Understanding what to expect after the ventilator is taken off can help ease your worries and prepare you for the road ahead. You’ll discover the common experiences, possible challenges, and helpful tips to support your recovery.
Keep reading to learn how to take control of this important step in your healing process.

Credit: www.agapehospicepc.org
Physical Changes After Ventilator Removal
After a ventilator is removed, your body begins a crucial recovery phase that includes several physical changes. These changes can affect how you breathe, move, and communicate. Understanding what happens next helps you prepare and manage your recovery more effectively.
Breathing Adjustments
Your lungs need time to regain their strength and normal function once the ventilator is out. You might notice that breathing feels different—sometimes shallow or rapid—because your respiratory muscles have been inactive. This is normal, and with gentle breathing exercises, your lungs will gradually improve their capacity and efficiency.
Have you tried simple deep breathing or pursed-lip breathing? These techniques can reduce discomfort and help you regain control over your breath.
Muscle Weakness
Being on a ventilator often means extended bed rest, which leads to muscle weakness throughout your body. You may feel tired or find everyday movements harder than before. This weakness isn’t permanent, but it requires patience and consistent physical activity to rebuild strength.
Start small by sitting up or walking short distances. Even these small steps can make a big difference in your recovery journey.
Swallowing And Speech Challenges
After ventilator removal, some people experience difficulty swallowing or speaking clearly. This happens because the muscles involved may have weakened or become uncoordinated during ventilation. Speech therapy and swallowing exercises can help you regain these important functions.
Have you noticed changes in your voice or trouble swallowing meals? Addressing these issues early with a therapist can prevent complications and improve your quality of life quickly.

Credit: medicalxpress.com
Emotional And Mental Effects
After the ventilator is removed, many people notice changes not just in their bodies but also in their emotions and mental state. This transition can bring a mix of feelings and cognitive shifts that might catch you off guard. Understanding these emotional and mental effects helps you prepare and manage them better.
Anxiety And Stress
It’s common to feel anxiety or stress once you’re off the ventilator. Your body and mind are adjusting to breathing independently, which can feel overwhelming.
You might experience sudden worries about your health or fear of needing the ventilator again. These feelings are real and valid, but they don’t have to control you.
Try to notice when anxiety spikes. Are there specific triggers, like certain noises or medical equipment? Recognizing these can help you find ways to calm your mind.
Cognitive Changes
Some people notice memory problems, trouble focusing, or slower thinking after ventilator removal. This can be frustrating when you want to get back to normal activities.
Fatigue and medication effects often play a role in these changes. Your brain needs time to heal and regain strength, just like your body.
Have you tried simple exercises like puzzles, reading, or even chatting with a friend? These activities can gently boost your mental sharpness.
Coping Strategies
Managing emotional and mental challenges after ventilator removal starts with patience. Accept that this is a process and give yourself permission to take it slow.
- Talk about your feelings.Share your worries with family, friends, or a counselor.
- Practice relaxation techniques.Deep breathing, meditation, or listening to calming music can reduce stress.
- Set small goals.Focus on daily achievements to build confidence and a sense of control.
What small step can you take today to support your mental health? Even one positive action can shift your outlook and help you move forward.
Recovery Milestones
Recovery after removing a ventilator happens step by step. The body needs time to heal and adjust. Each patient’s journey is unique but shares common milestones. These milestones help track progress and ensure safe recovery.
Regaining Strength
Muscle loss happens quickly during ventilation. Patients often feel weak and tired. Physical therapy helps rebuild muscle and energy. Simple movements start first, like sitting up or walking short distances. Regular activity improves endurance and confidence.
Improving Lung Function
Lungs need time to regain full function. Breathing exercises support lung recovery and capacity. Oxygen levels are carefully checked to ensure proper breathing. Coughing helps clear mucus and prevent infections. Gradual increase in breathing effort is expected.
Monitoring Vital Signs
Doctors watch vital signs closely after ventilator removal. Heart rate, blood pressure, and oxygen levels show how well the body copes. Any sudden changes can signal problems. Continuous monitoring keeps patients safe during recovery. Nurses often record these signs many times daily.

Credit: www.news18.com
Essential Care Tips
After a ventilator is removed, proper care is crucial for a smooth recovery. This stage requires attention to basic needs and health. Essential care supports healing and helps regain strength. Focus on nutrition, therapy, and infection prevention to ensure better outcomes.
Nutrition And Hydration
Good nutrition fuels the body’s recovery process. Meals should be balanced and easy to digest. Include proteins, vitamins, and minerals to rebuild muscle and energy. Hydration is equally important to keep the body functioning well. Offer water, juice, or broth in small, frequent amounts. Monitor fluid intake to avoid dehydration or overload.
Physical Therapy
Physical therapy helps regain muscle strength and movement. Start with gentle exercises tailored to the patient’s ability. Simple stretches and walking support lung and muscle recovery. Consistent therapy reduces stiffness and improves overall mobility. Patience is key as progress may be slow but steady.
Avoiding Infections
Infection risk is high after ventilator removal. Maintain good hygiene around the patient and in their environment. Clean hands thoroughly before and after care activities. Keep wounds or tubes clean and dry. Watch for signs of infection like fever, redness, or swelling. Early detection and treatment prevent serious complications.
Support Systems
Support systems play a vital role after ventilator removal. Family, friends, and healthcare teams offer emotional and physical help. This support aids recovery and builds confidence during the healing process.
Support systems play a crucial role after ventilator removal. Patients need physical and emotional support. This support helps them recover smoothly and regain strength. Different support systems work together for the patient’s well-being. Families, medical teams, and community resources form this network. They provide guidance and care tailored to each patient’s needs.Family And Caregiver Roles
Family members and caregivers provide essential support. They offer emotional comfort and practical help. Their presence reassures patients during recovery. Families help with daily tasks. They ensure the patient follows medical advice. Caregivers assist with mobility and medication management. This close involvement speeds up recovery.Medical Team Involvement
The medical team continues to monitor progress after ventilator removal. Doctors and nurses check vital signs regularly. They adjust treatments as needed. Respiratory therapists work on breathing exercises. These exercises strengthen lungs. Nutritionists ensure the patient receives proper nourishment. This collective effort aims for a full recovery.Community Resources
Community resources extend support beyond the hospital. Local support groups provide a space to share experiences. They offer emotional support and practical tips. Home health services may visit for continued care. These services can include therapy and nursing visits. Community programs also educate families on caregiving skills. This comprehensive support network aids in holistic recovery.When To Seek Medical Help
Knowing when to seek medical help after a ventilator is removed is crucial for your recovery. Your body is adjusting, and some warning signs may indicate complications. Paying attention to these signals can make a significant difference in your health and peace of mind.
Warning Signs
Watch closely for any breathing difficulties, such as shortness of breath or rapid breathing. Persistent coughing, chest pain, or unusual fatigue should not be ignored. If you notice swelling in your legs or face, or if your skin turns blue or pale, these are urgent signs that require immediate attention.
Remember how one patient shared feeling unusually dizzy and weak a few days after coming off the ventilator? That turned out to be a sign of low oxygen levels. Listening to your body can help you avoid serious issues.
Emergency Contacts
Keep a list of emergency contacts handy, including your primary care doctor and the hospital where you received treatment. Make sure family members or caregivers know these numbers too. In case you experience severe symptoms like chest pain or loss of consciousness, call emergency services right away.
- Your primary care physician
- Respiratory therapist or pulmonologist
- Local emergency services (911 or equivalent)
- Close family or friends who can assist
Follow-up Appointments
Attending all scheduled follow-up appointments is essential. These visits allow your healthcare team to monitor your lung function and overall recovery. Missing these could delay identifying problems early on.
During appointments, be honest about any new symptoms, no matter how small they seem. This open communication helps your doctor adjust your care plan effectively. Are you prepared to track your symptoms daily to share with your medical team?
Frequently Asked Questions
What Physical Changes Occur After Ventilator Removal?
After ventilator removal, patients may experience muscle weakness and fatigue. Breathing effort improves gradually. Cough and swallowing reflexes may need monitoring to prevent complications.
How Long Does Recovery Take Post-ventilator?
Recovery time varies by individual health and illness severity. Some improve within days, others take weeks. Physical therapy often aids faster recovery and lung function restoration.
Are Breathing Difficulties Common After Ventilator Removal?
Mild breathing difficulties are common initially. Lungs adjust to independent breathing. Medical staff monitor oxygen levels and provide support if needed.
What Emotional Effects Follow Ventilator Removal?
Patients may feel anxiety or confusion post-removal. Emotional support and counseling help manage stress and promote mental well-being during recovery.
Conclusion
Recovery after a ventilator is a slow, steady process. Breathing feels different at first but grows easier each day. Strength returns as the body heals and muscles get stronger. Doctors and nurses guide every step with care and patience. Emotions may rise and fall, which is normal and expected.
Support from family and friends helps a lot. Remember, healing takes time and effort. Stay positive and follow medical advice closely. Soon, life will feel more normal again. Trust the process and keep moving forward.