If you work with patients on ventilators or want to understand how these machines help save lives, knowing how to read ventilator settings is crucial. It might seem complicated at first, but once you grasp the basics, you’ll feel more confident and in control.
This knowledge not only helps you make better decisions but can also improve patient care. Keep reading, and you’ll discover simple steps to decode ventilator settings quickly and easily—no jargon, just clear explanations designed for you.

Credit: www.anaestheasier.com
Basics Of Ventilator Settings
Understanding ventilator settings is essential for safe and effective patient care. These settings control how air is delivered to the lungs. Knowing the basics helps in monitoring and adjusting the machine correctly. It improves communication among healthcare providers and supports better patient outcomes.
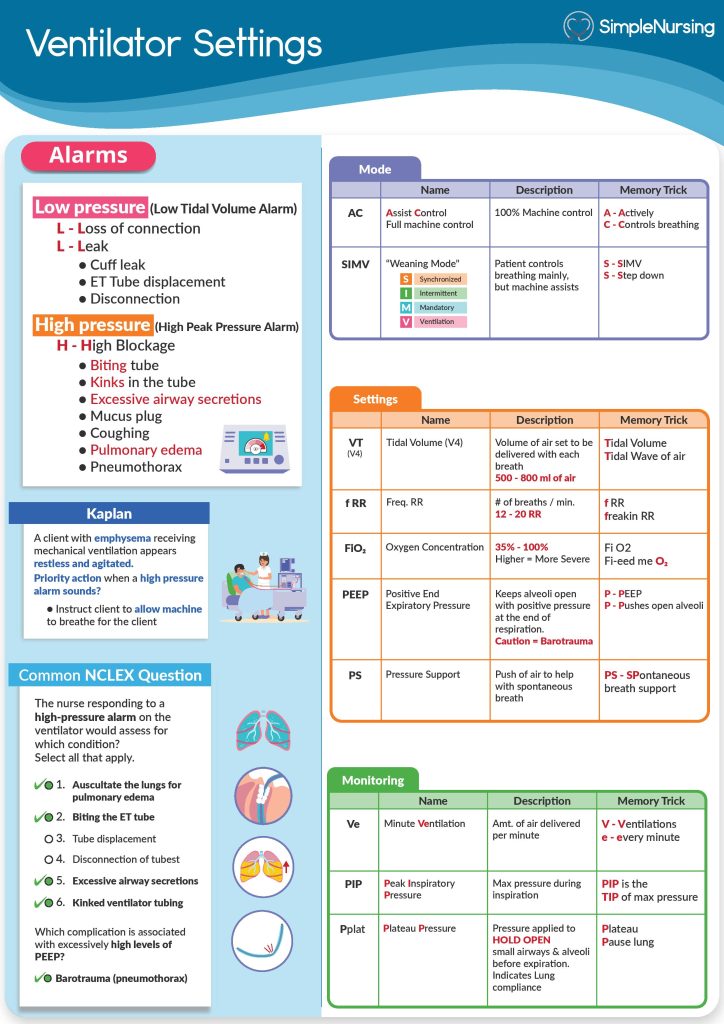
Key Parameters To Know
- Tidal Volume (VT):The amount of air given with each breath.
- Respiratory Rate (RR):Number of breaths per minute.
- FiO2:Fraction of inspired oxygen, or oxygen concentration.
- PEEP:Positive end-expiratory pressure, keeps lungs open after exhalation.
- Inspiratory Pressure:Pressure used to deliver air during inhalation.
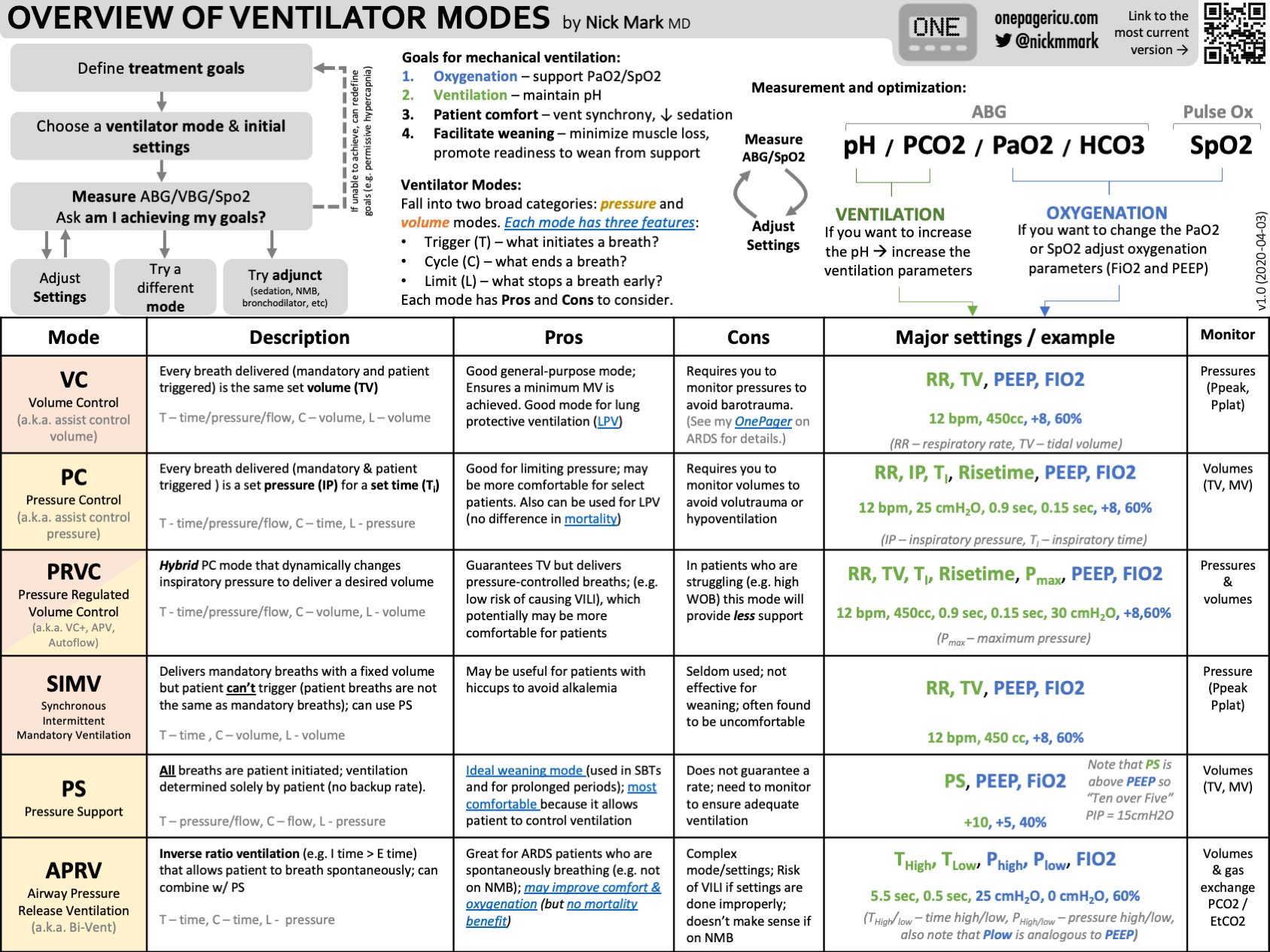
Types Of Ventilation Modes
- Assist-Control (AC):Machine delivers set breaths, patient can trigger extra breaths.
- SIMV (Synchronized Intermittent Mandatory Ventilation):Mix of machine and patient breaths.
- Pressure Support Ventilation (PSV):Patient controls breathing, machine supports effort.
- CPAP (Continuous Positive Airway Pressure):Provides constant pressure to keep airways open.
Common Terminology
- Trigger:How the ventilator detects patient effort to start a breath.
- Cycle:How the machine ends the breath delivery.
- Compliance:Lung’s ability to stretch and expand.
- Resistance:Obstruction to airflow in the airways.
- Alarm Settings:Alerts for changes in pressure, volume, or disconnection.
Interpreting Pressure Settings
Interpreting pressure settings on a ventilator can feel overwhelming at first. Yet, understanding these numbers is key to ensuring your patient’s lungs are protected and receiving adequate support. Let’s break down the main pressure parameters you’ll encounter and why they matter to your patient’s care.
Peak Inspiratory Pressure
Peak Inspiratory Pressure (PIP) shows the highest pressure reached during a breath. It reflects how much force the ventilator uses to push air into the lungs.
If PIP is too high, it might indicate airway resistance or stiff lungs, which can cause damage. You might notice PIP rising if secretions block the airway or if the tube is kinked. Ask yourself: is this pressure necessary, or can it be lowered safely?
Positive End-expiratory Pressure
Positive End-Expiratory Pressure (PEEP) keeps the lungs open at the end of exhalation. It prevents alveoli from collapsing, improving oxygen exchange.
Too little PEEP can cause lung areas to collapse, but too much can overinflate the lungs. Adjusting PEEP requires balancing oxygen needs with lung protection—what’s the minimum PEEP that keeps oxygen levels stable?
Plateau Pressure
Plateau Pressure is measured during a pause in inhalation when airflow stops. It reflects the pressure in the small airways and alveoli, indicating lung compliance.
A high plateau pressure suggests stiff lungs and higher risk of injury. You want to keep this pressure below 30 cm H2O to reduce damage. Consider how changes in patient position or sedation might affect this value.
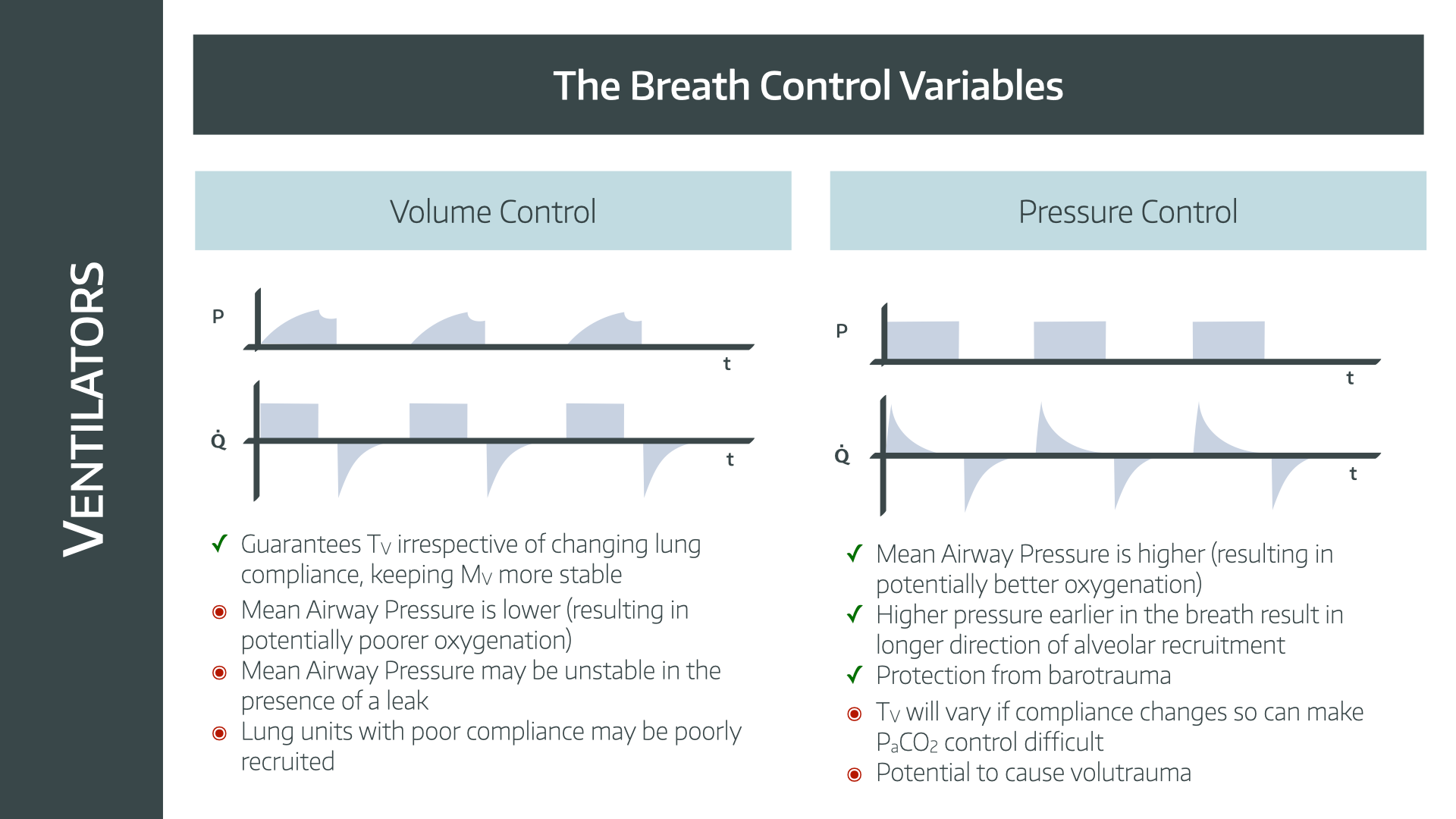
Understanding Volume Controls
Understanding volume controls is key to reading ventilator settings accurately. These controls manage the amount of air delivered to the patient’s lungs. Proper volume settings ensure effective breathing support while avoiding lung injury. Each volume parameter plays a specific role in ventilation management.
Tidal Volume
Tidal volume is the amount of air given to the lungs with each breath. It is usually measured in milliliters (mL). Setting the right tidal volume helps maintain proper oxygen and carbon dioxide levels. Too high a tidal volume can cause lung damage. Too low may lead to insufficient ventilation.
Minute Ventilation
Minute ventilation is the total air volume breathed in one minute. It equals tidal volume multiplied by the number of breaths per minute. This value shows how much air moves in and out of the lungs over time. Monitoring minute ventilation helps adjust breathing rate and volume for better care.
Inspiratory Flow Rate
Inspiratory flow rate controls how fast air enters the lungs during inhalation. It is measured in liters per minute (L/min). A correct flow rate ensures comfort and proper gas exchange. Too fast can cause discomfort. Too slow may reduce ventilation efficiency.
Credit: www.anaestheasier.com
Setting Respiratory Rates
Respiratory rate shows how many breaths a ventilator gives each minute. Adjusting this helps control oxygen and carbon dioxide levels in the body. Knowing the rate ensures proper breathing support for the patient’s needs.
Setting respiratory rates on a ventilator is crucial for patient care. It determines how often a breath is delivered to the patient. Understanding this helps ensure adequate oxygen and carbon dioxide exchange.Spontaneous Vs. Controlled Breaths
Spontaneous breaths are initiated by the patient. The ventilator supports these efforts. Controlled breaths are fully managed by the ventilator. It delivers breaths at preset intervals.Adjusting For Patient Needs
Adjust the respiratory rate based on the patient’s condition. Consider factors like age, lung function, and overall health. A higher rate may be needed for some conditions. Lower rates may suit others with different needs. Regularly monitor and reassess settings for effectiveness.Oxygen Delivery Settings
Oxygen delivery settings on a ventilator control how much oxygen the patient receives. Understanding these settings helps ensure the patient gets the right oxygen level for their needs. Proper oxygen delivery supports breathing and prevents complications. The key setting to watch is the fraction of inspired oxygen, or FiO2.
Fio2 Levels
FiO2 stands for the percentage of oxygen in the air a patient breathes. Normal room air has about 21% oxygen. Ventilators can increase this up to 100% if needed.
- Low FiO2 (21-40%) suits patients with mild breathing problems.
- Moderate FiO2 (40-60%) helps patients with moderate oxygen needs.
- High FiO2 (above 60%) supports severe oxygen deficiency.
Doctors adjust FiO2 based on blood oxygen tests and patient condition. The goal is to keep oxygen levels safe and effective.
Oxygen Toxicity Risks
High oxygen levels for a long time can harm the lungs. This harm is called oxygen toxicity. It causes inflammation and tissue damage.
- Symptoms include coughing, chest pain, and difficulty breathing.
- Risk increases with FiO2 over 60% for many hours or days.
- Doctors balance oxygen needs and toxicity risks carefully.
Ventilator settings aim to provide enough oxygen while avoiding these risks. Monitoring and adjustments are essential for patient safety.

Credit: www.icureach.com
Alarms And Safety Features
Ventilator alarms and safety features protect patients by alerting medical staff. They monitor breathing patterns and machine functions. These alerts help prevent harm and ensure proper ventilation. Understanding alarms helps caregivers act quickly and keep patients safe.
Common Alarm Types
- High Pressure Alarm:Signals airway blockage or coughing.
- Low Pressure Alarm:Indicates a possible disconnection or leak.
- Apnea Alarm:Alerts when no breath is detected for a set time.
- High Respiratory Rate Alarm:Warns of rapid breathing.
- Low Tidal Volume Alarm:Shows inadequate air delivery per breath.
Responding To Alerts
Pause and check the patient immediately after an alarm sounds. Look for signs of distress or discomfort. Inspect the ventilator tubing for disconnections or kinks. Adjust settings only if you are trained and authorized. Always notify medical staff if alarms continue or patient condition worsens.
Quick Tips For Fast Mastery
Mastering ventilator settings quickly requires a focused approach and practical experience. You need clear strategies that help you absorb information fast while avoiding common pitfalls. The tips below will guide you through essential steps to build confidence and skill in reading ventilator settings effectively.
Practice Scenarios
Nothing beats hands-on practice for understanding ventilator settings. Use case studies or simulation software to see how changes impact patient breathing in real time.
Start with simple cases, like adjusting tidal volume or respiratory rate, before moving to complex settings such as pressure control or FiO2. This gradual exposure helps build your intuition.
Ask yourself: How would you adjust the settings if oxygen levels drop? Practicing these scenarios helps you think critically and act quickly in real situations.
Common Mistakes To Avoid
- Ignoring patient response:Ventilator settings are not one-size-fits-all. Always check how the patient is reacting before making changes.
- Overcomplicating adjustments:Keep it simple. Small, incremental changes often work better than drastic shifts.
- Missing alarms:Don’t overlook alarms or warnings. They provide vital clues about patient status and equipment function.
Recognizing these pitfalls early can save time and prevent harm. Have you noticed any mistakes that slowed your learning curve? Reflecting on them sharpens your skills.
Resources For Ongoing Learning
Continuous learning keeps your skills sharp. Use trusted online courses, ventilator manuals, and clinical guidelines to stay updated.
Join forums or social media groups where professionals share tips and real-life experiences. These communities offer valuable insights that textbooks may miss.
Remember, every expert started where you are now. What resource has changed the way you understand ventilator settings? Keep exploring and asking questions.
Frequently Asked Questions
What Are The Basic Ventilator Settings To Understand?
Basic ventilator settings include tidal volume, respiratory rate, FiO2, and PEEP. These control breath size, speed, oxygen level, and airway pressure. Knowing these helps you monitor patient ventilation effectively and adjust settings safely.
How To Interpret Tidal Volume On A Ventilator?
Tidal volume indicates the air amount delivered per breath. It’s usually set based on patient weight to avoid lung injury. Understanding this helps ensure adequate ventilation without overdistension.
What Does Peep Mean In Ventilator Settings?
PEEP stands for Positive End-Expiratory Pressure. It keeps airways open during exhalation, improving oxygenation. Proper PEEP prevents alveolar collapse and enhances lung function.
How To Read Fio2 On A Ventilator?
FiO2 is the fraction of inspired oxygen. It ranges from 21% (room air) to 100%. Adjusting FiO2 controls oxygen delivery to meet patient needs.
Conclusion
Reading ventilator settings helps ensure proper care for patients. Understanding key terms makes it easier to follow and adjust settings. Always check each parameter carefully before making changes. Practice and patience will improve your confidence over time. Stay curious and keep learning to help patients breathe better.
Ventilator knowledge is a valuable skill for healthcare workers and caregivers alike.