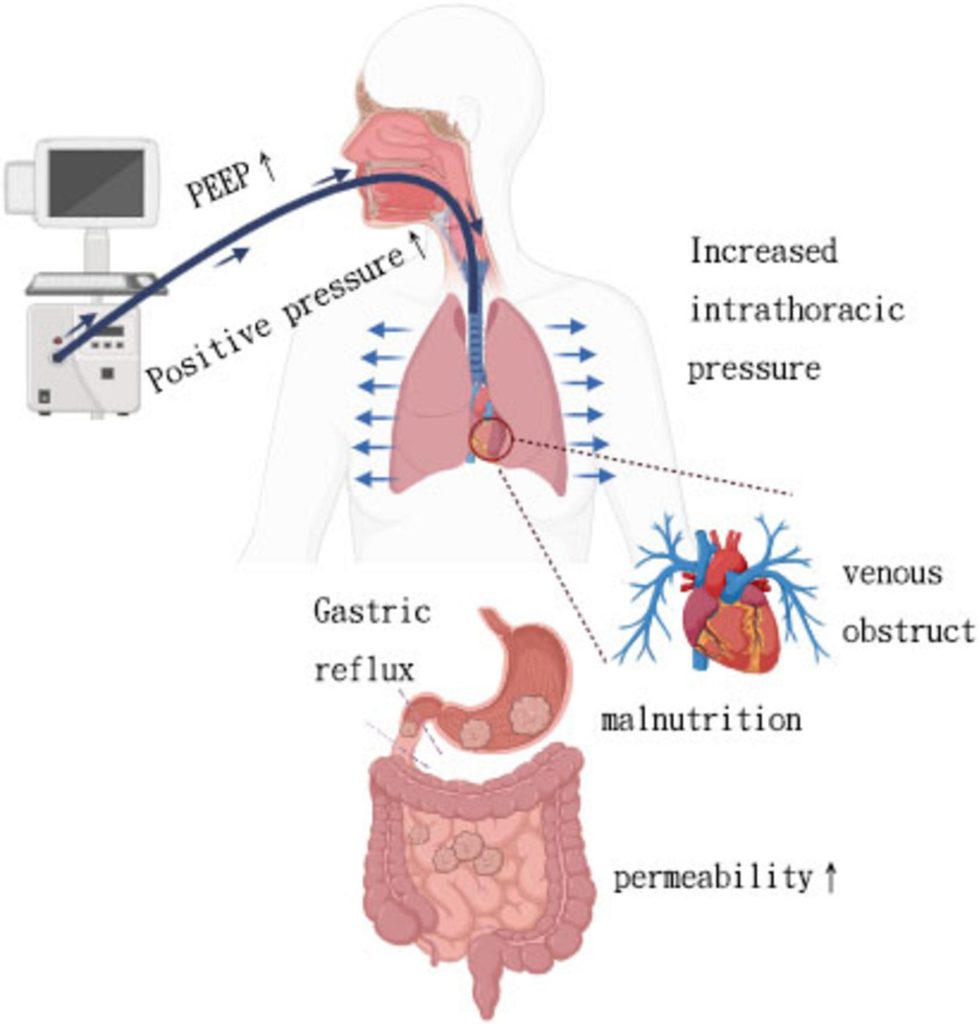
Have you ever wondered why your stomach feels swollen or uncomfortable during ventilation? Gastric distention can be more than just a nuisance—it can affect your breathing and overall comfort.
Understanding the cause of this problem is key to preventing it and ensuring effective ventilation. You’ll discover exactly what leads to gastric distention during ventilation and how it impacts your health. Keep reading to learn the simple facts that could make a big difference for you or someone you care about.
Gastric Distention In Ventilation
Gastric distention during ventilation happens when air enters the stomach instead of the lungs. This can cause discomfort and complications for patients receiving mechanical ventilation or mask ventilation. Understanding the reasons behind this helps healthcare providers prevent and manage the condition effectively.
How Air Enters The Stomach During Ventilation
Air can move into the stomach if the airway is not properly sealed. This often happens with mask ventilation when the mask fit is loose. Excessive pressure during ventilation also forces air past the esophagus into the stomach.
Impact Of Ventilation Techniques On Gastric Distention
Using high ventilation pressures increases the risk of air leaking into the stomach. Rapid or forceful breaths push more air through the esophageal opening. Gentle, controlled ventilation lowers the chance of gastric inflation.
Role Of Patient Factors In Gastric Distention
Patients with weak or relaxed esophageal sphincters are more prone to gastric distention. Conditions like muscle weakness or sedation reduce the ability to keep air out of the stomach. Proper assessment can identify patients at higher risk.
Signs And Symptoms Of Gastric Distention During Ventilation
- Abdominal bloating and discomfort
- Increased stomach size
- Difficulty ventilating the lungs
- Gurgling sounds during ventilation

Credit: quizlet.com
Role Of Airway Pressure
Airway pressure plays a critical role in the development of gastric distention during mechanical ventilation. It controls how much air is pushed into the lungs, but sometimes excess pressure can divert air into the stomach instead. Understanding this balance helps you manage ventilation more safely and avoid complications.
Effects Of High Peak Inspiratory Pressure
High peak inspiratory pressure (PIP) means more force is used to deliver air into the lungs with each breath. If this pressure is too strong, it can cause air to leak into the esophagus and stomach, leading to gastric distention.
Think about how a balloon inflates: too much force can cause unwanted expansion in nearby areas. Similarly, high PIP can push air past the lower esophageal sphincter, filling the stomach with air and causing discomfort or even vomiting.
Have you noticed that adjusting the ventilator settings to lower PIP often reduces abdominal bloating? This simple change can improve patient comfort and reduce risks during ventilation.
Impact Of Positive End-expiratory Pressure
Positive end-expiratory pressure (PEEP) keeps the lungs partially inflated after exhalation, improving oxygenation. However, higher PEEP levels increase baseline airway pressure, which can also contribute to air entering the stomach.
With increased PEEP, the pressure gradient between the airway and esophagus shifts, making it easier for air to pass into the stomach. This risk grows especially if the patient’s esophageal sphincter tone is weak or compromised.
Managing PEEP carefully is essential. You might try lowering PEEP step-by-step to see if it relieves gastric distention without sacrificing oxygen levels. Balancing these pressures can be a game-changer in ventilation management.
Patient-related Factors
Gastric distention during ventilation often puzzles clinicians, but understanding patient-related factors can shed light on why it happens. These factors directly affect how air moves through the body during assisted breathing. By focusing on specific patient characteristics, you can better anticipate and manage this complication.
Esophageal Sphincter Function
The esophageal sphincter acts as a gatekeeper between the throat and the stomach. If it doesn’t close properly, air can slip into the stomach during ventilation. This is common in patients with weakened sphincter muscles due to age, acid reflux, or certain medications.
Imagine providing ventilation to a patient who has chronic acid reflux; their sphincter might already be compromised. This increases the risk that air will travel down the esophagus instead of the lungs, causing gastric distention. Have you noticed how some patients tend to bloat more easily during ventilation? This might be why.
Airway Anatomy Variations
Not all patients have the same airway structure, and these differences can influence ventilation outcomes. Variations like a shorter neck, enlarged tongue, or abnormal airway shape can make it harder to direct air exclusively into the lungs.
In some cases, these anatomical quirks force air into the stomach, especially if the airway is partially blocked. Knowing your patient’s airway anatomy beforehand can help you adjust your ventilation technique to reduce gastric distention risk. Could paying closer attention to these physical traits change your approach?
Ventilation Techniques
Gastric distention during ventilation happens when air enters the stomach instead of the lungs. This often occurs due to improper airway placement or excessive ventilation pressure. Managing ventilation carefully helps reduce this risk.
Understanding the nuances of ventilation techniques is crucial when tackling the issue of gastric distention during ventilation. Each method has its own impact on the patient’s body, and knowing which technique to apply can make a significant difference. Proper ventilation not only ensures adequate oxygenation but also minimizes the risk of unwanted complications like gastric distention.Bag-valve-mask Ventilation
Bag-valve-mask (BVM) ventilation is a common technique used in emergency settings. It requires precision and care to prevent excessive air from entering the stomach. When applying BVM, ensure the mask fits snugly over the patient’s face to create an airtight seal. Deliver breaths slowly and steadily. Rapid or forceful ventilation can increase the risk of air entering the stomach, leading to distention. Have you ever experienced the difficulty of balancing speed and pressure? It’s a delicate art that requires practice and attention.Mechanical Ventilation Settings
Mechanical ventilation offers more controlled settings, which can be adjusted to minimize gastric distention. Set the tidal volume appropriately to ensure adequate lung expansion without pushing excess air into the stomach. Monitoring pressure settings is equally important. High pressure can force air down the esophagus, especially if the lower esophageal sphincter is compromised. Regularly check ventilator settings and patient response. Are you confident in adjusting settings in real-time to match the patient’s needs? It’s vital to adapt quickly to changing situations to prevent complications.Equipment And Circuit Issues
Gastric distention during ventilation often traces back to issues with the equipment and circuit. Even small faults can cause air to enter the stomach instead of the lungs, leading to discomfort and complications. Understanding these equipment-related causes helps you prevent and quickly address the problem.
Mask Fit And Seal
A poor mask fit is one of the most common reasons for gastric distention. If the mask does not seal properly around the face, air escapes and may enter the esophagus instead of the airway.
Check the mask size and adjust straps to ensure a snug fit without causing discomfort. Pay special attention when working with patients who have facial hair or irregular facial shapes, as these factors can make achieving a proper seal tricky.
Have you noticed how even slight leaks can increase the risk of air swallowing? That’s why continuous monitoring and adjusting the mask are vital during ventilation.
Use Of Nasogastric Tubes
Nasogastric tubes can sometimes contribute to gastric distention if not managed correctly. While they help decompress the stomach, improper positioning or blockage can trap air inside.
Ensure the tube is correctly placed and functioning before ventilation begins. Regularly check for kinks or obstructions that might prevent the tube from releasing air or gastric contents.
Think about how you can integrate routine tube checks into your ventilation protocol to catch problems early. Small steps like this can significantly reduce gastric distention risks.

Credit: studyx.ai
Consequences Of Gastric Distention
Gastric distention during ventilation can lead to several serious problems. The stomach fills with air, causing it to expand. This expansion affects nearby organs and body functions. Understanding the consequences helps in managing ventilation safely and effectively.
Respiratory Complications
The swollen stomach pushes against the diaphragm. This pressure reduces lung space, making breathing harder. It lowers lung volume and oxygen exchange. Breathing becomes less efficient and more difficult. This can cause low oxygen levels in the blood. Patients may struggle to get enough air.
Risk Of Aspiration
Air-filled stomach increases pressure on the lower esophagus. This pressure can push stomach contents upward. Vomiting or regurgitation may occur during ventilation. Stomach fluids can enter the lungs. This leads to aspiration pneumonia, a serious lung infection. Aspiration causes coughing, choking, and breathing problems.
Preventive Strategies
Preventing gastric distention during ventilation requires careful attention to how air is delivered and monitored. Small changes in technique can make a big difference in patient comfort and safety. Understanding practical ways to avoid this complication helps you provide better care and avoid unnecessary risks.
Proper Ventilation Techniques
Using the right ventilation method is key to reducing the chance of air entering the stomach. Always aim to deliver the minimum effective tidal volume and avoid excessive pressure. Gentle, controlled breaths prevent pushing air into the esophagus, which often leads to gastric distention.
Consider using a bag-valve mask with a pressure relief valve to avoid over-inflation. Positioning the patient correctly can also help; slightly elevating the head may reduce the risk of air swallowing. These small adjustments can change outcomes significantly.
Monitoring And Adjustments
Continuous monitoring during ventilation lets you catch early signs of gastric distention. Watch for abdominal swelling or increased resistance during ventilation. If you notice these, adjust the ventilation parameters immediately.
Using capnography and pulse oximetry provides real-time feedback on ventilation effectiveness. If the stomach is filling with air, you might see changes in these readings. Promptly lowering ventilation pressures or volumes can prevent worsening distention.

Credit: www.jacc.org
Frequently Asked Questions
What Causes Gastric Distention During Mechanical Ventilation?
Gastric distention occurs when air unintentionally enters the stomach during ventilation. This happens due to improper airway management, high ventilation pressures, or mask leaks. Excess air inflates the stomach, risking discomfort and complications like aspiration.
How Does Mask Ventilation Lead To Gastric Distention?
Mask ventilation can cause air to enter the esophagus if the mask seal is poor. Excess pressure forces air into the stomach instead of the lungs, leading to gastric distention.
Can High Ventilation Pressure Increase Gastric Distention Risk?
Yes, high ventilation pressures can push air past the lower esophageal sphincter into the stomach. This increases the risk of gastric distention during ventilation.
How Can Gastric Distention Be Prevented During Ventilation?
Proper airway techniques, using appropriate ventilation pressures, and ensuring a good mask seal help prevent air from entering the stomach and reduce gastric distention risk.
Conclusion
Gastric distention during ventilation happens when air enters the stomach. This can cause discomfort and breathing problems. It often results from high ventilation pressure or improper tube placement. Understanding these causes helps reduce risks. Proper techniques and careful monitoring are key.
Always watch for signs to act quickly. Preventing gastric distention improves patient safety and care. Stay aware and keep ventilation safe.