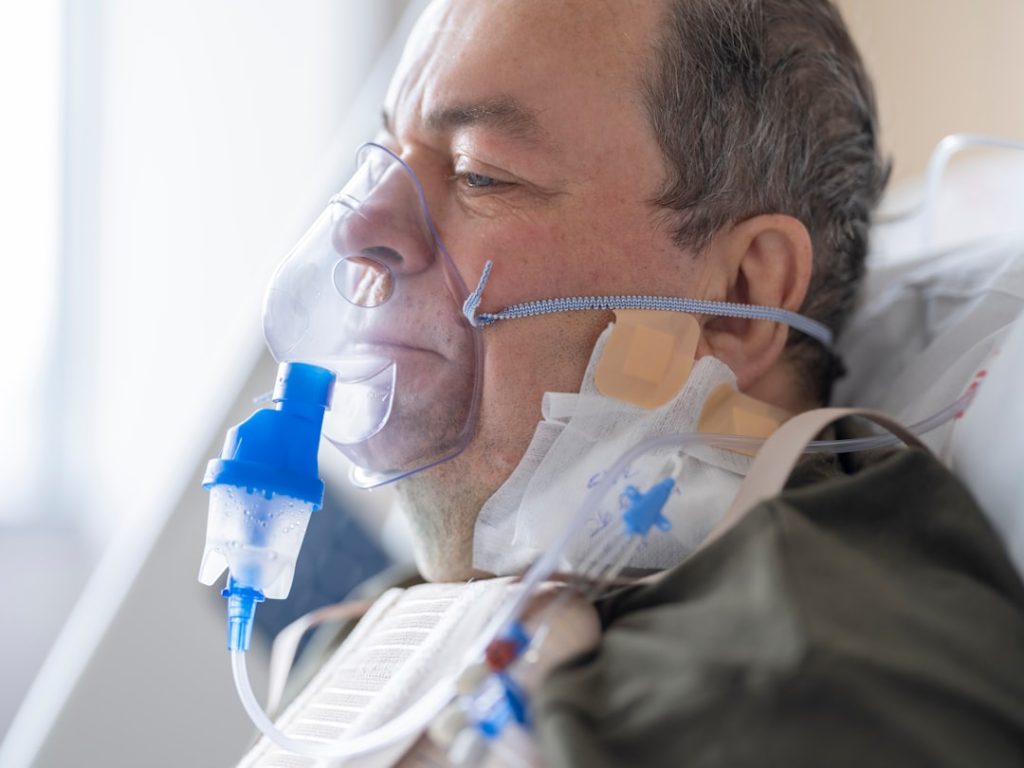
If you care for someone on a ventilator or work in healthcare, preventing ventilator-acquired pneumonia (VAP) is crucial. This serious infection can make recovery longer and harder.
But here’s the good news: there are simple, proven steps you can take to lower the risk. You’ll discover practical tips that protect your loved one or patients from VAP. Keep reading to learn how small actions can make a big difference in keeping lungs healthy and speeding up recovery.
Your attention now could save lives later.

Credit: www.liebertpub.com
Causes Of Ventilator Acquired Pneumonia
Ventilator Acquired Pneumonia (VAP) develops in patients using mechanical ventilators. Understanding its causes is vital to prevent it. VAP occurs when harmful germs enter the lungs through the breathing tube. Several factors increase the risk of infection.
The breathing tube bypasses natural defenses in the throat and airway. This allows bacteria to reach the lungs more easily. Poor oral hygiene and contaminated equipment can also introduce germs. The patient’s weakened immune system plays a role too.
Microbial Colonization Of The Endotracheal Tube
Bacteria can attach and grow on the surface of the breathing tube. This creates a biofilm that protects germs from the immune system. The biofilm can release bacteria into the lungs, causing infection.
Aspiration Of Secretions
Secretions from the mouth or stomach can leak into the lungs. This often happens around the cuff of the breathing tube. Aspiration carries bacteria directly into the lower respiratory tract.
Impaired Host Defenses
Patients on ventilators often have weakened immune responses. Illness, sedation, or poor nutrition reduce the body’s ability to fight infection. This makes it easier for bacteria to cause pneumonia.
Contaminated Equipment And Environment
Non-sterile ventilator parts or poor hygiene increase infection risk. Healthcare workers can transfer germs if hand hygiene is not followed. The hospital environment may harbor resistant bacteria.
Risk Factors To Watch
Ventilator Acquired Pneumonia (VAP) is a serious risk for patients on mechanical ventilation. Understanding the risk factors helps in preventing this infection. Some patients face higher risks due to their health conditions or treatment methods.
Identifying these risks early allows healthcare providers to take extra precautions. This section highlights key risk factors to watch closely.
Prolonged Ventilation Duration
Longer use of a ventilator raises the chance of infection. Bacteria can build up over time in the breathing tubes. The risk grows significantly after 48 hours of ventilation.
Patient Age And Health Status
Older adults and those with weak immune systems have higher risks. Chronic illnesses like diabetes or lung disease increase vulnerability. Poor nutrition and general weakness also contribute.
Improper Oral Care
Poor mouth hygiene allows harmful bacteria to grow. These bacteria can enter the lungs through the ventilator. Regular oral cleaning helps reduce this risk.
Use Of Sedatives And Muscle Relaxants
Drugs that reduce consciousness or muscle movement affect natural cough reflexes. This allows secretions to collect in the lungs. It creates a breeding ground for bacteria.
Contaminated Ventilator Equipment
Unclean ventilator parts or humidifiers carry germs. These germs can enter the lungs directly. Strict sterilization is essential to prevent contamination.
Hygiene Practices For Prevention
Practicing good hygiene is key in preventing ventilator-acquired pneumonia. Regular hand washing and disinfecting surfaces reduce infection risks. Elevating the head of the bed and ensuring oral care can also help.
Hygiene Practices for Prevention Preventing ventilator-acquired pneumonia (VAP) is a critical concern in healthcare settings. Adhering to strict hygiene practices can significantly reduce the risk of this serious condition. Implementing effective hygiene protocols not only safeguards patients but also enhances the overall care quality.Hand Hygiene Protocols
Proper hand hygiene is the first line of defense against infections. Ensure you wash your hands thoroughly with soap and water before and after patient contact. Use alcohol-based hand sanitizers when soap and water aren’t available. Healthcare workers should be mindful of the areas often missed, such as the backs of hands and between fingers. Consistency in these practices can drastically lower infection rates. Have you checked if your facility has enough hand sanitizer stations?Oral Care Techniques
Oral care is a vital, yet sometimes overlooked, part of preventing VAP. Regular brushing of the patient’s teeth and gums can reduce harmful bacteria. Use antiseptic mouthwash to further decrease bacterial load in the mouth. Swabbing the mouth with a cleaning solution is crucial if brushing isn’t possible. How often are you performing oral care for ventilated patients? Increasing frequency can make a big difference.Cleaning Ventilator Equipment
Ensuring ventilator equipment is clean is non-negotiable. Disassemble and clean each component following the manufacturer’s guidelines. Use disinfectants that are effective against the pathogens commonly found in healthcare settings. Regularly inspect and replace ventilator filters and tubing. Are there scheduled checks in your routine to ensure equipment cleanliness? A small oversight can lead to significant consequences. Adopting these hygiene practices is essential for preventing VAP. Each step you take towards maintaining a clean environment contributes to safer patient care. Are you ready to implement these practices consistently?Patient Positioning Strategies
Patient positioning plays a crucial role in preventing ventilator acquired pneumonia (VAP). Proper positioning helps reduce the risk of aspiration, which is a common cause of pneumonia in ventilated patients. Small changes in how the patient is positioned can make a big difference in outcomes.
Elevating The Head Of Bed
Raising the head of the bed to an angle between 30 to 45 degrees is a simple yet effective strategy. This position helps prevent stomach contents from flowing back into the lungs, lowering the chance of infection. Nurses and caregivers should regularly check and maintain this elevation to ensure consistency.
Think about a patient lying flat after a heavy meal. Gravity is not on their side, increasing the risk of aspiration. Elevation acts like a natural barrier, keeping the airway safer.
Avoiding Supine Position
Lying flat on the back (supine position) increases the risk of secretions pooling near the airway. This can create a breeding ground for bacteria and lead to pneumonia. Encouraging side-lying or semi-recumbent positions can reduce this risk significantly.
Have you ever noticed how uncomfortable it feels to lie completely flat after eating? Patients feel the same, and their lungs are more vulnerable. Changing their position regularly not only improves comfort but also helps clear secretions effectively.
Ventilator Management Tips
Effective ventilator management plays a crucial role in preventing ventilator-acquired pneumonia (VAP). By paying close attention to how ventilation is controlled and adjusted, you can significantly lower the risk of infection. Small changes in your approach can make a big difference in patient outcomes.
Minimizing Ventilation Duration
Keeping the time a patient spends on a ventilator as short as possible reduces the chance of bacteria building up in the lungs. You should regularly assess whether the patient still needs mechanical support and try to start weaning as soon as it’s safe.
Daily spontaneous breathing trials can help determine if a patient is ready to breathe on their own. Have you considered how often ventilator assessments are done in your care routine? Shorter ventilation times often lead to fewer complications.
Using Appropriate Ventilator Settings
Setting the ventilator correctly avoids unnecessary lung injury and helps maintain good airway hygiene. Use lower tidal volumes and appropriate positive end-expiratory pressure (PEEP) to protect the lungs.
Adjusting oxygen levels to the minimum required can prevent damage from excessive oxygen. Have you checked if your ventilator settings are tailored to each patient’s lung condition? Fine-tuning these parameters can prevent inflammation and reduce infection risk.
Medication And Antibiotic Use
Medication and antibiotics play a vital role in preventing ventilator-acquired pneumonia (VAP). Proper use of these drugs helps reduce infection risks and improve patient outcomes. Careful management of medication ensures that treatments support healing without causing harm or resistance.
Role Of Prophylactic Antibiotics
Prophylactic antibiotics are given to stop infections before they start. They target bacteria that might enter the lungs through the ventilator. Using these antibiotics wisely can lower pneumonia rates in ventilated patients.
Doctors choose antibiotics based on the patient’s health and local bacteria types. Overuse or misuse can lead to resistant bacteria, making infections harder to treat. Monitoring and adjusting antibiotic use is essential to keep patients safe.
Managing Sedatives And Other Drugs
Sedatives and other medications affect breathing and immune response. Too much sedation can weaken lung defense and increase pneumonia risk. Careful dosing helps maintain patient comfort and reduces infection chances.
Regular review of all drugs given to ventilated patients is important. This prevents side effects that may harm lung function. Balancing medication supports recovery and prevents ventilator-acquired pneumonia effectively.
Staff Training And Protocols
Preventing ventilator-acquired pneumonia (VAP) relies heavily on the competence and vigilance of healthcare staff. Proper training and strict adherence to protocols create a frontline defense against infections. When every team member understands their role and follows the rules, patient safety improves dramatically.
Regular Training Sessions
Regular training keeps staff updated on the latest VAP prevention techniques. It also reinforces critical habits like hand hygiene and equipment sterilization. Training sessions can include simulations, quizzes, and case reviews to make learning interactive and memorable.
Have you noticed how quickly skills can fade without practice? Frequent refreshers help keep knowledge sharp and make sure no one skips essential steps during patient care.
- Schedule monthly or quarterly training updates
- Use real-life scenarios to highlight risks and solutions
- Encourage staff to share experiences and ask questions
Adhering To Clinical Guidelines
Clinical guidelines offer a clear roadmap for preventing VAP. These protocols cover everything from patient positioning to ventilator circuit care. Following them reduces variability in care and ensures everyone acts consistently.
Imagine the chaos if each nurse or doctor had a different approach. Guidelines unify practices, making prevention more reliable and measurable.
| Guideline | Key Action | Impact on VAP Prevention |
|---|---|---|
| Head-of-Bed Elevation | Keep patient’s head elevated at 30-45° | Reduces aspiration risk |
| Oral Care Protocol | Regular oral hygiene with antiseptics | Limits bacterial colonization |
| Ventilator Circuit Management | Change circuits only when visibly soiled | Prevents unnecessary contamination |
Do you think your team’s current practices align with these guidelines? Regular audits and feedback help ensure compliance and highlight areas for improvement.

Credit: www.vhtc.org
Monitoring And Early Detection
Monitoring and early detection play a key role in preventing ventilator-acquired pneumonia (VAP). Careful observation helps catch signs of infection before it worsens. Early action can reduce complications and improve patient outcomes. Constant vigilance by healthcare staff ensures timely intervention and treatment.
Recognizing Symptoms Early
Identifying early symptoms of VAP is vital. Watch for signs like:
- Fever or chills
- Increased mucus or pus in the airway
- Changes in breathing patterns
- Lower oxygen levels
- New or worsening cough
Regular checks of vital signs and lung sounds help detect problems fast. Prompt reporting of any changes allows quick response and care.
Routine Microbiological Surveillance
Routine microbiological tests detect infections early. Samples from the respiratory tract can identify harmful bacteria. This helps guide targeted antibiotic treatment.
Surveillance includes:
- Periodic cultures of tracheal secretions
- Monitoring bacterial growth patterns
- Tracking antibiotic resistance trends
Early identification of pathogens limits infection spread. It supports effective treatment choices and better patient recovery.
Credit: vcu.mediaspace.kaltura.com
Frequently Asked Questions
What Are Common Causes Of Ventilator Acquired Pneumonia?
Ventilator acquired pneumonia (VAP) is mainly caused by bacteria entering the lungs via the ventilator tube. Poor hygiene and prolonged ventilation increase risk. Contaminated equipment and impaired immunity also contribute to VAP development.
How Can Oral Care Prevent Ventilator Acquired Pneumonia?
Regular oral care reduces bacteria in the mouth, lowering infection risk. Cleaning teeth and gums helps remove harmful microbes that can reach the lungs through the ventilator. Consistent oral hygiene is crucial for VAP prevention.
Why Is Head Elevation Important In Preventing Vap?
Elevating the patient’s head to 30-45 degrees helps prevent aspiration of secretions into the lungs. This position reduces bacterial entry via the ventilator tube, significantly lowering the chances of developing pneumonia.
How Does Hand Hygiene Reduce Ventilator Acquired Pneumonia?
Proper hand hygiene by healthcare workers prevents the transfer of bacteria to the ventilator or patient. Washing hands before and after patient care is a simple, effective step to control VAP infections.
Conclusion
Preventing ventilator-acquired pneumonia saves lives and reduces hospital stays. Clean equipment and hand hygiene play a big role. Nurses and doctors must follow safety steps every time. Early mouth care and proper patient positioning help too. Families can support by asking questions and staying informed.
Small actions make a big difference in care quality. Keep these tips in mind to protect patients from infection. Simple steps can lead to safer, healthier recovery journeys.