Have you ever wondered how long someone can be sedated while on a ventilator? If you or a loved one is facing this situation, it’s natural to have questions and concerns.
Understanding the time frame and what it means for recovery can help you feel more in control during a difficult time. You’ll discover the key facts about sedation on a ventilator, why it’s needed, and what factors affect how long it can safely last.
Keep reading to get clear answers that matter to you.
Sedation Basics On Ventilators
Understanding sedation basics on ventilators is crucial if you or a loved one faces this situation. Sedation helps manage discomfort and anxiety while ensuring the ventilator can do its job effectively. But how does sedation work, and what medications are commonly used? Let’s break it down.
Purpose Of Sedation
Sedation on a ventilator primarily aims to keep you calm and pain-free. It prevents you from fighting against the breathing machine, which can cause complications. Additionally, sedation helps reduce oxygen demand by relaxing your muscles and lowering stress levels.
Have you ever wondered why some patients stay sedated for days or even weeks? The answer lies in balancing comfort with safety. Too little sedation can cause distress, while too much might prolong recovery or cause side effects.
Common Sedative Medications
Doctors select sedatives based on your condition and how long you need ventilation. Here are some frequently used medications:
- Propofol:Acts quickly and wears off fast, making it easy to adjust doses.
- Midazolam:A benzodiazepine that calms anxiety and induces sleep.
- Fentanyl:A strong painkiller often combined with sedatives to control pain.
- Dexmedetomidine:Provides sedation without heavy respiratory depression, useful for lighter sedation.
Each medication has pros and cons, and your care team will monitor you closely to find the right balance. Have you ever experienced unexpected effects from medication? That’s why personalized care is key during sedation.
Duration Factors
Understanding the factors that influence how long someone can be sedated on a ventilator is crucial. The duration varies widely depending on several key elements. Knowing these can help you better grasp the complexity behind sedation timelines and what to expect in different situations.
Patient Condition
The overall health and underlying illnesses of the patient play a major role in sedation duration. Someone with severe respiratory issues or multiple organ failures may need longer sedation to stabilize. On the other hand, healthier patients might only require sedation for a short period.
Age, immune system strength, and response to medications also affect how long sedation is necessary. Have you noticed how some patients recover faster despite similar conditions? This highlights how individual differences matter a lot.
Type Of Procedure
The kind of medical procedure or surgery directly impacts sedation length. Minor surgeries often need brief sedation, sometimes just a few hours. More complex or emergency operations may require prolonged sedation to ensure patient safety.
For example, a lung transplant patient typically stays sedated longer than someone undergoing a routine appendectomy. This is because the body needs more time to heal and adjust. Thinking about your own medical history, how did different procedures affect your recovery time?
Sedation Depth
The depth or level of sedation influences how long a person remains on a ventilator. Light sedation allows quicker waking and shorter ventilation periods. Deep sedation, however, is sometimes necessary for critical patients, extending the time they are sedated.
Doctors carefully balance sedation depth to avoid complications like delirium or muscle weakness. They adjust medication doses based on how the patient responds. Have you ever wondered why sedation feels different for each person? This is why the depth and management of sedation matter so much.
Short-term Vs Long-term Sedation
Sedation helps patients on ventilators stay calm and comfortable. Doctors decide sedation length based on patient needs. Sedation can be short-term or long-term. Each type has different uses and effects. Understanding these differences is important for patients and families.
Typical Timeframes
Short-term sedation usually lasts a few hours to a few days. It is common after surgery or during acute illness. Long-term sedation can last weeks or even months. This happens in severe cases needing extended ventilation support.
Doctors carefully monitor sedation time. They adjust doses to avoid complications. The goal is to balance comfort and safety.
Risks Of Prolonged Sedation
Long-term sedation carries more risks than short-term use. Patients may develop muscle weakness or nerve damage. Breathing muscles can weaken, making weaning from ventilators hard.
Other risks include infections, blood clots, and delirium. The brain might also be affected, causing confusion or memory problems. Medical teams watch closely to reduce these risks.

Credit: www.goodrx.com
Monitoring During Sedation
Monitoring during sedation is crucial when someone is on a ventilator. It ensures their safety and helps healthcare providers adjust medications and ventilation settings effectively. Keeping a close eye on the patient can prevent complications and improve recovery outcomes.
Vital Signs Tracking
Tracking vital signs is a constant process while a patient remains sedated on a ventilator. This includes measuring heart rate, blood pressure, oxygen saturation, and respiratory rate. Sudden changes in these numbers can signal distress or inadequate sedation, prompting immediate action.
Continuous monitoring allows for quick responses. For example, if oxygen levels drop, the medical team can adjust ventilator settings or oxygen delivery right away. Have you ever wondered how a slight change in blood pressure might indicate a bigger problem during sedation?
Neurological Assessments
Even under sedation, checking neurological status matters. Nurses and doctors assess pupil response, reflexes, and sometimes use sedation scales to gauge brain activity. This helps identify if sedation is too deep or too light, which can affect breathing and recovery.
Regular neurological checks provide insight beyond vital signs alone. They can reveal subtle changes in brain function that might otherwise go unnoticed. How often do you think such assessments are performed to keep patients safe?
Complications And Risks
Complications and Risks Sedation on a ventilator can lead to infections or lung damage. Prolonged sedation increases risks like blood clots and weakened muscles. Monitoring is crucial to manage these potential complications effectively.
Sedation is often necessary for patients on ventilators, but it comes with its own set of complications and risks. Understanding these can help you make informed decisions and ask the right questions. Let’s explore some of the challenges associated with prolonged sedation.Respiratory Issues
Prolonged sedation can lead to respiratory complications. When sedated, patients may have a reduced ability to cough and clear their airways. This can increase the risk of fluid buildup and infections. Moreover, the muscles involved in breathing can weaken over time. This weakness can make it difficult to wean the patient off the ventilator.Delirium And Cognitive Effects
Sedation can impact brain function. Patients may experience delirium, a state of confusion and disorientation. Cognitive effects can linger even after sedation is reduced. This might include memory issues or difficulty concentrating, affecting recovery and quality of life.Infections And Other Concerns
Sedation can increase the risk of infections, particularly pneumonia. The use of a ventilator itself is a factor, but sedation may compound this risk. Other concerns include pressure sores and blood clots. These occur from prolonged immobility, emphasizing the need for careful monitoring and care strategies. Have you considered discussing these risks with your healthcare provider? Their insights can be invaluable in navigating the complexities of sedation and ventilation.
Credit: medium.com
Weaning Off Sedation
Weaning off sedation is a critical phase for anyone who has been sedated on a ventilator. It requires careful monitoring and adjustments to ensure the patient wakes up safely and comfortably. You might wonder how doctors decide the right moment to start this process and how they keep it safe. Understanding these details can help you feel more confident if you or a loved one faces this situation.
Criteria For Reducing Sedation
Doctors look for several signs before reducing sedation. The patient’s vital signs, like heart rate and breathing, need to be stable. They also check if the underlying illness is improving and if the patient can start breathing more on their own.
Another important factor is the patient’s neurological status. Are they responsive to simple commands? Can they move their limbs or open their eyes? These clues help determine readiness for less sedation.
Have you ever noticed how small improvements can signal big progress? In this case, even tiny changes in alertness or breathing effort make a big difference.
Strategies For Safe Weaning
Reducing sedation is done gradually to avoid discomfort or complications. Doctors often lower the sedative dose in small steps, watching the patient closely after each change. This slow approach helps prevent agitation or sudden breathing difficulties.
- Daily sedation vacations: temporarily stopping sedatives to assess how the patient responds.
- Using sedation scales: tools that measure sedation depth to guide dose adjustments.
- Combining medications: sometimes switching to shorter-acting drugs makes weaning easier.
One nurse shared how a patient’s mood changed during sedation breaks, becoming more alert and cooperative. This real-time feedback is crucial for tailoring the weaning plan.
What questions would you ask if you were in the patient’s shoes during this process? Understanding the why and how can help you stay calm and informed.
Role Of Multidisciplinary Team
The care of someone sedated on a ventilator is complex and demands more than just one skill set. A multidisciplinary team plays a crucial role in managing sedation safely and effectively. Each professional brings unique expertise to monitor, adjust, and support the patient’s condition over time.
Doctors And Nurses
Doctors make key decisions about the level and duration of sedation based on the patient’s medical condition. They regularly assess sedation depth to avoid both under- and over-sedation, which can have serious consequences.
Nurses are the eyes and ears at the bedside. They continuously monitor vital signs and sedation levels, adjusting care as needed. Their close observation helps catch early signs of complications like delirium or breathing difficulties.
Respiratory Therapists
Respiratory therapists manage the ventilator settings to ensure proper breathing support while minimizing lung injury. They work closely with doctors to balance ventilation needs with sedation, optimizing comfort and safety.
These specialists also teach patients and families about the ventilator process, easing anxiety and improving cooperation. Have you ever thought about how much breathing support can affect sedation choices?
Pharmacists
Pharmacists play a vital role in selecting and dosing sedative medications. They consider drug interactions, patient kidney and liver function, and sedation goals to personalize therapy.
Their input helps prevent adverse effects and ensures sedation is effective but reversible. You might be surprised how subtle medication adjustments can change sedation outcomes significantly.
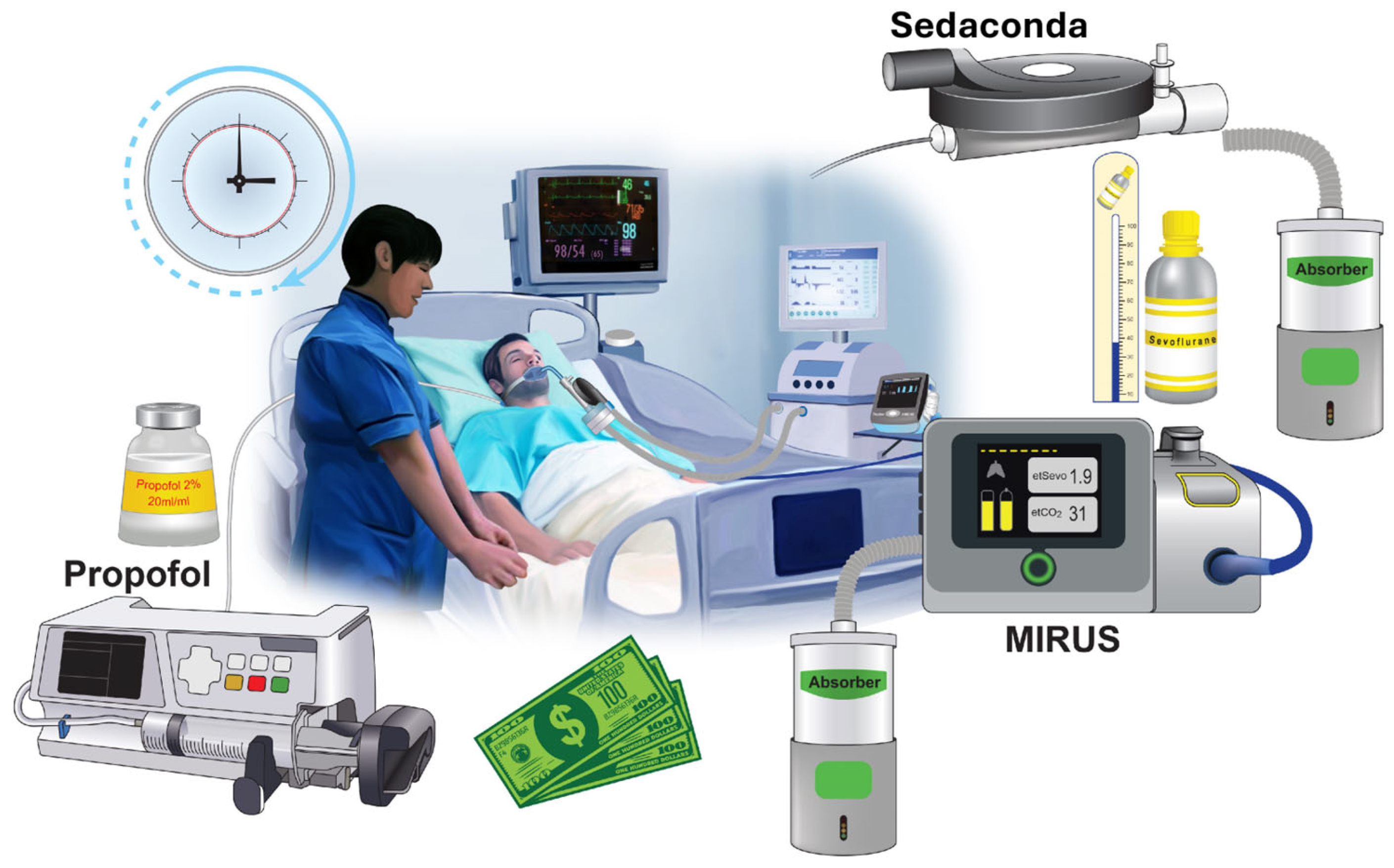
Credit: www.mdpi.com
Frequently Asked Questions
How Long Can Sedation Last On A Ventilator?
Sedation duration on a ventilator varies from days to weeks. It depends on the patient’s condition and response to treatment. Doctors carefully monitor sedation levels to balance comfort and safety. Prolonged sedation requires regular assessment to prevent complications.
What Factors Affect Sedation Duration On Ventilators?
Sedation time depends on illness severity, patient age, and organ function. Medication type and dosage also influence sedation length. Patient response and need for mechanical ventilation play crucial roles in determining sedation duration.
Is Long-term Sedation On A Ventilator Safe?
Long-term sedation can be safe with proper medical supervision. Risks include muscle weakness, infections, and delirium. Healthcare teams regularly assess sedation depth and adjust medications to minimize side effects and promote recovery.
Can Sedation Be Stopped Abruptly On A Ventilator?
Sedation is usually tapered gradually to avoid withdrawal symptoms. Abrupt stopping can cause agitation, anxiety, or respiratory distress. Doctors follow protocols to safely reduce sedation as the patient’s condition improves.
Conclusion
Sedation length on a ventilator varies per patient need. Doctors watch closely to keep patients safe. Long sedation can cause side effects or complications. Care teams adjust medicine to balance comfort and health. Families should ask questions and stay informed.
Understanding sedation helps ease worry during tough times. Each case is unique, so decisions depend on many factors. Trust healthcare providers to make the best choices. Clear communication remains key throughout the treatment process.





