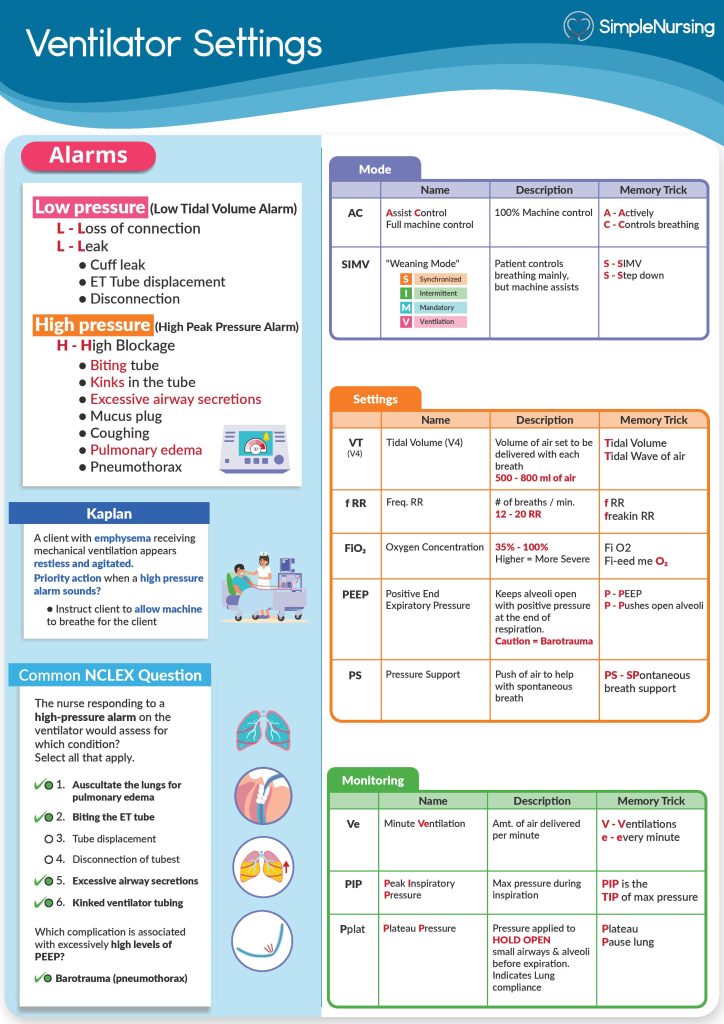
Are you wondering why your ventilator might be delivering a high tidal volume? Understanding what causes this can be crucial for ensuring the safety and comfort of patients relying on mechanical breathing support.
High tidal volume can lead to serious complications, but knowing the reasons behind it helps you take control and make informed decisions. You’ll discover the common factors that cause high tidal volume on a ventilator and how to address them effectively.
Keep reading to protect your patients and improve ventilator care.
Basics Of Tidal Volume
Understanding the basics of tidal volume is key to grasping what causes high tidal volume on a ventilator. Tidal volume refers to the amount of air delivered to the lungs with each breath during mechanical ventilation. Knowing how it works helps you recognize when adjustments are necessary and why they matter for patient care.
Definition And Importance
Tidal volume is the volume of air moved in or out of the lungs during a normal breath. On a ventilator, it’s the set amount of air given to the patient with each mechanical breath. This value is crucial because it affects oxygen delivery and lung protection.
Too low tidal volume may lead to inadequate oxygenation, while too high can cause lung injury. Have you ever wondered how balancing this volume impacts recovery speed? Getting tidal volume right helps prevent complications like barotrauma or volutrauma, which result from excessive lung stretch.
Normal Tidal Volume Ranges
Typical tidal volumes range from 6 to 8 milliliters per kilogram of ideal body weight. For example, a 70 kg adult usually receives between 420 to 560 milliliters per breath. This range aims to provide enough air without overdistending the lungs.
In some cases, such as acute respiratory distress syndrome (ARDS), clinicians may choose lower tidal volumes around 4 to 6 ml/kg to minimize lung injury. Are you aware that even small changes in tidal volume can significantly affect a patient’s lung mechanics? It’s important to tailor these settings based on individual patient needs and clinical condition.

Credit: www.liebertpub.com
Ventilator Settings Influencing Tidal Volume
Ventilator settings play a key role in controlling tidal volume. Adjusting these settings can increase or decrease the volume of air delivered to the lungs. Understanding how these settings influence tidal volume helps in managing patient care effectively.
Set Tidal Volume Parameters
The tidal volume parameter sets the target volume of air per breath. This is usually measured in milliliters or milliliters per kilogram of body weight. Setting a higher tidal volume directly causes the ventilator to deliver more air with each breath. It is crucial to balance this setting to avoid lung injury or inadequate ventilation.
Clinicians often adjust tidal volume based on patient needs, lung compliance, and disease state. Accurate settings help ensure proper oxygenation and carbon dioxide removal.
Impact Of Pressure And Flow Settings
Pressure settings affect the force used to deliver air into the lungs. Higher inspiratory pressures can increase tidal volume if lung compliance allows. Low compliance or stiff lungs can limit volume despite pressure changes.
Flow rate controls how fast air is delivered during inspiration. Faster flow can increase tidal volume by filling the lungs more quickly. Slower flow rates may reduce volume, especially if the breath cycle is short.
Adjusting pressure and flow together helps optimize tidal volume and patient comfort. Careful monitoring is essential to avoid volutrauma or barotrauma from excessive pressures or volumes.
Patient-related Factors
Patient-related factors play a major role in causing high tidal volume on a ventilator. These factors affect how air moves in and out of the lungs during mechanical ventilation. Understanding these elements helps manage ventilation settings better and protect the patient’s lungs.
Changes in the patient’s lung condition can alter how much air the lungs accept with each breath. Variations in airway resistance and the patient’s own breathing effort also impact tidal volume. These factors often interact, making ventilation management complex.
Lung Compliance Changes
Lung compliance is the ability of the lungs to stretch and expand. High lung compliance means the lungs fill easily with air. When compliance increases, the ventilator may deliver a larger tidal volume than expected.
Conditions like emphysema or recovery from lung stiffness can increase compliance. On the other hand, low compliance makes lungs stiff, reducing tidal volume. Changes in compliance need close monitoring to adjust ventilator settings safely.
Airway Resistance Variations
Airway resistance is the opposition to airflow in the respiratory tract. Higher resistance means harder airflow through the airways. If resistance decreases, the ventilator can push more air, raising tidal volume.
Factors like bronchospasm, mucus buildup, or tube obstruction increase airway resistance. Clearing these blockages or reducing spasms helps normalize tidal volume. Resistance changes can happen quickly and affect ventilation immediately.
Patient Effort And Spontaneous Breathing
Patients on ventilators may still try to breathe on their own. Their effort to inhale can add to the ventilator’s push, increasing tidal volume. Strong spontaneous breaths can lead to high tidal volume.
Awake or lightly sedated patients often show more breathing effort. Monitoring patient effort helps avoid lung overdistension. Adjusting sedation or ventilator support can balance patient effort and tidal volume.
Equipment And Circuit Issues
Equipment and circuit problems can cause high tidal volume on a ventilator. These issues affect how air is delivered and measured. Faulty parts or poor setup can lead to incorrect volumes. Checking the equipment thoroughly helps find and fix these problems quickly.
Leaks And Malfunctions
Leaks in the ventilator circuit cause inaccurate tidal volume delivery. Air escapes before reaching the patient, so the machine may increase volume to compensate. This can result in unexpectedly high tidal volumes. Malfunctions like broken valves or loose connections also disrupt airflow. Regular inspection of tubes and connectors prevents leaks and ensures proper ventilation.
Sensor Calibration Errors
Ventilators rely on sensors to measure tidal volume accurately. Calibration errors cause false readings and improper volume settings. Sensors may drift over time or after maintenance. Incorrect calibration leads to overestimation of tidal volume. Routine sensor checks and recalibration keep measurements accurate and prevent high tidal volume issues.
Clinical Conditions Affecting Tidal Volume
Certain lung diseases and brain injuries can cause high tidal volume on a ventilator. This means the lungs take in more air than usual during each breath. Changes in lung compliance or respiratory drive often lead to this increase.
Understanding the clinical conditions that affect tidal volume is crucial for anyone managing ventilated patients. Tidal volume is the amount of air moved into or out of the lungs during a normal breath. Various health issues can lead to changes in this volume, necessitating different approaches to ventilation.Acute Respiratory Distress Syndrome
Acute Respiratory Distress Syndrome (ARDS) significantly impacts tidal volume. Patients with ARDS often have stiff lungs due to fluid accumulation, making it difficult to deliver adequate ventilation. Lower tidal volumes are usually required to prevent further lung injury, but this must be carefully managed to ensure sufficient oxygenation.Copd And Asthma Effects
Chronic Obstructive Pulmonary Disease (COPD) and asthma can also alter tidal volume. In these conditions, airway obstruction makes it challenging to exhale fully, leading to air trapping and increased lung volumes. Adjusting ventilator settings to accommodate these changes is essential to avoid over-distention and barotrauma.Neuromuscular Disorders
Neuromuscular disorders, such as ALS or muscular dystrophy, can lead to reduced tidal volume due to weakened respiratory muscles. This reduction can result in inadequate ventilation and the need for ventilatory support. Tailoring ventilator settings to the patient’s specific muscular capability is crucial for effective management. Recognizing how these conditions affect tidal volume helps in optimizing ventilator settings. Have you encountered these challenges in patient care? How do you ensure your approach adapts to the unique needs of each clinical condition?Credit: www.droracle.ai
Monitoring And Adjusting Tidal Volume
Monitoring and adjusting tidal volume on a ventilator is essential to ensure patient safety and effective respiratory support. Tidal volume that is too high can cause lung injury, while too low a volume might lead to inadequate ventilation. You need to closely track and tweak settings based on real-time data and patient response.
Continuous Monitoring Techniques
Continuous monitoring allows you to catch changes in tidal volume early. Modern ventilators often have built-in sensors that provide real-time feedback on volume, pressure, and flow rates. Watching these parameters helps you spot trends before complications arise.
Using waveform displays can be especially helpful. They show breath-by-breath information, letting you see if tidal volume is consistent or if sudden spikes occur. This visual data can guide quick adjustments to ventilator settings.
Another useful tool is capnography, which measures exhaled CO2. It indirectly reflects ventilation efficiency and can alert you to inadequate tidal volume or patient-ventilator asynchrony. Have you ever noticed subtle changes on the waveform that hinted at a problem before vital signs changed?
Strategies For Volume Control
Adjusting tidal volume isn’t just about turning a dial. You must consider the patient’s lung compliance, airway resistance, and overall condition. Setting a volume based on ideal body weight rather than actual weight helps avoid overdistension.
Pressure-controlled ventilation modes can help limit tidal volume by capping airway pressure, reducing the risk of lung injury. You might also use volume-targeted modes, which adjust pressure to achieve a set tidal volume, balancing safety and effectiveness.
Regularly reassess settings as the patient’s condition changes. Small tweaks can prevent complications and improve comfort. Ask yourself: is the current tidal volume supporting gas exchange without causing harm?

Credit: www.respiratorytherapyzone.com
Frequently Asked Questions
What Causes High Tidal Volume On A Ventilator?
High tidal volume can result from improper ventilator settings, patient-ventilator asynchrony, or lung compliance changes. It may also occur due to excessive pressure support or incorrect tidal volume presets, risking lung injury if not managed carefully.
How Does Lung Compliance Affect Tidal Volume?
Increased lung compliance allows lungs to expand more easily, potentially raising tidal volume. Conversely, decreased compliance restricts lung expansion, reducing tidal volume. Monitoring compliance helps adjust ventilator settings to maintain safe and effective tidal volumes.
Can Patient Effort Increase Tidal Volume On A Ventilator?
Yes, spontaneous breathing efforts by a patient can increase tidal volume. When patients trigger breaths or exert effort, they may inadvertently raise delivered volumes, necessitating close monitoring and ventilator adjustments to avoid overdistension.
What Risks Are Associated With High Tidal Volume?
High tidal volume can cause lung overdistension, barotrauma, volutrauma, and worsen lung injury. It increases the risk of ventilator-induced lung damage and prolonged mechanical ventilation, emphasizing the need for careful tidal volume control.
Conclusion
High tidal volume on a ventilator can cause serious problems. It often results from incorrect settings or patient changes. Doctors and nurses must watch these signs closely. Adjustments help keep breathing safe and effective. Understanding causes helps prevent lung injury and other risks.
Stay informed and ask questions about ventilator care. This knowledge supports better treatment and recovery.