Have you ever wondered how long someone can stay on a ventilator? Whether it’s for yourself, a loved one, or just out of curiosity, understanding this can make a big difference.
Knowing the facts helps you feel more in control during a stressful time. You’ll discover what affects the length of time on a ventilator and what it means for recovery. Keep reading—you’ll find answers that can ease your worries and prepare you for what’s ahead.
Ventilator Basics
Understanding the basics of ventilators is crucial if you or a loved one faces a situation where breathing support becomes necessary. Ventilators are life-saving machines but knowing what they do and when they are needed can ease fears and help you engage better with healthcare providers.
What Is A Ventilator
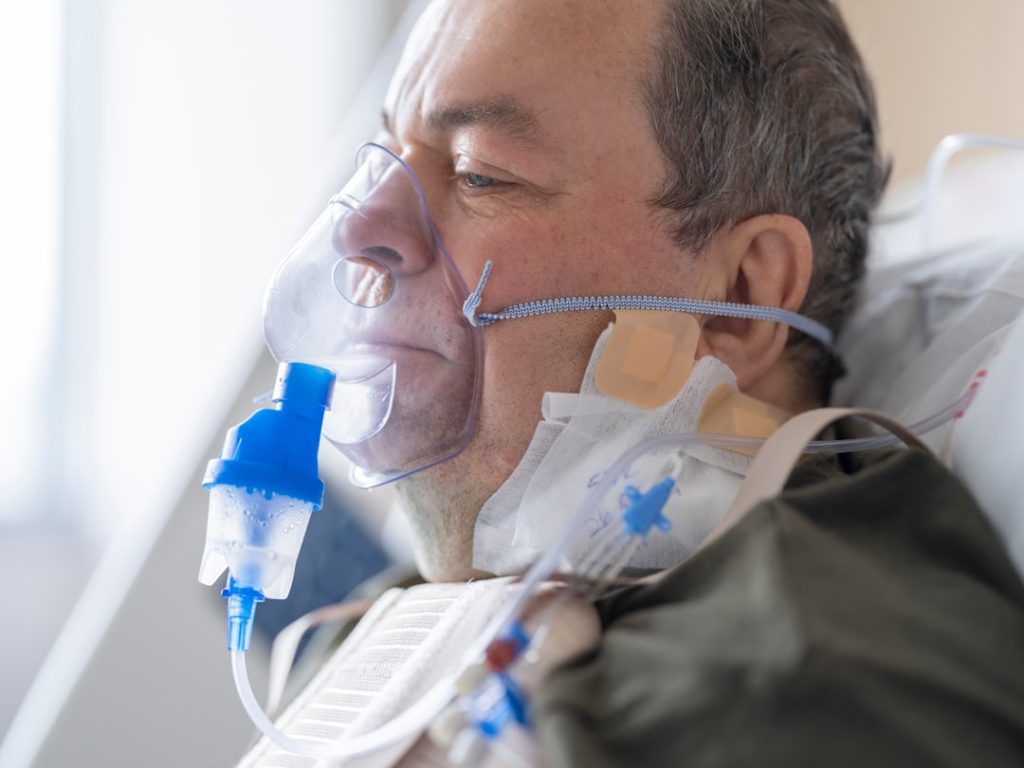
A ventilator is a machine that helps you breathe when your lungs can’t do the job on their own. It pushes air in and out of your lungs through a tube inserted into your windpipe. This process ensures your body gets the oxygen it needs and removes carbon dioxide efficiently.
Ventilators come in different types, including invasive and non-invasive. Invasive ventilation uses a tube inserted into your airway, while non-invasive uses masks. Both support breathing but are chosen based on how severe your condition is.
When Is Ventilation Needed
You might wonder when a ventilator becomes necessary. It’s typically needed when your lungs cannot provide enough oxygen or remove carbon dioxide adequately. This can happen due to severe illnesses like pneumonia, COVID-19, or after major surgery.
Sometimes, ventilation is short-term, such as during surgery or a brief illness. Other times, it may be required for longer periods if the lungs remain weak. The key is that a ventilator buys time for your body to heal or for doctors to treat the underlying problem.
Have you ever faced a situation where breathing became difficult? Knowing when and why a ventilator is used can help you feel more in control during emergencies or critical care moments.
Duration Factors
The length of time a person stays on a ventilator varies greatly. Many factors influence this duration. Understanding these factors helps in predicting recovery and care needs. Some patients may need ventilators for just a few days, while others require weeks or more.
Underlying Health Conditions
Chronic illnesses affect how long a patient stays on a ventilator. Conditions like diabetes, heart disease, or lung problems slow healing. These diseases reduce the body’s ability to recover quickly. Patients with weak immune systems often need longer ventilation support.
Type Of Illness Or Injury
The reason for ventilation impacts the duration. Severe infections or major injuries often require extended use. For example, pneumonia or trauma to the chest may prolong ventilator time. Some illnesses improve faster, allowing earlier removal from the ventilator.
Patient Age And Strength
Older patients generally take longer to recover breathing on their own. Age weakens lung function and muscle strength. Younger, stronger patients often come off ventilators sooner. Physical fitness before illness also helps shorten ventilation duration.
Short-term Ventilation
Short-term ventilation refers to the use of a mechanical ventilator to support a person’s breathing for a limited period. This usually happens when someone experiences a sudden medical event that makes it hard to breathe on their own. Understanding how long you or a loved one might need this support can help you prepare emotionally and practically.
Typical Time Frames
Most people stay on a ventilator for a few hours to several days. The exact duration depends on the underlying cause and how quickly the lungs recover. For example, after surgery, ventilation might last only a few hours until you wake up fully and can breathe independently.
In cases like severe infections or trauma, the time on a ventilator might extend to several days. Doctors monitor your progress daily and try to reduce ventilator support as soon as it’s safe. Have you ever wondered how medical teams decide the right moment to start weaning someone off the ventilator?
Common Scenarios
- Post-Surgery Recovery:Ventilation helps maintain breathing after anesthesia wears off, often lasting a few hours.
- Severe Pneumonia or Lung Injury:You might need a ventilator for several days until your lungs heal enough to work alone.
- Acute Respiratory Failure:Sudden conditions like asthma attacks or heart failure can require short-term ventilator support.
Each situation demands careful attention to avoid complications like lung damage or infections. I once witnessed a patient come off a ventilator just two days after a severe asthma attack, showing how quickly recovery can happen with the right care. What would you want to know if someone you care about needed short-term ventilation?

Credit: www.michiganmedicine.org
Long-term Ventilation
Long-term ventilation supports patients who cannot breathe on their own for extended periods. It helps maintain oxygen levels and remove carbon dioxide from the body. Some patients may need this support for weeks, months, or even years. The process requires careful management to avoid serious health issues.
Extended Use Challenges
Using a ventilator for a long time brings many challenges. Patients may feel discomfort from the breathing tube. It can cause soreness in the throat and mouth. Communication becomes hard since speaking is limited. Mobility also decreases because of the attached machines.
Healthcare teams must monitor patients closely. They adjust settings to fit changing needs. Preventing infections around the tube is critical. Patients often need physical therapy to keep muscles strong. Emotional support helps reduce anxiety and stress.
Risks And Complications
Long-term ventilation carries risks and complications. Lung infections, such as pneumonia, are common. The breathing tube can damage vocal cords or airways. Muscle weakness can develop from less natural breathing effort. Skin sores may form from pressure by tubes and devices.
Other risks include lung damage due to high pressure. Blood clots might form from limited movement. Patients may face difficulty weaning off the ventilator. Regular care and monitoring reduce these dangers. Early detection is key to managing problems.
Weaning Off The Ventilator
Weaning off the ventilator is a critical phase in a patient’s recovery. It means gradually reducing the support the machine provides until the person can breathe independently. This process requires careful monitoring and precise timing to avoid complications.
Signs Of Readiness
Recognizing when a person is ready to wean is essential. Some common signs include stable vital signs, improved lung function, and the ability to cough and clear secretions.
Doctors also look for:
- Steady breathing rate without excessive effort
- Good oxygen levels on minimal ventilator support
- Alertness and ability to follow commands
Have you ever wondered how doctors decide the exact moment to start this delicate process? It’s about balancing risks and benefits, ensuring the patient is strong enough to handle breathing on their own.
Weaning Methods
There are several ways to help a person wean off the ventilator. The method chosen depends on the patient’s condition and response.
Common approaches include:
- Spontaneous Breathing Trials (SBTs):The patient breathes without assistance for short periods, testing their strength.
- Pressure Support Ventilation:The machine reduces pressure gradually, encouraging the lungs to work harder.
- CPAP (Continuous Positive Airway Pressure):Keeps airways open while the patient breathes independently.
Each method requires close observation to catch any signs of distress early. Have you thought about how your body would react after being on a ventilator? The goal is to make the transition as smooth and safe as possible.
Impact On Quality Of Life
The use of a ventilator can significantly affect a person’s quality of life. Extended ventilator support can lead to various challenges. These challenges often impact physical, emotional, and psychological well-being. Understanding these effects helps in better managing patient care.
Physical Effects
Prolonged ventilator use can cause physical complications. Muscle weakness is a common issue. Patients may experience difficulty moving limbs. Skin problems, like pressure sores, can develop. Ventilators might lead to infections in the lungs. These infections can be serious.
Another concern is loss of muscle mass. This happens because of limited mobility. Reduced mobility affects overall health. Patients may need physiotherapy to regain strength.
Emotional And Psychological Aspects
Being on a ventilator can take a toll emotionally. Many patients feel anxiety or fear. The inability to speak can increase frustration. Communication becomes a major challenge. This can lead to feelings of isolation.
Depression is another risk for ventilated patients. The stress of being in a hospital environment adds to this. Support from family and mental health professionals is crucial. Positive interactions can improve emotional well-being.
Care And Monitoring
Care and monitoring play a key role in helping a person stay on a ventilator safely. The process requires constant attention to avoid complications and to support recovery. Medical staff and family work closely to provide the best care for the patient. Both groups help in different but important ways.
Role Of Medical Staff
Medical staff watch the patient’s breathing and vital signs all the time. They adjust the ventilator settings to match the patient’s needs. Nurses and doctors check for infections or other problems regularly. They also provide medicines and fluids to keep the body stable. Their goal is to help the patient breathe better and avoid risks.
Staff use special tools to monitor oxygen levels and lung function. They keep track of how the patient responds to treatment. If there are any changes, they act fast to solve issues. Their care helps prevent long-term damage or complications from ventilation.
Family Support
Family members give emotional strength to the patient. Their presence can comfort and calm someone on a ventilator. They also help doctors and nurses by sharing important health information. Families learn about the patient’s condition and care needs. This helps them understand the treatment plan better.
Families can assist with simple tasks like talking or holding the patient’s hand. Their love and support improve the patient’s mood and hope. This positive effect can speed up healing and make recovery smoother. Family involvement is a vital part of care and monitoring.
Credit: emedicine.medscape.com
Technological Advances
Advances in technology have improved ventilator care, allowing some patients to stay on them for weeks or months. The exact time depends on health, illness, and treatment progress. Doctors closely monitor patients to ensure the best possible recovery.
In recent years, technological advances have dramatically transformed the way ventilators are used in healthcare settings. These innovations not only enhance the efficiency and safety of ventilators but also significantly improve patient outcomes. With these advancements, the question of how long a person can safely stay on a ventilator is being redefined.Improved Ventilator Designs
Modern ventilators are designed with the patient’s comfort and safety in mind. These devices now come equipped with features like better airflow control and more precise oxygen delivery. Such innovations reduce the risk of complications, allowing patients to remain on ventilators for longer periods without adverse effects. For instance, newer ventilators can adjust the breathing support they provide based on the patient’s needs in real time. This adaptability helps in maintaining optimal respiratory function. Have you ever thought about how a machine could be so in tune with human needs?Remote Monitoring
Remote monitoring is another game-changer in ventilator technology. It allows healthcare professionals to keep a close watch on patients’ conditions without needing to be physically present. Through advanced sensors and internet connectivity, ventilators can send real-time data to medical staff. This means any changes in the patient’s condition can be detected and addressed promptly, enhancing patient safety. Think about the peace of mind this brings to both patients and caregivers. How much more confident would you feel knowing experts are virtually by your side 24/7? These technological advances are reshaping the landscape of mechanical ventilation, offering hope and extended care options for patients who need it the most.
Credit: www.weforum.org
Frequently Asked Questions
How Long Can A Person Stay On A Ventilator Safely?
A person can stay on a ventilator from a few days to several weeks. The duration depends on their condition and recovery rate. Doctors regularly assess to minimize risks like infections or lung damage. Prolonged use requires careful monitoring and specialized care.
What Factors Affect Ventilator Duration For Patients?
Factors include the patient’s age, overall health, and reason for ventilation. Severity of illness and lung function also impact duration. Recovery speed and response to treatment play key roles. Personalized care plans help determine how long ventilation is needed.
Can Long-term Ventilator Use Cause Complications?
Yes, long-term ventilator use can lead to complications. Risks include lung infections, muscle weakness, and airway damage. Proper care and hygiene reduce these risks. Medical teams work to balance ventilation benefits with potential side effects.
When Is It Safe To Wean Off A Ventilator?
Weaning is safe when the patient shows stable breathing and lung function. Doctors evaluate strength, oxygen levels, and overall health. Gradual reduction in support tests readiness. Successful weaning minimizes ventilator-related risks and promotes recovery.
Conclusion
Time on a ventilator varies for each patient. Some stay a few days, others weeks or months. Doctors watch closely to decide the best time to stop. Staying too long can cause problems, so care is careful and steady. Families should stay informed and ask questions.
Understanding the process helps ease worry. Ventilator use helps many people breathe when they cannot on their own. Recovery depends on health and response to treatment. Patience and good care make a big difference in the outcome.