Are you confused about whether BiPAP is a type of mechanical ventilation? You’re not alone.
Understanding medical terms can be tricky, especially when it comes to breathing support devices. Knowing the difference can make a big impact on how you view treatment options for respiratory issues. You’ll discover what BiPAP really is, how it works, and how it compares to mechanical ventilation.
By the end, you’ll feel more confident about these important tools for breathing support. Keep reading to clear up the confusion and learn what matters most for your health or that of someone you care about.
Credit: www.biosysmed.com
Bipap Basics
Understanding the basics of Bipap is key if you’re exploring respiratory support options. Bipap, short for Bilevel Positive Airway Pressure, helps people breathe easier without the need for invasive machines. It offers a unique approach that sits between simple oxygen therapy and full mechanical ventilation.
What Bipap Does
Bipap delivers two levels of air pressure to support your breathing. One pressure helps you inhale, while a lower pressure assists your exhale. This dual-pressure system reduces the effort your lungs need to take in and push out air.
Unlike traditional mechanical ventilators that fully control breathing, Bipap works with your natural breathing pattern. It’s often used for conditions like sleep apnea, COPD, or other breathing difficulties where you need extra help but can still breathe on your own.
Think about how tiring it feels when you’re short of breath. Bipap gives your respiratory muscles a break, making breathing less exhausting. Have you ever wondered how this non-invasive device can provide such relief without a tube down your throat?
How Bipap Works
Bipap machines connect to a mask covering your nose or mouth. The machine senses when you breathe in and increases air pressure to open your airways. When you breathe out, the pressure decreases to make exhaling easier.
This process happens continuously and automatically. The machine adjusts to your breathing pattern, providing support only when needed. This helps maintain steady oxygen and carbon dioxide levels in your blood.
Imagine the machine as a gentle guide that matches your breath’s rhythm. It doesn’t take over but helps you breathe more efficiently. Have you ever noticed how a little support can make a big difference in managing your symptoms?
Mechanical Ventilation Explained
Mechanical ventilation is a lifesaving technique used when people cannot breathe adequately on their own. It supports or replaces natural breathing by moving air into and out of the lungs. Understanding how mechanical ventilation works can help you grasp where devices like BiPAP fit in.
Types Of Mechanical Ventilators
Mechanical ventilators come in various forms, each designed for specific needs. The main types include:
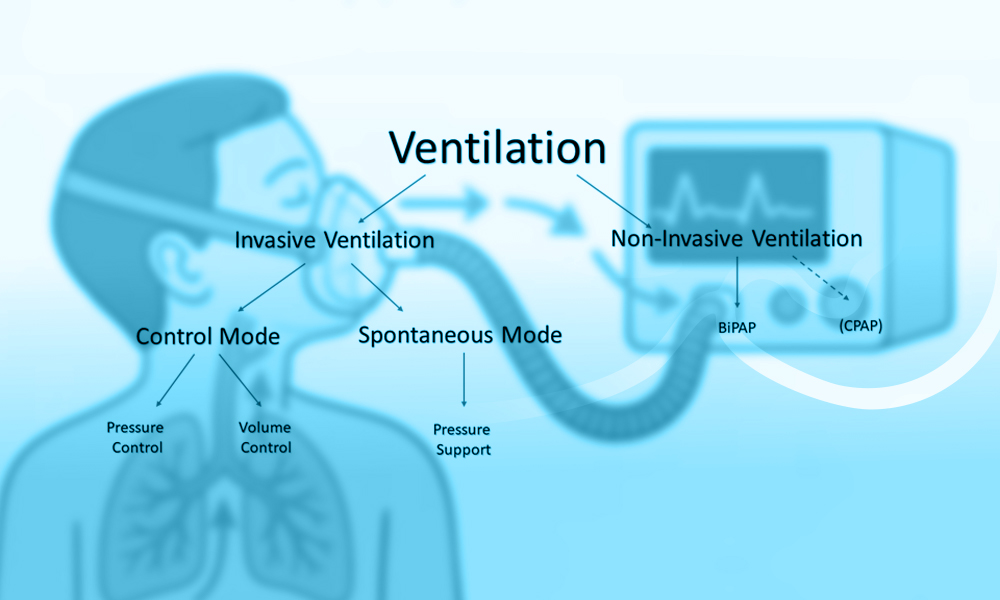
- Invasive Ventilators:These require a tube inserted into the airway, usually through the mouth or neck. They provide full control over breathing.
- Non-Invasive Ventilators:These use masks or similar devices to support breathing without needing intubation. BiPAP machines fall under this category.
- Portable Ventilators:Designed for mobility, these allow patients to move while still receiving ventilation support.
Have you ever wondered why some patients use a mask instead of a tube? The answer lies in the level of support needed and how invasive the treatment must be.
Functions Of Mechanical Ventilation
Mechanical ventilation helps your lungs by doing one or more of the following:
- Oxygen Delivery:It ensures your body receives enough oxygen when your lungs can’t do it alone.
- Carbon Dioxide Removal:Ventilators help remove excess carbon dioxide, preventing harmful buildup.
- Breath Assistance:They can fully control breathing or assist your natural efforts, depending on your condition.
Imagine struggling to catch your breath after intense exercise—that’s what some patients experience constantly. Mechanical ventilation steps in to ease this burden and maintain vital functions.
Bipap Vs Mechanical Ventilation
Understanding the difference between Bipap and mechanical ventilation can be confusing, especially if you’re new to respiratory support options. Both help people breathe, but they do so in distinct ways. Knowing these differences can help you or your loved ones make informed decisions about respiratory care.
Similarities Between Bipap And Ventilators
Both Bipap and mechanical ventilators assist with breathing by delivering air to the lungs.
They are used when a person struggles to breathe on their own due to illness or injury.
- Both systems use masks or tubes to deliver air.
- They can control the amount and pressure of air given.
- Each can improve oxygen levels and reduce the work of breathing.
When my father needed help breathing after surgery, the medical team initially used Bipap before moving to full mechanical ventilation. This shift highlighted how both systems support breathing but serve different needs.
Key Differences To Know
Bipap stands for Bilevel Positive Airway Pressure and is a non-invasive method. It uses a mask to deliver two levels of pressure: one for inhaling and a lower one for exhaling.
Mechanical ventilation can be invasive, often involving a tube inserted into the airway. It provides full control over breathing rate, volume, and pressure.
| Aspect | Bipap | Mechanical Ventilation |
|---|---|---|
| Invasiveness | Non-invasive (mask) | Often invasive (intubation) |
| Usage | For moderate breathing difficulties | For severe respiratory failure |
| Control | Assists spontaneous breathing | Can fully control breathing |
| Mobility | More portable and comfortable | Less portable, requires intensive monitoring |
Have you ever wondered why some patients start with Bipap but later need mechanical ventilation? The answer lies in the severity of their condition and how much breathing support they require. Knowing these differences can guide you in recognizing what each treatment means for patient care.
When Bipap Is Used
BIPAP, or Bilevel Positive Airway Pressure, helps people breathe better without a tube in the windpipe. It provides two levels of air pressure: one for inhaling and one for exhaling. This support helps the lungs get enough air and reduces the work of breathing. BIPAP is used in certain medical situations where breathing is difficult but a full ventilator is not yet needed.
Conditions Treated With Bipap
- Chronic obstructive pulmonary disease (COPD) flare-ups
- Sleep apnea causing breathing pauses at night
- Heart failure leading to fluid buildup in the lungs
- Respiratory failure from pneumonia or lung infections
- Neuromuscular diseases that weaken breathing muscles
BIPAP helps by keeping airways open and improving oxygen levels. It reduces the need for invasive mechanical ventilation in many cases.
Patient Suitability
BIPAP suits patients who can breathe on their own but need extra help. It works best if the patient is awake and able to cooperate. Patients must be able to clear their own airway and cough effectively. It is not suitable for those with severe unconsciousness or high risk of vomiting.
Doctors carefully evaluate each patient’s breathing status before recommending BIPAP. The goal is to avoid more invasive ventilation when possible, while ensuring safety.
Risks And Benefits
Understanding the risks and benefits of Bipap helps in making informed health decisions. Bipap offers breathing support without invasive procedures. It assists patients who struggle with breathing but do not require full mechanical ventilation. The balance of its advantages and limitations defines its role in respiratory care.
Advantages Of Bipap
- Improves oxygen levels and reduces carbon dioxide in the blood.
- Non-invasive method, avoiding the need for intubation.
- Allows patients to speak and eat while receiving support.
- Can be used at home for chronic respiratory conditions.
- Reduces work of breathing and respiratory muscle fatigue.
- Helps prevent respiratory failure in certain cases.
Potential Risks And Limitations
- May cause discomfort or skin irritation from the mask.
- Possible air leaks reduce effectiveness of treatment.
- Not suitable for patients with severe respiratory failure.
- Risk of aspiration if vomiting occurs during use.
- Can cause dryness or nosebleeds due to airflow.
- Requires careful monitoring by healthcare professionals.

Credit: www.apexhospitals.com
Bipap In Clinical Practice
BiPAP provides non-invasive breathing support by delivering air pressure through a mask. It is not a full mechanical ventilator but helps patients breathe better. This device supports breathing without the need for intubation.
Bipap in Clinical Practice Bipap, or Bilevel Positive Airway Pressure, is common in clinical settings. It helps patients with breathing difficulties. This device supports those with respiratory issues. It offers a non-invasive way to assist breathing. In clinical practice, its use is widespread. Medical staff must understand its operation and care. Let’s explore its settings and adjustments, as well as monitoring and care.Settings And Adjustments
Bipap devices have customizable settings. Each patient needs specific adjustments. The machine has two pressure settings. Inspiratory Positive Airway Pressure (IPAP) supports inhalation. Expiratory Positive Airway Pressure (EPAP) assists exhalation. Adjustments depend on patient needs. Factors include comfort and breathing patterns. Medical professionals set the pressures carefully. This ensures effective and comfortable breathing support.Monitoring And Care
Regular monitoring is essential for Bipap therapy. It ensures the device works properly. Careful observation helps track patient progress. Healthcare providers check patient response to therapy. They adjust settings if needed. Proper mask fit is crucial. A well-fitted mask prevents air leaks. It enhances the effectiveness of the therapy. Staff must ensure cleanliness. Regular cleaning of the device and mask is important. It prevents infections and maintains device function. Proper care enhances the patient’s comfort and recovery..png?width=275&name=stencil.instagram-photo%20(90).png)
Credit: blog.nursing.com
Frequently Asked Questions
Is Bipap Considered A Form Of Mechanical Ventilation?
BiPAP is a non-invasive mechanical ventilation method. It supports breathing by delivering two pressure levels. It is less invasive than traditional ventilators and helps patients with respiratory issues breathe easier.
How Does Bipap Differ From Invasive Mechanical Ventilation?
BiPAP uses a mask and does not require intubation. Invasive ventilation involves a tube inserted into the airway. BiPAP is used for milder respiratory distress and is more comfortable for patients.
Can Bipap Treat Respiratory Failure Effectively?
BiPAP can manage mild to moderate respiratory failure. It improves oxygenation and reduces breathing effort. However, severe cases may require invasive mechanical ventilation for better control.
When Is Bipap Preferred Over Mechanical Ventilation?
BiPAP is preferred for patients who need respiratory support but can breathe independently. It is ideal for sleep apnea, COPD exacerbations, and some heart failure cases. It avoids complications linked to invasive ventilation.
Conclusion
BiPAP is a type of breathing support but not full mechanical ventilation. It helps people breathe by giving air pressure through a mask. Mechanical ventilation usually means a machine takes full control of breathing. BiPAP supports breathing without replacing it completely.
Many patients use BiPAP at home or in hospitals for breathing help. Understanding the difference helps in choosing the right treatment. Breathing support is important, and knowing these terms can make a big difference. Always ask a doctor for advice on breathing devices.





