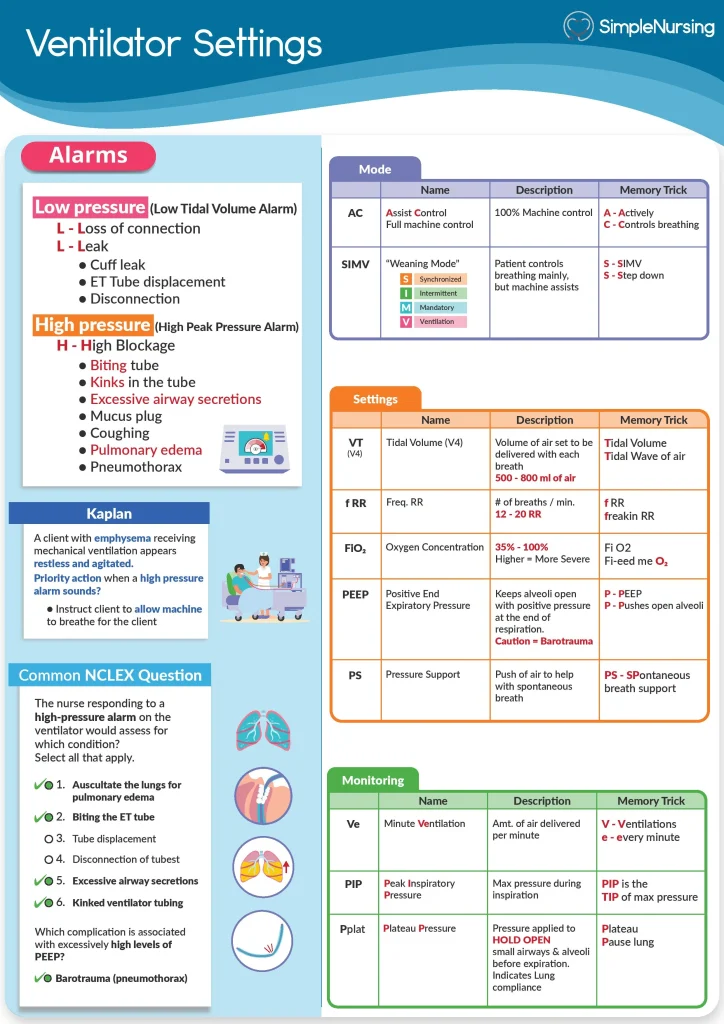
If you’re involved in critical care or respiratory therapy, knowing how to write ventilator settings correctly is essential. These settings directly impact a patient’s breathing and recovery, so precision matters.
But where do you start? How do you make sure every detail is clear and accurate? This guide will walk you through the steps, breaking down complex terms into simple language you can use confidently. By the end, you’ll have the tools to document ventilator settings like a pro—helping you provide better care and avoid costly mistakes.
Keep reading to master this vital skill.
Key Ventilator Parameters
Understanding key ventilator parameters is essential for setting up a ventilator that matches your patient’s needs. Each parameter influences how the machine supports breathing and affects patient comfort and safety. Knowing what each one does helps you adjust settings confidently and respond effectively to changes.
Tidal Volume
Tidal volume refers to the amount of air delivered to the lungs with each breath. It’s usually measured in milliliters or milliliters per kilogram of body weight. Setting this too high can cause lung injury, while too low may not provide enough oxygen. Think about a patient with ARDS; lower tidal volumes around 6 ml/kg help prevent further lung damage.
Respiratory Rate
This is how many breaths the ventilator gives per minute. Adjusting the respiratory rate helps control carbon dioxide levels in the blood. A higher rate can remove more CO2, but if set too fast, it may cause discomfort or breath stacking. Have you noticed how patients react differently to rate changes? Monitoring their comfort is key.
Fio2 Levels
FiO2 stands for the fraction of inspired oxygen. It tells you how much oxygen the ventilator delivers, ranging from 21% (room air) up to 100%. The goal is to provide enough oxygen without causing oxygen toxicity. You might start at 100% in emergencies, but gradually lower it to avoid lung injury as the patient stabilizes.
Peep Settings
Positive End-Expiratory Pressure (PEEP) keeps the lungs partially inflated between breaths. This prevents alveoli from collapsing and improves oxygenation. However, too much PEEP can reduce blood return to the heart and lower blood pressure. Balancing PEEP is like walking a tightrope—too little or too much can harm the patient.
Inspiratory Time
Inspiratory time is how long each breath lasts during inhalation. Adjusting it changes the pattern of airflow and gas exchange. A longer inspiratory time can improve oxygenation but may cause discomfort or air trapping if overdone. Have you ever adjusted this and noticed changes in patient tolerance? Watch closely and adjust based on response.

Credit: www.youtube.com
Patient Assessment Factors
Understanding patient assessment factors is crucial when setting a ventilator. Each patient’s condition varies, and your ability to tailor the settings can directly impact their recovery. Assessing key physiological parameters helps you decide the right ventilator adjustments that meet the patient’s real-time needs.
Lung Compliance
Lung compliance measures how easily the lungs expand and contract. Low compliance means stiff lungs, often seen in conditions like ARDS or fibrosis. You need to adjust tidal volume and pressures carefully to avoid lung injury.
Have you noticed how patients with different lung compliance respond to the same ventilator settings? Adjusting based on compliance can prevent overdistension or inadequate ventilation.
Oxygenation Needs
Oxygenation reflects how well oxygen moves from the lungs into the blood. Patients with pneumonia or pulmonary edema often need higher oxygen settings. Monitoring saturation levels (SpO2) and arterial blood gases guides you to set the right FiO2 and PEEP.
Think about a time when a slight increase in PEEP improved your patient’s oxygen levels significantly. Small changes can make a big difference in oxygen delivery.
Co2 Clearance
CO2 clearance depends on how effectively the lungs remove carbon dioxide. If CO2 builds up, it signals the need to increase ventilation rate or tidal volume. Watch for signs like altered pH or rising PaCO2 in blood gases to adjust settings promptly.
Have you ever adjusted ventilation to quickly correct a patient’s high CO2? Timely changes can prevent acidosis and respiratory distress.
Hemodynamic Status
Hemodynamics refers to blood flow and pressure within the cardiovascular system. Ventilator settings can impact heart function, especially with high PEEP or pressures. Monitor blood pressure, heart rate, and signs of poor perfusion to balance ventilation and circulation.
Remember, pushing ventilation too hard can reduce cardiac output. How do you usually balance oxygenation needs without compromising hemodynamics?
Common Ventilator Modes
Understanding common ventilator modes helps healthcare workers set machines correctly. Each mode controls how air is delivered to the patient’s lungs. Knowing these modes ensures better patient care and safer ventilation.
Volume-controlled Ventilation
This mode delivers a fixed volume of air with each breath. The ventilator controls the amount of air, not the pressure. It ensures the patient receives a consistent volume every time. Pressure may vary depending on lung resistance.
Pressure-controlled Ventilation
Here, the ventilator sets a fixed pressure for each breath. The volume of air can change based on lung compliance. This mode protects lungs from high pressure. It is useful for patients with fragile lung tissue.
Assist-control Ventilation
The ventilator helps the patient breathe by providing full breaths. It supports every breath the patient tries to take. If the patient does not initiate a breath, the machine gives one automatically. This mode is helpful for weak or tired patients.
Simv Mode
SIMV stands for Synchronized Intermittent Mandatory Ventilation. It gives set breaths at regular intervals. The patient can breathe spontaneously between these breaths. This mode helps patients regain normal breathing. It balances machine support and patient effort.

Credit: www.healthyjeenasikho.com
Steps For Accurate Documentation
Accurate documentation of ventilator settings is essential for patient safety and effective care. Clear records ensure proper communication among healthcare providers. It helps track changes and monitor patient progress. Precise documentation reduces errors and supports better treatment decisions.
Recording Initial Settings
Start by noting all initial ventilator parameters clearly. Include tidal volume, respiratory rate, FiO2, and PEEP values. Record the date and time of the start. Write the patient’s identification details for accuracy. Use legible handwriting or electronic entry to avoid mistakes.
Updating Changes Timely
Document any changes to settings immediately after adjustments. Note the reason for the change and the new values. Timely updates help keep the care team informed. Avoid delays to reduce confusion during patient care. Keep all changes consistent with the patient’s condition.
Using Standardized Forms
Use standardized forms or templates for uniform documentation. These forms guide what information to record. They ensure no vital data is missed. Standard forms improve clarity and speed during documentation. Many hospitals provide specific ventilator setting charts to use.
Double-checking Entries
Always review entries for accuracy after recording. Check numbers, units, and patient details carefully. Cross-verify with the ventilator screen or electronic system. A second check prevents errors that could harm the patient. Encourage team members to verify each other’s documentation.
Avoiding Common Errors
Setting ventilator parameters correctly is crucial. Mistakes can impact patient safety. Common errors are easy to avoid with awareness and attention.
Misreading Device Displays
Device displays can be complex. Misreading them leads to incorrect settings. Always double-check the display readings. Ensure the display is clear and functioning properly.
Incorrect Units
Incorrect units can cause serious mistakes. Always verify units for each parameter. Know the difference between milliliters and liters. Pay attention to pressure units, too.
Omitting Critical Parameters
Missing parameters can affect treatment. Always include tidal volume, rate, and FiO2. Check the ventilator mode and alarms. Ensure nothing is overlooked.
Failure To Communicate Changes
Communication is key in healthcare. Inform the team of any ventilator changes. Document each adjustment clearly. Keep everyone updated for patient safety.
Tips For Effective Communication
Effective communication is essential when writing ventilator settings. Clear and precise information helps ensure patient safety. It also promotes teamwork and reduces errors.
Sharing ventilator details in a way everyone understands is key. Use simple language and avoid jargon. Confirm that all team members know the plan and any changes.
Clear Handoffs
Handoffs between shifts or teams must be clear and complete. Include all important ventilator settings and patient responses. Use checklists or standardized forms to avoid missing details. Speak slowly and clearly. Confirm understanding by asking questions.
Collaborating With Team
Work closely with nurses, respiratory therapists, and doctors. Discuss ventilator settings and patient needs regularly. Share observations and concerns openly. Respect each team member’s input. This cooperation improves patient care and avoids confusion.
Using Visual Aids
Visual aids like charts, graphs, and diagrams help explain ventilator settings. Use color-coded charts to show changes over time. Post key settings at the bedside for quick reference. Visual tools make complex information easier to understand.
Patient-centered Adjustments
Adjust ventilator settings based on the patient’s condition and comfort. Communicate changes clearly to the whole team. Note patient reactions and progress in records. Always keep the patient’s needs as the top priority.
Technology And Tools
Technology and tools play a vital role in writing ventilator settings accurately. They help healthcare providers record, monitor, and adjust settings efficiently. Using the right tools reduces errors and improves patient care. Technology also makes it easier to share information among medical teams.
Electronic Medical Records
Electronic Medical Records (EMRs) store patient data digitally. They keep ventilator settings safe and easy to access. Doctors can quickly check past settings and changes. EMRs support better communication across departments. This saves time and helps track patient progress clearly.
Ventilator Software Integration
Modern ventilators connect with software systems for real-time data. This integration allows automatic updates of settings in patient charts. It helps in adjusting ventilator parameters based on patient needs. Software can alert staff about unusual readings. This ensures fast responses and safer care.
Alarm Settings
Alarm settings notify staff about changes in patient status. Proper alarm configuration prevents missing critical alerts. Alarms can be set for pressure, volume, and oxygen levels. Clear alarms help avoid alarm fatigue among healthcare workers. They play a key role in patient safety.
Mobile Apps For Monitoring
Mobile apps offer remote access to ventilator data. Nurses and doctors can monitor patients from anywhere. Apps provide real-time alerts and trend analysis. This improves response time and decision-making. Mobile tools make patient care more flexible and efficient.

Credit: www.icureach.com
Frequently Asked Questions
What Are The Essential Ventilator Settings To Know?
Essential ventilator settings include tidal volume, respiratory rate, FiO2, PEEP, and inspiratory flow. These control ventilation and oxygenation. Proper adjustment ensures patient comfort and safety.
How Do You Choose The Right Tidal Volume?
Tidal volume is typically 6-8 mL/kg of ideal body weight. It prevents lung injury and ensures adequate ventilation. Adjust based on patient condition and lung compliance.
Why Is Peep Important In Ventilator Settings?
PEEP prevents alveolar collapse and improves oxygenation. It maintains airway pressure during exhalation. Proper PEEP reduces lung injury and supports gas exchange.
How To Set Respiratory Rate For Mechanical Ventilation?
Set respiratory rate based on patient’s CO2 levels and clinical condition. Normal adult rates range from 12-20 breaths per minute. Adjust to maintain adequate ventilation and acid-base balance.
Conclusion
Writing ventilator settings clearly helps ensure patient safety and care. Always check and adjust settings based on patient needs. Keep notes simple and accurate for easy reading. Practice makes understanding settings easier over time. Stay confident and careful when documenting ventilator parameters.
This skill supports better communication among healthcare teams. It also helps avoid errors and improves treatment outcomes. Keep learning and reviewing guidelines to stay updated. Clear, precise settings matter in every medical situation.