Have you ever wondered what it really means when someone is placed on a ventilator? Is being on a ventilator the same as being on life support?
These questions can feel overwhelming, especially when it involves someone you care about. Understanding the truth behind ventilators and life support can help you make informed decisions and ease your worries. Keep reading to discover the facts, clear up common misunderstandings, and learn how this critical care tool fits into the bigger picture of life support.
Your peace of mind starts here.
Credit: www.agapehospicepc.org
What Is A Ventilator
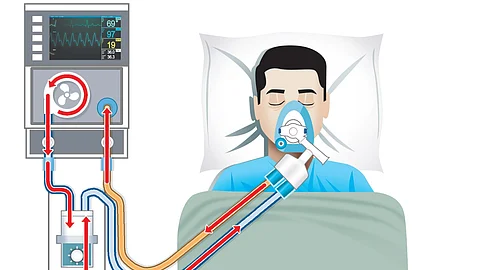
A ventilator is a machine that helps people breathe when they cannot do it on their own. It supports or replaces the work of the lungs. Doctors use ventilators in hospitals for patients with serious breathing problems. These machines deliver air, sometimes with extra oxygen, into the lungs. Ventilators play a key role in life support treatments.
How Ventilators Work
Ventilators push air into the lungs through a tube in the airway. They control the flow, pressure, and oxygen level of the air. The machine can work with the patient’s breathing or take over completely. Sensors in the ventilator monitor breathing effort and adjust the air delivery. This helps keep oxygen and carbon dioxide levels balanced in the blood.
Types Of Ventilators
- Invasive Ventilators:Use a tube inserted into the windpipe. Provide full breathing support.
- Non-invasive Ventilators:Use masks over the nose or mouth. Support breathing without surgery.
- Portable Ventilators:Small and mobile. Used for patients needing breathing help outside hospitals.
- High-frequency Ventilators:Deliver very fast, small breaths. Used in special cases like lung injury.

Credit: www.news18.com
Ventilators And Life Support
Understanding the relationship between ventilators and life support helps clarify a lot of confusion about medical care in critical situations. Many people wonder if being on a ventilator automatically means a person is on life support. Let’s break down what life support truly means and where ventilators fit in this context.
Definition Of Life Support
Life support refers to treatments that replace or support essential bodily functions when they fail. These treatments help maintain life while the underlying cause is treated or the body heals. Life support can include mechanical devices, medications, or therapies that assist breathing, circulation, or other vital functions.
It’s important to understand that life support is not a single treatment but a range of interventions. Some examples include dialysis for kidney failure, mechanical ventilation for breathing, and medications to support heart function.
Role Of Ventilators In Life Support
Ventilators are machines that help patients breathe when they cannot do so on their own. They deliver oxygen to the lungs and remove carbon dioxide, which is critical for survival in many severe illnesses or injuries.
Being on a ventilator is considered a form of life support because it takes over the vital function of breathing. However, not every patient on a ventilator is in the same situation; some might use it temporarily after surgery, while others may require it long-term.
Have you ever thought about how much we rely on breathing without even noticing? Ventilators step in when your body needs help with this basic function, showing how crucial they are in life support systems.
When Is Ventilator Use Considered Life Support
Ventilator use becomes life support based on how and why it is used. It depends on the length of time and the medical condition involved. Understanding these factors helps clarify when a ventilator supports life or aids recovery.
Temporary Vs. Long-term Use
Ventilators can be used for short or long periods. Short-term use usually supports breathing during surgery or illness. The patient often recovers and breathes independently afterward.
Long-term use means the ventilator helps the patient breathe continuously. This often happens when lungs or breathing muscles are weak. The ventilator acts as a life support machine in these cases.
Medical Conditions Requiring Ventilators
Several conditions need ventilator support. Examples include:
- Severe pneumonia or lung infections
- Chronic obstructive pulmonary disease (COPD)
- Neuromuscular diseases like ALS
- Spinal cord injuries affecting breathing
- Trauma or brain injury causing breathing failure
In these conditions, the ventilator maintains breathing when the body cannot do it alone. It keeps vital organs alive, classifying it as life support.
Credit: www.expressnews.com
Ethical And Legal Considerations
Being on a ventilator is not just a medical decision; it carries deep ethical and legal weight. Understanding these considerations helps you navigate complex situations, especially when it involves life support choices for yourself or a loved one. You face questions about autonomy, rights, and what defines quality of life in critical moments.
Patient Consent And Decision Making
Consent is a cornerstone of ethical medical care. You must have the right to accept or refuse ventilation, except in emergencies where you can’t communicate. Advance directives or living wills can guide healthcare providers if you’re unable to speak for yourself.
It’s important to discuss your wishes with family members and medical teams early. This reduces confusion and conflict later on. Imagine a scenario where a patient’s wishes are unclear—family members may disagree, causing emotional strain and legal disputes.
Doctors also balance respecting your autonomy with their duty to preserve life. They may encourage ventilation but cannot force it without your consent or legal authorization. Are you prepared to make these decisions, or have you shared your preferences with those who will advocate for you?
End-of-life Care And Ventilation
Ventilation at the end of life raises tough questions about prolonging life versus prolonging suffering. You might wonder if continuing ventilation truly improves your quality of life or just extends the dying process.
Hospitals often have ethics committees to help resolve conflicts about stopping or starting ventilation. These committees consider medical facts, patient values, and legal standards to recommend the best course of action.
Many people find comfort in knowing they can refuse ventilation if it no longer aligns with their goals. This decision is deeply personal and can involve spiritual, cultural, and emotional factors. Have you thought about what matters most to you if faced with this choice?
Alternatives And Complementary Supports
Being on a ventilator is often seen as a critical measure. Yet, it is not the only life support option available. Many patients benefit from alternatives or complementary supports. These solutions can sometimes offer less invasive and more comfortable care. Understanding these options can help in making informed decisions.
Non-invasive Ventilation Options
Non-invasive ventilation (NIV) is a gentler alternative. It uses a mask to support breathing. This method avoids tubes in the throat. Patients often prefer NIV due to comfort. It is useful for conditions like sleep apnea or COPD.
BiPAP and CPAP are common NIV methods. BiPAP provides two pressure levels. One for inhalation, another for exhalation. This makes breathing easier. CPAP delivers a constant pressure. It keeps airways open during sleep.
Other Life Support Measures
Life support includes more than just ventilation. Intravenous (IV) therapy is crucial. It delivers fluids and medications directly into the bloodstream. This supports hydration and nutrition.
Dialysis is another life-saving measure. It helps when kidneys fail. The machine filters waste from the blood. It takes over the kidney’s job temporarily.
Cardiac support devices assist the heart. Pacemakers and defibrillators regulate heartbeats. They ensure the heart pumps efficiently. These devices can be life-changing for heart patients.
Impact On Patients And Families
The impact of being on a ventilator extends far beyond the medical realm. It deeply affects both patients and their families in ways that are emotional, psychological, and practical. Understanding these effects can help you navigate this challenging experience with greater awareness and compassion.
Emotional And Psychological Effects
Patients on ventilators often face feelings of fear and vulnerability. The loss of control over basic functions like breathing can be overwhelming and disorienting.
Families, too, experience intense stress. Watching a loved one rely on machines for survival raises questions about hope, quality of life, and future decisions.
Sometimes, patients struggle with anxiety or depression after coming off the ventilator. Families might feel guilt or helplessness during the process.
Have you considered how these emotions might influence medical decisions or communication within your family?
Support Resources
Access to support resources can make a significant difference. Hospitals often provide counseling services for both patients and families.
- Peer support groups where you can share experiences and advice
- Professional mental health support tailored for critical illness recovery
- Educational materials explaining ventilator use and what to expect
Connecting with others who have faced similar situations can reduce feelings of isolation. You can also ask your healthcare team about social workers or patient advocates who specialize in helping families cope.
What kind of support would help you feel more confident during such a difficult time?
Frequently Asked Questions
Is Being On A Ventilator Considered Life Support?
Yes, being on a ventilator is considered a form of life support. It helps patients breathe when they cannot do so on their own. Ventilators provide mechanical breathing assistance in critical medical conditions.
How Does A Ventilator Support Life?
A ventilator supports life by delivering oxygen and removing carbon dioxide. It mechanically assists or replaces spontaneous breathing. This support is crucial for patients with severe respiratory failure or during surgery.
Can A Patient Survive Without A Ventilator?
Patients who cannot breathe independently usually cannot survive without a ventilator. The device maintains vital oxygen levels. However, some patients may recover and eventually breathe without assistance.
What Conditions Require Ventilator Life Support?
Ventilator life support is needed in conditions like pneumonia, COPD, COVID-19, or trauma. It also supports patients during anesthesia and critical care situations. The goal is to ensure adequate oxygenation and breathing.
Conclusion
Being on a ventilator means a machine helps you breathe. It supports life by doing the work your lungs cannot. This support can be short-term or long-term depending on your health. Doctors use ventilators to save lives in critical situations.
Understanding this helps reduce fear and confusion about treatment. Always ask medical staff for clear information about your care. Knowing the facts gives you control and peace of mind. Life support is serious but often necessary to help recovery.