If you’re caring for someone on a ventilator, you know how important it is to keep their breathing as comfortable as possible. One key factor is Peak Inspiratory Pressure, or PIP, which can sometimes rise and cause discomfort or even harm.
But don’t worry—there are clear, practical steps you can take to safely decrease PIP and improve your patient’s comfort and outcomes. You’ll discover simple, effective ways to manage PIP on a ventilator, so you can feel confident in providing the best care possible.
Keep reading to learn exactly what actions you can take right now.

Credit: www.jacc.org
Causes Of High Pip On Ventilator
High peak inspiratory pressure (PIP) on a ventilator signals that your patient’s lungs or airways are facing resistance. Understanding the root causes can help you act quickly to protect lung tissue and improve ventilation efficiency. Let’s look at the common factors that push PIP higher than desired and what you can do about them.
Airway Obstruction
Airway obstruction is a frequent cause of elevated PIP. It can occur due to kinked endotracheal tubes, biting, or external compression. Even subtle blockages can make your ventilator work harder, raising pressure.
Have you checked the tube position and patency lately? Removing obstructions or repositioning the tube often lowers PIP immediately.
Reduced Lung Compliance
When lung tissue becomes stiff or less elastic, the ventilator faces difficulty inflating the lungs. Conditions like pulmonary edema, fibrosis, or acute respiratory distress syndrome (ARDS) reduce compliance and spike PIP.
Consider whether your patient’s lung condition has changed recently. Adjusting ventilator settings to accommodate reduced compliance can ease the pressure burden.
Patient-ventilator Asynchrony
When your patient’s breathing efforts don’t match the ventilator cycle, pressures can surge unexpectedly. Asynchrony might result from improper sedation levels or incorrect trigger sensitivity.
Are you monitoring waveforms closely? Tweaking settings or sedating appropriately can synchronize breaths and prevent high PIP.
Excessive Secretions
Thick or abundant secretions clog the airways and increase resistance, pushing PIP higher. This is common in patients with infections or inadequate humidification.
Regular suctioning and humidifier checks can keep secretions in check. Don’t overlook this simple step—it often leads to quick PIP improvement.

Credit: www.respiratorytherapyzone.com
Monitoring Pip Levels
Monitoring Pip Levels involves closely observing the pressure levels on a ventilator to ensure patient safety. To decrease pip on ventilator, clinicians must carefully assess and adjust the pressure settings to meet individual patient needs. Proper monitoring helps prevent complications and ensures optimal respiratory support.
Monitoring Pip Levels is crucial in ventilator management. Keeping Pip (Peak Inspiratory Pressure) within safe limits ensures effective ventilation. It helps prevent lung injury and other complications. Regularly checking Pip levels can optimize patient outcomes.Regular Ventilator Checks
Regular checks are essential for maintaining ventilator performance. Schedule routine inspections to identify potential issues early. Check the ventilator settings and compare them with prescribed parameters. Ensure all components function properly to avoid unexpected faults. Document all findings for accurate records and future reference.Using Alarms Effectively
Alarms alert caregivers to changes in Pip levels. Set alarms to the appropriate thresholds for timely interventions. Respond to alarms immediately to prevent patient distress. Regularly test alarm systems to confirm they work correctly. Adjust alarm settings based on individual patient needs.Interpreting Pressure Waveforms
Pressure waveforms provide insight into ventilator function. Learn to read these waveforms to identify abnormalities. Analyze the waveform patterns for signs of increased Pip. Use waveform data to adjust ventilator settings accordingly. Understanding waveforms enhances decision-making and patient care.Adjusting Ventilator Settings
Adjusting ventilator settings can effectively reduce peak inspiratory pressure (PIP). Small changes in settings impact patient comfort and lung safety. Careful adjustments help avoid lung injury and improve ventilation efficiency.
Reducing Tidal Volume
Lowering tidal volume decreases the amount of air delivered with each breath. This reduces lung stretch and pressure inside the airways. Start with a modest decrease and monitor patient response closely. Aim for lung-protective volumes, usually around 6-8 mL/kg of ideal body weight.
Modifying Inspiratory Flow
Slowing the inspiratory flow rate can lower PIP by reducing resistance. A slower flow allows air to enter lungs gently, preventing sudden pressure spikes. Adjust the flow pattern from square to decelerating if possible. Observe the patient’s comfort and oxygenation during changes.
Optimizing Peep Levels
Positive end-expiratory pressure (PEEP) helps keep airways open but can increase PIP if set too high. Lower PEEP carefully to balance oxygenation and pressure. Use the minimal PEEP that maintains lung recruitment. Regular reassessment is vital to avoid lung collapse or overdistension.
Changing Ventilation Modes
Switching ventilation modes may reduce PIP by altering breath delivery. Pressure-controlled modes limit peak pressure directly, which can protect the lungs. Volume-controlled modes ensure a set tidal volume but may increase PIP if resistance rises. Choose a mode that fits the patient’s condition and goals.
Managing Airway Issues
Managing airway issues is a key part of decreasing Peak Inspiratory Pressure (PIP) on a ventilator. If your patient’s airway isn’t clear or the tube isn’t positioned correctly, the ventilator has to work harder to deliver breaths. This extra effort increases PIP and can cause discomfort or even damage.
Suctioning Techniques
Proper suctioning removes mucus and secretions that block the airway. Use gentle, controlled suctioning to avoid irritating the airway lining, which can cause swelling and increase resistance.
Try limiting suction duration to 10-15 seconds and allow the patient to rest between attempts. You might be surprised how quickly airway resistance drops after effective suctioning.
Ensuring Proper Tube Placement
Incorrect tube placement often leads to increased PIP because of partial airway obstruction or kinking. Always check the tube position by verifying depth markings and listening for breath sounds on both sides of the chest.
Even slight tube movement can cause problems. If you notice rising PIP, consider rechecking the tube before adjusting ventilator settings.
Addressing Secretions
Thick, sticky secretions make it harder for air to flow freely, raising PIP. Hydration helps thin secretions, making suctioning easier and more effective.
Humidify the inspired air to prevent secretions from becoming dry and crusty. Have you noticed how small changes in airway moisture can dramatically ease breathing efforts?
Improving Lung Compliance
Improving lung compliance helps reduce Peak Inspiratory Pressure (PIP) on a ventilator. Better lung compliance means the lungs expand more easily. This lowers the pressure needed to deliver air. Focus on techniques that open airways and reduce stiffness. These strategies support better breathing with less force.
Positioning Strategies
Position affects lung expansion and oxygen flow. Changing the patient’s posture can improve lung compliance. Use these positioning tips:
- Place the patient in a semi-upright position to reduce pressure on the lungs.
- Use prone positioning to open collapsed lung areas.
- Adjust the head and neck to keep airways clear and open.
These simple changes help air move easier, lowering PIP.
Using Recruitment Maneuvers
Recruitment maneuvers open closed lung units. They improve lung volume and flexibility. This reduces lung stiffness and pressure. Common techniques include:
- Applying sustained positive airway pressure for a short time.
- Increasing PEEP temporarily to open alveoli.
These maneuvers help restore lung function and ease ventilation.
Administering Bronchodilators
Bronchodilators relax airway muscles. They widen air passages and ease airflow. This improves lung compliance and lowers PIP. Use bronchodilators carefully as directed by medical staff. Common options include:
- Inhaled beta-agonists like albuterol.
- Anticholinergic drugs to reduce airway constriction.
These medications help reduce airway resistance and improve breathing.
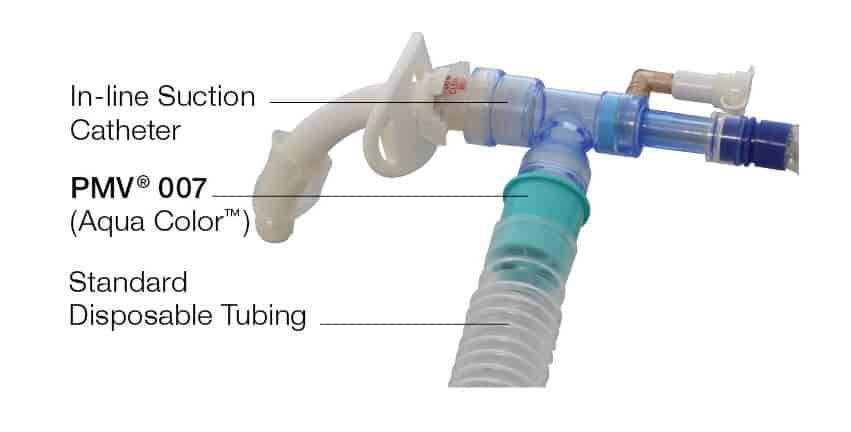
Credit: tracheostomyeducation.com
Enhancing Patient Comfort
Enhancing patient comfort is a crucial step in decreasing Peak Inspiratory Pressure (PIP) on a ventilator. When patients feel more at ease, their breathing synchronizes better with the machine, which can lower the pressure needed to support their lungs. Comfort isn’t just about kindness—it directly impacts the effectiveness of ventilation and overall recovery.
Sedation Management
Proper sedation helps patients relax without over-suppressing their respiratory drive. Too much sedation can weaken breathing muscles, while too little can cause agitation and breath fighting.
Adjust sedation levels carefully by observing your patient’s response. Use medications that provide calmness yet allow spontaneous breathing efforts. Have you noticed how subtle changes in sedation can improve ventilator synchrony?
Synchronizing Ventilator Support
Matching the ventilator’s timing with the patient’s natural breaths reduces discomfort and lowers PIP. Pay attention to trigger sensitivity and flow settings to avoid delays or excessive pressure.
Try adjusting the inspiratory time or switching to modes like pressure support that encourage patient participation. When the ventilator “follows” your patient’s lead, you’ll see smoother breaths and reduced pressure spikes.
Addressing Anxiety And Pain
Anxiety and pain raise respiratory rates and muscle tension, driving up PIP. Managing these symptoms can make a big difference in reducing pressure.
Use non-pharmacologic methods like gentle reassurance and controlled breathing exercises alongside pain medications. Have you found that even small comfort measures change how a patient breathes on the ventilator?
Preventive Measures
Preventive measures help reduce the peak inspiratory pressure (PIP) on ventilators. Lowering PIP protects the lungs and improves patient comfort. Taking steps before problems arise ensures safer ventilation and fewer complications.
Regular Equipment Maintenance
Check ventilator parts often for wear or damage. Clean filters and tubing regularly to avoid blockages. Replace faulty valves and sensors immediately. Proper equipment function keeps pressure stable and prevents sudden rises in PIP.
Staff Training
Train staff to recognize signs of high PIP early. Teach proper ventilator settings and adjustments. Practice quick response to alarms and patient distress. Skilled teams act fast to keep ventilation safe and effective.
Early Detection Of Complications
Monitor patients closely for changes in breathing or lung sounds. Use tools like capnography and pulse oximetry to spot issues early. Detecting problems early allows timely intervention. This prevents PIP from increasing and causing harm.
Frequently Asked Questions
What Is Pip On A Ventilator?
PIP stands for Peak Inspiratory Pressure. It indicates the highest pressure applied to the lungs during inhalation on a ventilator. Monitoring PIP helps prevent lung injury and ensures effective ventilation.
How Can I Safely Decrease Pip On A Ventilator?
You can decrease PIP by adjusting tidal volume, reducing inspiratory flow, or increasing expiratory time. Always consult clinical guidelines and monitor patient response carefully.
Why Is Lowering Pip Important For Patients?
Lowering PIP reduces the risk of lung barotrauma and volutrauma. It helps protect delicate lung tissues and improves patient comfort during mechanical ventilation.
Can Ventilator Settings Affect Pip Levels?
Yes, settings like tidal volume, respiratory rate, and inspiratory flow directly impact PIP. Properly tuning these helps manage and decrease high PIP values effectively.
Conclusion
Controlling peak inspiratory pressure helps protect the lungs during ventilation. Adjust ventilator settings carefully and watch the patient’s response. Use lower tidal volumes and proper PEEP levels. Always check for leaks or blockages in the circuit. Regular monitoring keeps pressure within safe limits.
Small changes can make a big difference in care. Stay attentive and act quickly to avoid complications. This approach supports better breathing and patient comfort. Remember, safety comes first with every adjustment made.





