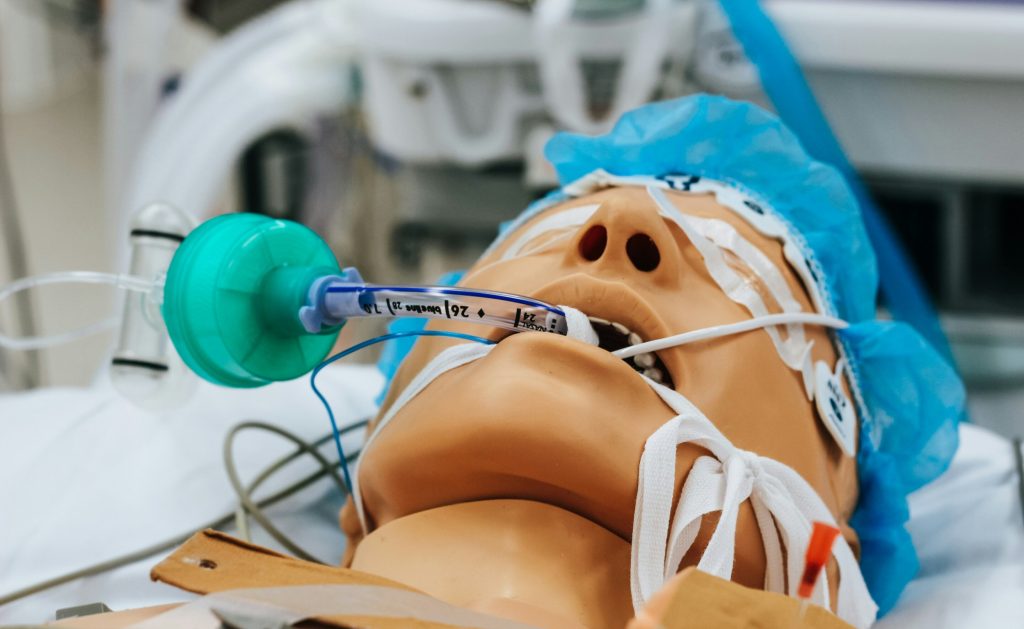
If you or a loved one ever face the need for a ventilator, you probably wonder: how long can someone stay on one? This question is natural and important because it touches on health, recovery, and hope.
Understanding the time frame helps you prepare emotionally and make informed decisions. You will discover the factors that affect ventilator use, what to expect during the process, and how medical teams work to support patients like you or your family member.
Keep reading to get clear answers that can ease your mind and guide you through this challenging time.
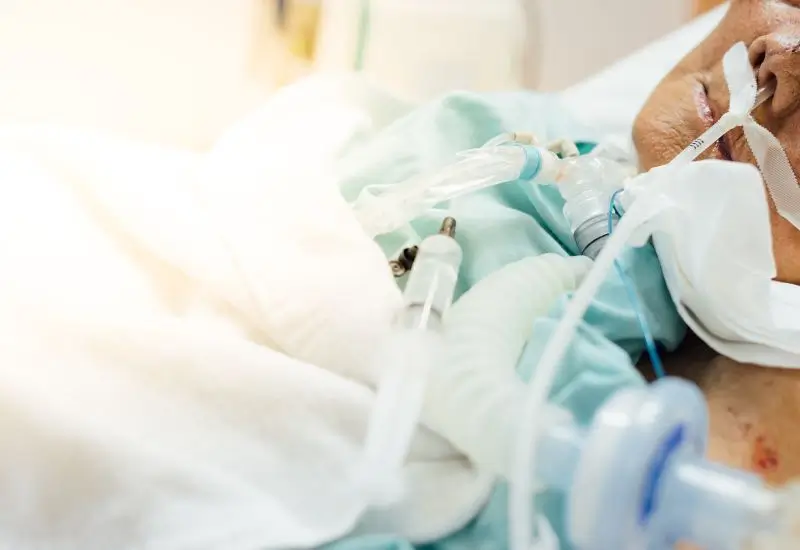
Credit: www.agapehospicepc.org
Ventilator Basics
Understanding ventilator basics helps patients and families grasp critical care better. Ventilators support breathing when lungs cannot work well. They push air into the lungs and help remove carbon dioxide. This support can last hours, days, or even weeks, depending on the illness.
Types Of Ventilators
- Invasive Ventilators:Use a tube inserted into the windpipe.
- Non-invasive Ventilators:Use masks to support breathing without tubes.
- Portable Ventilators:Small machines for use outside hospitals or during transport.
When Ventilation Is Needed
- Severe lung infections like pneumonia.
- Serious injuries affecting breathing muscles.
- During surgery under general anesthesia.
- Chronic lung diseases in critical stages.
- Conditions causing respiratory failure.
Ventilator Settings Explained
| Setting | What It Does |
|---|---|
| Respiratory Rate | Controls breaths per minute delivered by the ventilator. |
| Tidal Volume | Amount of air given with each breath. |
| Oxygen Concentration (FiO2) | Percentage of oxygen in the air delivered. |
| PEEP (Positive End-Expiratory Pressure) | Keeps lungs open by maintaining pressure after exhaling. |
Duration Factors
The time a patient spends on a ventilator varies greatly. Many factors affect this duration. Understanding these helps families and caregivers prepare for what lies ahead.
Each patient’s situation is unique. The body’s response to ventilation depends on health and other variables. Doctors consider these carefully before making decisions.
Patient Health Conditions
Pre-existing illnesses influence how long ventilation lasts. Lung diseases, heart problems, or infections can slow recovery. Severe conditions often require longer support from the ventilator.
Patients with weak immune systems face higher risks. Their bodies struggle to heal, which extends ventilation time. Chronic illnesses may cause complications during treatment.
Age And Recovery Ability
Age plays a crucial role in healing speed. Younger patients usually recover faster than older ones. Children and adults tend to have stronger lung function.
Older adults may take longer to wean off the ventilator. Aging weakens muscles and reduces lung capacity. This slows the process of regaining independent breathing.
Complications During Ventilation
Problems during ventilation can prolong its use. Infections like pneumonia can develop in the lungs. This delays recovery and requires more care.
Other issues include lung injury or difficulty clearing secretions. These complications make it harder to remove the ventilator. Care teams monitor closely to manage risks.
Short-term Ventilation
Short-term ventilation supports patients who need help breathing for a brief period. It assists the lungs while the body recovers from illness or surgery. This type of ventilation usually lasts from a few hours to several days. Medical teams watch patients closely during this time to ensure safe breathing and recovery.
Typical Time Frames
Short-term ventilation often lasts less than two weeks. Many patients use a ventilator for just a few hours or days. Some cases require support for up to seven days. The goal is to remove the ventilator as soon as breathing improves. Quick recovery helps reduce risks linked to longer use.
Common Causes For Brief Use
- Surgery requiring anesthesia
- Severe pneumonia or lung infection
- Acute asthma attacks
- Trauma or injury affecting breathing
- Temporary respiratory failure
Doctors choose short-term ventilation to stabilize breathing. It helps patients regain normal lung function fast.
Risks And Management
Even short ventilation carries risks. These include lung injury and infections. Doctors prevent problems by monitoring oxygen levels and lung pressure. They also use sterile techniques to avoid infections. Regular assessments help decide the right time to stop ventilation.
Long-term Ventilation
Long-term ventilation refers to the use of mechanical breathing support over an extended period, often weeks, months, or even years. This approach helps patients who cannot breathe adequately on their own due to various medical conditions. Understanding how long a patient can remain on a ventilator involves considering the reasons for ventilation, the patient’s health status, and the impact on their daily life.
Extended Use Scenarios
Some patients require ventilators for longer than the typical ICU stay. These scenarios include recovery from severe respiratory failure, prolonged coma, or complex surgeries where breathing muscles need time to regain strength.
In some cases, patients may transition from hospital ventilators to home-based systems. This switch allows them to live outside the hospital but still receive necessary respiratory support.
Have you ever wondered how families manage the emotional and physical demands when a loved one needs long-term ventilation?
Chronic Conditions Requiring Support
Certain chronic illnesses often lead to long-term ventilator use. These include conditions like chronic obstructive pulmonary disease (COPD), muscular dystrophy, and spinal cord injuries.
Patients with neuromuscular diseases may lose the ability to breathe independently over time. Mechanical ventilation becomes a critical part of their daily care.
Recognizing these conditions early can help patients and caregivers prepare for the challenges of long-term respiratory support.
Impact On Quality Of Life
Living on a ventilator changes many aspects of daily life. It can limit mobility, affect communication, and require constant medical attention.
However, many patients find ways to adapt and maintain meaningful social interactions and activities. Support from healthcare teams and family plays a crucial role in this adjustment.
What strategies would you consider to improve quality of life if you or a loved one needed long-term ventilation?
Weaning Off The Ventilator
Patients can stay on a ventilator from a few days to several weeks, depending on their condition. Doctors carefully watch progress to decide the best time to start weaning off the ventilator. Gradual reduction helps the patient breathe independently and safely.
Weaning off a ventilator is a crucial phase in a patient’s recovery. It involves gradually reducing dependence on the machine. This process helps the patient breathe independently. Weaning should be done carefully to ensure the patient’s safety. It requires a detailed assessment of the patient’s readiness.Signs Of Readiness
Certain signs indicate a patient is ready to wean. Stable vital signs are essential. The patient should have adequate oxygen levels. They should also show improved lung function. Mental alertness is another key indicator. The patient must be able to follow simple instructions.Weaning Methods
Various methods exist for weaning off ventilators. Spontaneous breathing trials are common. These trials test the patient’s ability to breathe on their own. Another method is pressure support ventilation. It reduces the machine’s assistance gradually. Intermittent mandatory ventilation is also used. It combines spontaneous breathing with machine assistance.Challenges In Weaning
Weaning can present several challenges. Some patients may experience anxiety. Others might have weak respiratory muscles. Medical conditions can also complicate the process. Close monitoring is essential to address these issues. Adjustments might be needed for a successful wean.
Credit: www.youtube.com
Complications And Risks
Spending time on a ventilator is a critical step in recovery for many patients, but it also comes with its own set of complications and risks. Understanding these challenges can help you better prepare for what lies ahead and participate actively in care decisions. Let’s look closely at some of the most common issues that can arise during prolonged ventilator use.
Ventilator-associated Pneumonia
Ventilator-Associated Pneumonia (VAP) is a serious infection that occurs in the lungs after a patient has been on a ventilator for a certain period. Bacteria can enter the airway through the breathing tube, leading to inflammation and infection.
This condition can worsen recovery times and increase the risk of further complications. You can reduce the risk by ensuring strict hygiene practices and regular monitoring by healthcare providers. Asking your care team about measures like oral care protocols can make a real difference.
Muscle Weakness
Being on a ventilator for a long time often leads to muscle weakness, especially in the respiratory muscles. The ventilator does much of the breathing work, which can cause your body to lose strength and endurance.
This weakness may extend beyond the lungs, affecting your arms and legs, making rehabilitation a longer journey. Early physical therapy and gradual weaning from the ventilator can help you regain strength faster. Have you discussed a physical therapy plan with your doctors yet?
Psychological Effects
The experience of being on a ventilator can be frightening and stressful. Many patients report feelings of anxiety, confusion, or even post-traumatic stress after their time on mechanical ventilation.
These psychological effects can impact your overall recovery and quality of life. Open communication with your healthcare team and access to counseling or support groups can provide valuable help. How do you think emotional support could change your recovery experience?
Care And Monitoring
The care and monitoring of a patient on a ventilator are crucial. This process ensures the patient’s safety and supports recovery. It involves a dedicated healthcare team, regular monitoring, and communication with families. Each plays a vital role in managing the patient’s condition effectively.
Role Of Healthcare Team
The healthcare team includes doctors, nurses, and respiratory therapists. They work together to provide comprehensive care. Each team member has specific duties. Doctors oversee the treatment plan. Nurses monitor vital signs and administer medications. Respiratory therapists manage the ventilator settings. Their collaboration ensures optimal patient outcomes.
Patient Monitoring Techniques
Monitoring techniques help track a patient’s progress. These include checking vital signs and blood tests. Nurses often use machines to monitor heart rate and oxygen levels. Regular assessments help detect changes in the patient’s condition. Adjustments to care are made based on these findings. Consistent monitoring is essential for timely interventions.
Family Support And Communication
Family support is important for patient morale. Families often feel anxious about their loved one’s condition. Regular updates from the healthcare team help ease their concerns. Clear communication ensures families understand the treatment plan. It also allows them to ask questions and voice concerns. This support network plays a key role in the patient’s recovery journey.
Technological Advances
Technological advances have changed how patients use ventilators. These improvements help patients stay on ventilators longer with more comfort and fewer risks. They also help doctors provide better care. Technology continues to evolve, making respiratory support safer and more effective.
Improved Ventilator Designs
Modern ventilators are smaller and more portable. They use smarter sensors to adjust airflow automatically. This reduces patient discomfort and lowers lung injury risks. New designs also include better alarms and monitoring systems. They alert caregivers quickly about any issues. These features help patients receive timely and precise care.
Non-invasive Ventilation Options
Non-invasive ventilation uses masks or nasal devices instead of tubes. This method lowers infection risks and improves patient comfort. It suits patients needing breathing help without full intubation. Non-invasive options help some patients avoid long-term ventilator use. They offer a gentler way to support breathing.
Future Trends In Respiratory Support
Future trends focus on AI and machine learning integration. These technologies aim to predict patient needs and adjust settings faster. Researchers also explore wearable ventilators for more mobility. New materials will make devices lighter and more flexible. These trends promise better outcomes and easier long-term ventilation.

Credit: www.news18.com
Frequently Asked Questions
How Long Can A Patient Stay On A Ventilator?
Patients can remain on a ventilator from a few days to several weeks. The duration depends on illness severity and recovery speed. Doctors closely monitor progress to decide when to wean off ventilation safely.
What Factors Affect Ventilator Duration For Patients?
Ventilator time varies due to lung health, infection type, and patient age. Chronic diseases and complications can extend ventilation needs. Individual responses to treatment also influence how long a patient requires support.
Can Long-term Ventilation Cause Complications?
Yes, prolonged ventilation may lead to infections, lung damage, or muscle weakness. Proper care and regular assessment help minimize these risks. Early intervention can improve outcomes and reduce ventilation time.
How Do Doctors Decide When To Remove A Ventilator?
Doctors assess breathing strength, oxygen levels, and overall health. They perform weaning trials to test if patients can breathe independently. The decision balances safety with the goal of reducing ventilator dependency.
Conclusion
Ventilator use varies for each patient and depends on many factors. Doctors watch patients closely to decide when to reduce support. Some people need a few days, others may need weeks. Recovery speed depends on illness, age, and overall health.
The goal always remains to help patients breathe on their own. Families should stay informed and ask questions during care. Patience and good medical care improve chances of success. Every case is different, and care teams adjust as needed.