If you or a loved one ever face a serious health challenge, you might wonder: how long can you stay on a vent? This question is more than just medical—it’s about hope, recovery, and understanding what comes next.
Knowing the answer can help you prepare mentally and emotionally. You’ll discover the facts, what affects the time on a ventilator, and what it means for your future. Keep reading to get clear, honest information that can make a real difference for you and those you care about.
Ventilator Basics
Ventilator use duration varies depending on health and recovery. Some patients need support for days, others for weeks or longer. Doctors monitor progress to decide when to reduce or stop ventilation.
Ventilator Basics Understanding how a ventilator works can be crucial, especially if you or a loved one may need one. Ventilators are life-saving machines that assist in breathing when the body cannot do so on its own. They are often the difference between life and death in critical care settings.What Is A Ventilator?
A ventilator is a machine designed to support or take over the breathing process. It works by delivering air into the lungs through a tube inserted into the windpipe. This allows oxygen to be delivered to the body while removing carbon dioxide. Ventilators can be used in hospitals, and sometimes at home, depending on the patient’s condition. They are crucial in treating patients with severe respiratory issues.When Is Ventilation Needed?
Ventilation becomes necessary when a person cannot breathe adequately on their own. This can occur due to various reasons such as severe pneumonia, chronic obstructive pulmonary disease (COPD), or during surgery when general anesthesia is required. Imagine a scenario where someone has a severe lung infection and struggles to breathe. The ventilator steps in to provide the necessary oxygen, buying time for the body to heal. Have you ever wondered how long one might need to rely on a ventilator? It’s a common question, and the answer varies based on the individual’s condition and response to treatment. Understanding these basics is the first step in navigating such challenging situations.Duration On A Ventilator
Duration on a ventilator varies widely depending on the patient’s condition. Ventilators help patients breathe when they cannot do so alone. Some patients need support for a short time, while others require longer assistance. Understanding typical timeframes and factors influencing stay helps families and caregivers prepare.
Typical Timeframes
Most patients stay on a ventilator for a few days to two weeks. Short-term ventilation usually lasts less than 48 hours. Long-term ventilation can extend for weeks or months. Some patients recover quickly and are taken off the ventilator within days.
Others with serious lung or brain problems may need weeks of support. Prolonged use increases the risk of infections and other complications. Doctors monitor progress daily to decide when to remove the ventilator.
Factors Influencing Length Of Stay
- Severity of illness or injury
- Age and overall health of the patient
- Type of lung or breathing problem
- Response to treatments and medications
- Presence of other medical conditions
- Complications during ventilation, such as infections
Each patient’s needs differ, so doctors tailor care accordingly. Some recover fast; others need extended support. Family involvement and clear communication with medical staff can ease the process.
Risks Of Prolonged Ventilation
Spending an extended time on a ventilator can save lives, but it also comes with serious risks. The longer you stay on mechanical ventilation, the higher the chance of facing complications that affect both your body and mind. Understanding these risks helps you or your loved ones prepare for what lies ahead and discuss care options with medical professionals.
Physical Complications
Prolonged ventilation can cause muscle weakness, especially in the diaphragm, which is critical for breathing. This weakness makes it harder to breathe independently once the ventilator is removed.
Other physical issues include lung infections like pneumonia, since the breathing tube bypasses natural defenses in your airway. Skin breakdown or pressure sores may also develop from lying in one position too long.
- Increased risk of blood clots due to immobility
- Damage to vocal cords from the breathing tube
- Lung injury from high oxygen levels or pressure settings
Have you ever thought about how your body reacts to being inactive for long periods? This can be a critical part of recovery discussions.
Psychological Effects
Being on a ventilator often means sedation or restricted communication, which can lead to anxiety and confusion. Many patients experience ICU delirium, a state of severe disorientation and hallucinations.
Long-term mental health effects might include depression or post-traumatic stress disorder (PTSD). These conditions sometimes persist even after physical recovery.
Family members and caregivers also face emotional stress during this time. Recognizing these psychological impacts early can improve support strategies for everyone involved.

Credit: www.goodrx.com
Weaning Off The Vent
Weaning off a ventilator is a crucial step in recovery for anyone who has been dependent on mechanical breathing support. It involves gradually reducing the ventilator’s assistance while ensuring your lungs and muscles can handle breathing on their own. This process requires careful monitoring and patience, as rushing can lead to setbacks or complications.
Signs Of Readiness
Recognizing when you are ready to start weaning is key to a successful transition. Your healthcare team will look for signs such as stable oxygen levels and improved lung function. You might notice you can breathe more easily without heavy support, and your overall strength and alertness will improve.
Have you felt moments when taking a breath feels less forced or tiring? That’s a good indicator your body might be ready to try breathing with less help. Other signs include a steady heart rate and the absence of infections or other complications.
Weaning Methods
Several methods help you come off the ventilator safely. One common approach is called “spontaneous breathing trials,” where you breathe on your own for short periods while being closely watched. This helps doctors see how your lungs cope without full ventilator support.
Another method uses gradual pressure reduction, where the ventilator slowly decreases the assistance it provides over time. You might experience periods where the machine supports you less, allowing your respiratory muscles to strengthen.
- Pressure support ventilation: The ventilator helps only when you initiate a breath.
- CPAP (Continuous Positive Airway Pressure): Keeps your airways open while you breathe spontaneously.
- SIMV (Synchronized Intermittent Mandatory Ventilation): Combines machine breaths with spontaneous breaths.
Each method has its advantages, and your care team will choose the best fit based on how you respond. The key is to progress at a pace that feels manageable and safe for you, avoiding stress on your lungs and body.
Long-term Ventilation
Long-term ventilation is a critical aspect for individuals who require respiratory support beyond the acute phase of illness. It involves the use of mechanical ventilators for extended periods, sometimes lasting months or even years. Understanding how long you can stay on a ventilator depends on various factors including your health condition, environment, and personal goals.
Home Ventilator Use
Using a ventilator at home allows many patients to regain a sense of normalcy. Home ventilators are designed to be portable and user-friendly, enabling patients to live outside hospital walls.
Families often receive training to manage the equipment safely. This can include tasks like adjusting settings, performing basic maintenance, and recognizing warning signs. The ability to stay on a ventilator at home greatly depends on the availability of support and proper care.
Have you thought about what resources you might need if you or a loved one were to transition to home ventilation?
Quality Of Life Considerations
Long-term ventilation can affect your daily life in many ways. It might limit mobility or change how you communicate, but it can also extend your time with loved ones and allow participation in activities you enjoy.
Each person’s experience is unique, and it’s important to weigh the benefits against the challenges. For example, some patients find comfort in knowing that ventilation supports their breathing, while others struggle with the dependence it creates.
Discussing your goals with healthcare providers can help tailor a ventilation plan that respects your quality of life. What matters most to you when living with a ventilator?
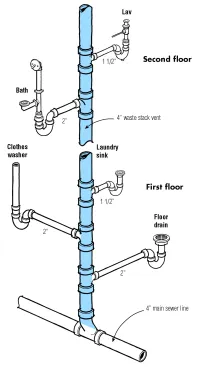
Credit: www.jlconline.com
Support For Patients And Families
Being on a ventilator can be a challenging experience for both patients and their families. Support plays a vital role in helping everyone cope with the physical and emotional demands. Understanding the available help can ease stress and provide comfort during this time.
Emotional Support
Patients on a ventilator often face fear and uncertainty. Families may feel overwhelmed and anxious. Emotional support helps manage these feelings. Counseling and support groups offer a safe space to share worries. Talking openly reduces isolation and builds strength.
Simple acts like listening and showing empathy make a big difference. Staying connected with loved ones boosts morale. Encouragement and patience help patients and families face daily challenges.
Resources And Care Teams
Hospitals have skilled care teams dedicated to ventilated patients. These teams include doctors, nurses, respiratory therapists, and social workers. They monitor health, adjust treatments, and provide guidance.
Families can ask questions and learn about care plans. Educational materials explain ventilator use and patient needs. Resources may include:
- Patient and family education programs
- Home care support options
- Financial and legal advice
- Community support services
Access to these resources helps families prepare and feel more confident. Team collaboration improves patient outcomes and family well-being.

Credit: www.goodrx.com
Frequently Asked Questions
How Long Can A Patient Safely Stay On A Ventilator?
The duration varies based on illness severity and patient condition. Some stay for days, others for weeks. Doctors monitor closely to prevent complications and decide the best time to wean off.
What Factors Determine Ventilator Duration For Patients?
Patient’s underlying health, lung function, and response to treatment affect ventilator time. Complications like infections can prolong use. Doctors assess daily to adjust support and plan removal.
Can Long-term Ventilation Cause Health Problems?
Yes, prolonged ventilation may lead to lung damage, infections, or muscle weakness. Regular monitoring and care minimize risks. Early weaning is preferred when the patient is stable.
How Do Doctors Decide When To Remove Ventilation?
Doctors evaluate breathing strength, oxygen levels, and overall recovery. They perform tests to ensure patients can breathe independently. A gradual reduction in support often precedes removal.
Conclusion
Time on a ventilator varies for each person’s health needs. Some may need support for days, others for weeks. Doctors watch closely to decide the right time to stop. Staying on a vent too long can cause problems. But it also gives the body time to heal.
Families and patients should ask questions and stay informed. Understanding this helps reduce fear and stress. Every case is unique, and care plans change often. Support and patience matter most during this time.