If you or a loved one ever faces a stay in the ICU, the thought of being on a ventilator can feel overwhelming. You might wonder, “How long can you stay on a ventilator in the ICU?” This question is natural and important because the length of time on a ventilator affects recovery and overall health.
Understanding what to expect can ease your fears and help you make informed decisions. You’ll discover the factors that influence ventilator use, what the timeline might look like, and what it means for you or your loved one’s journey to recovery.
Keep reading to find answers that can bring clarity during a challenging time.

Credit: www.apexhospitals.com
Ventilator Basics
Understanding ventilators helps you grasp how they support patients in the ICU. Ventilators assist breathing when patients cannot breathe well on their own. They deliver oxygen and remove carbon dioxide from the lungs. This support can be lifesaving during serious illnesses or injuries.
Purpose And Function
Ventilators help patients who struggle to breathe. They take over the work of breathing by pushing air into the lungs. The machine controls the amount and pressure of air delivered. It also ensures the right balance of oxygen and carbon dioxide. This support allows the lungs to rest and heal.
Doctors adjust ventilator settings based on the patient’s needs. The goal is to provide enough oxygen while minimizing lung damage. Ventilators also help remove carbon dioxide from the body efficiently. They can be used short-term or for longer periods.
Types Of Ventilators
There are several types of ventilators used in the ICU:
- Invasive Ventilators:These use a tube inserted into the windpipe. They provide strong, controlled breathing support.
- Non-invasive Ventilators:These use masks to support breathing without tubes. They are less invasive but offer less control.
- Portable Ventilators:Small machines used during patient transport or at home.
Each type has specific uses based on the patient’s condition. The ICU team selects the best option to support recovery safely.
Factors Influencing Ventilator Duration
Several factors determine how long a patient stays on a ventilator in the ICU. These factors influence the recovery process and the ability to breathe independently. Understanding them helps families and caregivers prepare for what lies ahead.
Patient’s Medical Condition
The underlying illness plays a major role in ventilator duration. Patients with severe lung diseases or infections may need longer support. Trauma or surgery affecting breathing can also extend the time. Some conditions improve quickly, while others take weeks or months.
Age And Overall Health
Older patients often take more time to recover. Their bodies are less resilient and heal slower. Good overall health may shorten ventilator use. Chronic diseases like diabetes or heart problems can delay recovery. Each patient’s unique health status affects the process.
Complications And Risks
Ventilator use carries risks that may prolong its duration. Infections, such as pneumonia, can develop during ventilation. Muscle weakness from long-term ventilation may slow weaning. Other complications include lung injury or airway problems. Careful monitoring helps manage these risks.
Typical Ventilation Timeframes
Understanding typical ventilation timeframes in the ICU is crucial for patients and families facing this challenging situation. Ventilation duration varies widely based on individual health conditions and recovery progress. Knowing what to expect can help you prepare mentally and ask informed questions.
Short-term Ventilation
Short-term ventilation usually lasts from a few hours up to several days. This period often applies to patients recovering from surgery or acute illnesses that impair breathing temporarily. The goal here is to support your lungs until you can breathe independently again.
During short-term ventilation, doctors monitor your progress closely. They look for signs that your lungs are healing and your breathing muscles are regaining strength. Have you ever wondered how quickly your body can bounce back with the right support?
Prolonged Ventilation
Prolonged ventilation extends beyond a week and can sometimes last several weeks or months. This happens when lung recovery is slow, or complications arise, such as infections or muscle weakness. Patients on prolonged ventilation often require more intensive care and specialized therapies.
Living on a ventilator for a long time can affect your overall health and well-being. Muscle loss and mental fatigue are common challenges that caregivers must address. Would you consider additional therapies to speed up recovery if given the chance?
When To Consider Weaning
Weaning from a ventilator starts once your lungs and muscles show improvement. Medical teams assess your ability to breathe on your own through tests and gradual reduction of ventilator support. This phase requires careful balance to avoid setbacks.
Successful weaning depends on many factors, including your strength, lung function, and overall health. Sometimes, the process takes several attempts before you can fully breathe independently. How confident do you feel about the steps needed to regain your natural breathing?
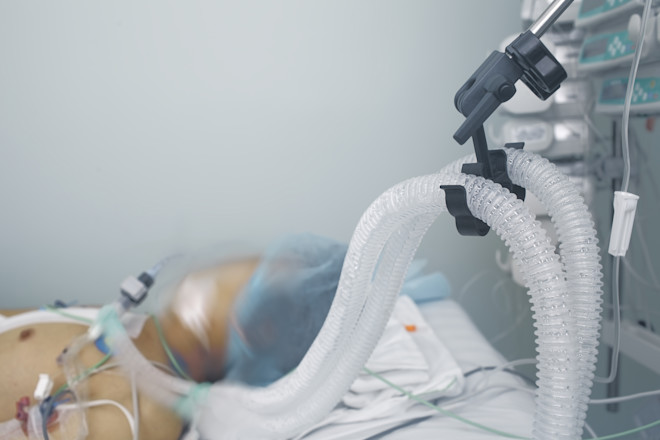
Credit: www.discovermagazine.com
Weaning From The Ventilator
Weaning from the ventilator is a crucial phase in the recovery process for patients in the ICU. It involves gradually reducing ventilator support as the patient’s lungs and muscles regain strength. This step requires careful monitoring and assessment to ensure safety and success.
Signs Of Readiness
How do you know when it’s time to start weaning? Medical teams look for several key signs that suggest you might be ready. These include stable breathing patterns, improved oxygen levels, and the ability to initiate breaths on your own.
Other signs include:
- Normal blood pressure without heavy medication
- Good mental alertness and ability to follow commands
- Minimal secretions and effective cough
Noticing these signs can feel like a breakthrough moment for both you and your caregivers. It signals that your body is ready to take on more work.
Weaning Methods
There are several approaches to weaning, each tailored to your condition and progress. One common method is the spontaneous breathing trial (SBT), where you breathe without assistance for a short time to test your readiness.
Another technique involves gradually decreasing ventilator support levels, allowing your respiratory muscles to strengthen bit by bit. Some patients benefit from pressure support ventilation, which helps reduce the work of breathing as you regain strength.
Choosing the right method depends on your overall health and how well you respond to trials. Your medical team will adjust the plan based on your daily progress.
Challenges During Weaning
Weaning is not always smooth. You might experience fatigue, anxiety, or trouble maintaining stable breathing. These challenges can slow down progress and require extra care.
Sometimes, underlying issues like infections or muscle weakness can make weaning harder. It’s important to communicate how you feel so the team can address these obstacles promptly.
Have you ever wondered how patience and persistence play a role in recovery? Staying positive and engaged in your care can make a big difference during tough moments.
Risks Of Extended Ventilation
Extended ventilation in ICU can lead to complications such as lung damage and infections. Staying on a ventilator too long might also cause muscle weakness. Monitoring and timely interventions are crucial to minimize these risks.
Extended use of a ventilator in the ICU can save lives, but it comes with its own set of risks. Understanding these risks is crucial, especially if you or a loved one is facing long-term ventilation. Prolonged mechanical ventilation can lead to complications that affect both physical and mental health.Infections And Pneumonia
Being on a ventilator for an extended period increases the likelihood of infections. The risk of developing pneumonia, especially ventilator-associated pneumonia (VAP), is significant. This is because the tube used for ventilation can bypass the body’s natural defenses against bacteria and viruses. Even with the best care, infections can occur, requiring additional treatments and extending ICU stays. Have you considered how these infections could affect recovery?Muscle Weakness
Long-term ventilation often leads to muscle weakness, a condition known as ICU-acquired weakness. This weakness can affect respiratory muscles, making it harder to wean off the ventilator. It can also impact overall mobility, prolonging rehabilitation efforts. Imagine the challenge of relearning to walk after weeks of immobility. Would you be prepared for the physical demands of recovery?Psychological Effects
Extended ventilation can also take a toll on mental health. Patients may experience confusion, anxiety, or even post-traumatic stress disorder (PTSD) due to the ICU environment and the effects of sedation. Being aware of these potential psychological impacts can help in preparing for a comprehensive recovery plan. How might these mental health challenges affect your return to daily life? Understanding these risks can empower you to make informed decisions and advocate for the best possible care. Each patient’s journey is unique, so it’s essential to discuss these aspects with healthcare providers.Supportive Care In Icu
Supportive care in the ICU is essential for patients on ventilators. It goes beyond just managing the breathing machine. The care team focuses on the whole person, ensuring that their body and mind stay as strong as possible during this challenging time.
Nutritional Support
Your body needs fuel to heal, especially when you’re on a ventilator. Nurses and dietitians work together to provide the right nutrients, often through feeding tubes if you can’t eat by mouth.
Proper nutrition helps prevent muscle loss and supports your immune system. Have you ever thought about how much energy your body uses just to breathe when you’re sick? That’s why calories and vitamins matter so much here.
Physical Therapy
Physical therapy isn’t just for after you leave the ICU. Therapists often start gentle exercises while you’re still on the ventilator.
These exercises can include moving your arms or legs to prevent stiffness and muscle wasting. Even small movements can make a big difference in how quickly you recover.
Imagine being able to sit up or take a few steps sooner—this can improve your lung function and boost your mood.
Emotional And Psychological Support
Being on a ventilator can feel isolating and frightening. ICU staff understand this and provide emotional support to you and your family.
Talking about your fears or having a counselor visit can reduce anxiety and confusion. Have you noticed how your mental state affects your physical healing? Emotional care is just as important as medical treatment.
Patient And Family Considerations
Being on a ventilator in the ICU is a tough experience for patients and their families. It brings many emotions and questions. Understanding what to expect helps families cope better. It also supports patients’ well-being during this critical time.
Families play a key role in care decisions and emotional support. Clear communication with doctors and nurses is very important. Preparing for life after the ICU starts early. This section covers important points for patients and families.
Communication With Medical Team
Talk openly with doctors and nurses about the patient’s condition. Ask simple questions about the ventilator and treatment plan. Request updates regularly to stay informed. Share concerns and preferences clearly. Good communication helps reduce anxiety and builds trust. It ensures everyone understands the care goals.
Decision-making And Consent
Families often face tough decisions about continuing ventilation. Doctors explain risks, benefits, and possible outcomes. Patients’ wishes and values guide these choices. Legal consent is needed for many treatments. Discuss advance directives or living wills if available. Support from social workers or counselors can help with decisions.
Preparing For Post-icu Recovery
Recovery after ventilation may take time and effort. Patients might need physical therapy and breathing exercises. Cognitive and emotional changes can occur. Families should learn about follow-up care and home support. Planning ahead makes the transition smoother. It helps patients regain strength and independence.
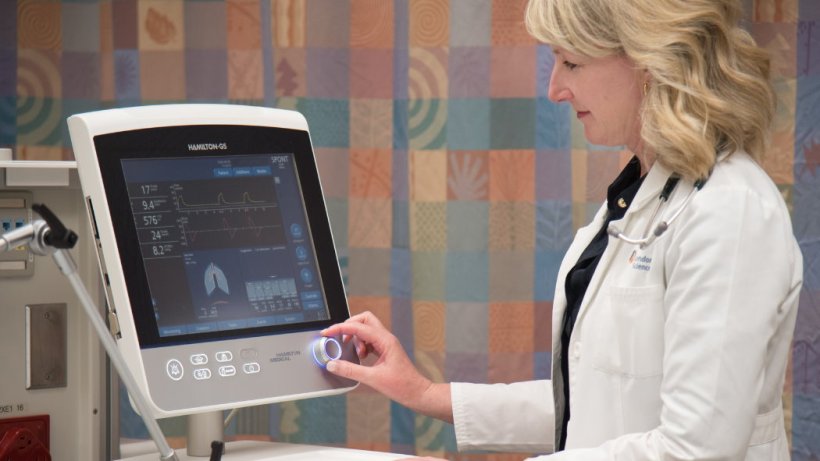
Credit: healthcare-in-europe.com
Frequently Asked Questions
How Long Do Patients Usually Stay On Ventilators In Icu?
Patients typically stay on ventilators in the ICU from a few days to several weeks. Duration depends on illness severity and recovery speed. Doctors monitor progress closely and aim to wean patients off ventilation as soon as it’s safe. Prolonged use increases risks like infections.
What Factors Influence Ventilator Duration In Icu Patients?
Ventilator duration depends on illness type, patient age, overall health, and lung function. Complications like infections or lung damage can extend use. Recovery pace and response to treatment also play key roles in determining how long ventilation support is needed.
Can Long-term Ventilator Use Cause Complications?
Yes, long-term ventilator use can lead to infections, lung injury, and muscle weakness. Prolonged ventilation increases the risk of pneumonia and other respiratory issues. Medical teams work to minimize these risks by monitoring and adjusting care regularly.
Is It Possible To Wean Off Ventilators Quickly?
Weaning speed varies based on patient condition and lung recovery. Some patients can be weaned off within days, while others require gradual reduction over weeks. Careful assessment and support are essential to ensure safe and effective ventilator removal.
Conclusion
Staying on a ventilator varies by patient needs and health. Doctors watch closely to decide when to reduce support. Some people recover quickly, while others need longer care. Risks increase the longer a ventilator is used. Family support and good medical care help during this time.
Understanding the process can ease worry and stress. Every case is different, and medical teams work hard daily. Patience and hope remain important throughout the recovery journey.





