Have you ever wondered how machines help people breathe when they can’t do it on their own? Assist Control Ventilation is a key lifesaving tool used in hospitals to support patients struggling to breathe.
Understanding what it is and how it works can give you peace of mind if you or a loved one ever face breathing difficulties. You’ll discover exactly what Assist Control Ventilation means, why it’s important, and how it impacts patient care.
Keep reading to learn how this technology could make a difference in critical moments.
Assist Control Ventilation Basics
Assist Control Ventilation (ACV) is a common mode used in mechanical ventilation. It helps patients breathe by supporting or taking over their breaths. This method ensures a steady flow of air into the lungs. It suits patients who cannot breathe fully on their own or need help with breathing effort.
ACV delivers breaths at a set rate and volume. It also allows patients to trigger extra breaths if they try to breathe. This flexibility makes it useful in many medical situations. Understanding its basics helps caregivers provide better care.
How It Works
Assist Control Ventilation works by setting a fixed number of breaths per minute. The ventilator gives a preset volume of air with each breath. If the patient tries to breathe faster, the machine assists by delivering the full breath. This support reduces the patient’s work of breathing. The ventilator senses the patient’s effort and responds quickly.
Primary Components
- Ventilator Machine:Controls breath rate and volume.
- Pressure Sensors:Detect patient’s breathing effort.
- Airway Tubing:Connects the ventilator to the patient.
- Humidifier:Adds moisture to the air to prevent dryness.
- Alarms:Alert caregivers to issues like high pressure or disconnection.
When It’s Used
Assist Control Ventilation (ACV) is a critical tool used in intensive care to support patients who cannot breathe adequately on their own. Knowing when to use this mode can make a significant difference in patient outcomes. It’s not just about mechanical support; it’s about matching the patient’s needs precisely and avoiding complications.
Common Medical Conditions
ACV is often chosen for patients facing severe respiratory challenges. Conditions like acute respiratory distress syndrome (ARDS), pneumonia, or chronic obstructive pulmonary disease (COPD) frequently require this support.
In these cases, the lungs struggle to maintain proper oxygen and carbon dioxide levels. ACV helps by ensuring each breath is delivered with consistent volume or pressure, reducing the work of breathing.
Have you ever considered how vital it is to maintain a steady breathing rhythm in these illnesses? ACV provides that rhythm when the body cannot.
Patient Scenarios
- Post-Surgery Recovery:Patients emerging from major surgeries, especially those involving the chest or abdomen, may need ACV to manage pain and ensure effective breathing while they regain strength.
- Neurological Impairments:If a patient has suffered a stroke or spinal cord injury affecting respiratory muscles, ACV steps in to control breathing mechanics.
- Severe Fatigue:Sometimes, patients with chronic illnesses reach a point where their respiratory muscles tire out completely. ACV can take over until they recover enough to breathe independently again.
Can you imagine the relief for patients whose bodies are too weak to maintain breathing on their own? ACV doesn’t just save lives; it buys time for healing.
Modes And Settings
Assist Control Ventilation (ACV) has different modes and settings. These allow doctors to adjust how the machine helps patients breathe. Choosing the right mode depends on the patient’s condition and needs. Each mode controls airflow and pressure differently to support breathing.
Volume Control Mode
In Volume Control Mode, the ventilator delivers a set amount of air with each breath. The volume stays the same, no matter how hard the patient tries to breathe. The machine controls the breathing rate and volume. It ensures the patient gets enough air every time.
This mode suits patients who need stable breathing support. Doctors set the tidal volume and breathing rate. The pressure may change depending on lung resistance and compliance.
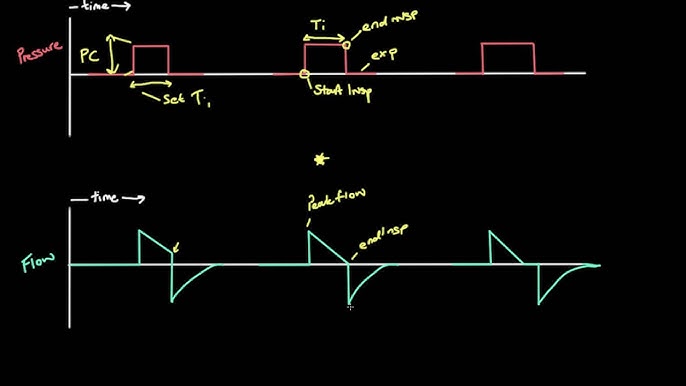
Pressure Control Mode
Pressure Control Mode focuses on keeping the airway pressure constant. The machine adjusts the volume to maintain this pressure. Breaths may vary in size based on the patient’s lung condition.
This mode helps protect the lungs from high pressure. It is useful for patients with weak or stiff lungs. Doctors set the pressure limit and the breathing rate. The ventilator changes the volume to keep pressure steady.

Credit: mfimedical.com
Benefits Of Assist Control Ventilation
Assist Control Ventilation (ACV) offers many benefits for patients needing breathing support. It ensures steady breathing and helps improve lung function. ACV adjusts to the patient’s breathing efforts and provides full support when needed. This balance helps patients get better oxygen levels and reduces the strain on their respiratory muscles. Understanding these benefits helps explain why ACV is widely used in critical care.
Improved Oxygenation
ACV helps increase the amount of oxygen in the blood. It delivers breaths at a set volume or pressure, ensuring lungs receive enough air. This steady airflow opens the air sacs, making oxygen exchange easier. Patients with low oxygen levels benefit from this controlled ventilation. It stabilizes oxygen supply, which supports vital organs and speeds recovery.
Reduced Work Of Breathing
ACV lowers the effort needed to breathe. The machine assists every breath the patient tries to take. This support lessens muscle fatigue and prevents breathing exhaustion. Patients can rest more and heal faster. By reducing the work of breathing, ACV improves comfort and reduces stress on the body.
Potential Risks And Complications
Assist Control Ventilation (ACV) is a common mode of mechanical ventilation used in medical settings to support patients who are unable to breathe adequately on their own. While it offers significant benefits, it’s essential to be aware of its potential risks and complications. Understanding these risks can help you and your healthcare team make informed decisions about its use.
Barotrauma
Barotrauma is a condition that can occur when the lungs are exposed to excessive pressure during mechanical ventilation. This can lead to lung injury, as the delicate tissues of the lungs are not equipped to handle high pressure. If you’ve ever tried inflating a balloon too quickly, you know it can burst; similarly, high ventilator pressures can damage lung tissues. Monitoring and adjusting ventilator settings can help minimize this risk.
Respiratory Alkalosis
Respiratory alkalosis is another potential complication where the blood becomes too alkaline due to over-ventilation. This occurs when the ventilator delivers too many breaths or the breaths are too deep, causing excessive carbon dioxide to be exhaled. This imbalance can lead to symptoms like dizziness, confusion, or even seizures. It’s crucial to work closely with healthcare providers to adjust the ventilator settings to match the patient’s specific needs.
Have you ever wondered how these risks might impact the recovery process? Understanding the balance between benefits and potential complications can empower you to have more informed discussions with your healthcare team. Always remember, your engagement and advocacy play a crucial role in your care.
Monitoring And Adjustments
Monitoring and adjusting Assist Control Ventilation (ACV) is crucial to ensure your patient receives the right support without causing discomfort or lung injury. You need to keep a close eye on several indicators that reveal how well the ventilation matches your patient’s breathing needs. These observations help you make timely tweaks to improve comfort and effectiveness.
Key Parameters To Watch
Start by tracking the patient’s respiratory rate and tidal volume. These show how often and how deeply the patient breathes, which is essential for adequate oxygen delivery.
Watch the peak inspiratory pressure closely. High pressures might signal stiff lungs or airway resistance, which could harm the patient if not addressed.
- Respiratory Rate (RR):Indicates breaths per minute—monitor for irregularities.
- Tidal Volume (VT):Measures air volume per breath—too high can cause lung injury.
- Peak Inspiratory Pressure (PIP):Alerts to airway resistance or lung compliance issues.
- Oxygen Saturation (SpO2):Reflects oxygen levels—critical to prevent hypoxia.
Have you noticed how small changes in these numbers can quickly affect your patient’s comfort? Keeping a detailed log helps you spot trends early.
Adjusting Settings For Patient Needs
Adjustments should always respond to what the patient’s body is telling you through the monitored parameters. If tidal volume is too low, raising it slightly can improve oxygenation but beware of causing lung strain.
Changing the respiratory rate can help if the patient is breathing too fast or too slow. For example, lowering the rate might reduce fatigue, while increasing it can support patients who struggle to maintain adequate ventilation.
Don’t forget to tailor the oxygen concentration to keep saturation in a safe range without exposing the patient to excessive oxygen, which can be harmful over time.
- Increase tidal volume carefully to enhance ventilation without overdistension.
- Modify respiratory rate based on patient effort and blood gas results.
- Adjust inspiratory flow rates to improve comfort and synchrony.
- Fine-tune oxygen levels to maintain target saturation.
Have you ever had to make quick adjustments during a critical moment? The key is understanding the balance between support and patient comfort to avoid unnecessary interventions.
Comparison With Other Ventilation Modes
Understanding how Assist Control Ventilation (ACV) differs from other ventilation modes helps in choosing the right support for patients. Each mode has unique features tailored to patient needs and lung conditions. The main differences lie in how breaths are delivered and controlled. This affects patient comfort and overall treatment effectiveness.
Simv Vs Assist Control
Synchronized Intermittent Mandatory Ventilation (SIMV) allows patients to breathe spontaneously between machine-delivered breaths. The ventilator gives a set number of mandatory breaths but lets the patient control additional breaths. This mode supports muscle activity and reduces ventilator dependence.
Assist Control delivers every breath either triggered by the patient or timed by the machine. Each breath has a fixed volume or pressure, ensuring consistent ventilation. Patients get full support, which helps those with weak breathing effort.
- SIMV:Patient controls some breaths, ventilator assists periodically.
- Assist Control:Ventilator controls all breaths, patient triggers or time triggers.
- Muscle use:SIMV encourages, Assist Control reduces effort.
- Use case:SIMV for weaning, Assist Control for full support.
Pressure Support Ventilation Differences
Pressure Support Ventilation (PSV) helps patients breathe by adding pressure during spontaneous breaths. It does not deliver mandatory breaths but assists the patient’s own effort. This mode improves comfort and reduces work of breathing.
Assist Control provides full ventilator-driven breaths with set volume or pressure. It does not rely on patient effort to start breaths, making it suitable for weak or sedated patients.
- PSV:Patient initiates all breaths, ventilator supports pressure.
- Assist Control:Ventilator initiates or assists every breath.
- Comfort:PSV feels more natural, Assist Control feels controlled.
- Application:PSV for spontaneous breathing, Assist Control for full ventilation.
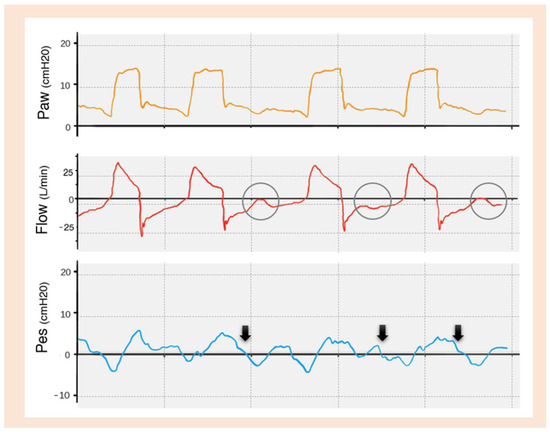
Credit: www.mdpi.com
Future Trends In Ventilation
Assist Control Ventilation helps patients breathe by supporting each breath with a set volume or pressure. This method ensures steady airflow, aiding those who struggle to breathe on their own. Future trends focus on improving comfort and adapting support to patient needs.
The future of ventilation is rapidly evolving, with exciting developments on the horizon. As technology continues to advance, assist control ventilation systems are expected to become more efficient and patient-focused. Let’s explore how these trends are set to transform the field of ventilation.Technological Advances
Technology is the driving force behind the next generation of ventilation systems. Smart sensors and AI algorithms are being integrated to provide real-time data analysis. This means ventilators can adjust settings automatically, optimizing patient care with minimal human intervention. Imagine a ventilator that learns and adapts to a patient’s unique breathing patterns. Such innovations can potentially reduce complications and improve outcomes. With every technological leap, the goal is to make ventilation more intuitive and less invasive.Personalized Ventilation Approaches
Personalization is key in the future of healthcare, and ventilation is no exception. Tailoring ventilation settings to individual patient needs can significantly enhance treatment effectiveness. New research is paving the way for ventilators that can be fine-tuned to match specific medical conditions and personal preferences. Have you ever wondered if a machine could understand your body’s unique needs? Personalized ventilation aims to do just that, ensuring each breath is as comfortable and efficient as possible. This approach not only improves patient comfort but also speeds up recovery times. As you consider these future trends, think about the impact they could have on patient care. How might these innovations change the way we approach respiratory support? The possibilities are both exciting and endless.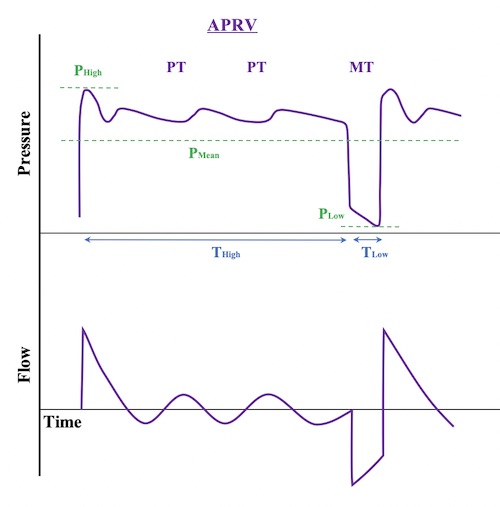
Credit: traumaicu.org
Frequently Asked Questions
What Is Assist Control Ventilation In Simple Terms?
Assist Control Ventilation is a mechanical breathing mode that supports patients’ breaths. It delivers a preset volume or pressure with each breath, whether patient-initiated or machine-triggered, ensuring consistent ventilation.
How Does Assist Control Ventilation Benefit Patients?
It provides full respiratory support, reducing work of breathing. This mode maintains stable oxygen and carbon dioxide levels, aiding recovery in critically ill patients.
When Is Assist Control Ventilation Typically Used?
It’s used for patients with respiratory failure, sedation, or muscle weakness. It ensures adequate ventilation when patients cannot breathe effectively on their own.
What Are The Risks Of Assist Control Ventilation?
Risks include over-ventilation, lung injury, and respiratory alkalosis. Proper monitoring is essential to adjust settings and prevent complications.
Conclusion
Assist Control Ventilation helps patients breathe with support from a machine. It delivers breaths at set times or when the patient tries to breathe. This method ensures steady oxygen flow and reduces breathing effort. Understanding its use can improve patient care and outcomes.
Always consult healthcare professionals for the best ventilation plan. Clear knowledge about Assist Control Ventilation aids in making informed decisions. It remains a vital tool in respiratory support and critical care.