If you or a loved one has experienced a stroke, you might be facing many tough questions. One of the most pressing concerns is often about breathing support—specifically, how long you might need to stay on a ventilator.
This period can feel uncertain and overwhelming, but understanding what influences the length of time on a ventilator can help you prepare and feel more in control. You’ll discover key factors that affect ventilator duration after a stroke and what to expect during recovery.
Keep reading to get clear, straightforward answers that matter to you.

Credit: www.lhscri.ca
Ventilator Use After Stroke
After a stroke, your breathing can be affected, sometimes making ventilator support necessary. Ventilators help ensure your body gets enough oxygen while your brain and lungs recover. Understanding why and how ventilators are used can help you navigate this challenging time more confidently.
Reasons For Ventilator Support
Your brain controls your breathing, and a stroke can disrupt this vital function. You might need a ventilator if your respiratory muscles are weak or if you’re unable to clear secretions from your airway effectively.
Sometimes, sedation or coma caused by the stroke requires a ventilator to maintain breathing. Ventilator support also protects you from complications like pneumonia, which can occur if you can’t breathe deeply or cough well.
Have you ever wondered why some stroke survivors need breathing machines while others don’t? It often depends on the stroke’s severity and the areas of the brain affected.
Types Of Ventilators Used
There are different ventilators tailored to various needs after a stroke. The most common is the invasive ventilator, where a tube is inserted into your windpipe to assist breathing directly.
Another type is the non-invasive ventilator, which uses a mask over your nose or mouth. This option is less uncomfortable and is used when you can still breathe somewhat on your own.
Sometimes, your medical team may switch between these types depending on your progress. Understanding these options can help you feel more in control of your care.
Factors Influencing Ventilator Duration
Understanding what affects the length of time a stroke patient remains on a ventilator can help you prepare and support their recovery better. Several key factors come into play, each influencing how long breathing assistance might be necessary. Knowing these can guide discussions with medical teams and shape your expectations.
Stroke Severity And Location
The severity of the stroke is a major factor. A more severe stroke often causes greater brain damage, making it harder for the patient to breathe independently. For example, strokes affecting the brainstem can directly impact breathing control, increasing ventilator dependence.
Location matters as well. Strokes in areas controlling respiratory muscles or consciousness usually require longer ventilator support. Have you noticed how some patients recover quicker when the stroke spares critical breathing centers?
Preexisting Health Conditions
Chronic illnesses such as lung disease, heart problems, or diabetes can slow down recovery. These conditions may reduce lung function or weaken the body’s ability to heal, leading to prolonged ventilator use.
Imagine trying to breathe through a straw while running a marathon—that’s similar to how preexisting conditions strain the body post-stroke. Does your loved one have other health issues that might complicate their recovery?
Complications During Recovery
Complications like infections, pneumonia, or blood clots can extend the need for ventilation. These problems often arise during hospital stays and delay the process of weaning off the ventilator.
Even minor setbacks can add days or weeks to ventilator time. Are caregivers and medical teams vigilant in spotting and managing these complications early?
Typical Ventilator Timelines
Understanding typical ventilator timelines after a stroke helps set realistic expectations for recovery and care planning. The duration a patient might spend on a ventilator varies widely depending on the severity of the stroke and individual health factors. Knowing these timelines can guide you in preparing emotionally and practically for what lies ahead.
Short-term Ventilation
Many stroke patients require ventilator support for a brief period, often just a few days to a week. This short-term ventilation usually occurs when the stroke has caused temporary breathing difficulties or airway protection issues. In these cases, the medical team focuses on stabilizing the patient quickly, aiming to remove the ventilator as soon as it’s safe.
Think about a friend who was on a ventilator for just five days after a moderate stroke—they were able to start physical therapy soon after and made steady progress. This quick turnaround is common when the brain injury is less severe and there are no complications like infections.
Extended Ventilation Periods
Some patients face longer ventilation periods, lasting several weeks or even months. Extended ventilation often happens when the stroke causes significant brain damage affecting breathing control or when complications delay recovery. These longer timelines demand more intensive care and can impact the overall rehabilitation process.
Imagine a scenario where a loved one remains on a ventilator for over a month due to severe stroke effects. During this time, families often need to adjust their expectations and coordinate with healthcare providers about potential tracheostomy placement or long-term respiratory support options.
Have you considered how the length of ventilation might affect your loved one’s rehabilitation goals? Understanding this can help you advocate for appropriate therapies and support systems during recovery.
Weaning Off The Ventilator
Weaning off a ventilator after a stroke is a delicate process. It requires careful monitoring and assessment by medical professionals. The goal is to ensure the patient can breathe independently. This process involves gradual steps and keen observation. Understanding the stages involved can ease concerns for families and caregivers.
Signs Of Readiness
Before starting the weaning process, doctors look for specific signs. The patient should be stable and show improved lung function. Oxygen levels should remain adequate without assistance. The patient should be conscious and responsive. These indicators suggest they may handle breathing on their own.
Weaning Procedures
The weaning process involves several steps. Doctors might reduce ventilator support gradually. This helps the patient’s body adjust to breathing independently. Trials may be conducted where the ventilator is turned off for short periods. Monitoring during these trials ensures safety and assesses progress.
Challenges In Weaning
Weaning off a ventilator can present challenges. Some patients may experience difficulty breathing on their own. This can be due to muscle weakness or other complications. Anxiety and stress can also impact the process. Continuous support and reassurance are vital during this time.
Impact On Stroke Recovery
The time spent on a ventilator after a stroke can significantly affect your recovery journey. Mechanical ventilation supports breathing when stroke impairs respiratory function, but it also brings challenges that influence both physical and cognitive healing. Understanding these impacts can help you better prepare for the road ahead and advocate for the care you need.
Physical And Cognitive Effects
Being on a ventilator often means extended immobility. This can lead to muscle weakness, joint stiffness, and decreased endurance, making physical recovery slower. You might notice difficulties in regaining strength even after respiratory support ends.
Cognitive effects are equally important. Ventilation and the underlying stroke may cause confusion, memory problems, or difficulty concentrating. These issues can complicate your ability to follow therapy instructions and manage daily activities.
Have you considered how these challenges might change your approach to rehabilitation? Recognizing the connection between ventilation and cognitive health can prompt early mental exercises that support recovery.
Rehabilitation Considerations
Rehabilitation after ventilator support requires a tailored approach. Therapists often focus on gradual physical activity to rebuild muscle and improve breathing efficiency. Early involvement in physical therapy can prevent complications like pneumonia or bedsores.
- Work closely with your care team to set realistic goals.
- Incorporate breathing exercises to regain lung strength.
- Include cognitive therapies such as memory drills or problem-solving tasks.
Your active participation matters. Small daily efforts can make a big difference in overcoming the setbacks caused by ventilation. What strategies can you try to stay motivated during this demanding phase?
Family And Caregiver Support
Family and caregiver support plays a crucial role when a loved one is on a ventilator after a stroke. This period is often filled with uncertainty and stress, demanding both emotional strength and practical involvement. Your presence and understanding can provide comfort and hope during this difficult time.
Emotional Challenges
Watching someone you care about rely on a ventilator can bring intense emotions like fear, frustration, and helplessness. You might feel overwhelmed by the sudden change in roles and responsibilities. Recognizing these feelings is important because they affect how you support your loved one and yourself.
It helps to share your emotions with others who understand your situation. Support groups or counseling can offer relief and prevent burnout. Ask yourself, how can you balance your needs with those of the patient to stay strong?
Communication With Medical Team
Clear and consistent communication with doctors, nurses, and therapists is essential. You have the right to ask questions and get updates about ventilator use, expected recovery, and care plans.
Keep a notebook or digital record of important information shared during visits. This helps you track progress and ensures you don’t miss critical details. How often do you check in with the medical team to stay informed?
Remember, you are a vital part of the care team. Sharing observations about your loved one’s condition can provide valuable insights to healthcare providers.
Advances In Ventilator Care
Advances in ventilator care have significantly changed how patients recover after a stroke. These improvements not only increase survival rates but also enhance the quality of life during and after ventilation. Understanding these developments can help you or your loved ones navigate the challenging recovery process with more confidence.
New Technologies
Modern ventilators come with smarter features that adjust breathing support automatically based on the patient’s needs. Sensors now monitor oxygen levels and lung function continuously, reducing the risk of complications.
One exciting technology is the use of non-invasive ventilation methods that avoid the discomfort of tubes. This can shorten the time you need to stay on a ventilator and lower infection risks.
Have you ever wondered how these machines can adapt so quickly? It’s thanks to real-time data analysis that allows doctors to fine-tune settings instantly, improving comfort and efficiency.
Improved Recovery Protocols
Recovery doesn’t stop when ventilation begins to decrease. New protocols focus on early mobilization and respiratory therapy to speed up lung healing.
Physical therapists now work closely with respiratory teams to design personalized plans that help patients regain strength faster. This teamwork reduces ventilator dependence time and supports better brain recovery after stroke.
Imagine being able to sit up and breathe more easily just days after being on a ventilator. That’s the goal of these improved protocols, which also include regular assessment to prevent setbacks.

Credit: www.youtube.com
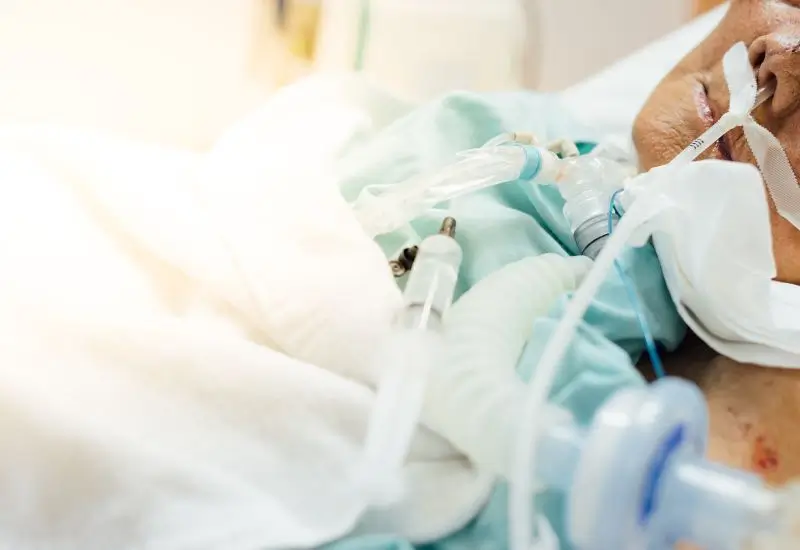
Credit: www.agapehospicepc.org
Frequently Asked Questions
How Long Is Ventilator Support After A Stroke?
Ventilator support duration varies based on stroke severity and complications. It can range from days to weeks. Doctors continuously assess breathing ability to decide when to wean off the ventilator safely.
What Factors Affect Ventilator Duration Post-stroke?
Factors include stroke size, location, patient’s overall health, and lung function. Complications like pneumonia or brain swelling can prolong ventilator use. Early rehabilitation and medical care also impact recovery speed.
Can Stroke Patients Recover Breathing Without A Ventilator?
Yes, many stroke patients regain independent breathing with proper treatment. Recovery depends on brain damage extent and respiratory muscle strength. Timely medical intervention improves chances of breathing without ventilator support.
When Is Ventilator Removal Considered Safe After Stroke?
Ventilator removal is safe once the patient can breathe independently and maintain oxygen levels. Doctors evaluate neurological status, respiratory function, and swallowing ability before extubation to prevent complications.
Conclusion
Recovery time on a ventilator after a stroke varies widely. Many factors affect how long someone needs breathing support. Doctors monitor progress daily to decide when to remove the ventilator. Some patients need it only for a few days. Others may require weeks or longer.
Family support and good care play key roles in recovery. Staying patient helps loved ones during this tough time. Each stroke case is unique, and healing takes time. Understanding this helps manage expectations and plan for the future.





