Are you struggling with low tidal volume on your ventilator? It can be frustrating and even dangerous when your patient isn’t getting the proper amount of air with each breath.
But don’t worry—fixing this issue is possible, and you can take the right steps to improve ventilation quickly. You’ll learn clear, practical tips to identify why the tidal volume is low and how to adjust your ventilator settings effectively. Keep reading to gain confidence in managing this critical problem and ensure the best care for your patient.
Causes Of Low Tidal Volume
Low tidal volume on a ventilator can be frustrating and dangerous if not addressed promptly. Understanding the causes is key to fixing the issue effectively. Let’s break down the main reasons why your ventilator might be delivering less air than expected.
Ventilator Settings Errors
Incorrect ventilator settings are a common cause of low tidal volume. If the tidal volume parameter is set too low, the machine will deliver less air than the patient needs. Sensitivity settings that are too high can also prevent the ventilator from triggering properly.
Sometimes, a simple recalibration or adjustment of the ventilator mode can solve the problem. Have you checked whether the set tidal volume matches the patient’s ideal body weight? This small detail can make a big difference.
Patient-related Factors
Changes in the patient’s lung compliance or airway resistance can reduce tidal volume. Conditions like pneumothorax, mucus plugging, or bronchospasm can limit airflow despite correct ventilator settings. Patient effort and sedation levels also influence the volume delivered.
If you notice sudden drops in tidal volume, consider whether the patient’s condition has changed. Are there signs of increased secretions or airway obstruction? These clues can guide your next steps.
Equipment Malfunctions
Faulty equipment may cause low tidal volume even if settings and patient factors are normal. Leaks in the ventilator circuit or damaged tubing can reduce the volume delivered. Additionally, malfunctioning valves or sensors can give inaccurate readings or prevent proper ventilation.
Regular equipment checks can save you time and prevent complications. When was the last time you inspected the entire ventilator circuit for leaks or damage? Don’t overlook this simple but critical step.

Credit: onlinejcf.com
Initial Assessment Steps
Low tidal volume on a ventilator needs quick and clear checks. The first assessment helps find the cause fast. This ensures the patient gets proper breathing support. Start by reviewing the machine and patient carefully. Then, check the ventilator circuit for any issues. These steps guide you to fix the problem without delay.
Check Ventilator Parameters
- Confirm the tidal volume set matches the prescription.
- Verify the mode of ventilation is correct for the patient.
- Look for alarms or error messages on the ventilator display.
- Check the inspiratory pressure and flow settings.
- Ensure the oxygen concentration and PEEP are stable.
Inspect Patient Condition
- Observe the patient’s chest rise and fall with breaths.
- Check for signs of airway obstruction or secretions.
- Listen to lung sounds for wheezes or crackles.
- Assess patient comfort and sedation level.
- Look for any sudden changes in vital signs.
Examine Ventilator Circuit
- Inspect tubing for kinks, disconnections, or leaks.
- Check the humidifier and filters are functioning well.
- Ensure the endotracheal tube or mask is secure.
- Look for condensation buildup that could block airflow.
- Replace any damaged or worn parts immediately.
Adjusting Ventilator Settings
Adjusting ventilator settings is a key step to fix low tidal volume effectively. Small changes can make a big difference in how well the ventilator supports breathing. Understanding which settings to tweak helps you respond quickly and keep your patient comfortable and safe.
Increasing Tidal Volume
Increasing the tidal volume directly raises the amount of air delivered with each breath. Start by raising the volume in small increments, such as 50 to 100 mL, to avoid lung injury. Watch closely for any signs of discomfort or over-distension, especially in patients with sensitive lungs.
Have you checked the patient’s lung compliance recently? Low compliance means the lungs are stiff, and simply increasing volume might not be enough or could cause harm. Always balance the tidal volume with the patient’s condition and ventilation goals.
Modifying Respiratory Rate
Adjusting the respiratory rate can improve overall ventilation without drastically changing volume. Increasing the rate adds more breaths per minute, which may help compensate for lower tidal volumes. However, be cautious—too fast a rate can cause air trapping and reduce oxygen exchange efficiency.
Ask yourself: Is the current rate causing breath stacking or patient discomfort? Sometimes slowing down the rate while raising volume improves gas exchange better than increasing rate alone. Monitor blood gases and patient response to find the right balance.
Optimizing Inspiratory Flow
Inspiratory flow controls how fast air is delivered during each breath. If the flow is too slow, the tidal volume may not reach the lungs fully before exhalation begins. Increasing the flow rate can help ensure the target volume is delivered within the inspiratory time.
Try adjusting the flow waveform and peak flow settings to see what feels more natural for your patient. Have you noticed any signs of patient-ventilator asynchrony? Fine-tuning inspiratory flow often reduces this issue and improves comfort.
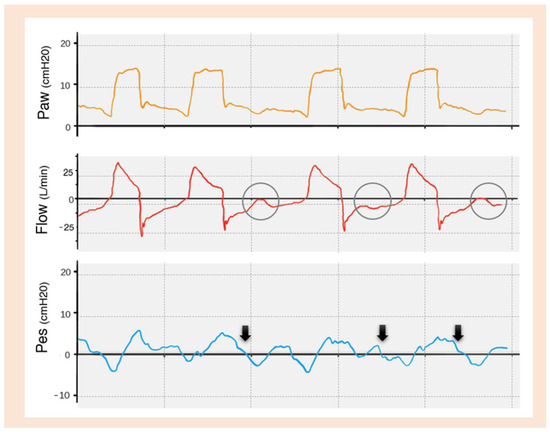
Credit: www.mdpi.com
Addressing Patient Factors
Low tidal volume on a ventilator can often be traced back to patient-specific factors. Understanding and addressing these factors is key to improving ventilation effectiveness. Let’s look closely at common patient-related causes and how you can manage them.
Managing Airway Obstruction
Airway obstruction is a frequent reason for low tidal volume. Mucus plugs, secretions, or swelling can block airflow, reducing the volume delivered to the lungs.
Regular suctioning and humidification can help keep the airway clear. Also, assess for any kinked or displaced endotracheal tubes that might restrict airflow. Have you checked the airway patency recently?
Treating Lung Compliance Issues
Lung compliance affects how easily the lungs expand. Conditions like pneumonia, pulmonary edema, or fibrosis make lungs stiffer and harder to ventilate.
Adjusting ventilator settings to increase pressure or using recruitment maneuvers may improve tidal volume. Sometimes, treating the underlying lung disease aggressively is the only way to restore compliance. How often do you reevaluate the patient’s lung mechanics?
Handling Patient-ventilator Asynchrony
When the patient’s breathing effort doesn’t match the ventilator’s cycle, tidal volume can drop. Asynchrony causes discomfort and ineffective ventilation.
Monitor for signs like irregular breathing patterns or increased work of breathing. Adjust trigger sensitivity, flow rates, or sedation levels to synchronize efforts. Have you observed patient-ventilator mismatch during recent shifts?
Troubleshooting Equipment Issues
Low tidal volume on a ventilator often signals a leak or blockage in the system. Checking tube connections and adjusting settings can quickly restore proper airflow. Regular maintenance helps prevent these common issues.
Troubleshooting equipment issues can be daunting, but it’s a crucial part of managing ventilators effectively. When you notice low tidal volume, the equipment might be the silent culprit. Understanding how to diagnose and fix these issues can make all the difference in patient care.Checking For Leaks
Leaks are a common issue that can lead to low tidal volume. Begin by checking all the connections from the ventilator to the patient. Ensure everything is securely attached. You might be surprised how often a simple adjustment can solve the problem. A personal experience I had involved a slight crack in a connector that was barely visible, yet it caused significant volume loss. Always keep a keen eye on every component.Inspecting Tubing And Connections
Inspect the tubing for any kinks or blockages. Even a minor obstruction can restrict airflow significantly. Run your fingers along the tubing to feel for any irregularities. If you find a problem, replacing the faulty part can restore optimal performance. The connections should also be tightly secured. Loose connections are often overlooked but can drastically affect functionality.Verifying Alarm Functionality
Alarm systems are your early warning signs. Ensure they’re properly set and functioning. If an alarm isn’t sounding when it should, it might be misconfigured or malfunctioning. Regularly test alarms to confirm they’re working as intended. Have you ever ignored an alarm, assuming it was a false alert? It might be time to reassess your approach. Alarms are there for a reason, and verifying their functionality should be a priority.Monitoring And Follow-up
Monitoring and follow-up are critical when managing low tidal volume on a ventilator. Keeping a close eye on the patient’s response allows you to make timely adjustments that can improve ventilation and prevent complications. Without consistent tracking and documentation, you risk missing subtle signs that the treatment plan needs revision.
Continuous Tidal Volume Tracking
Use ventilator display screens and monitoring systems to watch tidal volume in real time. Look for trends rather than isolated readings—small drops over time can signal the need for intervention. Consider setting alarms for volume thresholds to alert you immediately if tidal volume falls below a safe level.
Regular checks are essential, especially after changing ventilator settings or patient positioning. Have you noticed how tidal volume can vary with even minor adjustments? This is why continuous tracking prevents surprises and keeps you proactive.
Adjusting Based On Patient Response
Adjust ventilator settings according to how the patient tolerates changes in tidal volume. If you see signs of distress, such as increased work of breathing or dropping oxygen levels, reassess the volume settings. Sometimes small tweaks in pressure or rate can significantly improve ventilation without causing discomfort.
Remember that each patient is unique. What worked for one may not work for another. Stay alert to clinical cues and be ready to personalize your approach based on ongoing feedback from the patient’s condition.
Documenting Changes And Outcomes
Keep detailed records of all ventilator adjustments and the patient’s response to those changes. Documentation helps you track what works and what doesn’t, providing a clear history for future care decisions. It also supports communication with your healthcare team, ensuring everyone is updated.
Have you ever returned to a case and found your notes invaluable? Clear documentation reduces guesswork and promotes better outcomes. Use standardized forms or electronic health records to maintain consistency and ease of access.

Credit: onlinejcf.com
Frequently Asked Questions
What Causes Low Tidal Volume On A Ventilator?
Low tidal volume can result from leaks, tube obstruction, or incorrect ventilator settings. Patient factors like lung compliance also affect volume delivery.
How To Troubleshoot Low Tidal Volume Alarms?
Check for airway leaks, tube disconnections, or blockages. Verify ventilator settings and patient positioning to ensure proper ventilation.
Can Ventilator Settings Fix Low Tidal Volume Issues?
Yes, adjusting tidal volume, inspiratory pressure, or respiratory rate can correct low volume. Always tailor settings to patient needs.
When Should A Clinician Suspect Ventilator Malfunction?
If adjustments fail and alarms persist, suspect equipment malfunction. Inspect the ventilator and consider alternative devices if needed.
Conclusion
Fixing low tidal volume on a ventilator helps patients breathe better. Check the ventilator settings first to ensure correct values. Look for leaks or blockages in the breathing circuit. Adjust pressure or volume carefully, based on patient needs. Always monitor the patient’s response to changes closely.
Quick action can prevent serious breathing problems. Keep learning and practicing these steps for better care. This simple guide can make a big difference in treatment. Stay calm, focused, and ready to act.