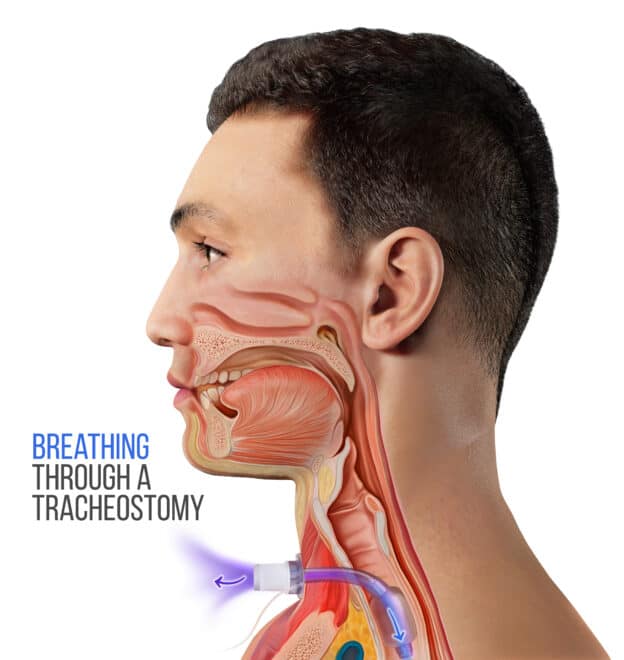
If you or a loved one faces serious breathing problems, you might be wondering: Is a tracheostomy better than a ventilator? This question matters because the choice can affect comfort, recovery, and daily life.
Understanding the differences can help you feel more confident about the best option for your health. Keep reading to discover what each option really means for you and how it could change your breathing experience.
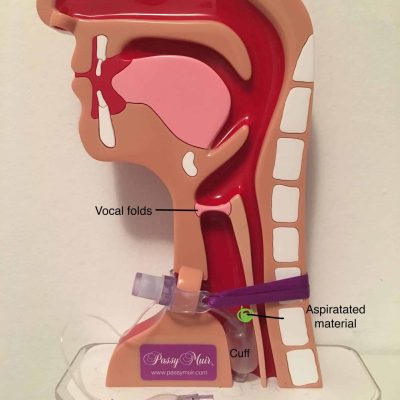
Credit: tracheostomyeducation.com
Tracheostomy Basics
Understanding the basics of a tracheostomy helps clarify its role in breathing support. This procedure creates a direct airway through the neck into the windpipe. It can offer a more comfortable and long-term solution for patients who need help breathing. Knowing what a tracheostomy is and when it is necessary helps in comparing it with other options like ventilators.
What Is A Tracheostomy
A tracheostomy is a small opening made in the front of the neck. A tube is placed through this opening into the windpipe. This tube helps air flow directly into the lungs. It bypasses the nose and mouth, making breathing easier for some patients. The tube can be temporary or long-term depending on the patient’s needs.
When Is It Needed
Doctors recommend a tracheostomy for several reasons:
- When the airway is blocked or damaged.
- If long-term breathing support is required.
- To help remove secretions from the lungs.
- When using a ventilator for a long time is difficult.
- To improve comfort for patients on long-term breathing machines.
This procedure can reduce risks linked to long-term use of breathing tubes through the mouth or nose. It also allows patients to speak and eat more easily in some cases.
Ventilator Essentials
Understanding ventilators is key when comparing them to tracheostomies. Ventilators support breathing by moving air in and out of the lungs. They are often life-saving devices, but knowing how they work and when they are used can help you make informed decisions about respiratory care.
How Ventilators Work
A ventilator pushes air into your lungs through a tube inserted into your airway. This tube can go through your mouth or nose, or directly into your trachea if you have a tracheostomy. The machine controls the amount and pressure of air, ensuring your lungs get enough oxygen.
Some ventilators assist your own breathing efforts, while others take over completely. Sensors monitor your breathing patterns and adjust airflow accordingly. This helps reduce the work your lungs and muscles have to do.
Common Uses
- Respiratory failure caused by illness or injury
- During surgery when general anesthesia prevents natural breathing
- Severe lung infections like pneumonia
- Chronic conditions such as COPD or neuromuscular diseases
Have you ever wondered why some patients switch from ventilators to tracheostomies? Often, it’s about long-term comfort and easier breathing management. Ventilators excel in emergencies, but their use over weeks or months can be challenging without a tracheostomy.
Comparing Tracheostomy And Ventilator
Comparing a tracheostomy and a ventilator helps understand their roles in breathing support. Both assist patients who cannot breathe normally. Each has unique features, advantages, and risks. Choosing the right one depends on the patient’s condition and medical advice.
Advantages Of Tracheostomy
- Provides a direct airway to the lungs for easier breathing.
- Allows long-term use without discomfort in the mouth or throat.
- Improves patient comfort compared to a tube in the mouth.
- Facilitates better oral hygiene and speech with a speaking valve.
- Reduces the risk of damage to vocal cords and throat tissues.
- Enables easier removal of lung secretions and mucus.
Benefits Of Ventilator
- Offers full or partial breathing support through a mask or tube.
- Non-surgical and can be used quickly in emergencies.
- Flexible for short-term or long-term respiratory support.
- Adjustable settings to match patient’s breathing needs.
- Helps patients with weak respiratory muscles or lung disease.
- Can be used in hospitals, homes, or during transport.
Risks And Complications
- Tracheostomy may cause infection or bleeding at the site.
- Possible damage to the windpipe or nearby structures.
- Ventilators can cause lung injury if used improperly.
- Risk of pneumonia due to prolonged use of either method.
- Ventilator use may cause dry mouth or airway irritation.
- Both require careful monitoring to avoid complications.
Patient Experience And Comfort
When deciding between a tracheostomy and a ventilator, patient experience and comfort play a crucial role. Comfort isn’t just about physical ease; it also involves emotional well-being and the ability to engage with the world around you. Understanding how each option affects your daily life helps you make choices that align with your personal needs and goals.
Mobility And Communication
A tracheostomy can sometimes offer greater mobility compared to being tethered to a ventilator machine. Many patients report feeling less restricted because they can move around more freely without bulky equipment. This increased freedom can improve mood and reduce feelings of isolation.
Communication is another vital factor. Speaking with a tracheostomy tube often requires learning new techniques, but many find it easier than using a ventilator. You might be able to talk more naturally, which can make social interactions less frustrating and more fulfilling.
Care And Maintenance
Caring for a tracheostomy involves regular cleaning and monitoring to prevent infection. While this may seem demanding at first, many patients grow confident with routine care and appreciate the control it gives them over their health. It’s important to ask your healthcare team about specific steps to make this process easier for you.
Ventilators, on the other hand, require consistent technical support and can sometimes limit your independence. Have you considered how much assistance you want or need on a daily basis? Your comfort might increase if you choose the option that fits your lifestyle and support system best.
Long-term Outcomes
Long-term outcomes are vital when deciding between a tracheostomy and a ventilator. Both options support breathing but affect recovery and daily life differently. Understanding these effects helps patients and families make informed choices.
Recovery And Weaning
Recovery with a tracheostomy often allows more gradual weaning from breathing support. Patients may regain natural breathing faster compared to prolonged ventilator use. The tracheostomy tube can be adjusted or removed as lungs improve.
Ventilators may keep patients dependent on machines longer. Weaning can be challenging if lung strength remains weak. This can increase hospital stays and risk of complications.
Quality Of Life
Quality of life tends to improve with a tracheostomy. It allows easier speech and eating than a ventilator alone. Patients often feel more comfortable and mobile.
Ventilators can limit movement and social interactions. Noise and machine dependency may cause stress. Long-term use can affect sleep and mental health.
Credit: tracheostomyeducation.com
Choosing The Right Option
When faced with critical health decisions, choosing between a tracheostomy and a ventilator can be daunting. Each option comes with its unique set of benefits and challenges. Understanding these can help guide your decision towards the best choice for you or your loved one.
Medical Considerations
The choice between a tracheostomy and a ventilator often hinges on medical factors. A tracheostomy might be recommended for patients needing long-term respiratory support. It allows for easier breathing and speaking compared to a ventilator, which is typically used for short-term acute cases.
Doctors often evaluate the patient’s overall health, prognosis, and potential for recovery. They consider the risks and benefits of each option. It’s crucial to discuss these medical considerations with your healthcare provider to understand which option aligns best with the patient’s health condition.
Patient And Family Preferences
Your preferences and those of your family play a vital role in making this decision. Some families prioritize quality of life and comfort, leaning towards options that allow for more mobility and interaction, like a tracheostomy. Others might opt for a ventilator if they believe it offers a better chance of recovery or fits their personal values.
It’s important to have open discussions about what life on a tracheostomy or ventilator would entail. Consider how each option aligns with your lifestyle and goals. Have you thought about how each choice impacts daily routines and long-term plans?
Ultimately, the decision between a tracheostomy and a ventilator is deeply personal. It requires balancing medical advice with personal values and lifestyle considerations. Take the time to weigh each aspect thoughtfully.
Future Trends And Innovations
The landscape of respiratory care is evolving quickly, especially when deciding between a tracheostomy and a ventilator. New technologies and approaches aim to improve patient comfort, reduce complications, and enhance quality of life. Understanding these future trends can help you make informed decisions about long-term respiratory support.
Advancements In Smart Ventilator Technology
Smart ventilators are becoming more adaptive and user-friendly. They can adjust breathing support automatically based on your body’s changing needs. Imagine a ventilator that learns your breathing patterns and reacts instantly—this makes care more personalized and less invasive.
These devices also offer remote monitoring options, letting healthcare providers track your condition in real-time. This reduces hospital visits and helps catch problems early, giving you peace of mind.
Minimally Invasive Tracheostomy Techniques
New methods for performing tracheostomies are less invasive and safer. These techniques use smaller incisions and advanced imaging to guide the procedure precisely. The result? Faster recovery times and fewer complications.
If you worry about the surgery, these innovations might ease your concerns by making the process smoother and less painful. Would you feel more confident choosing a tracheostomy knowing it’s becoming less risky?
Integration Of Ai And Machine Learning In Respiratory Care
Artificial intelligence is starting to play a big role in respiratory health. AI systems analyze vast amounts of data to predict respiratory issues before they become severe. This proactive approach can help you avoid emergency situations and improve long-term outcomes.
Machine learning algorithms also help customize treatment plans, offering care that fits your unique needs. How would having a treatment plan tailored just for you change your experience?
Wearable And Portable Respiratory Devices
Wearable respiratory monitors are making it easier to track your lung function throughout the day. These small devices provide continuous feedback and alert you if something needs attention. You don’t have to wait for the next doctor’s appointment to know how you’re doing.
Portable ventilators are also getting lighter and more efficient, allowing greater freedom outside the hospital. This means you can maintain your lifestyle with fewer restrictions.
Emerging Therapies To Support Respiratory Health
Researchers are exploring new therapies that might reduce reliance on tracheostomies or ventilators altogether. Techniques like stem cell therapy and regenerative medicine show promise in repairing damaged lung tissue. While still in early stages, these options could transform respiratory care.
Would you consider experimental treatments if they offered a chance to breathe more naturally?
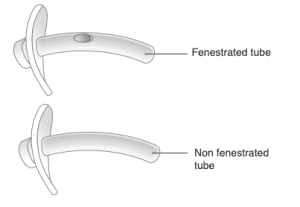
Credit: tracheostomyeducation.com
Frequently Asked Questions
What Is The Main Difference Between A Tracheostomy And Ventilator?
A tracheostomy is a surgical opening in the neck for breathing. A ventilator is a machine that supports or controls breathing. The tracheostomy can be connected to a ventilator or used independently for airway management.
When Is A Tracheostomy Preferred Over A Ventilator?
A tracheostomy is preferred for long-term breathing support or airway blockage. It reduces discomfort and allows easier oral care compared to prolonged ventilator use through a tube in the mouth.
Can A Patient Breathe Without A Ventilator After Tracheostomy?
Yes, some patients can breathe independently through a tracheostomy tube. This depends on their lung function and recovery. The tube keeps the airway open even without ventilator assistance.
What Are The Risks Of A Tracheostomy Versus A Ventilator?
Tracheostomy risks include infection, bleeding, and airway damage. Ventilator risks include lung injury and pneumonia. Both require careful medical supervision to minimize complications.
Conclusion
Choosing between a tracheostomy and a ventilator depends on many factors. Each option has its own benefits and risks. Doctors consider the patient’s health and needs carefully. Tracheostomy may offer more comfort for long-term breathing. Ventilators work well for short-term support.
Talk to healthcare providers to find the best choice. Understanding both options helps families make smart decisions. Breathing support is important, but safety matters most. The right care can improve quality of life.