Are you curious about how ventilators work and the different ways they support breathing? Understanding the 4 modes of a ventilator can help you grasp how these life-saving machines adjust to meet the needs of patients.
Whether you’re a healthcare professional, a student, or someone wanting to learn more, this guide will break down each mode in simple terms. By the end, you’ll feel confident about how ventilators assist breathing and why each mode matters. Keep reading to unlock the key facts that could make a real difference in understanding ventilator care.

Credit: www.vhtc.org
Basic Ventilator Functions
Understanding the basic functions of a ventilator is key to grasping how the different modes operate. Ventilators support breathing by assisting or controlling airflow, pressure, and volume to meet the patient’s needs. These core functions ensure the machine can adapt to various medical situations effectively.
Control Of Airflow
The ventilator carefully manages the flow of air into the lungs. It can deliver breaths at a set rate or allow you to breathe spontaneously with assistance. This control helps maintain proper oxygen and carbon dioxide levels in your body.
Have you ever wondered how the machine knows when to give a breath? Sensors monitor your breathing patterns to adjust airflow in real-time.
Pressure Regulation
Pressure is a critical factor in ventilation. The machine adjusts the pressure to open your airways and avoid lung injury. Too much pressure can cause damage, while too little might not support breathing adequately.
Think about blowing up a balloon—you need just the right pressure to inflate it without popping it. Ventilators apply this principle to your lungs.
Volume Delivery
Volume refers to the amount of air pushed into your lungs with each breath. The ventilator controls this to ensure your lungs receive enough air without overdistension. This function is particularly important for patients with lung conditions.
Imagine filling a glass with water—you want to pour enough to quench your thirst but not spill over. The ventilator does the same with air in your lungs.
Triggering And Cycling
Triggering decides when the ventilator starts a breath, either by sensing your effort or on a preset timer. Cycling determines when the breath ends, switching from inhalation to exhalation. Both functions work together to create a natural breathing rhythm.
Have you noticed how your breath changes when you relax versus when you exercise? The ventilator adapts its timing to match your body’s demands.
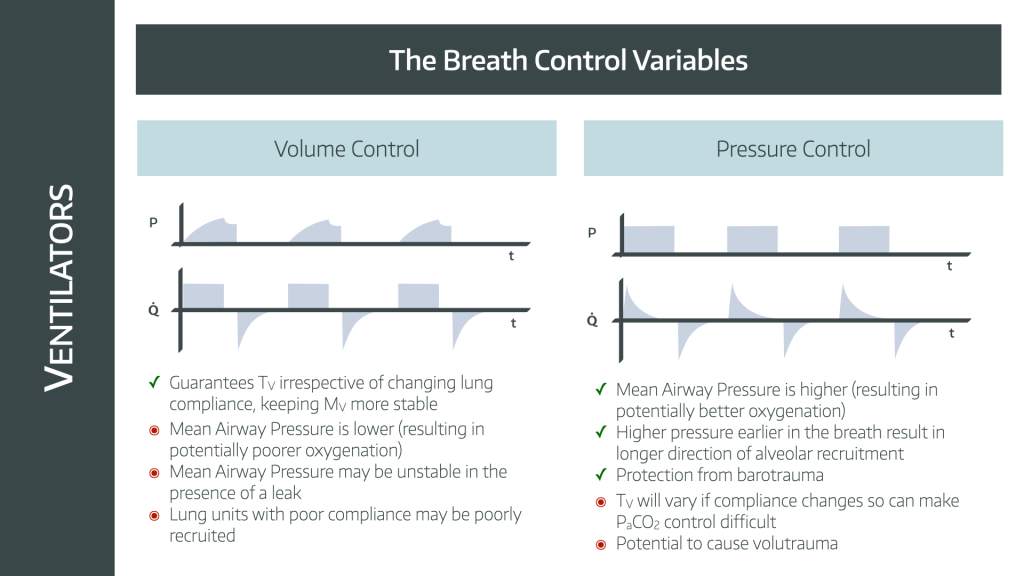
Volume Control Mode
Volume Control Mode is a fundamental setting on many ventilators, designed to ensure your lungs receive a precise amount of air with each breath. This mode gives you control over the volume of air delivered, making it easier to manage breathing support in critical situations. Understanding how this mode works can help you appreciate its role in patient care and when it’s most beneficial.
How It Works
In Volume Control Mode, the ventilator delivers a set volume of air during each breath, regardless of the pressure needed to push that air into your lungs.
The machine controls the amount of air, not the pressure, ensuring consistent tidal volume every time.
This means your lungs receive the exact volume programmed by the healthcare team, which can be crucial for maintaining stable oxygen levels.
When To Use
This mode is often used when precise control of lung volume is necessary, such as during surgery or in patients with unstable breathing patterns.
If you have weakened respiratory muscles or neurological conditions affecting breathing, Volume Control can help maintain consistent ventilation.
It is also beneficial when you need to ensure a fixed amount of oxygen delivery without relying on the patient’s effort.
Advantages And Limits
- Advantages:Guarantees a fixed tidal volume, making ventilation predictable and easier to monitor.
- Limits:Pressure can vary, which might cause discomfort or lung injury if the lungs are stiff or obstructed.
- It doesn’t adjust for changes in lung compliance or resistance, so close monitoring is essential.
Have you ever wondered how delivering a fixed air volume can sometimes lead to lung strain? That’s why clinicians must balance volume with pressure carefully in this mode.
Pressure Control Mode
Pressure Control Mode is a key setting on many ventilators. It controls the air pressure delivered to the patient’s lungs. This mode helps protect the lungs from damage by limiting the pressure during each breath. It is often used for patients with weak or injured lungs.
Mechanism
In Pressure Control Mode, the ventilator delivers air at a set pressure. The machine controls how hard the air pushes into the lungs. The breath continues until the set pressure is reached. The volume of air can change with each breath. The rate and pressure are fixed by the healthcare provider.
Clinical Applications
This mode suits patients with lung problems like ARDS or pneumonia. It helps keep lungs safe during ventilation. It is used when lung protection is a priority. Also, it assists in cases where patients need stable pressure. It supports patients who cannot breathe well on their own.
Benefits And Drawbacks
- Benefits:
- Limits lung pressure to prevent injury.
- Improves oxygen delivery in damaged lungs.
- Allows some control over breathing effort.
- Drawbacks:
- Air volume varies, making monitoring harder.
- May cause low oxygen if volume is too low.
- Not ideal for all patients, such as those needing fixed volumes.
Assist Control Mode
Assist Control Mode is a common ventilator setting used in intensive care. It helps patients breathe by providing support for every breath. This mode ensures that the patient gets a set number of breaths per minute, with each breath delivered fully by the machine. It is useful for patients who need help with breathing but still try to breathe on their own.
Operation
In Assist Control Mode, the ventilator delivers a preset volume or pressure with each breath. It can trigger breaths based on patient effort or time intervals. When the patient starts a breath, the machine assists by giving full support. If the patient does not breathe, the ventilator gives breaths automatically. This ensures steady and controlled breathing at all times.
Patient Interaction
The ventilator senses when the patient begins to inhale. It then provides a full breath to match the patient’s effort. This support helps reduce the work of breathing. The patient can breathe faster, but the ventilator will still provide full breaths. This mode is very responsive to the patient’s needs.
Suitability
- Patients who have weak breathing muscles
- Those recovering from surgery or illness
- Patients who need full ventilator support but can trigger breaths
- Not ideal for patients who breathe very fast or irregularly
Synchronized Intermittent Mandatory Ventilation
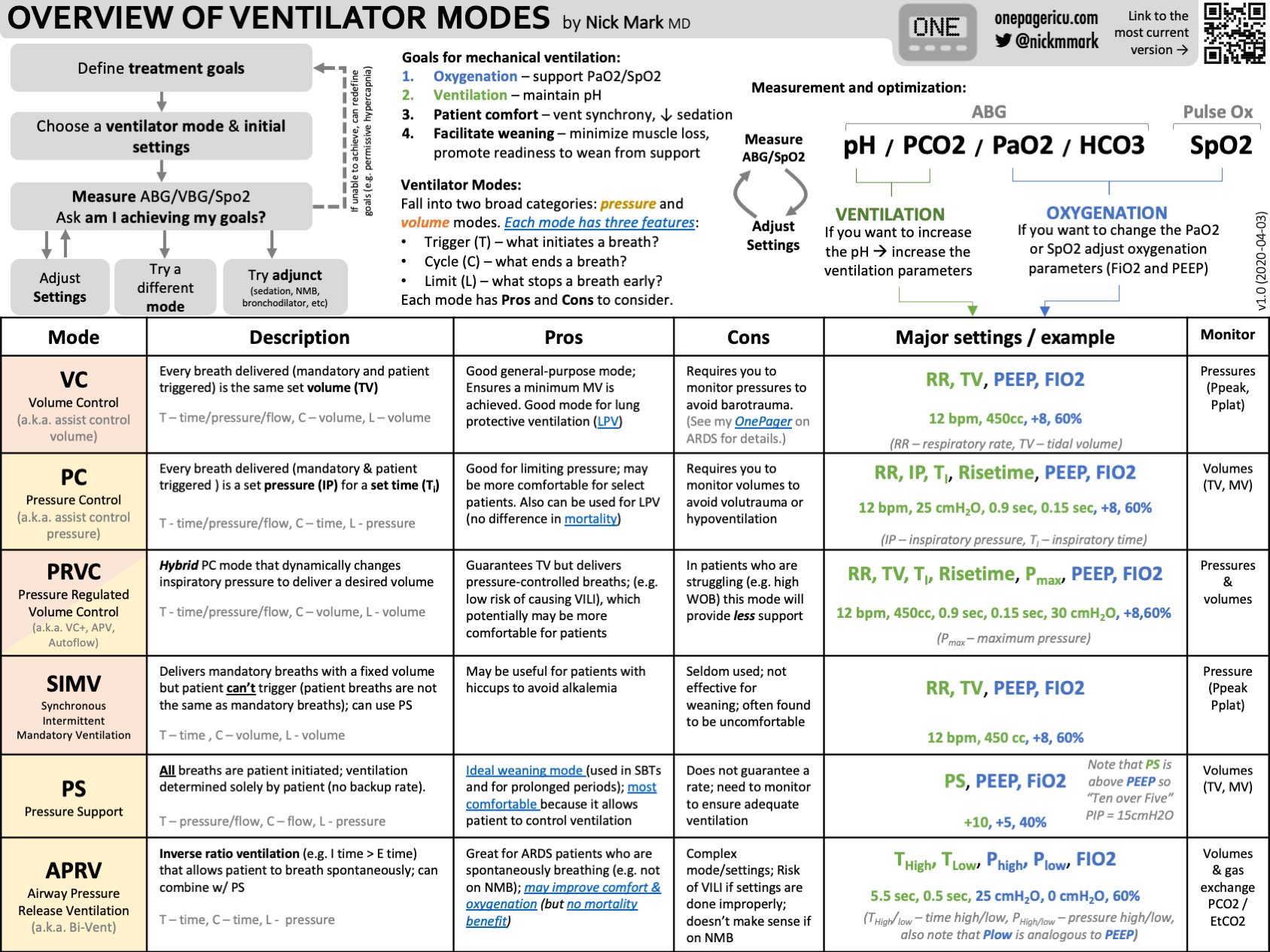
Synchronized Intermittent Mandatory Ventilation (SIMV) helps patients breathe with timed machine support and spontaneous breaths. It is one of the four main ventilator modes, which also include Assist-Control, Pressure Support, and Continuous Mandatory Ventilation. Each mode offers different breathing assistance levels.
Synchronized Intermittent Mandatory Ventilation (SIMV) is a key mode in mechanical ventilation. It provides mandatory breaths to patients at set intervals. SIMV allows spontaneous breathing between mechanical breaths. It combines controlled and assisted breathing, offering flexibility. This mode supports patients transitioning from full ventilation to independent breathing.Functioning
SIMV works by delivering breaths at regular intervals. The ventilator synchronizes these with the patient’s own breaths. It ensures the patient does not compete with the machine. This synchronization helps maintain effective breathing patterns. Patients can breathe on their own between machine-delivered breaths. The ventilator adjusts support based on patient’s efforts.Usage Scenarios
SIMV is useful in various clinical situations. It’s often used in weaning patients from full ventilation. It assists patients who have partial breathing ability. SIMV is suitable for post-surgery recovery. It supports patients with respiratory distress. It also helps in step-down care from intensive ventilation.Pros And Cons
- Pros:SIMV promotes spontaneous breathing. It reduces the risk of ventilator-induced lung injury. It can lower sedation needs. It offers flexibility in patient care.
- Cons:SIMV may cause patient-ventilator dyssynchrony. It can be challenging to adjust settings correctly. Over-reliance on spontaneous breaths may tire some patients.

Credit: www.anaestheasier.com
Choosing The Right Mode
Choosing the right ventilator mode can feel overwhelming, but it’s crucial for effective patient care. Each mode has unique features designed to support different breathing needs. Understanding how to match these modes with specific situations can improve outcomes and comfort.
Patient Factors
Consider the patient’s age, lung condition, and level of consciousness. For example, a patient with obstructive lung disease may benefit from a mode that allows for longer exhalation times.
Does the patient have spontaneous breathing efforts? If yes, a mode that supports spontaneous breaths might be better. Always think about how much control the patient can maintain over their breathing.
Clinical Goals
What are you trying to achieve with ventilation? Is it oxygenation, carbon dioxide removal, or both? Knowing your goal helps you select a mode that delivers the right pressure and volume.
For instance, if the goal is lung protection in ARDS patients, a mode that limits tidal volume is important. Tailor your mode choice to support healing, not just immediate breathing needs.
Monitoring And Adjustments
Once the mode is selected, continuous monitoring is key. Watch for changes in blood gases, lung mechanics, and patient comfort.
Be ready to adjust settings as the patient’s condition evolves. Ventilation isn’t set-and-forget; it requires ongoing evaluation and fine-tuning.
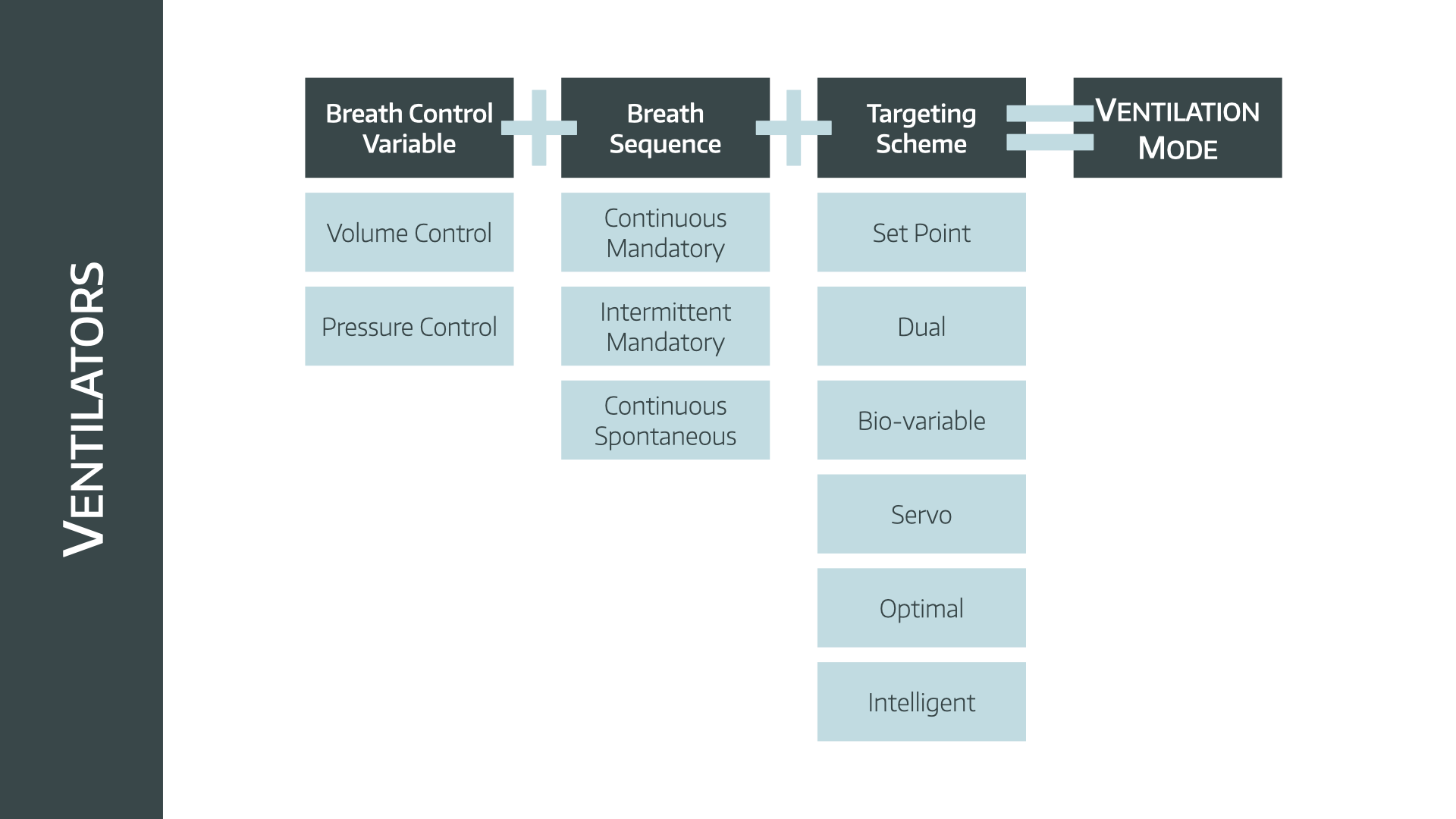
Credit: www.anaestheasier.com
Frequently Asked Questions
What Are The 4 Primary Ventilator Modes?
The 4 primary ventilator modes are Assist Control (AC), Synchronized Intermittent Mandatory Ventilation (SIMV), Pressure Support Ventilation (PSV), and Continuous Positive Airway Pressure (CPAP). Each mode supports breathing differently to meet patient needs.
How Does Assist Control Mode Work In Ventilation?
Assist Control (AC) mode delivers a preset tidal volume or pressure with each breath. It supports both mandatory and patient-initiated breaths to ensure adequate ventilation and oxygenation.
When Is Synchronized Intermittent Mandatory Ventilation Used?
SIMV mode provides mandatory breaths synchronized with the patient’s effort. It allows spontaneous breathing between mandatory breaths, aiding in weaning from the ventilator.
What Is The Role Of Pressure Support Ventilation?
Pressure Support Ventilation (PSV) assists spontaneous breaths by providing a preset pressure. It reduces the work of breathing and improves comfort during ventilation.
Conclusion
Understanding the four modes of ventilators helps in better patient care. Each mode serves a unique purpose in supporting breathing. Knowing these modes guides medical decisions clearly and quickly. It also helps patients and families feel more informed. Keep learning to stay confident with ventilator basics.
This knowledge makes a difference in healthcare settings. Simple and clear – that’s the key to understanding ventilator modes.