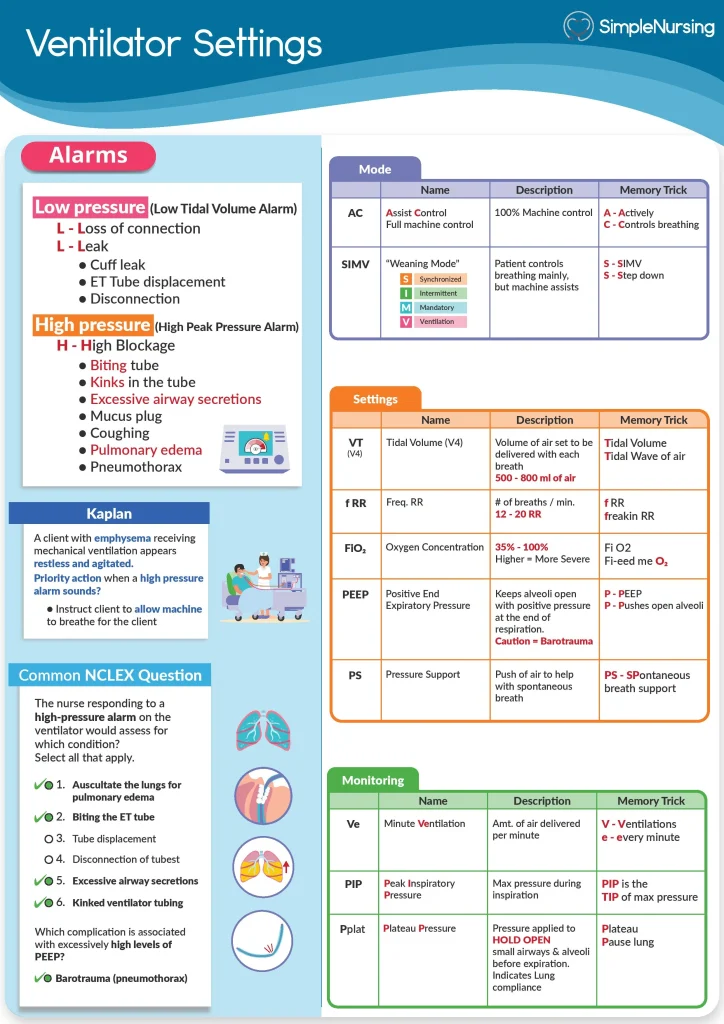
Have you ever wondered what triggers the high pressure alarm on your ventilator? If you’re caring for someone who relies on mechanical breathing support, this alarm can be both alarming and confusing.
Understanding what causes this warning is crucial because it helps you act quickly and keep your loved one safe. You’ll discover the common reasons behind high pressure alarms and learn how to handle them calmly and effectively. Keep reading to gain the knowledge that can make a real difference when every second counts.

Credit: tracheostomyeducation.com
Common Triggers
High pressure alarms on ventilators can startle you, especially when you’re focused on patient care. Understanding the common triggers helps you act quickly and effectively. Let’s look at what usually sets off these alarms and how to spot them fast.
Airway Obstruction
An airway obstruction is a primary cause of high pressure alarms. It happens when something blocks the flow of air, making it harder for the ventilator to push air into the lungs.
This blockage could be due to swelling, a foreign object, or even improper tube placement. Have you ever noticed how a small kink or twist in the airway can cause sudden alarm triggers? Checking the airway regularly can save critical time.
Patient Coughing
Coughing by the patient often causes a spike in airway pressure. It’s the body’s way of trying to clear irritants but can interfere with the ventilator’s function.
If the patient coughs frequently, the alarm might keep going off, creating stress for both you and the patient. Understanding this can help you differentiate between a true emergency and a temporary pressure rise.
Secretions And Mucus
Secretions and mucus build-up inside the airway or tubing can block airflow. This is a frequent problem, especially in patients with respiratory infections or impaired cough reflexes.
Regular suctioning and monitoring can prevent secretions from triggering the high pressure alarm. Have you ever found that clearing secretions promptly reduces alarms and improves patient comfort?
Kinks In Tubing
Kinks or bends in the ventilator tubing are simple yet common triggers of high pressure alarms. Even a slight twist can create resistance against airflow.
Carefully examine the tubing for any sharp bends or pressure points. Sometimes, the solution is as straightforward as repositioning or replacing the tubing to restore normal pressure levels.
Ventilator Settings Impact
Ventilator settings play a crucial role in managing patient breathing and ensuring safety. Incorrect adjustments can trigger a high pressure alarm, signaling potential risks. Understanding how each setting affects airway pressure can help you prevent these alarms and improve patient comfort.
Excessive Tidal Volume
Tidal volume is the amount of air delivered to the lungs with each breath. If this volume is set too high, the lungs can become overinflated, causing increased airway pressure. Have you noticed how even small increases in tidal volume can suddenly trigger alarms? Adjusting tidal volume to the patient’s lung capacity is key to avoiding unnecessary pressure spikes.
High Inspiratory Pressure
Inspiratory pressure controls the force used to push air into the lungs. Setting it too high can lead to excessive pressure buildup, which the ventilator senses and alarms about. It’s important to balance pressure levels to ensure adequate ventilation without causing lung injury. Are you regularly checking if the inspiratory pressure matches the patient’s lung compliance?
Peep Levels
Positive End-Expiratory Pressure (PEEP) keeps the airways open after exhalation. While necessary, too much PEEP can increase overall airway pressure and trigger alarms. Adjusting PEEP requires careful monitoring to maintain oxygenation without causing overdistension. Have you considered how even slight changes in PEEP might affect the pressure alarm status?
Lung Conditions
Lung conditions play a significant role in triggering the high pressure alarm on a ventilator. These conditions can cause airway obstruction or reduce lung compliance, leading to increased resistance during ventilation. Understanding how specific lung issues affect ventilator pressures can help you identify the root cause and respond appropriately.
Bronchospasm
Bronchospasm is a sudden tightening of the muscles around the airways. This narrowing makes it harder for air to flow, causing the ventilator to detect high pressure. You might notice this alarm during asthma attacks or allergic reactions when the airways constrict abruptly.
Managing bronchospasm quickly is crucial. Medications like bronchodilators can relax the muscles and open the airways, reducing the pressure. Have you ever experienced the frustration of a ventilator alarm during a patient’s sudden breathing difficulty? Recognizing bronchospasm early can prevent unnecessary complications.
Pulmonary Edema
Pulmonary edema happens when fluid builds up in the lungs, making them stiff and less able to expand. This stiffness increases airway pressure because the ventilator has to work harder to push air in. It often occurs in conditions like heart failure or after lung injury.
When you see a high pressure alarm with signs of fluid overload, consider pulmonary edema as a cause. Treating the underlying fluid problem can improve lung compliance and lower the pressure. How quickly you address this can make a big difference in patient outcomes.
Atelectasis
Atelectasis means part of the lung has collapsed or is not fully inflated. This reduces the available lung volume, which increases pressure during ventilation. It’s common after surgery or prolonged bed rest when deep breaths are limited.
Encouraging deep breathing exercises or using positive pressure techniques can help reopen collapsed lung areas. This reduces airway pressure and helps the ventilator work more efficiently. Have you noticed how simple interventions can sometimes resolve a high pressure alarm linked to atelectasis?

Credit: www.youtube.com
Equipment Malfunctions
Equipment malfunctions often trigger high pressure alarms on ventilators. These issues affect how the machine measures and controls airway pressure. Detecting malfunctions early helps prevent patient discomfort and potential harm. Understanding common equipment problems aids in quick troubleshooting and repair.
Faulty Pressure Sensors
Pressure sensors measure the airway pressure during ventilation. If these sensors fail, they may send incorrect readings. False high pressure alarms can occur despite normal airway conditions. Faulty sensors need prompt inspection and replacement to ensure accurate monitoring.
Leaks In Circuit
Leaks in the ventilator circuit cause pressure loss and irregular readings. Damaged tubing or loose connections often create leaks. The ventilator may respond by increasing pressure, triggering the alarm. Checking all circuit components helps identify and fix leaks quickly.
Ventilator Software Issues
Software errors can disrupt pressure regulation and alarm functions. Bugs or outdated software may cause false alarms or failure to detect real problems. Regular software updates and system checks maintain reliable ventilator performance and safety.
Patient Factors
Patient factors like coughing, biting the tube, or secretions in the airway can trigger a high-pressure alarm on a ventilator. These actions increase resistance, causing the machine to detect higher pressure than normal.
Ventilators are life-saving machines, but they can sometimes trigger high pressure alarms, which can be concerning for healthcare providers. One of the key areas to consider is patient factors. These are the elements directly related to the patient that can cause these alarms. Understanding these factors can help you manage and prevent alarm situations more effectively. Let’s dive into some of the critical patient-related causes.Patient-ventilator Asynchrony
Patient-ventilator asynchrony occurs when the patient’s breathing pattern does not align with the ventilator’s settings. This mismatch can lead to increased pressure in the system. It can happen due to incorrect ventilator settings or changes in the patient’s condition. Imagine a patient trying to exhale while the ventilator is pushing air in. This can create a tug-of-war situation, causing pressure to spike. Regularly reassessing the ventilator settings according to the patient’s current needs is crucial.Increased Secretions
Excessive secretions in a patient’s airways can obstruct airflow and cause high pressure alarms. Thick mucus can block the airways, making it harder for the ventilator to deliver the set volume of air. Ensuring the patient’s airways are clear is vital. Regular suctioning and maintaining adequate hydration can help manage secretions, reducing the chances of alarm triggers.Chest Wall Compliance
Changes in chest wall compliance can also be a significant factor. If the chest wall becomes stiffer due to conditions like obesity or musculoskeletal disorders, it can affect how well the lungs expand. A stiff chest wall means the ventilator has to work harder to inflate the lungs, leading to high pressure. Understanding the patient’s medical history and tailoring ventilator settings accordingly can make a significant difference. Have you ever faced a high pressure alarm and wondered what could be wrong? Often, a deeper look into patient factors can provide the answers you need.Troubleshooting Tips
High pressure alarms on ventilators can be alarming, but they often point to issues that can be quickly identified and resolved. Troubleshooting these alarms effectively requires a systematic approach. Understanding where the problem lies can save valuable time and improve patient comfort.
Checking The Airway
Start by examining the patient’s airway for any blockages or obstructions. Mucus plugs, secretions, or kinks in the endotracheal tube often cause increased pressure. Have you noticed a sudden change in the patient’s breathing sounds or difficulty during suctioning? These signs can indicate the airway is compromised and needs immediate attention.
Adjusting Ventilator Settings
Sometimes the ventilator settings may be too aggressive for the patient’s current lung condition. Check if the tidal volume or flow rate is set too high, causing pressure to build up. Adjusting the inspiratory pressure or switching to a different mode can help reduce the alarm frequency. How do you decide the right balance between support and patient comfort?
Inspecting Equipment
Next, carefully inspect the ventilator circuit and all connections. Look for any leaks, disconnections, or water accumulation in the tubing. A clogged filter or malfunctioning valve can also trigger high pressure alarms. Have you ever found a loose connection that was easy to fix but initially overlooked?
Monitoring Patient Response
Finally, observe the patient closely to see how they respond to any changes you make. Look for signs of distress, increased work of breathing, or changes in oxygen saturation. Continuous monitoring helps you understand whether your interventions are effective or if further action is required. What subtle changes in patient behavior have you learned to recognize as early warning signs?
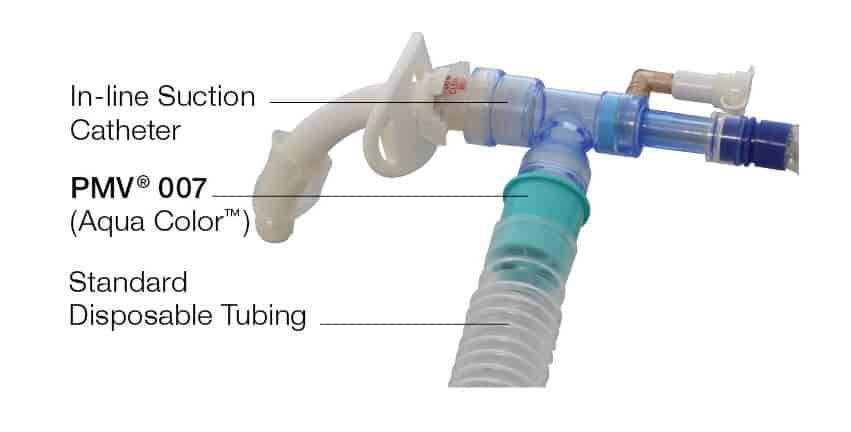
Credit: tracheostomyeducation.com
Frequently Asked Questions
What Triggers A High Pressure Alarm On A Ventilator?
High pressure alarms activate when airway pressure exceeds set limits. Causes include airway blockage, patient coughing, or lung stiffness. These alarms protect lungs from damage by alerting caregivers promptly.
How Does Mucus Buildup Cause High Pressure Alarms?
Mucus can block airways, increasing resistance during ventilation. This blockage raises airway pressure, triggering the high pressure alarm. Regular suctioning helps prevent mucus-related alarms.
Can Patient Biting The Tube Cause High Pressure Alarms?
Yes, biting the endotracheal tube narrows airflow, increasing pressure. This mechanical obstruction leads to high pressure alarms. Using bite blocks can reduce this risk.
Does Ventilator Setting Affect High Pressure Alarms?
Incorrect ventilator settings, such as high tidal volume or flow rates, raise airway pressure. Adjusting settings to patient needs helps prevent high pressure alarms.
Conclusion
High pressure alarms on ventilators often signal airway blockages or machine issues. Quick checks help find the cause and keep patients safe. Cleaning tubes and adjusting settings reduce alarm chances. Understanding these alarms helps caregivers respond fast and avoid harm.
Stay calm and act carefully when alarms sound. Keeping the ventilator working well supports better breathing for those who need it most.