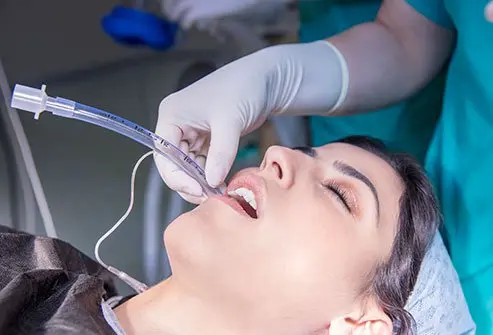
Have you ever wondered what a breathing tube looks like? If you or someone you care about ever needs help breathing, understanding this small but vital device can ease your worries.
A breathing tube might sound scary, but knowing what it is and how it works can give you a sense of control and peace of mind. You’ll discover exactly what a breathing tube looks like, why it’s used, and what to expect if you or a loved one needs one.
Keep reading—this knowledge could make a big difference when it matters most.

Credit: www.goodrx.com
Purpose Of A Breathing Tube
A breathing tube helps people breathe when they cannot do so on their own. It allows air to flow directly into the lungs. This tube is vital in many medical settings. It supports breathing and ensures oxygen reaches the body. Understanding its purpose shows why it is essential in healthcare.
Medical Uses
Breathing tubes assist patients during surgeries. They keep airways open while patients are asleep. Some people with lung diseases need these tubes for daily breathing support. They help in long-term care for patients who cannot breathe well. The tube connects to machines that help push air into the lungs.
Emergency Situations
In emergencies, breathing tubes save lives. They provide quick airflow when a person stops breathing. Paramedics and doctors use them in accidents or severe illnesses. The tube helps during heart attacks or severe injuries. It ensures oxygen reaches the brain and vital organs fast.
Common Types Of Breathing Tubes
Breathing tubes help patients breathe when they cannot do so on their own. Different types of tubes suit different medical needs. Each type has a unique shape and use. Understanding these tubes helps reduce fear and confusion.
Endotracheal Tubes
Endotracheal tubes are thin, flexible tubes inserted through the mouth. They go into the windpipe to keep the airway open. Usually made of clear plastic, they have a small balloon near the tip. The balloon inflates to hold the tube in place. Doctors use these tubes during surgery or emergencies.
Tracheostomy Tubes
Tracheostomy tubes are shorter and thicker. They enter the windpipe through a small hole in the neck. This type is used for long-term breathing support. Made from soft plastic or silicone, they often have a flange to secure them. Tracheostomy tubes allow easier breathing and help with suctioning mucus.
Nasotracheal Tubes
Nasotracheal tubes are similar to endotracheal tubes but go through the nose. They are flexible and clear, designed to fit the nasal passage. These tubes are less common but useful when mouth access is difficult. They also have a balloon cuff to seal the airway.
Materials And Design
The materials and design of a breathing tube play a crucial role in its effectiveness and safety. Understanding what these tubes are made of and how they are structured can help you appreciate why they function so well in critical medical situations. The right materials ensure flexibility, durability, and patient comfort, while the design elements focus on secure placement and preventing complications.
Tube Composition
Breathing tubes are usually made from medical-grade plastics such as polyvinyl chloride (PVC) or silicone. PVC is popular because it is firm yet flexible, allowing easy insertion and reliable airway support. Silicone tubes are softer and more comfortable but tend to be used for longer-term intubation because they cause less irritation.
These materials are chosen not only for their physical properties but also for being biocompatible, meaning they won’t cause adverse reactions inside the body. Have you ever wondered why some tubes feel stiffer than others during medical procedures? It often comes down to the specific plastic used.
Cuff And Balloon Features
Many breathing tubes include a cuff near the end that inflates like a tiny balloon. This cuff seals the airway inside the windpipe, preventing air leaks and stopping fluids from entering the lungs. It’s a simple yet vital feature that improves ventilation efficiency and patient safety.
Some cuffs are designed to be low-pressure and high-volume to reduce pressure on the trachea walls, minimizing tissue damage. Others might use foam or gel to provide a better seal. Have you ever thought about how such a small part can make a big difference in keeping a patient safe during intubation?
Size Variations
Breathing tubes come in a range of sizes to fit patients of all ages and body types, from tiny infants to adults. The size is measured by the internal diameter of the tube, which affects how much air can pass through. Choosing the right size is critical; a tube too small won’t provide enough airflow, while one too large can cause injury.
Hospitals often keep a variety of sizes on hand to match the patient’s anatomy precisely. Next time you hear about intubation, consider how much thought goes into selecting the perfect tube size to make the procedure both safe and effective.
Visual Characteristics
Understanding the visual characteristics of a breathing tube can make a big difference if you ever need to identify or assist with one. These tubes aren’t just simple hollow cylinders—they come with specific features designed to make them easy to use and recognize. Let’s break down what you’ll see when you look closely at a breathing tube.
Color Coding
Most breathing tubes use color coding to indicate their size and type. This helps healthcare professionals pick the right tube quickly, especially in urgent situations. You’ll often notice bright colors like blue, green, or purple on the tube’s connectors or body.
For example, a green band might indicate a size 7.0 tube, while a purple one could mean size 6.0. Have you ever wondered how a nurse or doctor can grab the correct tube without second-guessing? That’s the power of color coding.
Markings And Measurements
Look closely, and you’ll see numbers and lines running along the tube’s length. These markings show how far the tube has been inserted into the airway. It’s crucial for ensuring the tube is placed correctly and safely.
These measurements are usually printed in centimeters, making it easy to track insertion depth. If you’ve ever been curious about how medical staff know the tube is in the right spot, these markings are part of the answer.
Connector Types
The end of the breathing tube usually has a connector that links it to other devices like ventilators or breathing bags. These connectors come in different shapes and sizes to fit various equipment securely.
Some connectors are standard 15mm, designed to fit most machines, while others might be specialized for pediatric or emergency use. Have you noticed how some tubes snap or twist into place? Those connector types ensure a tight, leak-free fit, which is vital for effective breathing support.
How Breathing Tubes Are Inserted
A breathing tube is a thin, flexible tube used in medical procedures. It is inserted through the mouth or nose into the airway. This helps patients breathe during surgery or critical care situations.
Inserting a breathing tube is a crucial procedure in medical settings, especially during surgeries or emergencies. This process ensures that patients receive the necessary oxygen when they cannot breathe on their own. Understanding how these tubes are inserted can ease any anxiety you might have if you or a loved one needs this procedure.Preparation Steps
Before inserting a breathing tube, healthcare professionals prepare the patient and the required equipment. The patient is typically given a sedative or anesthesia to ensure comfort and prevent movement. The healthcare provider will gather essential tools, including the breathing tube, a laryngoscope, and any necessary monitoring devices.Insertion Process
The insertion of a breathing tube involves careful precision. The healthcare provider uses a laryngoscope to view the vocal cords and guide the tube into the trachea. The tube is then gently advanced until it is in the correct position, ensuring that it does not cause any trauma to the airways.Verification Methods
Once the tube is placed, verifying its correct position is crucial. The provider may use several methods, such as listening to breath sounds with a stethoscope or using a capnography device to measure carbon dioxide levels. Another common method is taking a chest X-ray to visually confirm the tube’s placement. Have you ever thought about how these procedures can save lives in critical situations? Understanding the steps involved can demystify the process and provide reassurance about the care you or your loved ones receive.Care And Maintenance
Taking care of a breathing tube is essential to keep it working properly and to avoid infections or other issues. Proper maintenance ensures comfort and safety for anyone relying on this medical device. You might be surprised how small actions in daily care can make a big difference.
Cleaning Procedures
Cleaning your breathing tube regularly prevents buildup of mucus and bacteria. Use sterile water or saline solution to rinse the tube gently. Avoid harsh chemicals that can damage the tube’s material.
Make cleaning part of your daily routine. If you notice any discoloration or unpleasant odor, it’s a sign to clean it more thoroughly. Always wash your hands before handling the tube to keep germs away.
Monitoring For Complications
Watch for signs like redness, swelling, or discomfort around the tube site. These could indicate infection or irritation. If your breathing feels obstructed or the tube seems loose, seek medical advice immediately.
Keep an eye on any changes in your breathing patterns. Sudden coughing or difficulty speaking might mean the tube needs adjustment. Your awareness is a key part of maintaining your health with a breathing tube.
Replacement Timing
Breathing tubes don’t last forever. They need to be replaced regularly to prevent damage and infection. Your healthcare provider will give you a schedule, but also trust your instincts if something feels wrong.
Delaying replacement can lead to blockages or leaks, which can be dangerous. Mark your calendar for replacements and have a backup tube ready if possible. How often do you check your medical supplies to ensure everything is up to date?
Common Myths And Facts
Breathing tubes often evoke strong images in people’s minds, shaped more by movies and hearsay than by reality. Separating myths from facts can help you feel more informed and less anxious if you or a loved one ever need one. Let’s clear up common misunderstandings and reveal what these devices really look like and how they work.
Misconceptions About Appearance
Many imagine breathing tubes as large, intimidating devices that cause discomfort or pain. In truth, they are usually slim, flexible tubes made from soft plastic designed to fit comfortably in the airway. You might be surprised to learn that some tubes are barely thicker than a pencil.
People often picture breathing tubes as one-size-fits-all, but they come in various sizes to suit different ages and medical needs. The clear or slightly tinted material helps medical staff easily check for blockages or secretions. If you’ve seen a breathing tube in a movie or TV show, keep in mind that actual tubes prioritize patient comfort and safety over dramatic effect.
Clarifying Usage
Breathing tubes are not just for emergencies or surgeries; they have a range of uses depending on the medical situation. For example, they help patients breathe during anesthesia, assist those with severe respiratory illnesses, and support long-term ventilation in intensive care.
Have you ever wondered how medical teams decide when to use a breathing tube? It’s based on careful assessment of your breathing ability, oxygen levels, and overall health. This decision is never taken lightly because the goal is always to provide the least invasive support necessary.
Understanding the real look and function of breathing tubes can ease fears and empower you to ask the right questions if you ever face this situation. What concerns do you have about medical devices that could help your breathing?

Credit: www.ems1.com

Credit: goodmenproject.com
Frequently Asked Questions
What Does A Breathing Tube Look Like?
A breathing tube is a flexible, clear or slightly tinted plastic tube. It usually has markings and a cuff near the end to seal the airway. The size varies depending on patient needs, and it often connects to ventilators or oxygen supplies.
How Is A Breathing Tube Used In Medical Settings?
Breathing tubes are inserted into the trachea to maintain an open airway. They assist with ventilation during surgery or critical illness. The tube ensures oxygen delivery and carbon dioxide removal when patients cannot breathe independently.
What Materials Are Breathing Tubes Made From?
Breathing tubes are commonly made from medical-grade PVC or silicone. These materials are flexible, durable, and safe for patient use. They allow easy insertion and reduce the risk of irritation or allergic reactions.
Can You See The Breathing Tube Inside The Throat?
Yes, during intubation, medical professionals visualize the tube inside the throat using a laryngoscope. However, the tube is not visible externally once placed. Its position is confirmed by chest X-rays or capnography.
Conclusion
A breathing tube is a clear, flexible tube designed to help people breathe. It usually has a small balloon near the end to keep it in place. Doctors use it during surgery or emergencies. Seeing and understanding this tube can ease worries about medical care.
Knowing its shape and purpose helps patients feel more comfortable. Breathing tubes play a key role in saving lives. They are simple but very important tools in healthcare.