Have you ever wondered how breathing support can be given without tubes or surgery? Non Invasive Ventilation (NIV) is a simple yet powerful way to help your lungs work better.
Whether you or someone you care about struggles with breathing issues, understanding NIV can make a big difference. You’ll discover what Non Invasive Ventilation is, how it works, and why it might be the solution you need. Keep reading to learn how this gentle method could change your breathing—and your life.
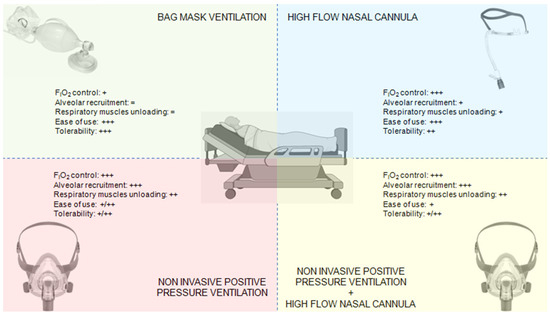
Credit: www.mdpi.com
Basics Of Non Invasive Ventilation
Non Invasive Ventilation (NIV) is a medical technique that helps people breathe without using invasive methods. It supports breathing through external devices instead of tubes placed inside the body. This approach is often used for patients with breathing difficulties due to various health conditions.
Understanding the basics of NIV is important for patients and caregivers. It explains how this treatment works and the types available. This knowledge helps in making informed decisions about respiratory care.
Definition And Purpose
Non Invasive Ventilation is a way to assist breathing without surgery or tubes inside the airway. It uses masks or similar devices to deliver air or oxygen. The main goal is to improve breathing and oxygen levels in the blood.
NIV is used to treat conditions like chronic obstructive pulmonary disease (COPD), sleep apnea, and other respiratory problems. It helps reduce the effort needed to breathe and prevents lung collapse.
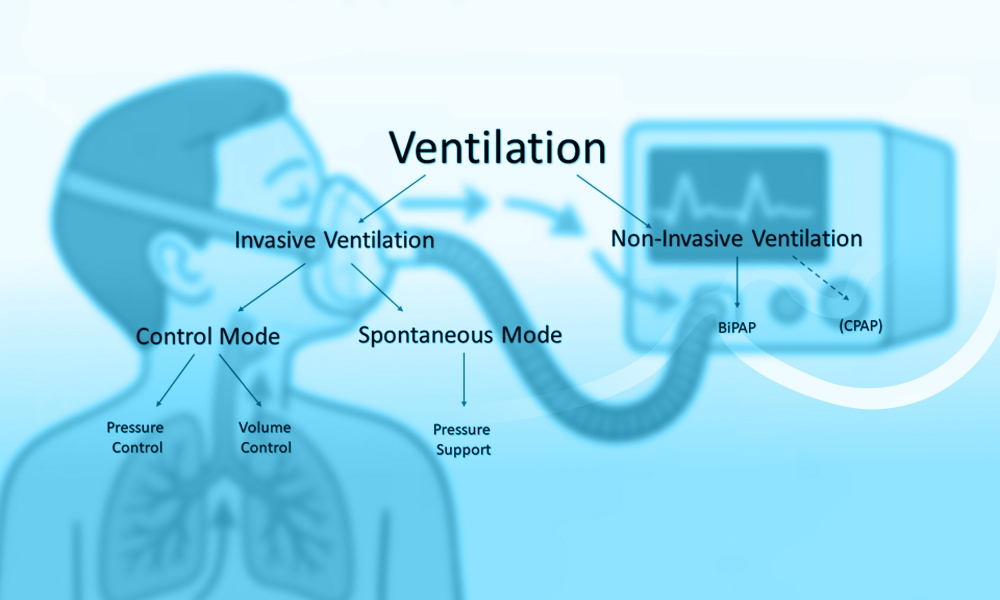
Types Of Non Invasive Ventilation
There are several types of NIV based on how air is delivered and controlled:
- CPAP (Continuous Positive Airway Pressure):Provides constant air pressure to keep airways open.
- BIPAP (Bilevel Positive Airway Pressure):Delivers two levels of pressure – one for inhaling and one for exhaling.
- High-Flow Nasal Cannula (HFNC):Supplies warm, humidified oxygen at high flow rates through nasal prongs.
Each type suits different medical needs and patient comfort levels.
How It Works
NIV works by pushing air into the lungs through a mask or nasal device. This air pressure helps keep the airways open and improves oxygen flow. The machine adjusts the pressure based on the patient’s breathing.
This support reduces the work of breathing and helps the lungs get enough oxygen. The patient can breathe more easily and rest better during treatment. The devices are designed to be comfortable and easy to use.
Common Uses And Benefits
Non Invasive Ventilation (NIV) plays a crucial role in treating various respiratory issues without the need for surgical procedures. Understanding its common uses and benefits can help you see why it’s often preferred in many medical situations. Let’s look at the conditions it treats, why it’s better than invasive methods, and how it improves patient comfort.
Conditions Treated
NIV is commonly used for patients experiencing respiratory failure due to chronic obstructive pulmonary disease (COPD), pneumonia, or acute asthma attacks. It also helps those with sleep apnea and certain neuromuscular disorders that weaken breathing muscles.
If you’ve ever witnessed someone struggling to breathe, you know how critical timely support is. NIV supports breathing without the risks of a tube in the windpipe, making it suitable for patients who need temporary help or cannot tolerate invasive ventilation.
Advantages Over Invasive Methods
One big advantage of NIV is that it avoids intubation, which means no tubes go down the throat. This reduces the risk of infections like pneumonia that can happen with invasive ventilation.
It also lowers hospital stays and medical costs by promoting faster recovery. You might wonder, why would anyone choose a method that feels less direct? NIV provides effective support while minimizing complications and preserving natural airway defenses.
Impact On Patient Comfort
Comfort is a major factor in choosing NIV. Instead of being sedated or restrained, patients remain awake and able to communicate.
Many find the masks used in NIV easier to tolerate than tubes, allowing them to eat, drink, and move more freely. This comfort can reduce anxiety and improve cooperation, which are essential for better outcomes.
Equipment And Technology
Non-invasive ventilation (NIV) uses special equipment to help people breathe without tubes inside their windpipe. The technology focuses on comfort and efficiency. It supports breathing by delivering air through masks or other interfaces. Modern NIV machines are compact and easy to use.
The equipment includes different types of masks, machines, and settings. Each part plays a key role in providing effective breathing support. Understanding the technology helps patients and caregivers use NIV safely and comfortably.
Masks And Interfaces
Masks form the main connection between the patient and the ventilator. They come in various styles:
- Nasal masks: Cover only the nose.
- Full face masks: Cover both nose and mouth.
- Nasal pillows: Fit directly into the nostrils.
Each mask type fits differently to ensure comfort and prevent air leaks. Soft cushions and adjustable straps improve the fit. Proper mask choice reduces skin irritation and improves breathing support.
Ventilator Machines
Ventilator machines deliver pressurized air to assist breathing. They vary in size and features but share common functions:
- Provide continuous or bi-level pressure.
- Monitor breathing patterns.
- Alert users to problems like leaks or disconnections.
Modern ventilators are lightweight and portable. They often include batteries for use during power outages or travel.
Settings And Adjustments
Settings on NIV machines control air pressure and timing. These adjustments tailor breathing support to the patient’s needs. Common settings include:
- Inspiratory pressure: Air pressure during inhalation.
- Expiratory pressure: Pressure during exhalation.
- Backup rate: Minimum breaths per minute.
Healthcare providers adjust these settings based on patient comfort and medical condition. Some machines also offer humidification to keep airways moist. Proper settings improve therapy effectiveness and patient comfort.
Procedure And Patient Experience
Non-invasive ventilation (NIV) helps patients breathe without the need for tubes inside their airways. The process involves a mask that fits over the nose or mouth. This section explains what patients can expect during the procedure and how it feels to use NIV.
Preparation And Setup
The healthcare team starts by choosing the right mask size. They check the patient’s comfort and ensure a good seal. The machine is connected to the mask with flexible tubing. The air pressure settings are adjusted based on the patient’s needs. Staff explain how to wear the mask and what to expect. Patients often lie down or sit in a relaxed position for better comfort.
Monitoring During Use
Medical staff watch the patient closely during NIV use. They check oxygen levels and breathing patterns. The machine may display pressure and flow rates. Nurses listen for any signs of distress or discomfort. Adjustments to pressure or mask fit happen as needed. Regular checks help ensure therapy works well and remains safe.
Potential Side Effects
- Skin irritation or redness where the mask touches
- Dry mouth or nose due to airflow
- Feeling of pressure or discomfort from the mask
- Possible bloating or stomach discomfort
- Rarely, eye irritation if air leaks near eyes
Most side effects are mild and can be managed. Patients should report any discomfort to the care team. Proper mask fit and humidification help reduce problems.
Challenges And Limitations
Non Invasive Ventilation (NIV) offers significant benefits for many patients, but it is not without its challenges and limitations. Understanding these hurdles helps you set realistic expectations and prepare better for the treatment journey. Knowing when NIV might not work and how to handle common issues can improve your experience and outcomes.
When Niv May Not Be Suitable
NIV is not a one-size-fits-all solution. If you have severe respiratory failure or need immediate airway protection, NIV might not be the right choice.
Conditions like facial trauma, excessive secretions, or a decreased level of consciousness can make it difficult to use NIV effectively. In such cases, invasive ventilation might be necessary.
Ask yourself: Are there any physical or medical reasons that could prevent you from tolerating the mask or the pressure settings? Being honest with your healthcare provider about discomfort or breathing difficulties is crucial.
Common Complications
Using NIV can sometimes lead to side effects that affect comfort and effectiveness.
- Skin irritation:Masks can cause pressure sores or redness, especially if worn for long periods.
- Dry mouth and nasal congestion:Airflow might dry out your mucous membranes, causing discomfort.
- Gastric distension:Swallowing air during NIV can lead to bloating and nausea.
- Eye irritation:Air leaks near the eyes may cause dryness or redness.
Recognizing these issues early can save you from bigger problems later.
Troubleshooting Tips
If you experience discomfort or complications, simple adjustments can make a big difference.
- Try different mask sizes or types to reduce pressure points and improve the seal.
- Use humidifiers to add moisture to the airflow, easing dryness in your mouth and nose.
- Adjust the pressure settings with your healthcare provider’s help to balance support and comfort.
- Practice relaxation techniques to reduce anxiety, which can worsen breathing difficulties.
Have you noticed specific discomforts during NIV? Keeping a diary of your symptoms and discussing them with your care team can lead to better, personalized solutions.

Credit: www.wikiwand.com
Future Trends In Non Invasive Ventilation
Non Invasive Ventilation (NIV) is a growing field in respiratory care. The future of NIV promises exciting developments. New technologies and expanding uses are shaping its course. Let’s explore these future trends.
Technological Advances
Technology in NIV is advancing rapidly. Improved sensors make devices more precise. Smart algorithms help customize treatment for each patient. Wireless connectivity allows remote monitoring. These advances enhance patient comfort and outcomes.
Expanding Applications
NIV applications are broadening. It’s not just for sleep apnea anymore. COPD and asthma patients benefit from NIV now. It’s also useful in emergency settings. This expansion means more patients receive non-invasive care.
Research And Innovations
Research in NIV is ongoing. Scientists are exploring new materials for masks. They’re also studying the impact of NIV on different conditions. Innovations aim to make NIV more accessible. The goal is to improve patient care and reduce hospital stays.

Credit: www.tandfonline.com
Frequently Asked Questions
What Is Non-invasive Ventilation Used For?
Non-invasive ventilation helps patients with breathing difficulties. It supports lung function without needing a tube in the airway. It is commonly used for conditions like COPD, sleep apnea, and respiratory failure.
How Does Non-invasive Ventilation Work?
Non-invasive ventilation delivers air through a mask or nasal prongs. It keeps airways open and improves oxygen flow. This method reduces the effort needed to breathe and prevents lung collapse.
What Are The Benefits Of Non-invasive Ventilation?
Non-invasive ventilation reduces the risk of infections linked to invasive tubes. It improves breathing comfort and helps avoid hospital stays. Patients recover faster with fewer complications using this method.
Who Can Use Non-invasive Ventilation?
Patients with chronic or acute respiratory issues can use it. It suits those with COPD, asthma exacerbations, or neuromuscular diseases. A healthcare provider determines suitability based on individual health needs.
Conclusion
Non-invasive ventilation helps people breathe without surgery. It uses a mask to support breathing gently. This method reduces risks and speeds recovery. Many patients find it comfortable and effective. Doctors recommend it for certain lung and heart problems. Understanding how it works can ease worries.
Always follow medical advice for best results. Non-invasive ventilation offers a safer way to improve breathing. It plays a key role in modern healthcare.