Have you ever wondered how fresh, clean air is delivered into spaces that need constant ventilation? Understanding positive pressure ventilation can unlock the secret behind keeping rooms fresh, safe, and comfortable.
Whether you’re managing a home, office, or industrial space, knowing how this system works can make a big difference in your environment. Keep reading, and you’ll discover how positive pressure ventilation can protect your health, improve air quality, and even save you money.
Ready to learn something that could change the way you breathe indoors? Let’s dive in.

Credit: www.jacc.org
Basics Of Positive Pressure Ventilation
Understanding the basics of Positive Pressure Ventilation (PPV) is key if you want to grasp how this life-saving technology supports breathing. PPV works by pushing air into the lungs, helping patients who struggle to breathe on their own. Knowing how it functions and the types of devices involved can help you appreciate its vital role in healthcare and emergency situations.
How Positive Pressure Works
Positive Pressure Ventilation delivers air by increasing the pressure inside the lungs, which forces air to flow in. Unlike normal breathing, where air moves in due to negative pressure created by the diaphragm, PPV actively pushes air into the lungs.
This process helps open the airways and improves oxygen exchange, especially when a person’s natural breathing is weak or stopped. Have you ever noticed how blowing air into a balloon requires more effort than just letting air out? PPV works similarly, using controlled pressure to inflate the lungs.
Types Of Ventilation Devices
Various devices provide positive pressure ventilation, each suited to different situations and patient needs. Here are some common types:
- Manual Resuscitators (Bag-Valve Masks):These hand-operated devices allow you to squeeze a bag to push air into the lungs. They are widely used in emergencies for quick ventilation support.
- Mechanical Ventilators:These machines deliver precise volumes and pressures of air automatically. They are common in hospitals for patients needing long-term or controlled breathing assistance.
- CPAP and BiPAP Machines:These non-invasive devices provide continuous or bi-level positive airway pressure, often used for sleep apnea or less severe respiratory issues.
Which type of device would best fit your needs or environment? Understanding these options helps you make informed decisions in critical moments.
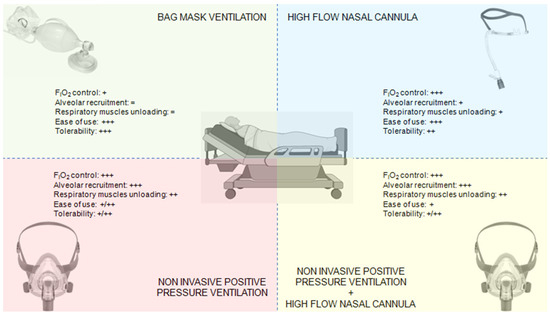
Credit: www.mdpi.com
Health Benefits Of Positive Pressure Ventilation
Positive pressure ventilation offers several health benefits. It supports breathing by pushing air into the lungs. This helps patients with weak lung function or breathing difficulties. The therapy improves oxygen supply and eases the effort of breathing.
Improved Oxygen Delivery
Positive pressure ventilation increases the amount of oxygen entering the lungs. This helps the blood carry more oxygen to the body. Better oxygen delivery supports vital organs like the brain and heart. Patients often feel more energetic and less tired.
Enhanced Lung Function
The pressure helps keep airways open during breathing. This prevents lung collapse and improves lung expansion. Improved lung function reduces infections and other complications. It also helps clear mucus and makes breathing easier.
Reduced Work Of Breathing
Positive pressure ventilation lowers the effort needed to breathe. It reduces strain on respiratory muscles. This allows patients to rest and recover faster. Less work breathing means less fatigue and discomfort.
Applications In Medical Settings
Positive Pressure Ventilation (PPV) plays a vital role in many medical settings. It helps support patients who cannot breathe well on their own. PPV pushes air into the lungs using controlled pressure. This method improves oxygen delivery and eases breathing effort.
Hospitals use PPV in various ways. It assists patients during critical moments and manages chronic breathing problems. The technology adapts to different needs, making it a key tool in healthcare.
Use In Critical Care
In critical care, PPV supports patients with severe breathing issues. It maintains airway pressure and keeps lungs open. This prevents lung collapse and helps gas exchange.
Ventilators use PPV in intensive care units (ICUs). They assist patients with trauma, surgery recovery, or respiratory failure. Care teams monitor ventilation closely to match patient needs.
Role In Respiratory Therapy
Respiratory therapists use PPV to treat lung diseases. It aids patients with conditions like pneumonia, COPD, or asthma. PPV reduces breathing work and improves oxygen levels.
Therapists adjust settings on devices to optimize support. They also educate patients on using PPV safely at home.
Benefits For Sleep Apnea Patients
PPV is common for treating sleep apnea. Devices like CPAP deliver steady air pressure to keep airways open.
This helps patients sleep better and reduces health risks. Improved breathing lowers daytime tiredness and heart strain.
Safety And Comfort Features
Safety and comfort are key in positive pressure ventilation. These systems help patients breathe easier while keeping them safe. Advanced features control pressure and watch patient health closely. These features reduce risks and improve the overall experience. Comfort is a priority, ensuring patients feel relaxed during use.
Pressure Regulation
Pressure regulation keeps air flow steady and safe. It prevents too much pressure that can harm lungs. The system adjusts pressure based on the patient’s needs. This avoids discomfort and possible lung injury. Smooth pressure changes help patients breathe naturally. Some devices allow manual or automatic pressure control for safety.
Patient Monitoring Systems
Patient monitoring systems track breathing and vital signs. Sensors measure oxygen levels, airflow, and respiratory rate. Alerts notify caregivers if something goes wrong. Continuous monitoring helps catch problems early. Data can be displayed on screens for easy reading. This feature supports quick responses and better patient care.
Challenges And Considerations
Positive pressure ventilation requires careful monitoring to avoid lung injury from too much pressure. Choosing the right settings depends on the patient’s condition and needs. Staff must be trained to recognize complications quickly for safe use.
Challenges and Considerations Positive Pressure Ventilation (PPV) is a critical medical intervention that can save lives. Yet, it comes with its own set of challenges and considerations. Understanding these nuances can make a significant difference in outcomes. One challenge is ensuring the correct pressure settings. If the pressure is too high, it can damage lung tissue. Too low, and it might not be effective. You must also consider the patient’s condition. For instance, some patients may experience discomfort or anxiety during PPV. How will you address these issues? Regular monitoring is crucial. It helps in adjusting the settings based on the patient’s response. This can prevent potential complications down the line. Making informed decisions is key. Are you ready to handle the intricacies of PPV?Potential Risks
PPV is not without risks. Over-inflation of the lungs can occur, leading to a pneumothorax. This is a condition where air leaks into the space between the lung and chest wall. There’s also a risk of decreased cardiac output. This happens when increased pressure in the chest affects the heart’s function. Monitoring is essential to mitigate these risks. Consider the risk of infection. Equipment needs to be sterile to avoid introducing pathogens. How vigilant are you in maintaining hygiene protocols? Patient tolerance is another concern. Some may experience agitation or fear during ventilation. Are you prepared to offer reassurance and support?When To Avoid Positive Pressure Ventilation
PPV is not suitable for everyone. Patients with certain conditions should avoid it. For instance, those with untreated pneumothorax are at risk of worsening their condition. Consider patients with severe hypotension. PPV may exacerbate low blood pressure, posing more harm than benefit. Those with facial injuries or obstructions might find PPV ineffective. Alternative methods should be considered in such scenarios. It’s essential to evaluate each case individually. Are there safer options available for the patient in front of you?
Credit: www.jacc.org
Future Trends And Innovations
The future of positive pressure ventilation shows promising trends and innovations. These developments aim to improve patient comfort, treatment effectiveness, and healthcare accessibility. Emerging technologies focus on making ventilators smarter and more connected. This helps healthcare providers deliver better care in various settings.
Advancements In Ventilation Technology
Ventilators are becoming smaller and more portable. New devices use advanced sensors to adjust airflow automatically. This ensures patients receive precise breathing support. Battery life improvements allow longer use outside hospitals. Materials used in devices are becoming lighter and more durable. Some models offer noise reduction for patient comfort. Software updates enable better monitoring and data collection. Artificial intelligence helps predict patient needs and adjust therapy quickly.
Integration With Telemedicine
Telemedicine integration is transforming how ventilators are managed. Remote monitoring allows doctors to track patient status in real time. This reduces hospital visits and saves time. Patients can receive ventilation support at home safely. Data from devices can be shared instantly with healthcare teams. This helps in early detection of issues and faster intervention. Telemedicine also supports training for caregivers and patients. It improves access to expert care in remote areas.
Frequently Asked Questions
What Is Positive Pressure Ventilation?
Positive pressure ventilation is a method that pushes air into the lungs using a machine. It helps patients breathe when they cannot do so effectively on their own. This technique ensures oxygen delivery and carbon dioxide removal, supporting critical respiratory function in medical settings.
How Does Positive Pressure Ventilation Work?
It delivers air under pressure through a tube into the lungs. This pressure inflates the lungs and helps keep airways open. The machine controls the volume and rate of airflow based on patient needs. It improves oxygen exchange and reduces breathing effort.
When Is Positive Pressure Ventilation Used?
It is used during surgery, respiratory failure, or severe lung conditions. Patients unable to breathe adequately benefit from this support. It helps maintain oxygen levels and removes carbon dioxide, preventing respiratory complications and supporting recovery.
What Are The Benefits Of Positive Pressure Ventilation?
This ventilation improves oxygen delivery and lung expansion. It reduces work of breathing and prevents lung collapse. It supports critical patients by stabilizing respiratory function. Additionally, it allows precise control over breathing patterns in intensive care.
Conclusion
Positive pressure ventilation helps move air into the lungs effectively. It supports breathing in many medical situations. This method improves oxygen delivery and keeps airways open. Health workers use it to assist patients who struggle to breathe. Understanding this technology can ease worries about its use.
It plays a key role in saving lives daily. Knowing how it works helps you appreciate medical care better. Simple but powerful—positive pressure ventilation supports breathing safely and clearly.





