When assessing an infant’s ventilation status, every second counts. You need to know exactly what to look for to make quick, confident decisions that could save a tiny life.
It’s not just about checking breathing—it’s about understanding subtle signs and responding the right way. You’ll discover clear, simple steps to evaluate an infant’s breathing effectively. By the end, you’ll feel more prepared and confident to act when it matters most.
Keep reading—your knowledge could make all the difference.

Credit: www.docsity.com
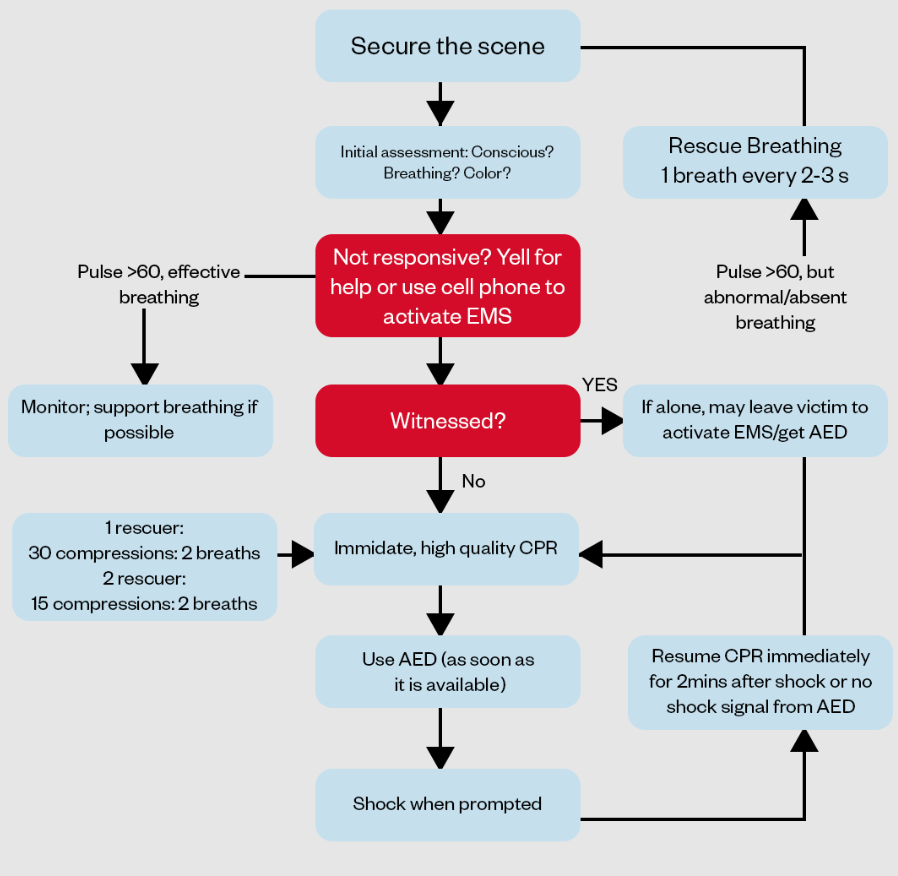
Signs Of Effective Ventilation
Recognizing the signs of effective ventilation in an infant is crucial for timely and appropriate intervention. You need to look beyond just the mechanical process of breathing and focus on clear, observable indicators that show the infant is receiving adequate oxygen. These signs can guide you in deciding whether to continue, adjust, or stop ventilation efforts.
Chest Rise And Fall
One of the most visible signs of effective ventilation is the chest rising and falling with each breath. When you provide breaths, watch closely to see if the chest expands smoothly and symmetrically.
If the chest does not rise, it could mean the airway is blocked or the breaths are not strong enough. This simple observation can save precious seconds—have you ever noticed how subtle changes in chest movement tell you more than any machine?
Skin Color Changes
Skin color is a quick indicator of oxygenation status. A healthy pink hue suggests good oxygen delivery, while a bluish or pale tint signals distress.
Keep in mind, changes in skin color might be subtle at first, so use natural light when possible. Have you ever caught a slight bluish tint around the lips or fingertips that made you act faster? That’s your cue to reassess ventilation.
Heart Rate Response
The infant’s heart rate responds quickly to ventilation quality. A rising heart rate usually means the baby is getting enough oxygen.
If the heart rate remains low or falls, it signals poor oxygen delivery despite ventilation efforts. Monitoring this vital sign closely helps you decide if you need to change your approach immediately to support the infant’s recovery.
Common Causes Of Ventilation Problems
Understanding common causes of ventilation problems in infants is crucial. Early recognition helps provide timely care. Ventilation issues can arise from several sources. Each cause affects breathing differently. Identifying the cause guides proper treatment and support.
Airway Obstruction
Airway obstruction blocks the flow of air to the lungs. It can occur due to mucus, swelling, or foreign objects. Infants have small airways that are easily blocked. Signs include noisy breathing, choking, or difficulty crying. Clearing the airway quickly is essential to restore ventilation.
Respiratory Distress
Respiratory distress means the infant struggles to breathe well. Common causes include infections like pneumonia or bronchiolitis. The infant may breathe fast or show chest retractions. Low oxygen levels cause skin to look pale or blue. Monitoring breathing effort and oxygen is vital.
Neuromuscular Issues
Neuromuscular problems affect muscles that control breathing. Conditions like muscular dystrophy or nerve damage may cause weak breaths. Infants may have poor chest movement or shallow breathing. These issues reduce the ability to ventilate properly. Supportive care and breathing assistance might be necessary.
Rapid Assessment Techniques
Assessing an infant’s ventilation status quickly is crucial in emergencies. Rapid assessment techniques help you gather essential information without wasting valuable time. These methods give you a clear picture of how well the infant is breathing and if immediate intervention is needed.
Visual Inspection
Look closely at the infant’s chest and abdomen. Notice if the chest rises and falls evenly with each breath. Irregular or shallow breathing can signal trouble.
Check for signs like nasal flaring, grunting, or the use of accessory muscles around the neck and ribs. These often indicate increased effort to breathe. Have you ever caught subtle signs that changed your approach to care?
Auscultation
Listening to breath sounds is a quick way to detect abnormalities. Use a stethoscope to listen over both lungs and the upper airway.
Pay attention to wheezes, crackles, or absence of breath sounds. These sounds can tell you if there’s an obstruction, fluid, or collapse in the lungs. A clear, quiet chest isn’t always a good sign—it might mean no air is moving.
Pulse Oximetry
This non-invasive tool measures oxygen saturation in the blood. Place the sensor gently on the infant’s hand or foot to get a reading.
Normal oxygen levels usually range from 95% to 100%. Values below this can signal inadequate ventilation or oxygenation. Have you noticed how pulse oximetry readings can guide urgent decisions almost instantly?
Credit: www.protrainings.com
Immediate Actions To Take
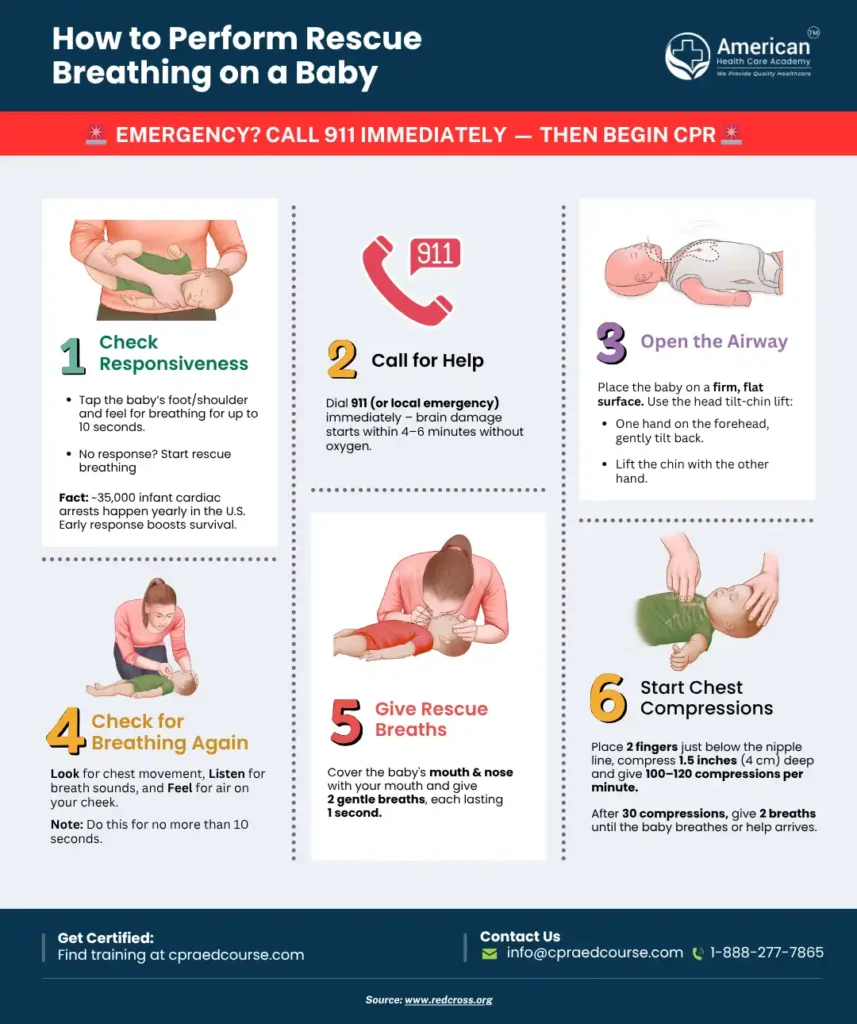
Check the infant’s chest rise and breathing sounds carefully. Observe skin color and listen for any breathing difficulties immediately. Act quickly if signs of poor ventilation appear.
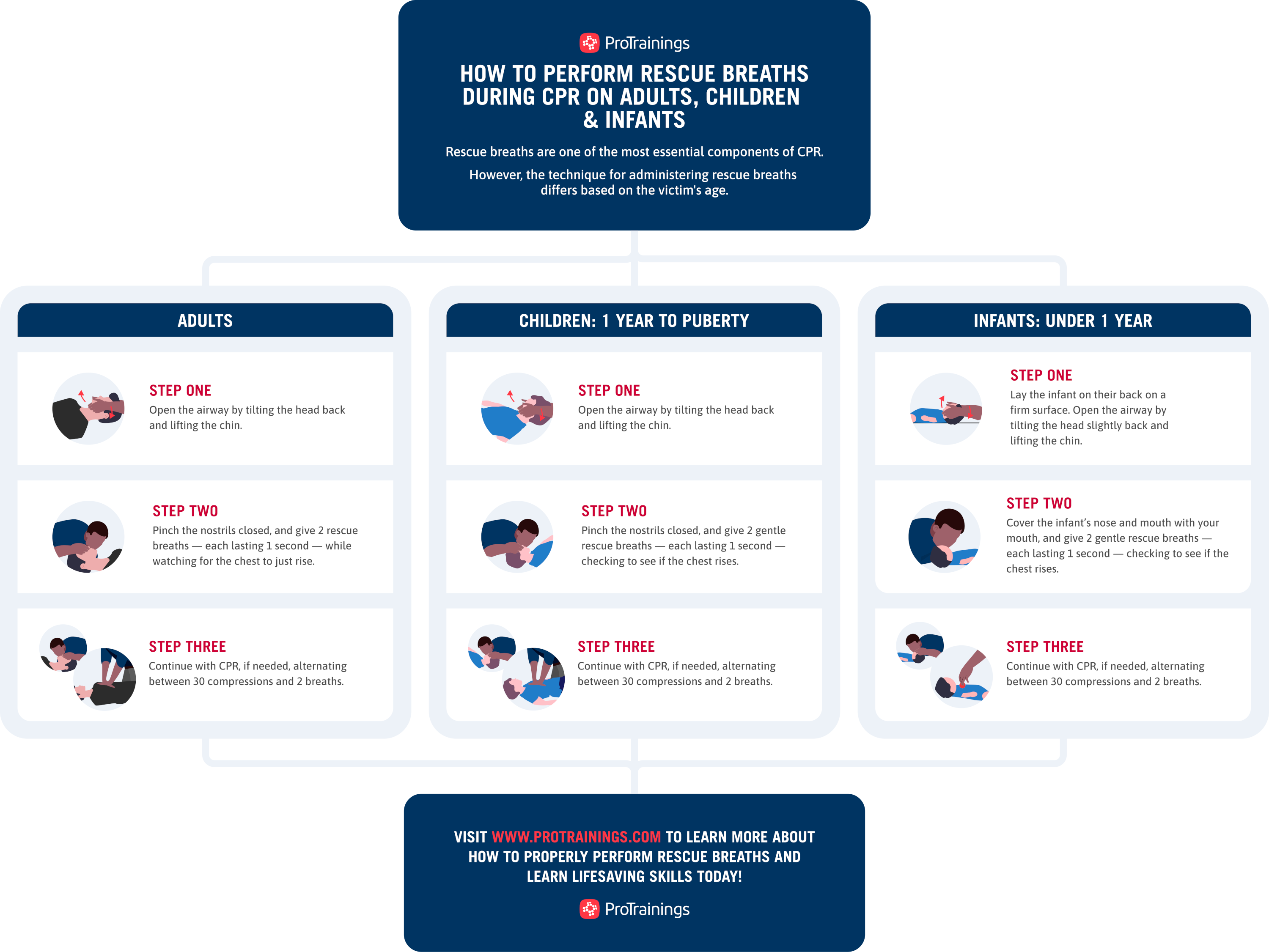
Immediate assessment of an infant’s ventilation status is crucial. Quick, effective actions can save lives. Every second counts. Here are the steps to take:Opening The Airway
Ensure the airway is clear. Gently tilt the infant’s head back. Lift the chin slightly. This aligns the airway for better airflow. Check for visible obstructions. Remove them carefully if present.Providing Positive Pressure Ventilation
If breathing is inadequate, use a bag-mask device. Position the mask over the infant’s mouth and nose. Create a good seal. Squeeze the bag gently. Deliver breaths at regular intervals. Monitor the chest for rise and fall.Calling For Advanced Support
If there’s no improvement, seek advanced help. Use emergency services immediately. Provide them with clear information. Stay with the infant until help arrives. Ensure continuous monitoring and support.Monitoring And Reassessment
Monitoring and reassessment are vital when checking an infant’s ventilation status. This process ensures the baby receives the right amount of air for healthy breathing. Careful observation helps spot any changes in breathing patterns or distress early. Quick responses can improve outcomes and avoid complications.
Continuous Observation
Keep a close watch on the infant’s breathing rate and effort. Look for signs like chest movement, nasal flaring, or grunting. Monitor oxygen levels using pulse oximetry regularly. Watch skin color for any signs of blueness or paleness. Observe the infant’s responsiveness and alertness during care.
Adjusting Ventilation Support
Change ventilation settings based on the infant’s current condition. Increase or decrease oxygen flow to keep saturation within safe limits. Modify pressure or volume on mechanical devices as needed. Always respond to signs of distress or improvement promptly. Consult guidelines and expert advice for safe adjustments.
Documenting Changes
Record all observations and interventions clearly. Note breathing rates, oxygen levels, and any changes made. Document the infant’s response to adjustments in ventilation support. Use charts or digital records for accurate tracking over time. Clear documentation helps maintain consistent care among healthcare providers.
Credit: cpraedcourse.com
Training And Preparedness
Training and preparedness are the backbone of accurately assessing an infant’s ventilation status. Without consistent practice and readiness, even the best knowledge can fall short during critical moments. You need to keep your skills sharp and your team in sync to respond effectively when every second counts.
Regular Simulation Drills
Simulation drills are not just about practice—they’re about building muscle memory. Running through emergency scenarios frequently helps you react faster and with more confidence. Try to include a variety of situations, such as airway obstructions or equipment failures, to prepare for any challenge.
Think about the last time you participated in a drill: Did you notice how your responses became quicker and more precise? That’s the power of repetition in a controlled setting. Schedule these drills regularly to keep your skills from getting rusty.
Equipment Familiarity
Knowing how to use ventilation equipment without hesitation can save an infant’s life. Spend time exploring each tool, from bag-valve masks to oxygen delivery systems, so you’re comfortable with their functions and limitations.
Have you ever reached for a device in a crisis only to realize you weren’t sure how to operate it? Avoid that moment by routinely checking and handling your equipment. This hands-on familiarity reduces errors and boosts your confidence during assessments.
Team Communication
Clear communication within your team ensures everyone knows their role and the infant’s condition at all times. Use simple, direct language and confirm instructions to avoid misunderstandings in high-pressure situations.
Ask yourself: Does your team have a communication protocol during ventilation assessments? If not, start by practicing briefings and debriefings after drills. This habit strengthens teamwork and improves overall outcomes for the infant.
Frequently Asked Questions
How Do You Assess An Infant’s Ventilation Status?
Check the infant’s breathing rate, chest movements, and listen for breath sounds. Use a pulse oximeter to monitor oxygen levels. Look for signs of respiratory distress like nasal flaring or grunting.
What Signs Indicate Poor Ventilation In Infants?
Poor ventilation signs include rapid or slow breathing, cyanosis, lethargy, and irregular chest movements. These suggest inadequate oxygen delivery and require immediate attention.
Why Is Monitoring Respiratory Rate Crucial In Infants?
Respiratory rate reflects lung function and oxygen needs. Changes can indicate distress or improvement, guiding timely interventions and ensuring effective ventilation support.
How Can Pulse Oximetry Aid In Ventilation Assessment?
Pulse oximetry measures oxygen saturation non-invasively. It helps detect hypoxia early and monitors response to treatment, ensuring the infant receives adequate ventilation and oxygenation.
Conclusion
Assessing an infant’s ventilation status takes careful attention. Watch their breathing rate and effort closely. Check for signs of distress or irregular patterns. Use simple tools to measure oxygen levels when possible. Quick action can prevent serious problems from developing.
Stay calm and act with confidence. Remember, early detection helps keep infants safe and healthy. Always trust your observations and seek help if unsure. This way, you ensure the best care for the little one.