When it comes to saving a life during a cardiac emergency, every second counts. You might already know that chest compressions and positive pressure ventilation are crucial steps in CPR.
But do you understand how to coordinate them effectively? Getting the timing right can make a huge difference in helping the heart and lungs work together. You’ll discover simple, clear ways to sync your breaths with chest compressions to give someone the best chance of survival.
Keep reading—you’ll learn techniques that could empower you to act confidently in a critical moment.
Basics Of Positive Pressure Ventilation
Positive Pressure Ventilation (PPV) is a key method to help patients breathe during emergencies. It pushes air into the lungs to keep oxygen flowing. Understanding its basics is vital for effective use alongside chest compressions. This section covers how PPV works and the types of devices used.
How Positive Pressure Ventilation Works
PPV forces air into the lungs through the mouth or nose. This helps inflate the lungs when a person cannot breathe well. The pressure created opens the airways and moves oxygen into the lungs. It also helps remove carbon dioxide from the body. The process supports the patient’s breathing until normal function returns.
During chest compressions, timing with ventilation is important. Coordinating breaths with compressions improves oxygen delivery to the heart and brain. The goal is to maintain blood flow and oxygen levels.
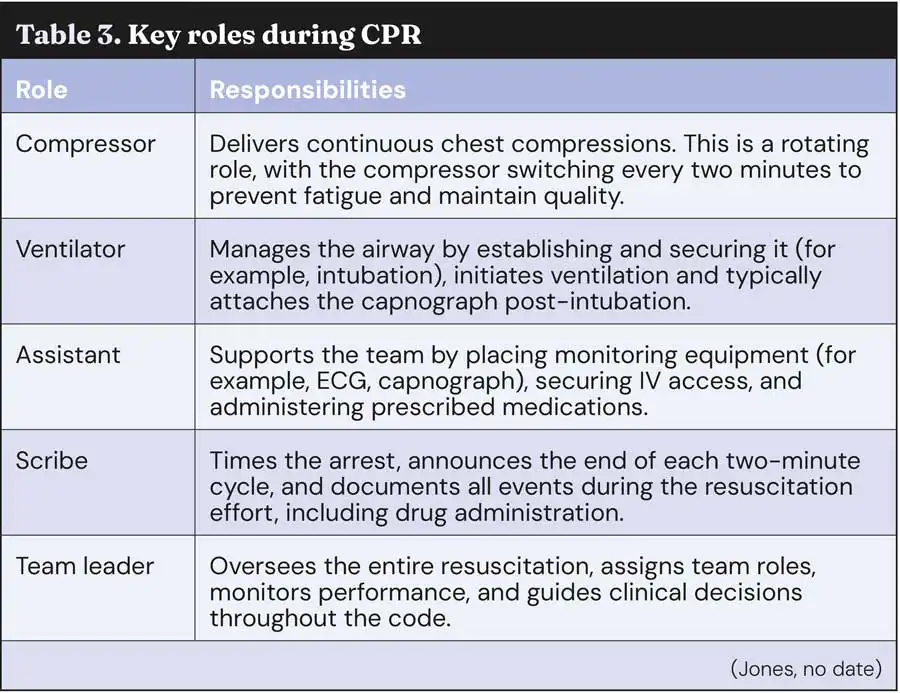
Types Of Ventilation Devices
- Bag-Valve-Mask (BVM):A hand-held device that delivers air by squeezing a bag. It fits over the patient’s face to provide breaths.
- Mechanical Ventilators:Machines that provide controlled air pressure and volume. Used in hospitals for long-term breathing support.
- CPAP and BiPAP:Devices that give continuous or variable air pressure. Mostly used for patients with breathing difficulties but awake.
- Endotracheal Tubes:Tubes inserted into the windpipe. Connected to ventilators for direct lung ventilation.
Choosing the right device depends on the situation and patient needs. Each device helps maintain airway pressure and oxygen flow during emergency care.

Credit: aneskey.com
Role Of Chest Compressions In Resuscitation
Chest compressions are the backbone of resuscitation efforts during cardiac arrest. They keep oxygen-rich blood flowing to vital organs, especially the brain and heart, buying crucial time until advanced care arrives. Understanding their role helps you perform them more confidently and effectively.
Importance Of Effective Compressions
Effective chest compressions are not just about pushing hard—they are about pushing smart. The right depth and rate ensure blood circulates adequately, which can be the difference between life and death.
Have you ever wondered why compressions sometimes fail despite your best effort? It’s often due to shallow compressions or interruptions that reduce blood flow.
Maintaining continuous, firm compressions at a rate of 100-120 per minute maximizes the chances of survival. Each pause allows the heart to lose momentum, so minimizing interruptions is critical.
Techniques For Optimal Chest Compressions
- Hand Placement:Place your hands on the center of the chest, right over the lower half of the sternum. This position targets the heart directly.
- Compression Depth:Push down at least 2 inches (5 cm) in adults. Shallow compressions won’t generate enough pressure to circulate blood.
- Allow Full Recoil:Let the chest rise completely between compressions. This helps the heart refill with blood.
- Consistent Rate:Keep a steady pace of 100-120 compressions per minute. You can count out loud or use a metronome app to stay on track.
- Minimize Interruptions:Try to keep pauses under 10 seconds, even when giving breaths or switching rescuers.
In my own experience, focusing on smooth, continuous compressions while coordinating breaths made a noticeable difference. The patient’s pulse returned faster and with more strength. How might your technique improve if you practiced these steps regularly?
Timing Coordination Between Ventilation And Compressions
Timing coordination between positive pressure ventilation and chest compressions is vital for effective resuscitation. Proper timing ensures that breaths support circulation without reducing blood flow. This balance improves oxygen delivery to the body and brain during CPR.
Good coordination reduces pauses in chest compressions. It also maximizes the chances of survival and recovery after cardiac arrest. Clear timing strategies help rescuers work smoothly and confidently.
Synchronizing Breaths With Compressions
Breaths should be delivered during brief pauses in chest compressions. This prevents air from pushing blood out of the chest and lowers the chance of lung injury. Each breath lasts about one second, enough to inflate the lungs.
Rescuers must watch for chest rise to confirm proper ventilation. Synchronizing breaths with pauses keeps circulation steady. It also allows oxygen to enter the lungs efficiently.
Avoiding Interruptions In Compressions
Minimizing breaks in chest compressions is critical. Interruptions reduce blood flow to the heart and brain. Rescuers should aim for less than 10 seconds of pause for breaths.
Using teamwork helps maintain continuous compressions. While one person gives breaths, another continues compressions without delay. Clear communication and practice improve timing and reduce errors.
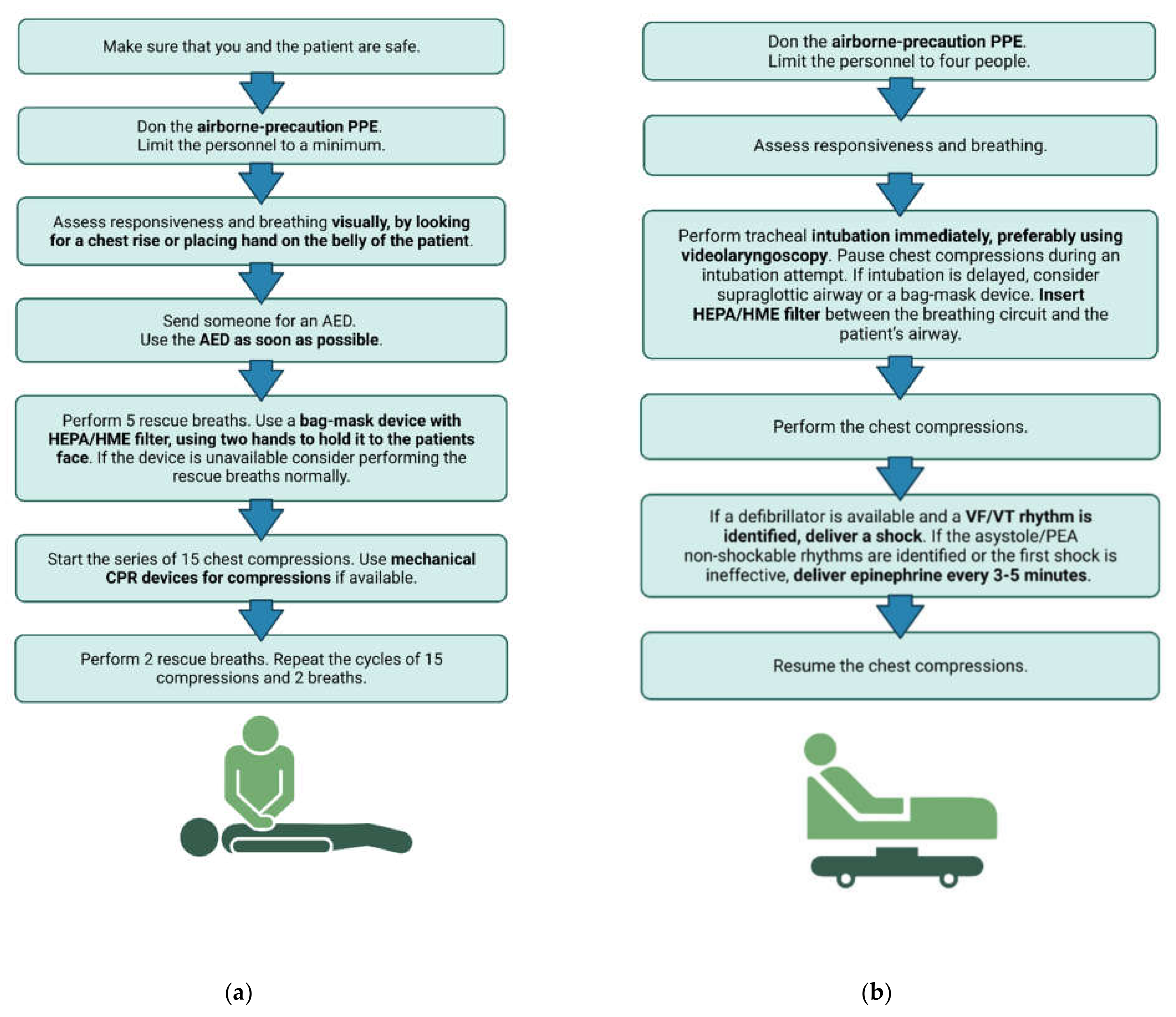
Credit: www.mdpi.com
Common Challenges And Solutions
Coordinating positive pressure ventilation (PPV) with chest compressions is a delicate balance. Challenges often arise that can reduce the effectiveness of resuscitation efforts. Understanding these obstacles and applying practical solutions can make a significant difference in patient outcomes.
Managing Airway Obstructions
Airway obstructions can block airflow during ventilation, making it harder to deliver breaths effectively. You might notice decreased chest rise or increased resistance when squeezing the bag. Quick identification is key to solving the problem.
Clearing the airway can involve repositioning the head or using suction to remove secretions. If you encounter persistent blockage, consider inserting an airway adjunct like an oropharyngeal or nasopharyngeal airway. These tools help keep the airway open and improve ventilation.
Have you ever struggled with a blocked airway during an emergency? Training on airway management can boost your confidence and improve your response time.
Preventing Hyperventilation
Hyperventilation is a common challenge when coordinating PPV with chest compressions. Delivering breaths too quickly or with excessive volume can increase intrathoracic pressure. This reduces blood return to the heart and lowers cardiac output.
Focus on providing slow, controlled breaths at the recommended rate—about one breath every 6 seconds. Use a timer or count out loud to keep your pace steady. Avoid squeezing the bag too hard; gentle pressure often achieves adequate chest rise.
Have you ever noticed how easy it is to speed up during high-stress moments? Practicing with feedback devices can help you maintain the right ventilation rate and volume every time.
Equipment Tips For Better Coordination
Using the right equipment helps keep chest compressions and positive pressure ventilation in sync. Clear communication and simple tools reduce delays and improve patient care. Proper setup ensures smooth teamwork during emergencies.
Coordinating positive pressure ventilation with chest compressions can be a delicate task requiring precision and teamwork. One of the most crucial aspects of this coordination is ensuring that your equipment is up to the task. Selecting the right tools and keeping them in optimal condition can make a world of difference. Let’s delve into some equipment tips that can enhance your coordination efforts and possibly save lives.Choosing The Right Ventilation Device
Selecting an appropriate ventilation device is not just about having the latest technology. It’s about finding a device that suits your team’s skill level and the patient’s needs. Consider devices with intuitive interfaces that reduce the risk of error during high-pressure situations. Some devices offer visual or audio cues to help synchronize with chest compressions. These features can be invaluable in maintaining the rhythm and efficiency of your resuscitation efforts. Remember, a device that integrates smoothly with your team’s workflow can significantly improve outcomes.Maintaining Equipment Readiness
Ensuring your equipment is ready to go at a moment’s notice is non-negotiable. Regular checks and maintenance should be part of your routine. Create a checklist for daily, weekly, and monthly equipment inspections to avoid surprises. Rechargeable devices should be kept fully charged, and disposable items stocked adequately. Consider conducting regular drills to ensure everyone knows how to assemble and troubleshoot the equipment quickly. Is your team prepared to handle an equipment malfunction during a critical moment? Ultimately, the right equipment can enhance your ability to coordinate effectively during resuscitation. By choosing wisely and maintaining readiness, you are investing in better outcomes for your patients.Training And Practice For Effective Coordination
Training and practice are key to effective coordination of positive pressure ventilation with chest compressions. These skills demand precise timing and teamwork. Regular drills build confidence and improve response speed. Practice helps identify challenges and smooth out actions during emergencies.
Simulation Drills
Simulation drills mimic real-life emergencies. They create a safe space for learning and correction. Teams practice delivering breaths and chest compressions at the right moments. These drills improve muscle memory and reduce errors. Feedback sessions after drills highlight areas for improvement. Using realistic equipment and scenarios makes training more effective.
Team Communication Strategies
Clear communication is vital during resuscitation efforts. Teams must use simple, direct language. Assigning roles before starting helps avoid confusion. Call out actions loudly and clearly. Use signals or short phrases to coordinate breaths and compressions. Regular team meetings encourage discussing communication improvements. Practicing communication builds trust and improves teamwork under stress.
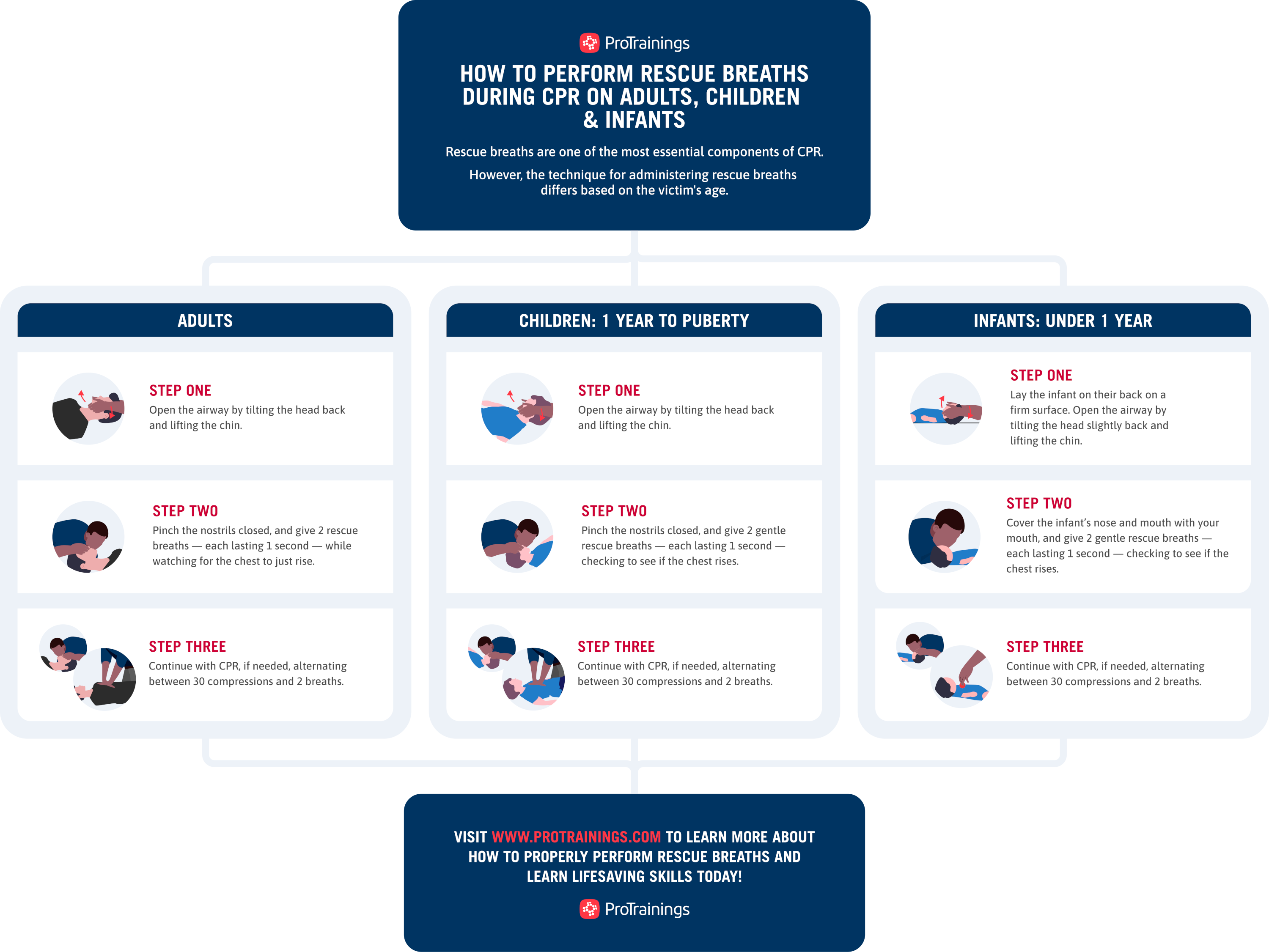
Credit: www.protrainings.com
Frequently Asked Questions
What Is Positive Pressure Ventilation During Chest Compressions?
Positive pressure ventilation delivers air into the lungs using a device during chest compressions. It helps maintain oxygen flow and supports circulation during CPR.
Why Coordinate Ventilation With Chest Compressions?
Coordinating ventilation with compressions improves blood oxygenation and prevents interruptions. It enhances the effectiveness of CPR by optimizing oxygen delivery and circulation.
How Often Should Breaths Be Given With Compressions?
Typically, give 2 breaths after every 30 chest compressions in adults. For children, the ratio may differ, often 15 compressions to 2 breaths.
What Devices Assist Positive Pressure Ventilation During Cpr?
Bag-valve masks and advanced airway devices like endotracheal tubes assist ventilation. These tools help deliver controlled breaths efficiently during chest compressions.
Conclusion
Coordinating positive pressure ventilation with chest compressions saves lives. Timing and technique matter a lot. Always give clear breaths while keeping compressions steady. This helps oxygen flow to the heart and brain. Practice this skill often to improve your response.
Stay calm and focus on smooth, continuous actions. Small steps make a big difference in emergencies. Remember, quick and correct care boosts survival chances. Keep learning and stay prepared for any situation.