If you or a loved one is on a ventilator, you might be wondering when it’s time to consider a tracheostomy. This decision is important and can feel overwhelming.
You want to understand the signs, benefits, and what to expect next. Knowing when to make this switch can improve comfort, reduce risks, and help with recovery. Keep reading to discover clear answers and practical advice that will guide you through this critical step with confidence.
Signs To Consider Tracheostomy
Deciding to switch from a ventilator to a tracheostomy is a critical step in patient care. Certain signs help guide this choice to improve breathing support and overall recovery. Recognizing these signs early can make a big difference in comfort and health outcomes.
Prolonged Ventilation Duration
When a patient needs breathing support for several weeks, prolonged ventilation is a key sign. Long-term use of an endotracheal tube can cause irritation and damage. Tracheostomy offers a safer and more stable airway for extended support.
Difficulty Weaning Off Ventilator
Struggling to reduce ventilator support indicates the need for tracheostomy. Patients who cannot breathe independently after multiple attempts benefit from a tracheostomy tube. It helps ease breathing and improves chances of successful weaning.
Airway Protection Needs
Patients who have trouble clearing secretions or protecting their airway may need tracheostomy. This procedure helps prevent aspiration and lung infections. It also allows easier suctioning and airway management.
Patient Comfort And Mobility
Tracheostomy increases comfort compared to an endotracheal tube. It reduces throat pain and allows patients to speak and eat more easily. It also supports better mobility, helping patients move and participate in therapy.
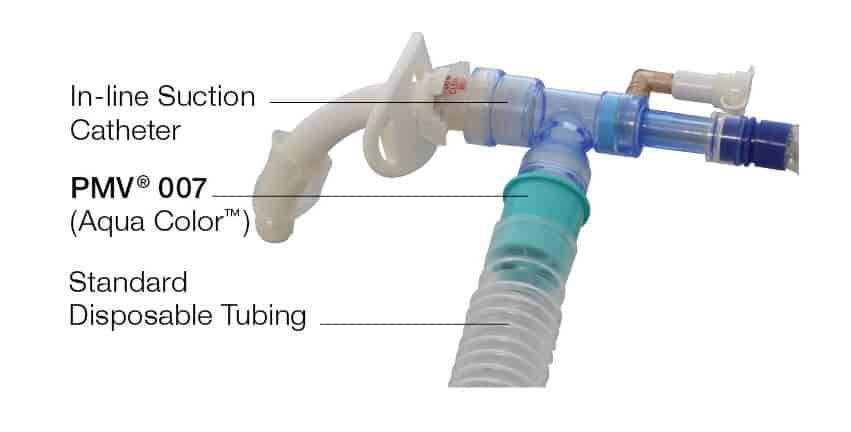
Credit: tracheostomyeducation.com
Benefits Of Tracheostomy
Tracheostomy offers many benefits for patients needing long-term breathing support. It improves airway management and can make recovery easier. The procedure helps patients breathe better and reduces problems linked to prolonged use of a ventilator.
Improved Breathing And Airway Clearance
A tracheostomy creates a direct airway through the neck. This allows air to flow more easily to the lungs. It also helps clear mucus and secretions, reducing the risk of lung infections. Better airway clearance supports faster healing and fewer breathing problems.
Enhanced Patient Comfort
Tracheostomy tubes are often more comfortable than endotracheal tubes. They reduce irritation in the throat and mouth. Patients can move their heads and necks with less discomfort. This comfort helps patients stay calm and recover more smoothly.
Reduced Sedation Requirements
With a tracheostomy, patients usually need less sedation. Sedation is often needed to tolerate a ventilator tube in the mouth or throat. Lower sedation means patients stay more alert and awake. It also decreases risks linked to heavy sedation.
Facilitated Communication
Tracheostomy can help patients speak more easily. Some tubes allow air to pass through the vocal cords. This lets patients talk or use speech aids. Being able to communicate improves mood and cooperation during recovery.
Risks And Complications
Deciding to transition from a ventilator to a tracheostomy involves weighing potential benefits against the risks and complications. While a tracheostomy can offer greater comfort and easier long-term ventilation, it also introduces new challenges that you need to understand. Being aware of these risks helps you make informed decisions and prepares you to manage any issues that may arise.
Infection Risks
Infections are a common concern with tracheostomies. The opening in the neck provides a direct path for bacteria to enter the airway, increasing the chance of infections like tracheitis or pneumonia.
Keeping the area clean and sterile is crucial. You or your caregiver must regularly clean the tracheostomy site and change dressings to prevent harmful bacteria buildup.
Have you considered how strict hygiene routines might fit into your daily life? Even minor lapses can lead to serious infections that require hospital treatment.
Bleeding And Injury
Bleeding can occur during or after the tracheostomy procedure. While minor bleeding is common, significant blood loss or injury to nearby structures like blood vessels or the thyroid gland can be dangerous.
Careful surgical technique reduces these risks, but unexpected complications can still happen. If you notice persistent bleeding or swelling, immediate medical attention is necessary.
Think about how quickly you could respond if bleeding starts suddenly at home. Having a plan and emergency contacts ready can make a big difference.
Tracheal Stenosis
Tracheal stenosis, or narrowing of the windpipe, can develop over time due to scarring from the tracheostomy tube. This condition makes breathing difficult and may require further treatment or surgery.
Regular follow-ups with your healthcare provider can help catch early signs of stenosis. Symptoms such as noisy breathing, coughing, or trouble breathing should never be ignored.
How will you monitor changes in your breathing? Early detection can prevent serious complications and improve your quality of life.
Long-term Care Challenges
Living with a tracheostomy demands ongoing care and attention. Managing suctioning, cleaning, and tube changes can be overwhelming, especially without professional support.
Emotional stress and social challenges also come into play. You might feel isolated or anxious about your appearance and voice changes.
Are you prepared to handle these demands daily? Building a support system and learning practical care techniques can ease the burden and improve your well-being.
Timing Considerations
Timing is a key factor when deciding to switch from a ventilator to a tracheostomy. The right timing can affect comfort, healing, and chances of recovery. Doctors weigh many elements before making this call. The goal is to find the best moment that suits the patient’s needs and medical condition.
Early Vs Late Tracheostomy
Early tracheostomy means placing the tube within the first week of ventilation. It may reduce lung infections and help patients breathe easier. Late tracheostomy happens after two weeks or more on a ventilator. It is often chosen when the patient’s recovery is uncertain.
Studies show early tracheostomy can shorten ICU stays. It may also decrease the time on a ventilator. Late tracheostomy may be safer in some cases, allowing time to see if the patient improves on a ventilator alone.
Impact On Recovery And Outcomes
Tracheostomy can improve comfort by reducing throat irritation. It also helps with speech and swallowing later on. Early tracheostomy often leads to faster weaning from the ventilator. This may improve overall recovery and reduce complications.
Patients with a tracheostomy often have fewer lung infections. They can begin physical therapy sooner, aiding muscle strength. The timing affects how quickly patients regain normal breathing and mobility.
Patient-specific Factors
- Age and general health
- Severity of lung or brain injury
- Risk of infection
- Ability to clear secretions
- Patient’s or family’s wishes
Each patient is unique. Doctors tailor timing based on these factors. Careful assessment ensures the decision supports the best possible outcome.
Decision-making Process
The decision-making process in moving from a ventilator to a tracheostomy is complex. It involves weighing various medical, ethical, and personal factors. This shift is not taken lightly and requires careful deliberation. Many aspects contribute to the final decision, ensuring patient-centered care.
Multidisciplinary Team Approach
A team of specialists assesses each case individually. This team often includes doctors, nurses, and respiratory therapists. Their combined expertise helps determine the best course of action. They consider medical history, current condition, and potential outcomes.
Patient And Family Involvement
The patient’s values and wishes are crucial in decision-making. Families play a significant role, offering insight into the patient’s preferences. Open communication ensures everyone understands the potential benefits and risks. Support from family can guide the team in making compassionate choices.
Assessing Prognosis And Goals
Understanding the patient’s prognosis is essential. The team evaluates the likelihood of recovery or improvement. They consider if a tracheostomy aligns with the patient’s long-term health goals. This assessment helps balance quality of life with medical necessity.
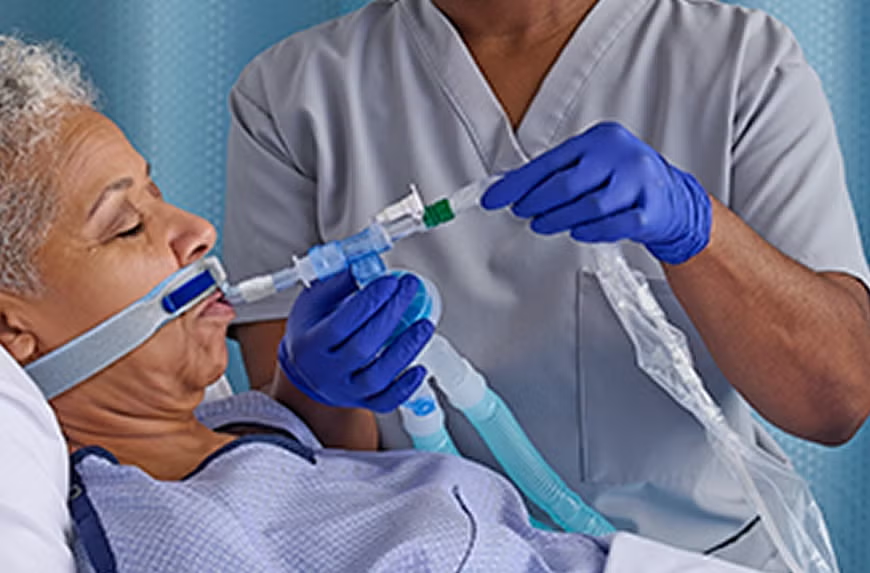
Credit: www.medline.com
Procedure Overview
Transitioning from a ventilator to a tracheostomy involves a careful surgical procedure. This step helps patients who need long-term breathing support. Understanding the procedure is important to know what to expect before, during, and after the surgery. The process can vary based on the technique used and patient condition.
Surgical Vs Percutaneous Techniques
Two main techniques exist for tracheostomy: surgical and percutaneous. Surgical tracheostomy is done through a larger neck incision. It offers clear visibility of structures, useful in complex cases. Percutaneous tracheostomy uses a smaller puncture and dilators. It is less invasive and often done at the bedside. Both methods create an opening in the windpipe to insert a tube. Choice depends on patient anatomy, condition, and healthcare setting.
Preoperative Preparation
Before the procedure, doctors assess the patient’s health thoroughly. Blood tests and imaging may be done to check the neck and airway. Patients must fast for several hours before surgery. Medication adjustments happen based on bleeding risk and other factors. The healthcare team explains the procedure and risks to the patient or family. Proper preparation reduces complications and ensures safety.
Postoperative Care
After tracheostomy, careful monitoring starts immediately. Nurses check the tube position and airway patency often. Cleaning around the stoma site prevents infection. Humidified air and suctioning help clear secretions. Patients may need pain control and respiratory support. Early mobilization and speech therapy begin when stable. Good care supports healing and improves comfort.
Weaning From Tracheostomy
Weaning from a tracheostomy marks a crucial step in patient recovery. It involves carefully removing the tracheostomy tube once the patient can breathe independently. This process reduces risks and improves comfort. Successful weaning depends on thorough assessment, a planned decannulation process, and close monitoring afterward.
Assessment Criteria
- Stable respiratory function without excessive oxygen support
- Ability to cough effectively to clear airway secretions
- Good swallowing function to reduce aspiration risk
- Clear mental status to protect the airway
- Resolution of the underlying cause for ventilation
- Normal or manageable blood gases and vital signs
Decannulation Process
Decannulation starts by gradually reducing tracheostomy tube size. This allows the airway to adapt slowly. Patients may use a speaking valve or capping trial to test breathing without the tube. Medical staff observe for signs of distress or difficulty during trials. If tolerated well, the tube is removed under controlled conditions. Emergency equipment must be ready in case of airway problems.
Monitoring After Removal
- Check breathing rate and oxygen levels frequently
- Watch for coughing, choking, or breathing difficulty
- Observe for signs of airway obstruction or infection
- Ensure patient can clear secretions independently
- Provide support for speech and swallowing as needed
- Schedule follow-up evaluations to confirm airway stability

Credit: tracheostomyeducation.com
Frequently Asked Questions
When Is Tracheostomy Preferred Over Ventilator Use?
Tracheostomy is preferred when long-term ventilation is needed. It reduces airway damage and improves comfort compared to prolonged intubation.
How Long Can A Patient Stay On A Ventilator?
Typically, patients stay on ventilators from days to weeks. If ventilation exceeds two weeks, tracheostomy is often considered.
What Are The Benefits Of Switching To Tracheostomy?
Tracheostomy lowers infection risk, eases breathing, and improves speech. It also facilitates easier airway care and patient mobility.
When Should Doctors Decide To Perform A Tracheostomy?
Doctors consider tracheostomy if ventilation is needed beyond 10-14 days. Patient condition and recovery prospects also influence timing.
Conclusion
Choosing the right time to switch from a ventilator to a tracheostomy matters a lot. It helps patients breathe more comfortably for longer periods. Doctors decide based on health, breathing ability, and recovery progress. This step can reduce risks and improve care quality.
Families should stay informed and ask questions. Clear communication with healthcare teams supports better choices. Every patient’s path is different and needs careful attention. Understanding these basics makes the process less scary and more manageable. Trust the medical team to guide through this important decision.





