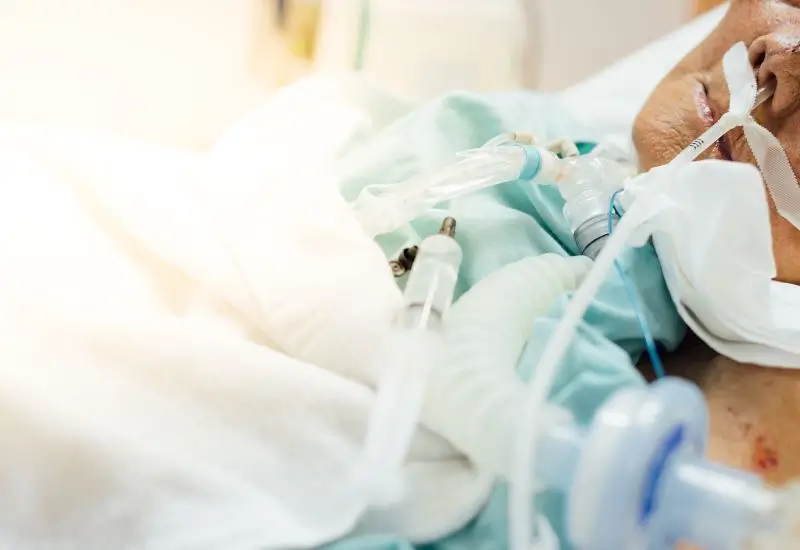
Have you ever wondered how long you—or someone you care about—can survive on a ventilator? It’s a question that sparks both curiosity and concern.
Understanding what a ventilator does, and how long it can support life, can help you feel more prepared and less anxious. You’ll discover the key facts about ventilator survival, what affects the timeline, and what you can expect along the way.
Keep reading to get clear, straightforward answers that could make all the difference for you and your loved ones.

Credit: www.theguardian.com
Ventilator Basics
Understanding the basics of a ventilator is essential before diving into how long someone can survive on one. Ventilators are complex machines, but their primary purpose is straightforward: they help people breathe when their lungs cannot do the job effectively. Knowing what ventilators do and the different types available can help you grasp the role they play in critical care.
What A Ventilator Does
A ventilator supports or replaces the natural breathing process. It pushes air, often enriched with oxygen, into the lungs and helps remove carbon dioxide. This process is vital for patients with severe respiratory issues or during surgery when they cannot breathe on their own.
You might wonder: can a ventilator fully take over breathing? In many cases, it can provide complete respiratory support, but it depends on the patient’s condition. The machine adjusts airflow and pressure based on the patient’s needs, making it a lifesaving tool in intensive care units.
Types Of Ventilators
There are several types of ventilators, each designed for specific situations. The most common ones include:
- Invasive Ventilators:These involve a tube inserted into the windpipe through the mouth or neck. They provide full respiratory support and are used in critical cases.
- Non-invasive Ventilators:These use masks that cover the nose or mouth. They assist breathing without the need for surgery or intubation, often used for less severe respiratory problems.
- Portable Ventilators:Compact and lightweight, these allow mobility for patients who need long-term respiratory support outside the hospital.
Each type serves a different purpose, but they all aim to keep the patient breathing efficiently. Have you ever considered how a simple mask or tube can make the difference between life and death? Understanding these basics helps you appreciate the technology behind critical respiratory care.

Credit: www.jacc.org
Factors Influencing Survival
Surviving on a ventilator depends on several key factors that affect your body’s ability to cope with mechanical breathing support. Understanding these influences can help you grasp why some patients manage longer durations than others. It also sheds light on what medical teams consider when planning care and recovery.
Underlying Health Conditions
Your existing health issues play a huge role in how well you can handle being on a ventilator. Chronic illnesses like diabetes, heart disease, or lung problems can make recovery slower and survival more challenging. For instance, someone with severe COPD may struggle more compared to a person with no lung history.
Doctors often assess these conditions to predict risks and tailor treatments. Have you ever wondered how your current health might affect your chances if you needed ventilation?
Age And Physical Fitness
Age is a critical factor but not the only one. Younger patients tend to have stronger immune systems and better physical reserves, which can improve outcomes. However, a fit older adult may do better than a sedentary younger person with multiple health issues.
Physical fitness before ventilation can influence muscle strength, including the respiratory muscles. This can determine how quickly you regain the ability to breathe on your own after being on a ventilator. How do you think your lifestyle choices impact your resilience in such situations?
Reason For Ventilation
The cause of why you need a ventilator heavily influences survival chances. Temporary issues like surgery recovery or mild pneumonia often have better outcomes. But long-term conditions such as severe lung damage or neurological problems can lead to prolonged ventilation with uncertain results.
Understanding the root cause helps medical staff decide on the best intervention and predict potential complications. It’s essential to ask about the reason behind ventilation to better understand your or your loved one’s situation.
Duration On A Ventilator
The duration a person can survive on a ventilator varies widely based on their underlying health, reason for ventilation, and the care they receive. Understanding the difference between short-term and long-term ventilator use can help you grasp the complexities involved. Let’s look closely at what each duration means for patients and their families.
Short-term Use
Short-term ventilation often lasts from a few hours to several days. It is typically used after surgeries or during acute respiratory illnesses where temporary breathing support is needed.
Patients on short-term ventilators usually have a clear path to recovery. The goal is to wean them off the machine as soon as their lungs can function independently again.
Have you ever wondered how quickly a person can regain normal breathing after surgery? Many recover within 24 to 72 hours, but this depends on individual health and complications.
Long-term Use Challenges
Long-term ventilation can extend for weeks, months, or even years, especially for chronic lung diseases or severe neurological conditions.
Living on a ventilator long-term presents many challenges. These include risks of infections, muscle weakness, and psychological effects like anxiety or depression.
Family members often face tough decisions about care goals and quality of life. Have you considered how much support and resources are needed to manage long-term ventilated patients?
- Risk of ventilator-associated pneumonia
- Possible lung damage from prolonged ventilation
- Need for specialized nursing care
- Emotional strain on patients and families
Knowing the potential difficulties can help you prepare better if you or a loved one ever require extended ventilator support.
Complications During Ventilation
Ventilation can cause problems like infections, lung injury, or breathing difficulties. Survival time varies based on health and illness severity. Close medical care helps manage risks and improve outcomes.
Complications during ventilation can be a challenging aspect of extended ventilator use. While ventilators are life-saving devices, they come with their own set of risks and complications. Understanding these can help you and your loved ones make informed decisions.Infections And Pneumonia
Ventilators can increase the risk of infections, particularly pneumonia. This is known as ventilator-associated pneumonia (VAP). Bacteria can enter the lungs through the ventilator tube, making it crucial for healthcare providers to maintain strict hygiene practices. Patients on ventilators often have weakened immune systems, making them more susceptible to infections. Regular monitoring and timely intervention can significantly reduce this risk. Did you know that elevating the head of the bed can help prevent pneumonia?Lung And Muscle Damage
Prolonged ventilation can lead to lung damage due to the pressure and volume of air being forced into the lungs. This is known as ventilator-induced lung injury (VILI). Adjusting ventilator settings carefully can help minimize this risk. Muscle weakness is another concern, as ventilators can cause the diaphragm and other muscles to weaken. Physical therapy and regular assessments can support muscle strength and prevent long-term damage. How often do you consider the impact of mechanical support on natural body functions? Understanding these complications is vital for anyone dealing with long-term ventilation. Being proactive can make a significant difference in outcomes.Weaning Off The Ventilator
Weaning off a ventilator marks a crucial step in a patient’s recovery journey. It means your lungs and body are beginning to function well enough to breathe independently. This process requires careful assessment and gradual adjustment to ensure safety and success.
Criteria For Weaning
Doctors look for specific signs before starting to reduce ventilator support. These include:
- Stable vital signs:Your heart rate, blood pressure, and oxygen levels should be steady without heavy support.
- Improved lung function:Your ability to breathe on your own should show progress, such as better oxygen exchange.
- Strong cough and airway protection:You need to clear secretions effectively to avoid infections.
- Good mental status:Being awake and able to follow commands helps in managing breathing efforts.
If these criteria aren’t met, premature weaning might put you at risk. Have you ever wondered how your body signals readiness to take over breathing duties again?
Weaning Process And Success Rates
The weaning process usually begins with a spontaneous breathing trial (SBT). During an SBT, you breathe with minimal or no ventilator support for a short period. Doctors closely monitor your response, watching for fatigue or distress.
Success rates vary depending on factors like age, underlying health, and how long you’ve been on the ventilator. Generally, about 70-80% of patients pass their first SBT and successfully get off ventilation.
Patience is key here. Some patients might need multiple attempts over days or weeks. The healthcare team adjusts settings and support based on your progress, ensuring you’re never pushed too hard too fast.
Remember, every step you take toward breathing independently is a victory. How would you feel knowing your body can gradually reclaim control over such a vital function?
Role Of Medical Care And Support
Medical care and support play a crucial role in determining how long someone can survive on a ventilator. The ventilator itself is just a machine that assists with breathing. It’s the continuous monitoring, expert care, and targeted therapies that make the difference in patient outcomes.
Nursing And Monitoring
Nurses are the frontline heroes in ventilator care. They monitor vital signs, adjust ventilator settings, and watch for any signs of complications like infections or lung injuries. Their vigilance helps catch problems early, which can be lifesaving.
Imagine being awake and aware but unable to breathe on your own. The constant presence of skilled nurses provides not only physical support but emotional reassurance. Their role in maintaining hygiene, turning patients regularly, and managing medications directly affects survival chances.
Physical Therapy And Rehabilitation
Physical therapy might seem unrelated to breathing support, but it’s essential. Early movement helps prevent muscle weakness and lung collapse, common risks in long-term ventilator use. Therapists guide gentle exercises even while you’re still dependent on the machine.
Rehabilitation is about preparing you to breathe independently again. It includes breathing exercises, strength training, and gradually reducing ventilator support. Without this step, recovery can stall, and survival times may shorten.
Have you ever thought about how your body responds when it’s immobilized for a long time? The interaction between medical care and your own physical resilience shapes your journey on a ventilator more than you might realize.
Emotional And Psychological Impact
Being on a ventilator affects more than just the body. It changes how patients feel and think. The emotional and psychological impact can be strong and lasting. Patients may feel scared, confused, or lonely. These feelings can affect recovery and overall well-being.
Patient Experience
Patients often face fear and anxiety while on a ventilator. They may feel trapped or unable to communicate well. Sleep can be disturbed, leading to tiredness and frustration. Some patients experience delirium or confusion. The lack of control over their body can cause stress.
Support from doctors and nurses helps reduce these feelings. Simple actions like explaining procedures and offering reassurance make a difference. Patients benefit from hearing familiar voices and seeing loved ones when possible. Small comforts improve their emotional state during this difficult time.
Support For Families
Families also face emotional challenges. They worry about their loved one’s survival and future. The uncertainty can cause stress and sadness. Families may feel helpless or overwhelmed by medical information.
Healthcare teams provide support through clear communication and guidance. Family meetings help answer questions and set expectations. Emotional support services, like counseling, offer relief. Connecting with other families in similar situations provides comfort and hope.

Credit: www.washingtonpost.com
Frequently Asked Questions
How Long Can A Patient Stay On A Ventilator?
A patient can stay on a ventilator from a few days to several weeks. Duration depends on illness severity and recovery speed. Long-term ventilation may require specialized care to prevent complications and support healing.
What Factors Affect Ventilator Survival Time?
Survival time on a ventilator depends on age, underlying health, illness severity, and response to treatment. Complications like infections or lung damage also impact survival. Each patient’s condition is unique, influencing their ventilator duration.
Can Patients Recover Fully After Ventilator Use?
Many patients recover fully after ventilator support with proper care and rehabilitation. Recovery depends on the underlying illness and overall health. Early medical intervention improves the chances of successful weaning and full recovery.
What Risks Are Associated With Long-term Ventilator Use?
Long-term ventilator use can lead to infections, lung injury, muscle weakness, and airway damage. Proper medical care reduces these risks. Monitoring and timely intervention are crucial to minimize complications during prolonged ventilation.
Conclusion
Surviving on a ventilator depends on many health factors. Some patients use it for days, others for weeks or months. Doctors watch closely to adjust care as needed. Quality of life and recovery chances vary a lot. Families should talk openly with medical teams for clear answers.
Ventilators help save lives but are not a cure. Each case is unique and needs careful attention. Understanding this helps prepare for what lies ahead.