If you or a loved one ever needs a ventilator, you probably have many questions. One big concern is, how long can you actually stay on a vent?
The answer matters because it affects your recovery, comfort, and future health. You’ll discover clear, simple facts about ventilator use. You’ll learn what to expect, what risks are involved, and how doctors decide the right time to wean you off.
Keep reading to understand what being on a vent means for you or someone you care about—and take control of your health with knowledge.
Purpose Of Mechanical Ventilation
Mechanical ventilation helps patients breathe when their lungs cannot work well. It supports oxygen delivery and removes carbon dioxide. This support can be short-term or longer, depending on the patient’s condition. Ventilators help save lives by giving the lungs time to heal. They are essential in many medical situations.
When Is Ventilation Needed
Ventilation is needed when the body cannot get enough oxygen. It is also used when the lungs cannot remove carbon dioxide properly. Common reasons include:
- Severe lung infections
- Injury to the chest or lungs
- During surgery under general anesthesia
- Chronic lung diseases in advanced stages
- Neurological problems affecting breathing muscles
Doctors decide on ventilation based on breathing tests and patient health.
Types Of Ventilators
Ventilators come in different types to match patient needs. Some types include:
- Invasive Ventilators:Use a tube inserted into the windpipe.
- Non-invasive Ventilators:Use masks to deliver air without tubes.
- Portable Ventilators:Small machines for use outside hospitals.
- High-Frequency Ventilators:Deliver very fast breaths with small volumes.
Each type helps patients in specific ways. Doctors choose the right ventilator based on the illness and breathing needs.

Credit: www.zoll.com
Duration Factors On A Ventilator
The time a person stays on a ventilator varies widely. Several factors affect this duration. Understanding these factors helps families and patients prepare for what lies ahead.
Doctors consider many elements before deciding how long to keep someone on a ventilator. Each patient’s situation is unique. The goal is to support breathing without causing harm.
Patient’s Medical Condition
The patient’s health plays a major role. Severe lung damage or chronic illnesses often require longer ventilation. Mild cases may need support for a short time only.
Age and overall strength also matter. Younger, healthier patients usually recover faster. Those with weak immune systems may take longer to improve.
Response To Treatment
How well the patient responds to treatment is crucial. Improvement in lung function signals readiness to reduce ventilator use. Lack of progress may extend the time on the machine.
Doctors monitor oxygen levels, breathing effort, and other vital signs. These help decide when to wean the patient off the ventilator safely.
Complications And Risks
Complications can lengthen ventilation time. Infections like pneumonia may develop during ventilation. These infections slow recovery and require more care.
Other risks include lung injury from the ventilator itself. Doctors aim to minimize these risks with careful settings and monitoring. If complications arise, the patient may need more time to heal.
Short-term Ventilation
Short-term ventilation supports breathing for a limited time. It helps patients during surgery or sudden breathing problems. This type of ventilation is temporary and aims to stabilize the patient quickly. Doctors monitor closely to avoid complications. The goal is to help the lungs recover and reduce stress.
Typical Time Frames
Short-term ventilation usually lasts from a few hours to several days. Most patients need it for less than one week. The exact duration depends on the patient’s condition and how well they respond to treatment. Doctors try to wean patients off the ventilator as soon as possible. Prolonged use increases the risk of lung infections and muscle weakness.
Common Scenarios
- During and after surgery requiring general anesthesia
- Acute respiratory failure due to illness or injury
- Severe infections like pneumonia causing breathing difficulty
- Trauma cases with chest injuries or unconsciousness
- Short-term respiratory support during sedation in ICU
Credit: www.jlconline.com
Long-term Ventilation
Long-term ventilation supports people who need breathing help over weeks, months, or years. It helps maintain breathing when lungs cannot work properly alone. Patients can live better with the right care and equipment.
Chronic Conditions Requiring Extended Support
Some illnesses need long-term ventilation to keep patients stable. Common conditions include:
- Chronic obstructive pulmonary disease (COPD)
- Neuromuscular diseases like ALS or muscular dystrophy
- Severe spinal cord injuries
- Advanced lung diseases such as cystic fibrosis
- Sleep apnea with respiratory failure
These conditions reduce lung function or muscle strength. Ventilation helps improve oxygen levels and reduces breathing effort.
Home Ventilation Options
Many patients use ventilators at home for comfort and independence. Home ventilation includes:
- Non-invasive ventilation with masks
- Tracheostomy ventilation with a breathing tube
- Portable ventilators for mobility
- Monitors to track breathing and alarms
Home care teams teach families to manage ventilators safely. Regular check-ups ensure equipment works well and patients stay healthy.
Risks Of Prolonged Ventilation
Prolonged ventilation can cause lung infections and muscle weakness. Staying on a ventilator too long may also increase the risk of breathing problems. Doctors carefully monitor patients to avoid these risks.
When you or a loved one is on a ventilator, the primary focus is often on immediate survival. However, it’s crucial to be aware of the risks associated with prolonged ventilation. While ventilators are life-saving devices, extended use can lead to several complications. Understanding these risks can empower you to ask the right questions and make informed decisions.Lung Damage
Prolonged ventilation can lead to lung damage. The constant pressure can injure the lung tissues, a condition known as ventilator-associated lung injury. You might wonder if there’s a safer way to support breathing. Discussing alternative ventilation strategies with your healthcare provider could be a step in the right direction.Infections
Being on a ventilator for an extended period increases the risk of infections. Ventilator-associated pneumonia is a significant concern. Bacteria can enter the lungs through the breathing tube, leading to serious complications. It’s vital to maintain vigilant hygiene practices and monitor for signs of infection, such as fever or increased mucus.Muscle Weakness
Muscle weakness is another potential risk of prolonged ventilation. You might notice that after days or weeks on a ventilator, basic movements become challenging. This condition, known as ventilator-induced diaphragmatic dysfunction, can make recovery slower. Regular physiotherapy and early mobilization can help mitigate this risk and aid in faster recovery. By understanding these risks, you can take proactive steps to ensure the best care for yourself or your loved one. Are there questions you’re still pondering? Engaging with healthcare professionals about these concerns can provide clarity and peace of mind.Weaning Off The Ventilator
Weaning off the ventilator is a critical step in recovery for patients who have been on mechanical breathing support. It involves gradually reducing the ventilator’s assistance until the patient can breathe independently. This process demands careful monitoring to ensure safety and success. The goal is to help the patient regain normal breathing without strain or risk.
Assessment For Readiness
Doctors check many factors to decide if a patient is ready to wean off the ventilator. They look at lung function, oxygen levels, and overall health. The patient must be stable, alert, and able to breathe with less help. Tests may include breathing trials and monitoring heart rate and blood pressure. Only when all signs are positive does the weaning process begin.
Weaning Methods
Different methods help patients adjust to breathing without the ventilator. Common approaches include:
- Spontaneous Breathing Trials (SBT): The patient breathes on their own for a short time.
- Pressure Support Ventilation (PSV): The machine helps only with extra effort.
- SIMV (Synchronized Intermittent Mandatory Ventilation): The ventilator and patient share breathing work.
The choice depends on the patient’s condition and response. Slow, steady progress is key.
Challenges During Weaning
Weaning can be difficult. Patients may feel tired or short of breath. Anxiety and muscle weakness can slow progress. Some develop lung problems or infections that delay weaning. Careful support from the medical team helps manage these challenges. Patience and close observation improve chances of success.
Emotional And Psychological Impact
The emotional and psychological impact of being on a ventilator often goes unnoticed but is deeply significant. Patients face a mix of fear, uncertainty, and frustration as they adjust to this life-supporting machine. Understanding these feelings can help you prepare mentally and emotionally for the journey.
Patient Experience
Being on a ventilator can feel isolating and overwhelming. Many patients describe moments of panic when they struggle to breathe on their own or when communication becomes difficult. This can lead to feelings of helplessness and anxiety.
One patient shared how small victories, like being able to say a word or take a few breaths independently, became powerful motivators. These moments show that progress may be slow but meaningful, reminding you to celebrate each step forward.
How do you cope when your body feels trapped but your mind is fully aware? Techniques like deep breathing exercises, guided imagery, or even simple conversations with caregivers can provide emotional relief and a sense of control.
Support For Families
Families often experience a rollercoaster of emotions alongside the patient. They may feel helpless watching a loved one rely on a ventilator, while also managing their own fears and exhaustion.
Support networks, including counseling services and support groups, can make a big difference. These resources offer a space to share worries and gain practical advice, helping families stay strong during challenging times.
Encourage open communication with the medical team to stay informed and involved. This connection can ease anxiety and empower families to advocate effectively for their loved ones.
Advances In Ventilation Technology
Ventilation technology has improved, allowing patients to stay on a ventilator longer with better comfort. The duration depends on health and specific needs. Doctors carefully monitor to avoid complications during extended use.
Advances in ventilation technology have significantly transformed patient care in recent years. These advancements have not only improved the effectiveness of ventilators but have also enhanced the overall experience for patients. Imagine a situation where being on a ventilator is less daunting, with increased safety and comfort—this is becoming a reality thanks to cutting-edge innovations.Improved Safety Features
Modern ventilators now come equipped with sophisticated safety features that minimize risks. Advanced sensors can detect changes in a patient’s condition almost instantly. This prompt response allows healthcare providers to make timely interventions, reducing the likelihood of complications. These features are designed to provide peace of mind to both the patient and their loved ones. Knowing that technology is actively working to safeguard their health can be incredibly reassuring.Enhanced Patient Comfort
Comfort has become a priority in the design of new ventilators. Soft, flexible tubing and quieter machines contribute to a more pleasant experience. This is crucial for patients who may be on ventilators for extended periods. Additionally, personalized settings allow for adjustments that cater to individual patient needs. Imagine being able to breathe more naturally and comfortably, even with the assistance of a machine. This focus on comfort can significantly improve a patient’s overall well-being and recovery process. Have you ever considered how these advancements might change the experience of being on a ventilator for you or someone you know? It’s fascinating to think about how technology continues to evolve to better meet human needs.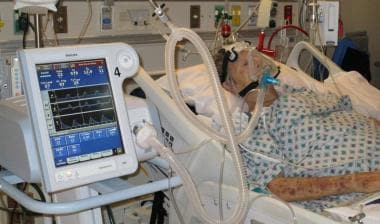
Credit: emedicine.medscape.com
Frequently Asked Questions
How Long Can A Patient Stay On A Ventilator?
Patients can stay on a ventilator from a few hours to several weeks. Duration depends on illness severity and recovery speed. Doctors regularly assess readiness to wean off the ventilator. Prolonged use may lead to complications, so careful monitoring is essential.
What Factors Affect Ventilator Duration?
Ventilator duration depends on patient age, underlying conditions, and illness severity. Recovery speed and response to treatment also play key roles. Complications like infections can extend ventilator use. Individualized care plans guide the length of ventilation support.
Can Long-term Ventilator Use Cause Complications?
Yes, long-term ventilator use can cause infections, lung damage, and muscle weakness. It may also increase the risk of pneumonia and airway injury. Medical teams work to minimize risks through careful monitoring and timely weaning.
When Can A Patient Be Weaned Off Ventilation?
Patients can be weaned off ventilation once they regain sufficient lung function and strength. Doctors evaluate breathing ability, oxygen levels, and overall health. Gradual reduction in ventilator support helps ensure safe breathing without assistance.
Conclusion
Being on a ventilator can last from days to weeks or longer. Doctors watch patients closely to decide the right time to stop. Each person’s situation is different. Recovery depends on many factors like health and illness severity. Ventilators help patients breathe when they cannot do it alone.
Knowing how long you might need one helps prepare for the journey. Always ask healthcare providers for updates and support. Understanding this process makes a tough time a bit easier to handle.





