Are you confused about the difference between a BiPAP machine and a ventilator? You’re not alone.
Many people wonder if these devices are the same or if one is better than the other. Understanding how each works can help you make informed decisions about respiratory care for yourself or a loved one. Keep reading to discover the key differences, how each device supports breathing, and which might be right for your situation.
This knowledge could make a big difference in your health and comfort.
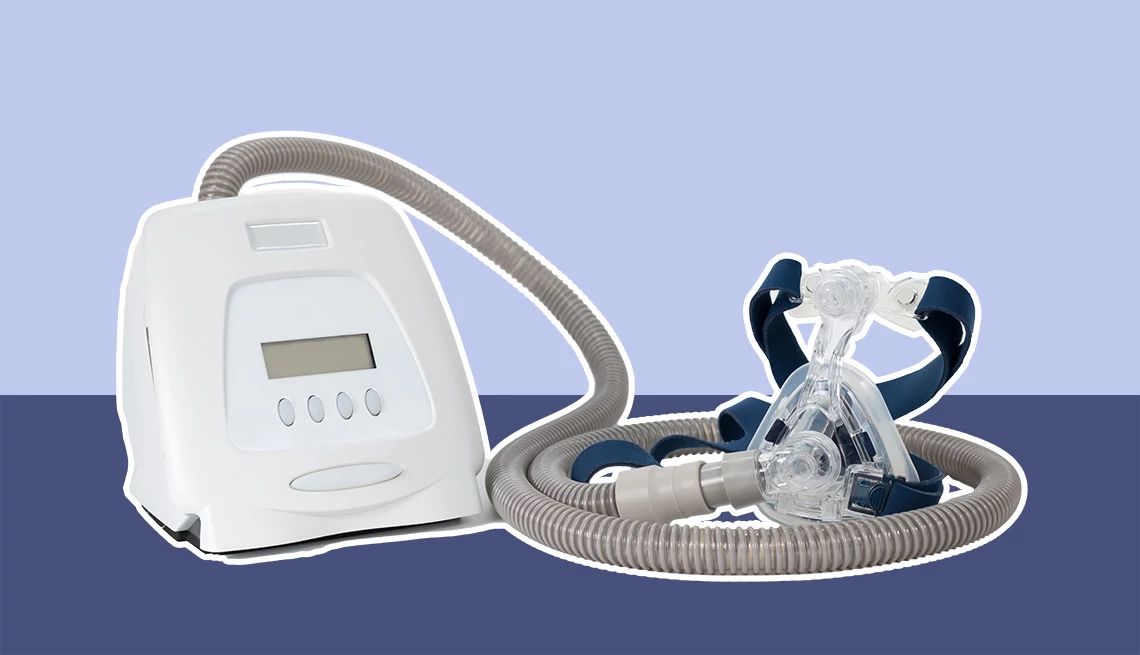
Credit: www.aarp.org
Basics Of Bipap
BiPAP, short for Bilevel Positive Airway Pressure, is a device that helps people breathe better. It delivers two levels of air pressure to the lungs. This support makes breathing easier for those with breathing problems. Understanding BiPAP basics helps clarify its role in respiratory care.
How Bipap Works
BiPAP uses two pressure levels. One level helps when you breathe in. It pushes air into your lungs. The other level helps when you breathe out. It lowers the pressure so you can exhale comfortably.
This alternating pressure helps keep the airways open. It improves oxygen flow and removes carbon dioxide. The machine adjusts automatically based on your breathing pattern.
Common Uses Of Bipap
- Sleep apnea treatment to prevent airway collapse during sleep
- Chronic obstructive pulmonary disease (COPD) to ease breathing
- Respiratory failure support without full ventilation
- Assisting patients with neuromuscular diseases affecting breathing
- Post-surgery breathing aid to reduce lung complications
What Is A Ventilator
A ventilator is a medical device designed to help people breathe when they cannot do so adequately on their own. It supports or completely takes over the breathing process, ensuring oxygen reaches the lungs and carbon dioxide is removed from the body. Understanding what a ventilator does is key to knowing how devices like BiPAP machines differ or relate to them.
Types Of Ventilators
Ventilators come in various forms depending on the patient’s needs and the level of respiratory support required. Here are the common types:
- Invasive Ventilators:These deliver air through a tube inserted into the windpipe. They are used in critical care when patients cannot breathe independently.
- Non-Invasive Ventilators:These use masks or nasal devices to provide support without needing tubes in the airway. BiPAP machines fall into this category.
- Transport Ventilators:Portable versions used during patient transfers or emergencies.
Knowing the type helps you understand how much control the machine has over breathing and how comfortable it might be.
Ventilator Functions
Ventilators perform several essential functions to assist breathing:
- Oxygen Delivery:They supply oxygen-rich air to improve blood oxygen levels.
- Carbon Dioxide Removal:By helping exhale properly, ventilators prevent CO2 buildup.
- Breath Support:They can either fully breathe for you or assist your natural breathing effort.
- Pressure Control:Ventilators regulate the air pressure to keep airways open and lungs inflated.
Think about how your lungs work naturally and how these machines step in when that process struggles.
Bipap Vs Ventilator
BiPAP and ventilators both help with breathing but serve different roles. Understanding their differences clarifies their use in healthcare. This section compares BiPAP machines and ventilators to highlight key features.
Modes Of Operation
BiPAP stands for Bilevel Positive Airway Pressure. It delivers air at two pressure levels: higher when you breathe in, lower when you breathe out. It supports natural breathing without taking full control.
Ventilators provide full or partial breathing support. They can control breathing completely or assist based on settings. Ventilators often manage more severe breathing problems.
Patient Interaction
BiPAP requires active patient effort to trigger breaths. It supports but does not replace natural breathing. Patients need enough strength to breathe with the machine.
Ventilators can breathe for patients. They are used when patients cannot breathe on their own. Ventilators can control the timing and depth of each breath.
Settings And Controls
- BiPAP settings include inhalation and exhalation pressures.
- BiPAP may adjust backup respiratory rate if needed.
- Ventilator settings are more complex, controlling volume, pressure, and oxygen levels.
- Ventilators allow precise control over breathing patterns and support.
When To Use Bipap
Knowing when to use BiPAP can make a significant difference in managing breathing difficulties. This device offers a non-invasive way to support your lungs without the complexity of full ventilation. Understanding the right situations for BiPAP helps you and your healthcare provider make informed choices.
Suitable Conditions
BiPAP is often recommended for people with conditions that cause breathing challenges but don’t require full ventilator support.
- Chronic Obstructive Pulmonary Disease (COPD):It helps reduce the work of breathing and improves oxygen levels.
- Sleep Apnea:BiPAP keeps your airway open during sleep, preventing pauses in breathing.
- Congestive Heart Failure:It can reduce fluid buildup in the lungs by improving ventilation.
- Neuromuscular Diseases:For those with weakened breathing muscles, BiPAP assists in maintaining proper ventilation.
If you experience sudden breathing difficulty but still maintain some control over your breaths, BiPAP might be the right option.
Advantages Of Bipap
BiPAP has clear benefits that set it apart from other respiratory support methods.
- Non-Invasive:It uses a mask instead of a tube, which lowers the risk of infections and discomfort.
- Adjustable Pressure:BiPAP provides different pressures for inhaling and exhaling, making breathing easier and more natural.
- Improves Gas Exchange:By supporting both inhalation and exhalation, it enhances oxygen intake and carbon dioxide removal.
- Flexible Use:You can use it at home or in the hospital, giving you more control over your treatment.
Have you ever wondered if a less invasive option could improve your breathing without confining you to a hospital bed? BiPAP offers that balance.
When Ventilators Are Needed
Bipap machines help support breathing by pushing air into the lungs but are not full ventilators. Ventilators take over breathing completely for patients who cannot breathe on their own. Bipap is often used for less severe breathing issues.
When ventilators are needed, it’s often a critical moment in a patient’s healthcare journey. The decision to use a ventilator isn’t taken lightly and usually occurs when a person can no longer breathe adequately on their own. This can be due to severe illness, surgery, or an unexpected medical emergency.Critical Conditions
In critical conditions, ventilators serve as a lifeline. They support patients who have severe respiratory illnesses, like pneumonia or COVID-19, by ensuring they get enough oxygen. Without this support, the body’s organs may not receive sufficient oxygen, leading to further complications. Ventilators are often essential in intensive care units. They aid patients who have experienced trauma, undergone major surgery, or suffered from conditions like stroke. Have you ever considered how quickly the situation can escalate from manageable to critical without timely intervention?Benefits Of Ventilator Support
Ventilator support provides several benefits that can be crucial for patient recovery. It allows the lungs to rest and heal while ensuring the body gets the oxygen it needs. This support can prevent further damage by maintaining a stable airway and reducing the work of breathing. For some patients, ventilators offer a temporary solution while they recover their strength. Have you seen someone regain their ability to breathe independently, thanks to ventilator support? It’s an empowering moment that underscores the importance of this medical device.
Credit: www.healthyjeenasikho.com
Risks And Limitations
Understanding the risks and limitations of BiPAP and ventilators is crucial. Both devices assist breathing but carry specific challenges. Recognizing these helps users and caregivers make safer choices.
Potential Complications With Bipap
BiPAP machines can cause discomfort or side effects. Common issues include:
- Dry mouth or nose due to airflow
- Skin irritation from the mask
- Eye irritation if air leaks near eyes
- Claustrophobia or anxiety from wearing the mask
- Sinus pain or headaches
In rare cases, improper use may lead to lung injury or worsened breathing. Users must follow medical advice and machine settings carefully.
Ventilator-associated Risks
Ventilators provide stronger breathing support but bring higher risks. These include:
- Infections, especially pneumonia
- Lung damage from high air pressure
- Dependence on the machine for breathing
- Discomfort and need for sedation
- Complications from prolonged use
Ventilator patients require close monitoring by healthcare professionals. Safety protocols reduce but do not eliminate these risks.
Choosing Between Bipap And Ventilator
Choosing between a BiPAP and a ventilator depends on the patient’s breathing needs and medical condition. Both devices support breathing but serve different roles. Understanding these differences helps make better care decisions.
Clinical Decision Factors
Doctors assess several key factors before choosing a BiPAP or ventilator. These include:
- Severity of breathing difficulty
- Level of consciousness
- Ability to protect the airway
- Underlying health conditions
- Oxygen and carbon dioxide levels in the blood
BiPAP is often used for moderate breathing problems. It helps patients breathe better without invasive tubes. Ventilators are used for severe cases needing full breathing support.
Role Of Healthcare Providers
Healthcare providers play a vital role in deciding the right treatment. They monitor patients closely and adjust support based on progress. Nurses, respiratory therapists, and doctors work together to ensure proper care.
Providers explain the options clearly and answer questions. They also watch for side effects or complications. Their expertise ensures the patient receives the safest and most effective support.
.png?width=275&name=stencil.instagram-photo%20(90).png)
Credit: blog.nursing.com
Future Trends In Respiratory Support
Respiratory support technology evolves rapidly. BiPAP machines and ventilators improve with new trends. These advances aim to enhance care and patient comfort. Let’s explore future trends in respiratory support.
Technological Advances
BiPAP devices integrate smart technology. They monitor breathing patterns closely. This data helps customize treatment for each patient. Machine learning algorithms predict patient needs. This leads to timely adjustments and better support.
Telemedicine is growing in respiratory care. Patients connect with doctors from home. Remote monitoring tools track their progress. This reduces hospital visits and enhances convenience. Advanced sensors now improve machine efficiency. They detect breathing issues early. This ensures prompt intervention and safety.
Improving Patient Outcomes
New materials make masks more comfortable. They fit better and reduce skin irritation. Noise reduction features in machines enhance sleep quality. Patients rest better and feel more refreshed.
BiPAP machines now offer humidification options. This prevents dry throat and nasal passages. Patients experience fewer discomforts and better therapy adherence. Continuous innovation leads to lightweight designs. Portable machines provide freedom for active lifestyles.
Education and training programs expand. Patients and caregivers gain valuable knowledge. They learn to manage devices effectively. This empowers them and improves overall outcomes.
Frequently Asked Questions
What Is The Main Difference Between Bipap And A Ventilator?
BiPAP provides non-invasive breathing support using a mask. Ventilators are invasive devices that assist or control breathing through intubation. BiPAP is typically used for milder respiratory issues, while ventilators support critical respiratory failure cases.
Can Bipap Replace A Ventilator For All Patients?
No, BiPAP cannot replace ventilators for all patients. BiPAP suits those with moderate breathing difficulties. Ventilators are essential for patients needing full respiratory support or unable to breathe independently.
How Does Bipap Help Patients With Breathing Problems?
BiPAP delivers pressurized air at two pressure levels to keep airways open. It improves oxygen intake and removes carbon dioxide. This helps patients with sleep apnea, COPD, and other breathing disorders breathe easier.
Is Bipap Considered A Mechanical Ventilator?
BiPAP is a type of non-invasive ventilatory support but not a full mechanical ventilator. It assists breathing without intubation, while mechanical ventilators provide controlled ventilation invasively for critical care.
Conclusion
A BiPAP is not the same as a ventilator, but both help with breathing. BiPAP machines assist by giving air pressure to keep airways open. Ventilators take over breathing completely for patients who cannot breathe alone. Understanding these differences helps you know the right treatment.
Always follow medical advice for the best care. Breathing support devices play a key role in health. Knowing how they work makes decisions clearer and easier.





